1 Introduction
1.1 Continence care
Incontinence is not a disease but a symptom of an underlying condition. Through informed assessment and investigation by a suitably trained professional, individuals suffering from bladder or bowel dysfunction may have symptoms resolved, improved or managed in the most appropriate way, without the primary focus placed on the supply of continence products. The importance of the assessment cannot be overestimated, as treatment for continence is dependent on the cause(s) (Button et al., 1999).
1.2 Urinary catheterisation
Urinary catheterisation is a common procedure both in acute and community settings. Catheterisation is not without risk, urinary tract infections (UTI’s) are the largest single group of Healthcare Associated Infections (HCAI) and the presence of a urinary catheter, and the duration of its insertion are contributory factors to the development of urinary tract infection. (Emmerson, 1996). Therefore, urinary catheters should only be used when there is no suitable alternative, and even then, kept in place for as short a time as possible, (National Institute for Health and Care Excellence, 2012) last updated 2017.
1.3 Referral pathway into the specialist continence service (SCS)
The registered healthcare professional remains accountable for the initial assessment of continence and instigation of first line treatment, such as fluid and basic constipation advice, following guidance from the trigger questions (see appendix A). Referral to the specialist continence service should then be made if symptoms persist.
The specialist continence service accepts referrals for the following:
- patients who require a comprehensive bladder and bowel assessment and treatment
- for assessment for trans anal irrigation
- trial without catheters
- intermittent self-catheterisation and intermittent self-dilatation
- non-housebound catheter patients for catheter clinic
- complex bladder and bowel patients
- for the long-term management of catheter products, excluding housebound patients with long term indwelling catheters
Patients aged over 18, registered with a Doncaster GP may be referred by the following:
- community nursing services
- primary care
- secondary care
- social care providers
- care homes (with or without nursing)
- other healthcare providers
Referrals to the specialist continence service can be made by electronic referral SystmOne or via email to single point of access (SPA) following completion of a referral form (appendix B). All referrals will be triaged by an appropriate member of the Specialist Continence Service team. The patient will be assessed for eligibility and acuity based on the following tiered criteria:
- urgent, assessments for patients not already on the specialist continence service caseload, presenting with sudden incontinence
- non-urgent, assessment or follow-up for patients on the specialist continence service caseload with a recurring issue or mild exacerbation
- planned, scheduling of planned activity, for example, trial without catheter (TWOCs) to support patients discharged into the community
Patients, or their carer and advocate, should be asked to complete a symptom diary for the appropriate period of time, with an appointment being offered within a maximum of 15 working days from receipt of referral.
1.4 Contact information
Specialist continence advice can be obtained from the trust specialist continence service on 03000 218 996.
2 Purpose
The purpose of the manual and the linked procedures is to provide clear, concise guidance on continence and urinary catheter care for all colleagues whether in a direct or indirect patient care role, regardless of the care environment. It is acknowledged that some colleagues work in premises over which they have little or no control (for example, patient’s own homes), therefore in some instances colleagues will have to use their own judgement in the interpretation of certain procedures.
The content of the manual and linked procedures is based on sound specialist continence principles and national guidance.
3 Scope
This manual applies to all clinical colleagues working in the Doncaster care group of the trust who deliver or provide continence or catheter care to adult patients over the age of 18. It is recognised that primary care practitioners are also part of the organisation and as such this manual is offered for use by them to adapt to their own practices and organisations as appropriate. The author of the manual is available to offer help and support to primary care practitioners who wish to use and implement this manual. As part of good employment practice, agency workers are also required to abide by the trust policies and procedures, as appropriate, to ensure their health, safety and welfare whilst undertaking work for the trust.
Adherence to the procedures within this manual is the responsibility of all trust colleagues, including agency, locum and bank colleagues. For colleagues working in Rotherham and Scunthorpe, they will need to refer to local guidelines.
4 Responsibilities, accountabilities and duties
The chief executive is responsible for ensuring the trust employs a comprehensive strategy to support the management of risk, including clinical risks associated with patient care across the organisation.
The board of directors is responsible for having policies and procedures in place to support best practice, effective management, service delivery, management of associated risks and meet national and local legislation.
Care group directors are responsible for the implementation of the policy within their specific areas.
The role of the specialist continence nurse includes:
- providing expert professional advice on bladder and bowel care, delegating responsibility to trust colleagues as appropriate
- providing education on bladder and bowel care to other professionals, multi-disciplinary groups, patients and carers
- assess, plan, deliver and evaluate person centred continence care to patients, in a variety of different care settings, including, patients own home, clinic and care homes
- managing the complex patients referred to the service
- undertake continence and catheter audits in care homes, reporting outcome to Doncaster Integrated Care Board (ICB)
- contributing to serious incidents (SIs) reports as required
Clinical team leaders or ward managers’ duties and responsibilities for areas under their control ensure that staff:
- can demonstrate compliance with the manual and the continence formulary
- are given protected time to attend the relevant continence and catheter study days
All colleagues who are involved with the care of a patient within the inpatient services and community must comply with this manual and procedures.
It is the responsibility of each individual member of colleagues to adhere to the requirements set out within this policy.
Duties of the continence link champions include:
- acting as a resource within their working environment, for patients, colleagues and visitors
- acting as role models, always encouraging good continence care
- liaising closely with the specialist continence service
5 Procedures
These will be listed here on the webpage as hyperlinks to each procedure document along with appendices, references and so on.
5.1 Autonomic dysreflexia safe management of bladder and bowel care procedure
5.1.1 Symptoms of autonomic dysreflexia
- Flushing.
- Sweating and goose pimples.
- Pounding headache.
- Peripheral cyanosis.
- Blurred vision and dizziness.
- Shortness of breath.
Slow pulse staff must consider autonomic dysreflexia (AD) and assess for potential causes listed below, as early recognition of autonomic dysreflexia is essential in order that treatment can be initiated immediately.
5.1.2 Common causes
5.1.2.1 Bladder
- Distended bladder.
- A kink in the catheter.
- An over-full catheter bag.
- Blockage or obstruction that prevents urine flowing from the bladder.
- Urinary tract infection or bladder spasms.
- Bladder stones.
5.1.2.2 Bowel
- Distended bowel which can be due to a full rectum, constipation or impaction.
- Any stimulation to the rectum including digital stimulation or digital removal of faeces.
- Haemorrhoids.
- Anal Fissures.
- Stretching of rectum or anus or skin breakdown in the area.
5.1.2.3 Examples of other causes
- Pressure sores.
- Sexual activity.
- Gynaecology-menstrual pain, labour and delivery.
- Bone fractures below the level of the spinal cord injury.
- Pain and trauma.
- Acute conditions such as gastric ulcer.
- Deep vein thrombosis.
Tight clothing, any noxious stimuli may trigger an autonomic response and therefore an autonomic dysreflexia event.
5.1.3 Treatment
If autonomic dysreflexia is suspected:
- assist the patient to sit upright as soon as possible
- record blood pressure (BP)
- if the systolic blood pressure is elevated (greater than 150mmHg) it should be treated until the cause is found and eliminated
- give Glyceryl tri-nitrate-(GNT) spray or nifedipine as prescribed
Once the cause has been addressed continue to monitor blood pressure. This must be monitored for a minimum of two hours after it has been stabilised.
5.1.3.1 Identify and remove the cause
5.1.3.1.1 Bladder
Do not attempt to administer a catheter maintenance solution as this could increase the blood pressure.
If the patient has an indwelling urethral or suprapubic catheter, check the following:
- is the drainage bag full?
- is the tubing kinked?
- is the drainage bag at a higher level than the bladder?
- is the catheter blocked? After correcting the obvious problem, and if the catheter is still not draining after 2 to 3 minutes, change the catheter immediately
5.1.3.1.2 Bowel
A digital rectal examination (DRE) is required to ascertain if the rectum is full and if so to remove the blockage. This is done by:
- donning personal protective equipment (PPE)
- inserting a gloved finger lubricated with an anaesthetic lubricant, such as 2% lignocaine gel (Instillagel) into the rectum
- if the rectum is full insert additional lubricant
- it is necessary to wait a minimum of 3 minutes to in order to reduce the sensation in the rectum. Not waiting for this length of time prior to performing digital stimulation (in order to trigger peristalsis) and digital rectal examination may worsen the autonomic dysreflexia
- please refer to the Royal College of Nursing, bowel care leaflet for further information
If autonomic dysreflexia symptoms develop whilst digital rectal examination is being undertaken the procedure must be stopped immediately and only resumed after the symptoms subside. If dysreflexia persists or no cause can be found, then an emergency medical assessment is required.
5.1.4 Prevention
Prevention is essential as most causes can be avoided by:
5.1.4.1 Bladder
- Change catheter regularly to prevent blockage.
- Keep catheters free of kinks, clean and ensure the intermittent catheterisation regime is followed to avoid an overfull bladder.
- Check signs of infection, for example, urinary tract infection (UTI).
- Have regular bladder and bowel check-ups with either the general practitioner (GP), community nurse or spinal injuries unit.
- Drink enough fluids.
5.1.4.2 Bowel
- Maintain a regular bowel management plan. If you have any concerns or queries about the bowel management plan, liaise with the spinal injuries or neurorehabilitation consultant involved with the patients care.
- Adequate fibre intake to help avoid constipation.
- Get treatment for haemorrhoids.
5.1.5 Autonomic dysreflexia emergency kit
Ensure the patient has an autonomic dysreflexia (AD) kit available with them, this should contain:
- catheter and supplies for catheterisation
- medication prescribed for autonomic dysreflexia (Glyceryl tri-nitrate- (GNT) Spray or Nifedipine)
- anaesthetic lubricant like 2% lidocaine gel
- dressing pack, including sterile gloves and apron
- wet wipes and disposable bag
5.2 Basic catheter care
To be developed.
5.3 Portable bladder scanner use procedure (CUBEscan 700 and 900)
5.3.1 Aim
To provide colleagues with best practice guidelines for performing ultrasound bladder scans.
Ultrasound bladder scanning is a non-invasive procedure that measures urinary bladder volume. Bladder scanning should be used in preference to using an indwelling catheter to measure urinary residuals on the grounds of acceptability and low incidence of adverse effects (National Institute for Health and Care Excellence clinical guidance 97 2015).
Appropriate and timely use of the scanner can prevent unnecessary catheterisation, assist in the managing of incontinence and help diagnose urinary and bladder dysfunction.
5.3.2 Scope
This procedure applies to all Doncaster care group colleagues, whether in a direct or indirect patient care role.
Adherence to the procedure is the responsibility of all Doncaster care group trust colleagues, including agency, locum, and bank colleagues.
For Rotherham and North Lincolnshire colleagues should refer to your local guidelines.
5.3.3 Procedure
The bladder scanner will only be used by a trained healthcare practitioner, for example, qualified nurse, health care assistants within the specialist continence service and by some healthcare assistants on in-patient wards who have received training and are competent in the procedure. Outcome of bladder scan results should be recorded within the patients record on SystmOne.
5.3.3.1 Clinical indications for use of bladder scanner
- To check for retention of urine, if symptoms suggest incomplete bladder emptying.
- To check for retention of urine prior to commencing anticholinergic therapy. Residuals over 100mls should not be commenced on anticholinergic therapy.
- To monitor urine output in those patients commenced on anticholinergic therapy to ensure bladder function has not been compromised.
- Assessing the degree of retention before catheterisation.
- Assessing volume of urine in bladder if catheter appears to be blocked or not draining.
- After a trial without catheter, evaluation of whether a patient is able to void and to what degree.
- Patients with neurogenic bladder should have regular bladder scanning to monitor residual urine, for example, for patients with progressive multiple sclerosis.
- Intermittent self-catheterisation training aid.
- Biofeedback mechanisms.
- Aid bladder retraining.
5.3.3.2 Urinary retention
Urinary retention can occur for a variety of reasons including:
- a physical or neurological impediment which obstructs the flow of urine or prevents the detrusor muscle from effective contraction
- effects of medication including anticholinergic drugs, opiates and epidural analgesia
- psychological effects
- functional ability, for example, not being able to sit on the toilet properly to empty properly
- effects of surgery
5.3.3.3 Signs and symptoms of urinary retention
- Hesitancy.
- Nocturia.
- Straining to void.
- Sensation of incomplete emptying of the bladder.
- Post micturition dribble.
- Urinary tract Infection.
- Prostatic symptoms.
- Palpable bladder.
- Frequency.
- Urgency.
- Dysuria.
5.3.3.4 Contraindications for use
- If the patient has a wound where the scanner head would usually be placed.
- If the patient withholds consent.
5.3.3.5 False readings
- Anxiety about the procedure.
- Foley catheter.
- Intravesical mass.
- Obesity.
- Fluid filled cyst.
- Patient on their side during the procedure.
- Pregnancy.
- Volumes over 1000mls.
- Volumes under 100mls.
- Anatomical anomalies.
5.3.3.6 Care of the CUBEscan 700 and 900
- Storage, the scanner will be stored in the supplied case in a cool dry place. It is especially important to protect the probe head.
- Handling, always rest the probe on the rubber part of the handle.
- Cleaning of the scanner and the probe, the scanner and probe must be cleaned in accordance with both manufacturers’ guidelines and in line with infection prevention and control recommended practice which is Clinell wipes.
- Each locality will have a designated base for their bladder scanner. This base is to have a designated member of staff who will be responsible for ensuring the maintenance of the scanner is carried out according to the maintenance contract. When the scanner is due for calibration, or if the scanner is not working properly contact the continence health advisory service who will arrange the bladder scanner to be serviced.
The bladder scanners CUBEscan 900s will be annually serviced by De Smit Medical.
The CUBEscan 700 and 900s has a built-in battery, when the unit is on charge the green and orange lights signal the battery is having a bulk charge to increase the batter’s capacity fast. Once the orange light has gone out it is important to keep the scanner on charge for a further 2 hours as the battery will still be charging but at a slower rate (green light permanently on). Should the battery appear to lose its charge quickly then operate the bladder scan by the mains and when possible, charge the unit overnight.
- Ensure the printer paper is loaded properly in the scanner.
- A supply of cleaning wipes and ultrasound gel should be kept with the scanner.
- All manufacturer’s instructions must be adhered to and care taken to prevent damage to the equipment. Should any part of the equipment be damaged, this should be reported immediately.
- Please note that in transit the temperature may fall, and the scanner can become too cold. If the unit does not switch on after holding the power button down for two seconds or the screen flickers put the scanner in a warm environment for approximately 30 minutes before retrying.
5.3.3.7 Methods
There are four accepted methods of carrying out the scan procedure (Addison 2000).
- A bladder scan is performed before and after voiding to assess the residual volume
- The patient is asked to void, and then a scan is taken within 10 minutes
- The bladder scan is performed first and if any urine is present the patient is asked to void into a jug which is then measured. The difference between the volume in the bladder according to the scan and the volume of the voided urine gives the residual volume
- The patient is given large amounts of fluid to drink. When they experience the urge to void a scan is taken. The patient is then asked to void. After voiding a second scan is taken to give the post void residual
5.3.3.8 Performing the procedure
The steps for performing bladder scanning are as follows:
- explain the procedure to the patient and gain consent
- ensure privacy
- decontaminate hands
- assemble the bladder scanner according to the manufacturer’s instructions, switch the scan on and set the scanner for the appropriate gender or condition
- assist the patient into a supine position with head raised
- adjust clothing to expose the lower abdomen
- place an ample quantity of ultrasound gel on the probe head. Palpate the patient’s pubic bone and place the probe midline on the patient’s abdomen, approximately one inch (3 fingers above the pubic bone)
- standing at the patient’s right side, place the probe on the gel and aim towards the expected location of the bladder. For most people this means tilting the probe slightly towards the patient’s coccyx
- press the “SCAN” button located on the probe. As the scan progresses, sections of the bladder will appear on the console screen. When you hear the end-tone, the scan is complete. When you have 3 consistent readings and a clear image through scanner press print or take a photo of the scan image and results and download into the patients electronic record
- at the end of the procedure the scanner head should be wiped free of gel and cleaned with a wipe as per infection prevention and control (IPC) manual
- remove the remaining gel from the patient’s abdomen using wipes and allow the patient to redress
- ensure all waste is disposed of in line with waste policy
- decontaminate hands
- explain the results to the patient
- if bladder contains a residual of urine under 200mls, teach bladder emptying techniques. If residual greater than 200ml, check urea and electrolytes and rescan in 7 days. If residual remains above 200mls contact specialist continence service or urology for further advice (see appendix C flow chart for bladder scanning)
5.3.4 Training implications
5.3.4.1 Community nurses, planned or unplanned qualified care home colleagues, qualified colleagues at Tickhill Road Hospital
- How often should this be undertaken: every other year.
- Length of training: half day.
- Delivery method: presentation practical.
- Training delivered by whom: specialist continence sisters.
- Where are the records of attendance held: electronic colleague record system (ESR).
5.4 Bladder washouts
To be developed.
5.5 Bowel care procedures
To be developed.
5.6 Catheter maintenance procedure
To provide colleagues with best practice guidelines for performing catheter maintenance.
5.6.1 Scope
This procedure applies to all colleagues, whether in a direct or indirect patient care role.
Adherence to the procedure is the responsibility of all trust colleagues, including NHS Professionals (NHSP) working in both the Doncaster mental health care group and Doncaster physical health and neurodiversity care group of the trust who deliver and provide continence or catheter care to adult patients over the age of 18. For colleagues working in Rotherham and Scunthorpe, they will need to refer to their local guidelines.
5.6.2 Procedure
5.6.2.1 Catheter maintenance
When considering catheter maintenance, there must be clear evidence to suggest that the patient may benefit from planned use of catheter maintenance solution to extend the life of the urinary catheter, or prior to removal of a urinary catheter to dissolve crystal formation to prevent trauma. Therefore, it is essential that the catheter history is clearly documented inpatient clinical record.
Please see appendix F for the flow chart for the management of blocked catheters.
5.6.2.2 Catheter maintenance solution
Catheter maintenance solution must only be used when all other options have been considered.
For catheters that regularly block due to encrustation, try to establish the life of 3 catheters. This will establish a clear pattern. Once the pattern has been established and a clear treatment plan has been written, the use of the appropriate catheter maintenance solution and planned catheter changes can be adopted.
Best practice in the treatment of encrustation is to use two solutions. Current research supports the use of two sequential instillations of a small volume are more effective at dissolving encrustation (Getliffe, et al. 2000). B-Braun Uro-Tainer Twin, has two chambers of 30mls solution, each chamber is instilled for 5 minutes and therefore you are only breaking the closed drainage system the once. Alternative solutions would therefore mean that you would have to break the closed drainage system twice to instil two solutions. By limiting the number of times that the closed drainage system is broken, reduces the risk of introducing infection.
Catheter maintenance in end-of-life patients:
- if able to determine the cause of a blocked catheter, use the appropriate catheter maintenance solution, Suby-G for encrustation and PHMB for debris or mucus
- if unable to determine cause of the catheter blockage, to administer PHMB twice per week and review (catheter maintenance solution can be administered up to twice per day if required)
If performing catheter maintenance more than once per week, use a Linc medical, bladder infusion kit (BIK).
If Suby-G is being used daily, please consider changing to the Solutio-R catheter maintenance and reduce the frequency of instillation.
Please see appendix G on how to administer catheter maintenance solution.
5.7 Catheter trouble shooting
To be developed.
5.8 Continence products home delivery purchase
5.8.1 Aim
The aim of this procedure is to provide staff with the information required when patients require products for continence.
5.8.2 Scope
This procedure applies to all staff, whether in a direct or indirect patient care role who deliver continence care to adult patients in Doncaster care group.
Adherence to the procedure is the responsibility of all trust staff, including agency, locum and bank staff.
5.8.3 Procedure
5.8.3.1 Home delivery of continence products
Doncaster specialist continence service (SCS) offers a comprehensive service based on the principle of individual assessment. Following this assessment and if conservative treatments have failed, then an assessment of disposable or reusable continence products will be undertaken.
5.8.3.2 Eligibility to receive provision of body worn incontinence products
The specialist continence service has overall responsibility for the provision and supply of continence products, following an assessment by health care professionals and an annual reassessment
5.8.3.3 Provision criteria
- Incontinence can be managed by a comprehensive range of products and pads should only be supplied in accordance with the continence provision guide.
- Products are only provided after a comprehensive assessment and pad weighing, such as two-piece system, wraparound, and belted. This will objectively assess the degree of incontinence and therefore enable the health care professional to prescribe products that will meet the patient’s needs. Alternative collection devices must be considered for example, prescription urinals, urinary sheaths and body worn urinals, bags, and adaptive underwear (for example, specialist briefs with adapted collection systems).
- Annual reassessments of a patient’s symptoms.
- Absorbent products should not be supplied for treatable medical conditions (or for bodily fluids other than urine or poo).
- The custom and practice of automatically providing products to adults (including those with an acknowledged disability) is not appropriate and could be considered discriminatory.
- If an individual is assessed to have capacity and declines treatment, provision of products will not be offered as an alternative (an exception will be end of life).
5.8.3.4 Continence product provision
- Patient’s that have a pad weight of less than 400mls will not be eligible for products.
- Maximum of 4 disposable pads in 24 hours will be prescribed. However, if following a pad weigh individual results indicate a need for an increase in products this will be discussed with the specialist continence service clinical team lead on an individual basis.
- Patients receiving the shaped range of products will be supplied with 5 pairs of fixation pants every 6 months. Individual cases will be reviewed should the need arise for more frequent replacement be identified.
- All-in-one products will only be provided to patients with a severe physical or mental impairment or for patients with profuse diarrhoea. Existing patients will continue to receive their current allocation of supplies.
- Disposable pull up pants are available on prescription, a maximum of 2 pairs, per day, dependent on clinical need and following a multidisciplinary team (MDT) within specialist continence service.
- Two washable absorbent bed sheets to be supplied every 12 months. For patients on an airwave mattress, they can be prescribed kylie sheets or pad and pants not both. Following guidance from the tissue viability specialist nurse kylie sheets can be used on air wave mattresses if they are not tucked in.
- Where appropriate a combination of reusable and disposable products for daytime and night-time may be provided at the discretion of the specialist continence service clinical team lead, maximum of 3 disposable pads and 2 washable bed sheets. Again, this is based on individual need
- Pad weigh has now become part of the continence assessment as incontinence is not easy to quantify. The Urodynamic Society (1997) have looked at recent research and evidence and now recommend the use of pad weighing as an objective assessment to record urine loss. Using this tool will clearly identify a patient’s level of incontinence and will ensure the most suitable product to be prescribed (see appendix Q pad weighing instructions)
- Patients and their carers will be offered practical support, advice and a choice of appropriate products for coping with symptoms during the period of assessment and for as long as they experience episodes of faecal incontinence. Pads in quantities sufficient for the individual’s continence needs will be prescribed (NICE 2007, 2014).
- Once assessed and products prescribed, all patients will have an annual phone reassessment.
5.8.3.5 Rapid response
Community nursing staff attending end-of-life (EOL) patients or patients in a crisis situation who requires an emergency supply of continence products will have access to a supply of continence products to meet patient needs. End of life packs are located at each community nurse base
The patient will be given 3 days’ supply of products. The community nurse will complete the fast-track prescription form, located on SystmOne under communications and letters, indicating that the patient is either end-of-life or in a crisis situation and that the patient has been given continence products (including the amount supplied from stock) to use prior to the 24-hour delivery.
Community nursing services must update the log sheet within the product store in order to evidence the management of stock levels and the appropriate use of products to meet the needs of end-of-life patients.
The ordering of all continence products will be carried out by specialist continence service administration colleagues through the information provided on the fast-track prescription form.
5.8.3.5 Self-care
A despatch note will be attached inside the delivery box. The despatch note contains the call back number and the date the next delivery will be available.
Self-care is designed for re-activating deliveries only and cannot be used to bring a delivery forward or to change the type or number of products prescribed. If patients try to do this, housebound patients will be advised to contact the specialist continence service as a reassessment may be needed.
Continence products will be supplied every 12 weeks to community patients. All community patients must call Essity to activate their next order.
5.8.3.6 Transition from children’s continence service
Once a child reaches the age of 19, they will be transferred from the children’s continence service into the specialist continence service. To ensure that the transition is a smooth and seamless process, the patient and their parents or carers will be made aware of what to expect during the transition period by the children’s continence service. Once the patient has received their last prescription order by the children’s continence service, arrangements will be made for the patient to be assessed by an adult specialist continence nurse. The Children’s continence team will refer over to the adult service when the patient is 17 years and 11 months of age to allow time for the adult service to allocate the initial assessment within their service.
Following the assessment, a pad weigh will be performed, and the most appropriate products prescribed to meet the young person’s needs. The specialist continence service will aim to ensure that a delivery of products will be delivered in line with their 12 weekly delivery cycle so that there are no gaps in service.
5.8.3.7 Nursing, residential and learning disabilities care homes
Care home deliveries are every 12 weeks. Care home deliveries are activated once the care home delivery order form has been sent to the specialist continence service from the relevant home. This form includes a list of patient’s names that need their next delivery, any reasons for suspension for example, patient death, catheterised or improved needs to be documented. This form will only be accepted if the signature of the care home staff placing the order is eligible.
It is the home’s responsibility to ensure that all patients who are on the home delivery service are added to the delivery form. Once the order has been activated and processed no changes can be made to the order. However, if there has been a problem with the delivery, they must contact specialist continence service within 48 hours. After this time Essity will not be able to deal with any discrepancies.
Patients who take up temporary residency in another area within England and Scotland or another country should be placed on a temporary stop. If patients do not activate their order for a year, then they will automatically be removed from the home delivery service. After this time the patient will need to be referred back into specialist continence service to have a full continence assessment and pad weigh.
5.8.3.8 Inpatient services
Pad use is based on individual holistic assessment and selection of the right product, if required. To maintain continuity of care, each ward will stock a core range.
Should continence symptoms become apparent during an inpatient stay, then a full continence assessment should be undertaken in order to ensure the most appropriate product is used.
On discharge, a referral should be made to the specialist continence service for a continence assessment, if required a supply of 7 day supply of body worn products should also be provided.
5.8.3.9 Annual reassessments
On an annual basis, all the house-bound patients will be reassessed by the community nursing teams, while non-house bound patients will continue to be reassessed by the specialist continence service. Patients will be sent a reassessment letter advising them to contact the specialist continence service within 14 days so that a review of their needs and associated products can be completed. Any patient that do not contact the specialist continence service within 14 days of receipt of the letter, will be sent another reminder informing them that if they fail to contact the service within the next 14 days then their products will be suspended until a reassessment is performed. Once products have been suspended a re-referral to specialist continence service will be required.
If a patient refuses to have a yearly reassessment, then their products will be suspended until a reassessment is carried out.
Following reassessment patients who have been identified as having deterioration in symptoms must undergo a further pad weigh, to objectively assess the degree of incontinence so that the correct product can be prescribed to meet their clinical need. The pad weigh will be carried out at the patient’s home by a member of the specialist continence service or community nursing service.
5.9 Continence assessment, treatments and provision of pads
To be developed.
5.10 Female catheterisation and removal procedure
5.10.1 Aim
To provide colleagues with best practice guidelines for performing female catheterisation.
5.10.2 Scope
This procedure applies to all clinical colleagues working in both the Doncaster mental health care group and Doncaster physical health care group of the trust who deliver and provide continence and catheter care to adult patients over the age of 18. For colleagues working in Rotherham and Scunthorpe, they will need to refer to their local guidelines.
It is recognised that primary care practitioners are also part of the organisation and as such this policy is offered for use by them to adapt to their own practices and organisations as appropriate.
The author of the policy is available to offer help and support to primary care practitioners who wish to use and implement this policy.
As part of good employment practice, whilst undertaking work for the trust. Agency workers are also required to abide by the trust policies and procedures, as appropriate, to ensure their health, safety and welfare.
5.10.3 Procedure
5.10.3.1 Female catheterisation
First time female catheterisation must only be performed by a qualified registered general nurse including nurse associate or non-registered healthcare professional who is required to undertake catheterisation as part of their role and has had catheter training.
Catheters should only be used after all alternatives have been considered. Therefore, it is essential that a urethral catheterisation assessment is performed before carrying out the catheterisation procedure. Reason for catheterisation must be clearly documented within the catheter integrated pathway of care (IPOC) within SystmOne and catheter passport. Please refer to appendix H for urethral catheterisation assessment guidance.
5.10.3.2 Risk of catheterisation
Using any form of catheterisation has associated risks. Therefore it is essential that a risk assessment is an integral part of catheter care. Please refer to appendix I for risk assessment.
5.10.3.3 Choice of catheter and catheter equipment
Female patients are usually catheterised with a standard-length catheter first, however the patient may then choose to have a female length catheter for discretion and comfort.
Choice of catheter and equipment used must be clearly documented within the catheter integrated pathway of care within SystmOne and catheter passport.
Please refer to appendix J for choice of Catheter and equipment.
5.10.3.4 Female re-catheterisation
Band 3 healthcare assistants who have attended the female re-catheterisation study day provided by the specialist continence service and have completed the relevant clinical skills package may perform simple female re-catheterisation on uncomplicated female patients who have been assessed by qualified nurse.
5.10.3.5 How to perform female catheterisation
Please see Royal Marsden manual female urinary catheterisation.
5.10.3.6 How to remove a catheter
Please see Royal Marsden manual urinary catheter removal.
5.10.3.7 Documentation
The catheter integrated pathway of care (IPOC) found within SystmOne provides a framework for best practice and follows Royal College of Nursing (RCN) guidelines for nurses on catheter care (2021). The integrated pathway of care supports the assessment process and should be followed by the healthcare practitioner to meet all the clinical and legal requirements for record keeping.
Each individual patient or carers should be given a “my catheter passport document”. This document provides the patient with written information about their catheter management (please see appendix P).
There are 2 distinct sections within the passport, patient and clinical. The patient section supports effective care of the catheter in order to reduce the risk of infection and the clinical section includes essential information around the catheterisation itself and should contain the plan of care, reason for catheterisation and plans for trial without catheter. There is also a catheter maintenance section which can be completed by the health care professional, carer or patient themselves.
5.11 Intermittent catheterisation procedure
5.11.1 Aim
To provide staff with best practice guidelines for performing intermittent catheterisation.
5.11.2 Scope
This procedure applies to all clinical colleagues including NHS Professional colleagues working within Doncaster in the trust who deliver and provide continence or catheter care to adult patients over the age of 18. For colleagues working in Rotherham and Scunthorpe, they will need to refer to their local guidelines.
It is recognised that primary care practitioners are also part of the organisation and as such this procedure is offered for use by them to adapt to their own practices and organisations as appropriate.
The author of the procedure is available to offer help and support to primary care practitioners who wish to use and implement this policy.
As part of good employment practice, whilst undertaking work for the trust.
5.11.3 Procedure
5.11.3.1 Intermittent catheterisation
Intermittent catheterisation should always be considered for incomplete emptying as a first option rather than indwelling catheterisation (HTG753 Intermittent urethral catheters for chronic incomplete bladder emptying in adults: late-stage assessment National Institute for Health and Care Excellence 2025), providing this is a safe and acceptable alternative for the individual and carers. It can be used as treatment for voiding problems due to disturbances or injuries to the nervous system, non-neurogenic bladder or obstruction with incomplete emptying.
It is therefore essential that a urethral catheterisation assessment is performed before carrying out the catheter procedure. Reason for catheterisation must be clearly documented within the catheter integrated pathway of care (IPOC) within the patient electronic record in SystmOne and catheter passport. Please refer to appendix H for urethral catheterisation assessment guidance.
5.11.3.2 Female re-catheterisation
Band 3 healthcare assistants who have attended the female catheterisation study day provided by the specialist continence service and have completed the relevant clinical skills package may perform simple female re-catheterisation with an intermittent catheter on uncomplicated female patients who have been assessed by a registered nurse.
5.11.3.3 Risk of catheterisation
Using any form of catheterisation has associated risks. Therefore, it is essential that a risk assessment is an integral part of catheter care. Please refer to appendix I for risk assessment.
Though intermittent catheterisation has a reduced infection rate when compared to indwelling catheters, there is still a risk.
Intermittent catheterisation should not be commenced solely on the residual urine. Before commencing a patient on intermittent catheterisation, their symptom severity, renal function, risk assessment, psychological and physical ability to perform intermittent catheterisation and residual urine must be considered.
5.11.3.4 Catheter choice
Male patients can only be catheterised with a standard length. The choice of catheter and equipment used should be clearly documented within the catheter integrated pathway of care within SystmOne and catheter passport.
Please refer to appendix J for choice of catheter and equipment.
5.11.3.5 Teaching intermittent self-catheterisation (ISC)
For further advice on patients performing intermittent self-catheterisation contact the specialist continence service who will carry out a full assessment and the patient’s ability to manage the procedure. It should also be noted with the patient’s consent a carer or spouse can be taught to perform intermittent self-catheterisation.
5.11.3.6 Frequency
The frequency and continued usage of intermittent catheterisation is based on the following:
- symptom severity improvement
- quality of life and lifestyle indicators
- volumes drained related to times of urinary output (please refer to appendix L for frequency guide)
- clinical requirement
- renal function
Intermittent catheterisation may need to be increased during periods of urinary tract infections.
For further advice regarding frequency and continued usage of intermittent catheterisation, please contact the specialist continence service.
5.11.3.7 12-month review
All patients who perform intermittent self-catheterisation will be reviewed every 12 months by the specialist continence service.
5.11.3.8 Performing female intermittent catheterisation
Please refer to the Royal Marsden manual intermittent self‐catheterization patient female guidance.
5.11.3.9 Performing male intermittent catheterisation
Please refer to the Royal Marsden manual intermittent self‐catheterization patient male guidance.
5.11.3.10 Documentation
The catheter integrated pathway of care (IPOC) found within SystmOne provides a framework for best practice and follows Royal College of Nursing guidelines for nurses on catheter care (2019). The integrated pathway of care supports the assessment process and should be followed by the healthcare practitioner to meet all the clinical and legal requirements for record keeping.
Each individual patient or carers should be given the “my catheter passport document”. This document provides the patient with written information about their catheter management.
There are 2 distinct sections within the passport, patient and clinical. The patient section supports effective care of the catheter in order to reduce the risk of infection, and the clinical section includes essential information around the catheterisation itself and should contain the plan of care, reason for catheterisation and plans for trial without catheter. There is also a catheter maintenance section which can be completed by the health care professional, carer or patient themselves.
5.12 Male catheterisation and removal procedure
5.12.1 Aim
To provide staff with best practice guidelines for performing male catheterisation.
5.12.2 Scope
This procedure applies to all clinical colleagues including NHS Professional colleagues working in both the Doncaster mental health care group and Doncaster physical health care group of the trust who deliver and provide continence or catheter care to adult patients over the age of 18. For colleagues working in Rotherham and Scunthorpe, they will need to refer to their local guidelines.
It is recognised that primary care practitioners are also part of the organisation and as such this policy is offered for use by them to adapt to their own practices and organisations as appropriate.
The author of the policy is available to offer help and support to primary care practitioners who wish to use and implement this policy.
5.12.3 Procedure
5.12.3.1 Catheterisation
Catheters should only be used after all alternatives have been considered. When catheterisation is being discussed as a treatment option or intervention, intermittent catheterisation should always be considered for incomplete emptying as a first option rather than indwelling catheterisation, providing this is a safe and acceptable alternative for the individual and carers. It is therefore essential that a urethral catheterisation assessment is performed before carrying out the catheter procedure. Reason for catheterisation must be clearly documented within the catheter integrated pathway of care (IPOC) within the patient electronic record in SystmOne and catheter passport. Please refer to appendix H for urethral catheterisation assessment guidance.
5.12.3.2 Catheterisation associated risks
Using any form of catheterisation has associated risks. Therefore, it is essential that a risk assessment is an integral part of catheter care. Please refer to appendix I for risk assessment.
5.12.3.3 Catheter choice
Please refer to appendix J for choice of catheter and equipment. Male patients must only be catheterised with a standard length. The choice of catheter and equipment used must be clearly documented within the catheter integrated pathway of care within SystmOne and catheter passport.
5.12.3.4 First time male catheterisation
First time male catheterisation can only be performed in the community setting by the Unplanned Care team for acute retention only. However, for end-of-life patients if the registered nurse is competent in male catheterisation and they have attended the catheter study day and have completed the relevant scope package, they may perform catheterisation.
A first-time male catheterisation is classed as someone who has never been catheterised before or has not had a catheter in place for 2 years.
A registered nurse within the Unplanned Care team may carry out first time male catheterisation for acute retention when they have completed the management of acute painful retention In men (MAPRIM) training, completed the relevant competency package and attended the catheter study day training provided by the specialist continence service. Please refer to appendix K management of acute and chronic retention in males first time male catheterisation pathway (MAPRIM pathway).
5.12.3.5 Male re-catheterisation
A registered nurse may carry out uncomplicated male re-catheterisation when they have completed the catheterisation care and clinical skills assessment tool (competency package and attended catheter study day training provided by the specialist continence service.
5.12.3.6 Catheter clinic
Non-house bound patients with catheters can be referred to the specialist continence catheter clinic for routine catheter change.
5.12.3.7 Catheter change
Catheter change should be a planned event according to the type of catheter selected and the patient’s previous history where a catheter is already in situ. Monitoring catheter change history can establish a pattern for any recurrent problems such as encrustation leading to blockage and can allow changes to be planned prior to problems developing.
5.12.4 How to perform male catheterisation
Please refer to the Royal Marsden manual male urinary catheterisation.
After catheterisation it is essential that the health care professional performing the catheterisation ensures that the foreskin is replaced, this is to prevent paraphimosis occurring (the foreskin becomes trapped behind the glans penis and cannot be reduced). If this condition persists for several hours or there is a lack of blood flow it must be classed as a medical emergency. Please refer to the trouble shooting with catheters procedure, continence manual advise the patient or carer to use alternate legs when attaching the catheter bags each day to reduce the risk of developing a split in their meatus.
Nurses should ensure that the patient is aware of basic catheter care and how to order catheter equipment.
5.12.4.1 How to remove a catheter
Please refer to the Royal Marsden urinary catheter removal.
5.12.4.2 Documentation
The catheter integrated pathway of care (IPOC) found within SystmOne provides a framework for best practice and follows Royal College of Nursing guidelines for nurses on catheter care (2019). The integrated pathway of care supports the assessment process and should be followed by the healthcare practitioner to meet all the clinical and legal requirements for record keeping.
Each individual patient or carer should be given a “my catheter passport document”. This document provides the patient with written information about their catheter management (please see appendix Q).
There are 2 distinct sections within the passport, patient and clinical. The patient section supports effective care of the catheter in order to reduce the risk of infection, and the clinical section includes essential information around the catheterisation itself and should contain the plan of care, reason for catheterisation and plans for trial without catheter. There is also a catheter maintenance section which can be completed by the health care professional, carer or patient themselves.
5.13 Managing constipation
To be developed.
5.14 Trans anal irrigation
To be developed.
5.15 Trial without catheter procedure
5.15.1 Aim
All community trial without catheters (TWOC) will be performed by the specialist continence service. While the intermediate care should attempt to perform a trial without catheters before discharging patients’ home with a urinary catheter.
The specialist continence service will receive referrals from general practitioners and other healthcare professionals for patients requiring a trial without catheter in the community.
The rationale behind this procedure is to:
- reduce avoidable hospital readmissions
- enhance patient care
- ensure that indwelling urinary catheters are removed at the earliest and safest opportunity
5.15.2 Scope
This procedure applies to all clinical colleagues working in the trust who deliver and provide continence or catheter care to adult patients over the age of 18. For colleagues working in Rotherham and Scunthorpe, they will need to refer to their local guidelines
It is recognised that primary care practitioners are also part of the organisation and as such this policy is offered for use by them to adapt to their own practices and organisations as appropriate.
The author of the policy is available to offer help and support to primary care practitioners who wish to use and implement this policy.
Adherence to the procedures within this manual is the responsibility of all trust colleagues, including NHS Professionals (NHSP).
5.15.3 Procedure
5.15.3.1 Trial without catheter
Trial without catheter (TWOC) is the term used when a catheter has been inserted via the urethra into the bladder for drainage purposes and is removed to determine whether the patient is able to pass urine safely and spontaneously without the need for further catheterisation.
5.15.3.2 When to refer a patient to the specialist continence service for a trial without catheters
When a catheter is already being used the healthcare practitioner should consider if it is necessary. This can be established using the HOUDINI indicators which lists clinical indications when it is appropriate for the continued use of a catheter (Adams et al., 2012).
HOUDINI:
- H: haematuria, only requires catheter if in clot retention
- O: obstructed or retention
- U: urologic surgery
- D: decubitus ulcers, open sacral or perineal wound in an incontinent patient
- I: input or output, fluid monitoring
- N: not for resuscitation, end of life or comfort care
- I: immobility due to physical constraint, for example unstable fracture and inability to use bottles or bedpans
If none of the above criteria are met, please complete the trial without catheter referral form for the specialist continence service to arrange a community trial without catheter.
5.15.3.3 Exclusion criteria
- Lacks capacity to consent then a best interest decision may be appropriate after a discussion with the patients general practitioner and or identified advocate.
- Unable to measure and record fluid in and output or does not have carer support.
- Unable to or has no carer support to make contact by phone to single point of access.
5.15.3.4 Considerations
Consideration should be given to patients who present with:
- constipation, should be treated with appropriate bowel management medication prior to removal of the catheter.
- symptomatic urinary tract infection (not just positive urinalysis). Treat the infection ensuring treatment is successful before community trial without catheter.
5.15.3.5 Contraindications
- Radical prostatectomy within 3 months.
- Patients who experience significant problems with catheter insertion (require multiple attempts by a consultant or additional instrumentation to place the catheter, history of haemorrhage in previous catheterisations).
- Patients who withhold consent for trial without catheter in the community.
5.16 Urinary catheterisation aftercare procedure
5.16.1 Aim
The aim of this procedure is to provide staff with the information required to manage and care for patients with a urinary catheter.
5.16.2 Scope
This procedure applies to all clinical colleagues including NHS Professionals (NHSP) working in both the of the trust who deliver and provide continence or catheter care to adult patients over the age of 18. For colleagues working in Rotherham and Scunthorpe, they will need to refer to their local guidelines.
It is recognised that primary care practitioners are also part of the organisation and as such this policy is offered for use by them to adapt to their own practices and organisations as appropriate.
The author of the policy is available to offer help and support to primary care practitioners who wish to use and implement this policy.
5.16.3 Procedure
5.16.3.1 Patient aftercare advise
Following catheterisation patients should be given the following advice on:
- how to care for the leg bag or catheter valve (please refer to appendix J)
- how to change a leg bag (please refer to appendix M)
- how to empty a leg bag (please refer to appendix N)
- how to attach a night drainage bag (please refer to appendix O)
- catheter passport should be given and discussed
- how to order repeat prescriptions
- how to contact single point of access (SPA): if they experience any problems or concerns, phone: 03000 218 996
5.16.3.2 Collecting a catheter specimen of urine (CSU)
Dipstick testing is not an effective method for detecting urinary tract infections in catheterised adults. This is because there is no relationship between the level of pyuria and infection in people with indwelling catheters (the presence of the catheter invariably induces pyuria without the presence of infection). To ensure that urinary tract infections are diagnosed accurately and to avoid false positive results, dipstick testing must not be used (National Institute for Health and Care Excellence clinical guidance 139 (CG139)).
- Samples of urine must be obtained from a sampling port using an aseptic technique.
- Samples of urine must only be obtained when the patient is symptomatic, there should be no routine sampling.
- Never disconnect the closed system to obtain a urine specimen.
- Never collect a sample of urine from the drainage bag as this does not represent the bacteria in the bladder and could lead to over-prescribing of antibiotics.
Urine samples for microscopic culture and sensitivity must be sent in a urine primary tube (UPTs), red top containing boric acid which acts as a preservative. Refrigeration of urine is therefore rendered unnecessary, and the sample will last for at least 48 hours at room temperature without any negative effect upon the result. Urine samples for all other urine tests should still be collected in their currently used containers.
When report states “possible contamination”, it is because there are microorganisms in the sample but no white cells. White cells would be present if infection was present.
Please refer to the Royal Marsden Manual for urine sampling.
5.16.3.3 Catheter associated urinary tract infections and when to change a catheter
If the urinary catheter has been in situ for more than 7 days and the patient is about to commence antibiotics for a confirmed catheter associated urinary tract infections (CAUTI’s), if possible, change the catheter at the beginning of the course of antibiotics.
5.16.3.4 Discharge of patients from hospital
Patients that are newly catheterised and are to be discharged should be given the relevant equipment to take home.
These include:
- 1 prefilled catheter
- 1 tube of anaesthetic jelly
- 2 night bags
- 1 normal saline
- 1 dressing pack
- 2 leg bags or valves
- catheter passport
A discharge form should be completed and sent through to the single point of access. A copy should go home with the patient.
Compliance with this will ensure patients are not re-admitted with a blocked catheter before community nurses can obtain supplies. The planned care team should visit the patient as soon as possible after receiving the referral to ensure that the patient has the appropriate equipment and to identify any problems or concerns that the patient may have following discharge.
5.16.3.5 Catheter passport
Each individual patient or carer should be given a “my catheter passport document”. This document provides the patient with written information about their catheter management (please refer to appendix P).
There are 2 distinct sections within the passport, patient and clinical. The patient section supports effective care of the catheter in order to reduce the risk of infection, and the clinical section includes essential information around the catheterisation itself and should contain the plan of care, reason for catheterisation and plans for trial without catheter. There is also a catheter maintenance section which can be completed by the health care professional, carer or patient themselves.
6 Training implications
6.1 Continence care day
- Staffing groups requiring training: district nurses, qualified care home staff, qualified staff TRH.
- How often should this be undertaken: on employment every 3 years.
- Length of training: 9:30am to 4:30pm.
- Delivery method: presentation.
- Training delivered by whom: Specialist Continence Service team.
- Where are the records attendance held: electronic staff record system (ESR).
6.2 Continence awareness day
- Staffing groups requiring training: healthcare assistants, care home care assistance, home carers (Doncaster Metropolitan Borough Council, Age Concern and other private agencies).
- How often should this be undertaken: on employment every 3 years.
- Length of training: 9:30am to 4:30pm.
- Delivery method: presentation.
- Training delivered by whom: Specialist Continence Service team.
- Where are the records attendance held: electronic staff record system (ESR).
6.3 Bowel care day
- Staffing groups requiring training: district nurses, qualified care home staff, qualified staff TRH.
- How often should this be undertaken: on employment every 3 years.
- Length of training: 9:30am to 4:30pm.
- Delivery method: presentation.
- Training delivered by whom: Specialist Continence Service team.
- Where are the records attendance held: electronic staff record system (ESR).
6.4 Catheter study day
- Staffing groups requiring training: district nurses, qualified care home staff, qualified staff TRH.
- How often should this be undertaken: on employment every 3 years.
- Length of training: 9:30am to 4:30pm.
- Delivery method: presentation.
- Training delivered by whom: Specialist Continence Service team.
- Where are the records attendance held: electronic staff record system (ESR).
6.5 Female re-catheterisation study day
- Staffing groups requiring training: band 3 healthcare.
- How often should this be undertaken: on employment every 3 years.
- Length of training: 9:30am to 4:30pm.
- Delivery method: presentation.
- Training delivered by whom: Specialist Continence Service team.
- Where are the records attendance held: electronic staff record system (ESR).
7 Equality impact assessment screening
To access the equality impact assessment for this policy, please email rdash.equalityanddiversity@nhs.net to request the document.
7.1 Privacy, dignity and respect
The NHS Constitution states that all patients should feel that their privacy and dignity are respected while they are in hospital. High Quality Care for All (2008), Lord Darzi’s review of the NHS, identifies the need to organise care around the individual, ‘not just clinically but in terms of dignity and respect’.
Consequently, the trust is required to articulate its intent to deliver care with privacy and dignity that treats all service users with respect. Therefore, all procedural documents will be considered, if relevant, to reflect the requirement to treat everyone with privacy, dignity, and respect, (when appropriate this should also include how same sex accommodation is provided).
7.1.1 Indicate how this will be met
Privacy, dignity and respect of the patient will be considered at all times. Sensitivity to the patient’s needs will also be addressed.
7.2 Mental Capacity Act (2005)
Central to any aspect of care delivered to adults and young people aged 16 years or over will be the consideration of the individual’s capacity to participate in the decision-making process. Consequently, no intervention should be carried out without either the individual’s informed consent, or the powers included in a legal framework, or by order of the court.
Therefore, the trust is required to make sure that all colleagues working with individuals who use our service are familiar with the provisions within the Mental Capacity Act (2005). For this reason, all procedural documents will be considered, if relevant to reflect the provisions of the Mental Capacity Act (2005) to ensure that the rights of individual are protected, and they are supported to make their own decisions where possible and that any decisions made on their behalf when they lack capacity are made in their best interests and least restrictive of their rights and freedoms.
7.2.1 Indicate how this will be achieved
All individuals involved in the implementation of this policy should do so in accordance with the guiding principles of the Mental Capacity Act 2005 (section 1). No issues have been identified.
8 Monitoring arrangements
8.1 Training compliance and following up on those who fail to attend
- How and who by: follow up in writing with relevant trainers and managers by continence sister.
- Reported to: community practice educators and managers.
- Frequency: following every study day.
8.2 Any patient feedback, complaints or your opinion counts which relate to non-compliance with the standards in this policy
- How and who by: investigation feedback and review by matrons and managers.
- Reported to: care group leadership and quality groups.
- Frequency: ongoing or as the need arises.
9 Any associated documents
- Infection prevention and control manual
- Chaperoning policy
- Personal protective equipment procedure
- Waste policy
10 References
- Addison, R. (2000) A guide to bladder ultrasound. Nursing Times Vol 96, No 40.
- British Association of Spinal Cord Injury Specialists (BASCIS), Multidisciplinary Association of Spinal Cord Injury Professionals (MASCIP), Spinal Injuries Association (SIA) 2014 Statement on Autonomic.
- Button, D. Roe, B. Webb, C. Frith, T. Colin-Thorne, D. Gardner, L. (1999), Continence Promotion and Management by the Primary Health Care Team. Consensus Guidelines. London, Whurr.
- Department of Health (2000) Good Practice in Continence Services. London, HMSO.
- Department of Health (2001a) National Service Framework for Older People. London, HMSO.
- Department of Health (2001b) Medicines and Older People. Implementing medicines related aspects of the NSF for Older People. London, Department of Health.
- Department of Health (DoH) (2001) Reference Guide to Consent to the Procedure. London, Crown
- Department of Health (DoH) (2005) Essence of care. Benchmarking for Privacy and Dignity, Record Keeping, Continence and Bladder and Bowel Care
- Department of Health (DoH) Essential Steps to Safe Clean Care (2007) Preventing the Spread of Infection
- Emmerson, AM, Enstone, JE, Griffin, M, et al. (1996) The Second National Prevalence Survey of Infection in Hospitals.
- Getliffe K and Dolman M (2000) Promoting Continence. A Clinical Research Resource. Whurr.
- Lower urinary tract symptoms in men, management (NICE 2015) (CG97.
- National Institute for Health and Care Excellence (NICE 2015) (NG123) Urinary Incontinence and pelvic organ prolapse in women: management.
- National Institute for Health and Care Excellence clinical guideline 2014 (CG49) Faecal incontinence in adults: management.
- National Institute for Heath and Care Excellence (2019).
- National Institute of Clinical Excellence, Guidance on the Management of Irritable Bowel Syndrome in Adults (2015).
- National Institute of Clinical Excellence, Infection Control: Preventing Healthcare Associated Infection in primary and community care (2012) last updated 2017.
- National Institute of Clinical Excellence, Lower Urinary Tract Symptoms in Men (2 National Institute of Clinical Excellence, Faecal Incontinence. The Management of Faecal In continence in Adults (2007) last updated 2015.
- National Institute of Clinical Excellence, Nocturnal enuresis. The Management of Nocturnal enuresis in Children and Young Adults (2010).
- National Institute of Clinical Excellence, Urinary Incontinence. The Management of Urinary Incontinence In Women. (2015) last updated 2019.
- National Patient Safety Agency 2004 Patient briefing and patient notice bowel care for patients with established spinal cord lesions.
- NHS England, Excellence in Continence Care Framework (2018) Nursing and Midwifery Council (updated 2018) The Code RCN, Catheter Care, RCN Guidance for Health Care Professionals (2019).
- NICE (2012) Infection Control: Preventing Healthcare Associated Infection in Primary and Secondary Care. National Institute of Clinical Excellence, Manchester.
- NICE (2017c) Healthcare-associated infections, prevention and control in primary and community care. National Institute for Health and Care Excellence.
- NMC (2015) Code of Professional Conduct, NMC, London.
- Pannek J, Vestwebster A (2011) Clinical utility of an antimicrobial blocking solution in patients with an indwelling catheter. Aktuelle Urology 42:51-4.
- Royal College of Nursing (2025) Catheter Care RCN Guidance for Health Care Professionals. London.
11 Appendices
11.1 Appendix A trigger questions around bladder and bowel symptoms
Is there any evidence that the patient may have a problem with their bladder or bowels?
Is there an odour in the house?
Are there any pads on show in the house?
If yes, ask the patient if they are having any problems with their “water works” or bowels.
Does it sting or burn when you pass water?
Is there blood in your water?
| Possible causes | Guidance |
|---|---|
| Infection | Urinalysis and, or MSU. Antibiotic treatment if advocated for clinic signs of infection. If repeated infection requires further investigation |
Do you leak when you cough, laugh, bend, or lift a heavy object?
| Possible causes | Guidance |
|---|---|
| Stress incontinence due too poor pelvic floor tone | Refer to the Continence Health Advisory Service |
Do you have an urgent need to use the toilet?
Do you need to use the toilet frequently?
Do you ever leak before you reach the toilet?
| Possible causes | Guidance |
|---|---|
| Unstable bladder due to medical condition, for example, MS, CVA, Post Prostatectomy. Poor fluid intake or type of fluids, infection | Bladder retraining. Advice on fluids. Refer to the GP for anticholinergic or antibiotic therapy. If no improvement in 3 months refer to continence health advisory service |
Do you only pass small amounts of water at a time?
Does your bladder still feel full after passing water?
Do you ever have to wait or strain to pass water?
Is your flow weak?
Do you have frequent water infections?
Do you dribble continuously, or after passing water?
| Possible causes | Guidance |
|---|---|
| Incomplete emptying due to enlarge prostate, Stricture, faecal Impaction, neurogenic bladder or Spinal Injuries | Bladder scan (refer to bladder scan flow chart) aids and appliances. Clear impaction. Bladder stimulation, intermittent self-catheterisation, refer to continence, take urea and electrolytes if residual volume greater than 200mls |
Have sudden wetness without warning?
Are you ever unaware that you have been incontinent?
| Possible causes | Guidance |
|---|---|
| Passive incontinence due to mental impairment, dementia or confusion | Habit retraining. Aids and appliances. Adapt the environment. Prompting, toilet programme |
Do you wet the bed?
| Possible causes | Guidance |
|---|---|
| Nocturnal enuresis due to vasopressin deficiency. Over active bladder | Review fluid intake. Review of caffeine intake. Desmopressin, bladder retraining, intermittent self-catheterisation, anticholinergic community only-referral to laundry services |
Do you have problems with mobility resulting in incontinence?
Do you have problems with dexterity resulting in incontinence?
Do Your present facilities cause or contribute to your incontinence?
Do you need to be reminded to go to the toilet to prevent incontinence?
| Possible causes | Guidance |
|---|---|
| Functional incontinence due to underlying clinical or environmental problems | Adapt the environment or clothing. Prompting toileting. Refer to Occupational therapist and physiotherapist |
Do you suffer constipation?
| Possible causes | Guidance |
|---|---|
| High fibre intake, low fluid intake, medication check fluid intake, review fibre intake, review medication | Speak with GP regarding soft laxative. Complete stool chart. No changes in 4 weeks refer to continence health advisory service |
Do you suffer from loose stools?
| Possible causes | Guidance |
|---|---|
| Infection, constipation, over use of laxatives, query bowel disorders, for example, IBS, diverticular disease etc. | Send stool sample. Review medication, Query overflow. Fibre intake. Stool chart. Refer to continence health advisory service |
11.2 Appendix B continence health advisory service referral form
Refer to appendix B: continence health advisory service referral form (staff access only).
11.3 Appendix C flow chart for bladder scanning
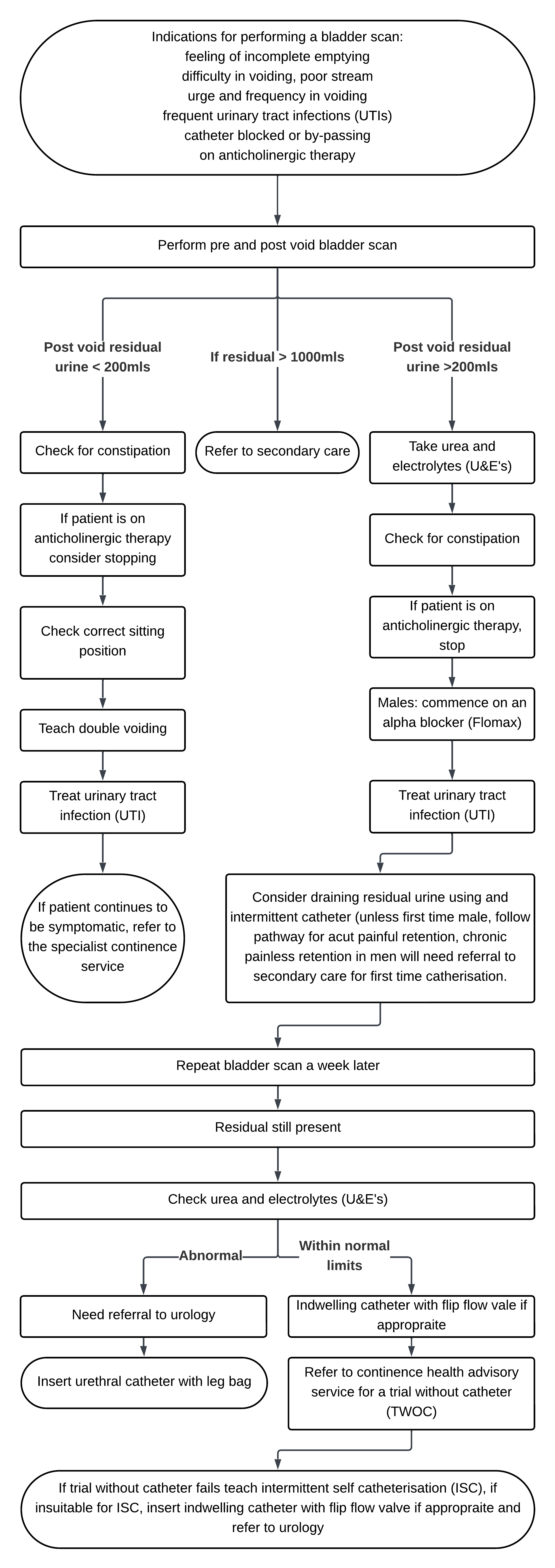
Indications for performing a bladder scan:
- feeling of incomplete emptying
- difficulty in voiding, poor stream
- urge and frequency in voiding
- frequent urinary tract infections (UTIs)
- catheter blocked or by-passing
- on anticholinergic therapy
Perform pre-void bladder scan and post-void bladder scan.
11.3.1 Post void residual urine less than 200mls
- Check for constipation.
- If patient is on anticholinergic therapy, consider stopping. Check correct sitting position. Teach double voiding. Treat urinary tract infection (UTI).
- If patient continues to be symptomatic, refer to the specialist continence service.
11.3.2 Residual greater than 1000mls
Refer to secondary care.
11.3.3 Post void residual urine less than 200mls
- Take urea and electrolytes (U&E’s). Check for constipation. If patient is on an anticholinergic therapy, stop. Males-Commence on an alpha blocker (Flomax). Treat urinary tract infection (UTI).
- Consider draining residual urine using an intermittent catheter (unless first time male, follow pathway for acute painful retention, chronic painless retention in men will need referral to secondary care for first time catheterisation).
- If no urine drained, female patients would need referral to gynaecology GP to arrange ultrasound scan.
- Repeat bladder scan a week later.
- Residual still present.
- Check urea and electrolytes (U&E’s).
11.3.3.1 If abnormal
- Needs referral to urology.
- Insert urethral catheter with leg bag.
11.3.3.2 If within normal limits
- If within normal limits indwelling catheter with flip flow valve (if appropriate).
- Refer to the continence health advisory service for a trial without catheter (TWOC).
- Continence health advisory service, if trial without catheter fails teach intermittent self-catheterisation (ISC), if unsuitable for intermittent self-catheterisation, insert indwelling catheter with flip flow valve (if appropriate) and refer to urology.
11.4 Appendix D trial without catheter procedure
11.4.1 On referral
Phone the patient to introduce the specialist continence service and assess their understanding of a trial without catheter.
If a urinary tract infection is present and the patient is on antibiotics, ensure treatment is successful before arranging the trial without catheter (TWOC).
If patient has been discharged from hospital, check to see if patient is known to the Planned Care team for basic catheter care. If not, arrange for a home visit by a continence nurse the following day to discuss basic catheter care, give a catheter passport if this has not been sent home with the patient, to order appropriate catheter equipment and to commence pre-trial without catheter assessment.
Ask if the patient is using a catheter valve or a leg bag.
Check patient is not constipated, if the patient is constipated, give advice and follow up within 7 days.
Add patient to the triage waiting list and explain that a nurse will be in touch as soon as possible to arrange an appointment.
Provide single point of access (SPA) number for unplanned care team and specialist continence service for support prior to trial without catheter first time male catheterisation for acute retention referral The trial without catheter needs to be performed within 7 working days. Provisionally book the patient in and add to the triage trial without catheter waiting list as a priority and notify the triage trial without catheter nurse. If the patient is not on an alpha blocker, for example, tamsulosin 400mcg at night, inform the patient that the continence sister will be writing to the GP for a prescription to be commenced 48 hours before the trial without catheter. Advise the patient that they will need to contact their GP practice in 2 working days to follow up on the prescription request.
11.4.2 Trial without catheter triage process
Check urea and electrolytes (U&E’s) for most recent results. If no recent urea and electrolytes result available arrange a blood test for urea and electrolytes. If urea and electrolytes results deranged seek advice from urology. First time male catheterisation, deranged urea and electrolytes repeat in one week and delay trial without catheter. If urea and electrolytes are within acceptable range, trial without catheter should be performed within 7 working days. Referrals from accident and emergency via urology, trial without catheter’s should be performed within 14 working days.
If patient has been catheterised in accident and emergency and no referral has been received from urology, confirm with urology that the patient is safe for a community trial without catheter to take place. If unable to discuss on the phone schedule a home visit to explain the procedure and complete a trial without catheter pre assessment.
Contact the patient and discuss the trial without catheter process and obtain verbal consent.
Discuss potential risks, and if trial without catheter is unsuccessful the potential for re-catheterisation.
If patient has a catheter valve, explain to the patient that on the morning of the trial without catheter they will need to empty their catheter valve at 6am and then to refrain from emptying it until the nurse visits at 8am to 8:30am. The nurse will then remove that catheter and ask the patient to pass urine.
If no catheter valve fitted, and urea and electrolytes are within acceptable range, arrange a home visit for a pre-trial without catheter assessment and assessment for a catheter valve.
Male patients. If the patient is not on an alpha blocker, for example, tamsulosin 400mcg at night, inform the patient that we will be writing to the GP for a prescription to be commenced 48 hours before the trial without catheter. Advise the patient will need to contact the GP practice in 2 working days to follow up on the prescription request.
Check catheter specimen of urine (CSU) results if appropriate.
Arrange antibiotics with GP if necessary and delay trial without catheter.
Check patient is not constipated (will need to delay trial without catheter if constipated for more than 3 days) if the patient is constipated, give advice and follow up within 7 days.
Explain to male patients that if the trial without catheter is successful, they will be offered an appointment at 2 weeks in the lower urinary tract clinic for a further review and assessment, this will include assessment of prostate.
11.4.3 Pre-trial without catheter assessment and first visit
Assess suitability for a catheter valve if required. If the patient has the dexterity and the mental capacity to use a catheter valve, change the catheter bag to a catheter valve.
Complete a falls assessment if required.
Consider toilet access for day of the trial without catheter, is a urinal required?
Consider HOUDINI assessment for suitability of a catheter.
Check medication to ensure that those on diuretics are aware of the need to take medication on the morning of the trial without catheter.
Check patient is not constipated (will need to delay trial without catheter if constipated for more than 3 days) if the patient is constipated, give advice and follow up within 7 days.
Discussed trial without catheter process and obtain verbal consent from the patient.
Advise patient that they may need to purchase some small pads for during the day of the trial without catheter.
Discuss basic catheter care and order appropriate equipment.
Assess to see if the patient will require a full continence assessment if the trial without catheter is successful.
11.4.4 Morning of the trial without catheter between 8am to 8:30am
Visit patient as planned.
Assess patient, explain procedure, discuss potential risks and ensure the patient has the contact information for single point of access should they have any problems or concerns during the procedure.
Discuss symptom diary and explain the importance of measuring and recording fluid intake or output during the day. Provide disposable measuring jug if required.
Only remove catheter if no clinical signs or symptoms of infection, for example, pain or fever and that the patient has given verbal consent to have the catheter removed.
Explain to the patient that the first void may sting, and they may notice a small amount of blood in their urine, this is due to the trauma from removing the catheter.
Ensure spare equipment is available to facilitate re-catheterisation if required.
If patient has a catheter valve, ask patient when they last emptied the catheter.
Remove the catheter using aseptic non touch technique and document in catheter integrated pathway of care within SystmOne.
If the patient has a catheter valve, ask the patient to void straight after removal, and perform immediate post void bladder scan.
Explain signs and symptoms of urinary retention and ensure the patient has single point of access number.
Instruct the patient to drink one 200mls cup or glass of recommended fluid each hour and to complete Fluid input and output chart.
11.4.5 1pm (5 hours after trial without catheter)
Visit the patient as planned, check:
- patient has no discomfort
- has passed urine since catheter was removed
- check fluid input and output chart to ensure patient has been drinking the recommended amounts
Perform bladder scan.
If no concerns revisit at 3pm.
If concerns, follow process 7 and 8 if at any time the patient becomes uncomfortable and is unable to void consider teaching intermittent self-catheterisation (ISC) or consider an indwelling catheter if intermittent self-catheterisation is not appropriate 7.
11.4.6 3pm
Visit the patient as planned, check patient has no discomfort and has passed urine since catheter was removed, check fluid input and output chart to ensure patient has been drinking the recommended amounts.
Perform bladder scan.
| Amount | Volume | Trial without catheter |
|---|---|---|
| Less than | 100mls | Trial without catheter successful advise patient on signs of retention and when to seek medical advice. Male patients, advise that they will receive a follow-up appointment in 2 weeks at the lower urinary tract clinic for men if they are not housebound. A letter to their GP will be sent asking for a prostate examination to be performed. Housebound male patients will be followed up at 2 weeks at home Female patients will be followed up at 6 weeks add to the successful trial without catheter list for review. |
| Between | 100 to 300mls | If patient is asymptomatic of urinary retention, for example, has no pain or discomfort and, or has had a poor fluid intake during the trial without catheter procedure, arrange a follow-up bladder scan the next day. Discuss with band 6 for advice if required. |
| More than | 300mls | Consider teaching intermittent intermittent self-catheterisation. If inappropriate, re-catheterise with an indwelling catheter. Consider using a flip flow valve if appropriate. Add to the unsuccessful trial without catheter list for review. |
Document actions within the catheter integrated pathway of care (IPOC) on SystmOne
11.4.7 Approximately 4pm
Whatever the outcome:
Inform planned care of outcome if patient is known to them for catheter care.
Ensure equipment available to facilitate re-catheterisation.
Arrange a follow-up bladder scan the following day if indicated above.
Add patient to the appropriate waiting list, for example, successful trial without catheter or unsuccessful trial without catheter.
11.4.8 Successful trial without catheter
Female patients will be followed up at 6 weeks in either clinic or at home.
Arrange a full continence assessment if indicated.
All male patients including the first-time male catheterisation pathway management of acute painful retention in men (MAPRIM) will be followed up in the lower urinary tract (LUTS) clinic in 2 weeks, prostate examination to be performed prior to clinic appointment.
11.4.9 Unsuccessful trial without catheter
If trial without catheter is unsuccessful, trial without catheter to be repeated in 2 weeks.
If second trial without catheter fails, the triage trial without catheter nurse will consider referral to be made to urology.
11.5 Appendix E trial without catheter procedure hospital wards
11.5.1 Protocol for community hospital wards performing a trial without catheter
Prior to discharge a patient with an indwelling urethral catheter should have trial without catheter (TWOC) preformed.
Results of the trial without catheter should be documented on the discharge form. If unsuccessful, results should be documented within the patient’s catheter passport and the catheter integrated pathway of care (IPOC) on SystmOne as well.
11.5.2 Pre-trial without catheter assessment
Consider Houdini assessment for suitability for an indwelling catheter.
Check urea and electrolytes (U&E’s) for most recent results. If no recent urea and electrolytes result available arrange a blood test for urea and electrolytes. If urea and electrolytes results deranged seek advice from urology.
If no catheter valve fitted, and urea and electrolytes are within acceptable range, assess suitability for a catheter valve. If the patient has the dexterity and the mental capacity to use a catheter valve, change the catheter bag to a catheter valve.
Male patients, if the patient is not on an alpha blocker, for example, tamsulosin 400mcg at night, inform the patient that we will be writing to the GP for a prescription to be commenced 48 hours before the trial without catheter.
Check catheter specimen of urine (CSU) results if appropriate.
Arrange antibiotics with doctor if necessary and delay trial without catheter.
Check patient is not constipated (will need to delay trial without catheter if constipated for more than 3 days) if the patient is constipated, give advice and follow up 7 days.
Discuss trial without catheter process and obtain verbal consent from the patient.
11.5.3 Morning of the trial without catheter between 8am to 8:30am
Assess patient, explain procedure and discuss potential risks.
Discussed symptom diary and explain the importance of measuring and recording fluid intake or output during the day.
Only remove catheter if no clinical signs or symptoms of infection, for example, pain or fever and that the patient has given verbal consent to have the catheter removed.
Explain to the patient that the first void may sting, and they may notice a small amount of blood in their urine, this is due to the trauma from removing the catheter.
If patient has a catheter valve, ask patient when they last emptied the catheter.
Remove the catheter using aseptic non touch technique and document in catheter care record.
If the patient has a catheter valve, ask the patient to void straight after removal, and perform immediate post void bladder scan.
Instruct the patient to drink one 200mls cup or glass of recommended fluid each hour. Complete fluid input and output chart 3.
11.5.4 Midnight (4 hours after trial without catheter)
Check patient has no discomfort and has passed urine since catheter was removed, check fluid input and output chart to ensure patient has been drinking the recommended amounts.
Perform bladder scan.
If no concerns rescan at 2pm.
If concerns, follow process 7 and 8 If at any time the patient becomes uncomfortable and is unable to void consider teaching intermittent self-catheterisation (ISC) or consider an indwelling catheter if intermittent self-catheterisation is not appropriate.
11.5.5 2pm (6 hours after trial without catheter)
Check patient has no discomfort and has passed urine since catheter was removed, check fluid input and output chart to ensure patient has been drinking the recommended amounts.
Perform bladder scan.
If no concerns rescan at 2pm.
If concerns, follow process 5 and 6.
If at any time the patient becomes uncomfortable and is unable to void consider teaching intermittent self-catheterisation (ISC) or consider an indwelling catheter if intermittent self-catheterisation is not appropriate.
11.5.6 4pm (8 hours after trial without catheter)
Check patient has no discomfort and has passed urine since catheter was removed, check fluid input and output chart to ensure patient has been drinking the recommended amounts.
Perform bladder scan.
| Amount | Volume | Trial without catheter |
|---|---|---|
| Less than | 100mls | Trial without catheter successful advise patient on signs of retention and when to seek medical advice. |
| Between | 100 to 300mls | If patient is asymptomatic of urinary retention, for example, has no pain or discomfort and, or has had a poor fluid intake during the trial without catheter procedure, arrange a follow-up bladder scan the next day. |
| More than | 300mls | Consider teaching intermittent self catheterisation. If inappropriate, re-catheterise with an indwelling catheter. Consider using a flip flow valve if appropriate. |
Document outcome within the catheter trial without catheter on SystmOne.
11.5.7 On Discharge
Ensure results of the trial without catheter are clearly documented on the discharge form and within the catheter integrated pathway of care on SystmOne including reason for catheterisation.
If unsuccessful trial without catheter, ensure a catheter passport is completed and given to the patient. A referral to the specialist continence service should be made for a follow-up and a second trial without catheter.
11.6 Appendix F managing blocked catheters flow chart
11.6.1 How to establish a catheter maintenance regime and how to manage blocked catheters
Catheter blocks first time.
Bladder scan to establish degree of retention.
Change catheter, document within the catheter integrated pathway of care if any encrustation, blood, mucus or debris is evident.
Catheter block second time, document within the catheter integrated pathway of care if any encrustation, blood, mucus or debris is evident.
Catheter block third time, document within the catheter integrated pathway of care if any encrustation, blood, mucus or debris is evident.
Once a pattern has been established, the use of an appropriate catheter maintenance solution and planned catheter change can be adopted. The effectiveness of the catheter maintenance solution may then be assessed, and the regime altered as necessary (should catheter maintenance be required more than once per week, the use of a bladder infusion kit (BIK) must be used to maintain the closed drainage system PIP or order code MC1/701. If no latex allergies, you may need to consider swapping to a short-term catheter.
Catheter maintenance in end-of-life patients:
- if able to determine the cause of a blocked catheter, use the appropriate catheter maintenance solution, Suby-G for encrustation and PHMB for debris or mucus
- if unable to determine cause of the catheter blockage, to administer PHMB twice per week and review (catheter maintenance solution can be administered up to twice per day if required)
- if performing catheter maintenance more than once per week, use a Linc medical, bladder infusion Kit (BIK)
- if Suby-G is being used daily, please consider changing to the Solutio-R catheter maintenance and reduce the frequency of instillation
11.6.2 Suby G
Treatment for encrustation, recommended for patients that are identified as a “blocker” due to encrustation. If irritation is experienced, treatment should be halted.
11.6.3 Solutio R
Recommended prior to catheter change and also for persistent “blockers”. Can be effective in clearing a catheter which is completely blocked by encrustation. Prior to catheter removal it will dissolve crystals formed in and around the catheter tip making removal less traumatic, note, Suby G should always be considered first before using the stronger solution of Solutio R.
11.6.4 Normal saline
Recommended to flush out debris and mucus, not suitable for encrustation.
11.6.5 Normal saline with polyhexamethylene biguanide (PHMB)
Recommended to flush out debris and mucus, not suitable for encrustation. Provides bacterial decolonisation of the catheter.
11.7 Appendix G how to administer catheter maintenance solution
| Action | Rationale |
|---|---|
| Explain reasons for procedure and gain consent from patient to undertake procedure | To ensure that patient is able to give informed consent |
| Ensure appropriate solution is prescribed and package is in date | To ensure patient safety |
| Ensure solution is at room temperature | To promote comfort |
| Ensure that patient is positioned comfortably, usually in a supine or sitting position in a private room | To ensure privacy or dignity is maintained |
| Decontaminate hands using alcohol hand gel or liquid soap and water or for community settings soapy hand wipes can be used followed by alcohol hand gel. Note, if in patients own home and hands are decontaminated with soap and water use only liquid soap and dry thoroughly with kitchen roll. Refer to hand hygiene procedure | Hand hygiene prior to contact with patient |
| Expose catheter site | To enable observation of any discharge or meatal problems |
| Check for allergies latex etc. | To ensure client safety |
| Open outer packaging of the solution | Content |
| Decontaminate hands with alcohol hand gel or soap and water or soapy hand wipes | To prevent cross-infection |
| Apply apron and sterile gloves and place sterile dressing field under catheter site | To prevent cross-infection |
| Disconnect drainage bag from catheter. Connect solution to catheter and instil as per manufactures instructions | To enable administration |
| Disconnect the solution and reconnect a new drainage bag with chosen method of support | To allow urine drainage |
| Dispose of equipment using appropriate waste stream | To prevent cross-infection |
| Remove and dispose of gloves and apron in the appropriate waste stream. Decontaminate hands with alcohol hand gel, soap and water or soapy hand wipes | To prevent cross-infection |
| Document procedure including reason and outcome | To meet legal requirements |
| Discuss result with patient | To involve and empower patient |
11.8 Appendix H indwelling urinary catheterisation assessment
Catheterisation is recognised as a skilled aseptic non-touch procedure that requires appropriate training and competences. When considering catheterisation nurses must follow the Royal College of Nursing (RCN) guidelines for nurses (2019) on catheter care.
| Indication | Action |
|---|---|
| Drainage |
|
| Investigations | Urodynamics x-ray investigations |
| Instillation | To irrigate the bladder For the instillation of drugs |
| Management of incontinence | For end of life patients, where catheterisation allows patients to cope with pain, frequency of micturition and maintenance of dignity facilitating continence and maintain skin integrity (when all conservative treatment methods have failed) |
11.8.1 Acute retention
Retention of urine can be acute or chronic. Chronic retention can be associated with either low or high intravesical pressure.
Acute retention:
- presents with inability to pass urine for
- several hours
- usually associated with lower abdominal
- pain
- bladder is visible and palpable
- bladder is tender on palpation
When to use with caution:
- recent urethral surgery
- unexplained haematuria
- history of false passages or strictures
- pelvic or perineal trauma-fractured pelvis
- urinary infection
11.8.2 Chronic retention
Chronic retention is usually relatively painless. High pressure chronic retention can cause hydro nephrosis and renal impairment.
Chronic retention:
- can present as late-onset enuresis
- may also present with hypertension
- low pressure chronic retention presents with symptoms of bladder outflow obstruction
- need to perform neurological examination to exclude disc prolapse
- patients with chronic retention and renal impairment need urgent urological assessment
11.8.3 Contra indications for urethral catheterisation
- Lack of consent.
- Urethral stricture or obstruction.
- Undiagnosed haematuria.
- History of difficult urethral catheterisation-including malformed genitalia.
- Previous failed attempt.
- Radical prostatectomy within 3 months.
- Mental health or cognitive status may affect the patient’s ability to give consent or cope with catheter care. Confused patients may attempt to forcibly remove the catheter which could lead to urethral trauma and infection.
- The patient may have dexterity and mobility problems which may affect the ability to manage the catheter and drainage systems. Carer availability must also be considered to undertake catheter care in these circumstances.
11.8.4 Haematuria, obstruction, urology, decubitus ulcer, input or output, nursing end of life and incontinence (HOUDINI)
When deciding if a catheter is still required, staff should consider the HOUDINI nurse led protocol which considers acceptable rationales for patients being catheterised.
- Haematuria, visible haematuria.
- Obstruction, urinary retention.
- Urology, surgery or retention.
- Decubitus ulcer, an open sacral or perineal wound in patient who is incontinent.
- Input or output, fluid monitoring, (should only be used in the acute setting).
- Nursing end of life, for comfort.
- Incontinence, only when all other alternative methods of management have been exhausted (this may include aids or intermittent self-catheterisation and discussion with the specialist continence sister.
If the answer to all of the above is “no”, then the patient should be referred to the specialist continence service for a trial without catheter as soon as possible to reduce the risks of catheter associated urinary tract infections (CAUTI’s).
The reason for catheterisation should be reviewed at each catheter intervention to see if it can be removed
11.9 Appendix I catheter risk assessment what you need to know
11.9.1 Questions to consider in catheter care
- Is the catheter in use, is it necessary? Follow HOUDINI protocol artificial.
- What type of catheter is in use? Long-term, short term, open tip, Tieman tip.
- Is a closed drainage system maintained?
- Is catheter inserted using dressing pack, catheter tray with catheter attached to the leg bag?
- Is the catheter secured to the patient’s body to prevent urethral tension?
- How secure is it? for example, Straps, fixation device.
- Is the bag below the level of the bladder? (except the belly bag).
- Is the tubing secured from the bed or chair to prevent pulling on entire system? (night bag stand).
- Is the bag hanging free without touching the floor?
- Does the patient have an individualised urinal or jug with their name on it for emptying the bag?
11.9.2 Patients where associated catheterisation infection risks may be of serious nature
- Heart valve.
- Heart defect.
- Immuno-suppressed.
- Organ transplant.
- Faecal incontinence.
- One kidney.
- Since having a catheter, the patient has had a urinary infection (high risk of further infections, potential to become resistant to).
11.9.3 Risk factors which increase the serious complications associated with catheter related infections
- The patient has been in hospital in the last 12 months, exposed to cross infection.
- The patient has taken antibiotics in the last 6 months.
- Pregnancy.
- Over 65 years of age increased vulnerability.
- Diabetes.
- More than six medications indicative of compromised health status.
- Chemotherapy within the last six months.
- Taking steroids.
- One functioning kidney, currently taking antibiotics for a urinary tract infection (UTI).
- Underlying renal tract abnormalities.
- At least one urinary tract infection since using a catheter.
- Chronic wounds requiring dressing will potentially cross-infect the catheter and drainage system.
11.9.4 Factors that could identify the risk of failing a trial without catheter in men
- Prostate.
- Previous episodes of acute episodes of retention.
- Over the age of 70 years old.
- Previous failed trial without catheter.
- Not on alpha blockers (tamusolisin).
11.9.5 Factors which identify underlying health problems
- Previous difficulty in catheter insertion and, or removal.
- History of catheter blockage.
- Catheter has fallen out.
- Bypassing.
- Patient is currently on antibiotics.
- Pain, discomfort and discharge associated with catheter usage.
11.9.6 Risks of haematuria include
- Medication such as aspirin or warfarin.
- Recent catheter related trauma.
- Recent urinary tract surgery.
- Known bladder or prostate cancer.
- Meatal bleeding observed by patient.
- Blood clots have been observed by the patient.
11.9.7 Allergy risks related to catheterisation to consider include
- Latex.
- Soap.
- Medication, for example, Lidocaine.
11.9.8 Risk factors which may increase urinary output when in supine position (important when considering flow rates or trial without catheter when patient is upright) include
- Heart disease.
- Diuretics.
- Postural oedema.
- Hypertension.
11.10 Appendix J catheter selection
| Catheter type | Advantage | Disadvantage | Duration |
|---|---|---|---|
| Plastic or polyvinyl chloride (PVC) | Large internal diameter allows good drainage postoperatively | Rigid and inflexible, may cause urethral discomfort | 7 days |
| Polytetrafluoroethylene (PTFE), Teflon coated latex | Smoother outer surface, reduces tissue damage and more resistant to encrustations than pure latex | Unsuitable for people with latex allergies, please refer to appendix H risk assessment | 28 days |
| Silicone Elastomer coated latex | Smooth internal and external surfaces, may reduce potential for encrustation over pure latex. | Unsuitable for people with latex allergies, please refer to appendix I risk assessment. | 12 weeks |
| Hydrogel coated latex | More compatible with body tissue, less trauma, low surface friction, improved patient comfort. | Unsuitable for people with latex allergies, please refer to appendix I risk assessment. | 12 weeks |
| All Silicone | They have a slightly wider lumen than that of coated catheters; therefore should be considered if the patient is prone to blockage of their catheter, suitable for patients with a latex allergy | Silicone allows diffusion of water, balloons may therefore occasionally deflate in situ, causing the catheter to fall out | 12 weeks |
11.11 Appendix K acute chronic retention in males first time male pathway
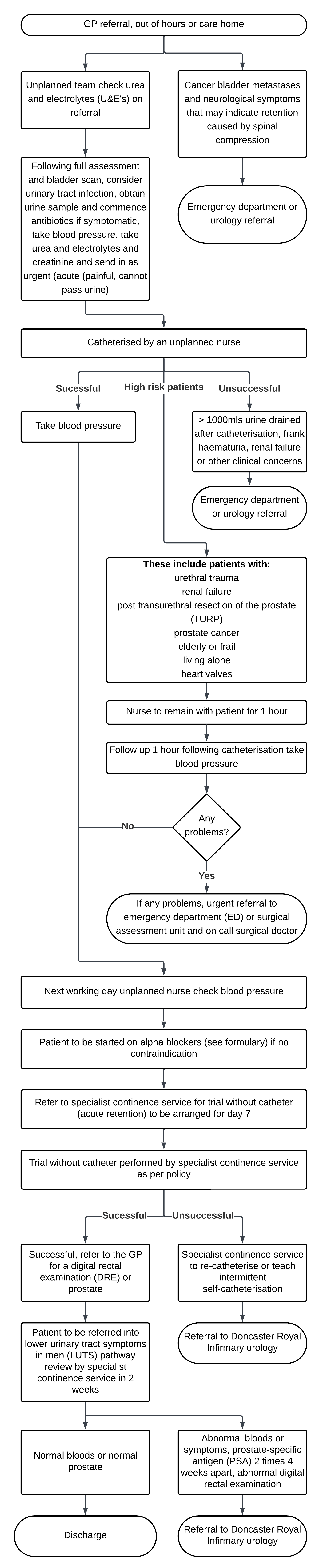
- GP referral, out of hours or care home
- Cancer bladder metastases and neurological symptoms that may indicate retention caused by spinal compression: emergency department or urology referral.
- Unplanned team check urea and electrolytes (U&E’s) on referral.
- Following full assessment and bladder scan, consider urinary tract infection. Obtain urine sample and commence antibiotics if symptomatic, take blood pressure, take urea and electrolytes and creatinine and send in as urgent (acute (painful, cannot pass urine).
- Catheterised by an unplanned nurse.
11.11.1 Catheterisation unsuccessful
- Unsuccessful catheterisation greater than 1000mls urine drained after catheterisation, frank haematuria, renal failure or other clinical concerns.
- Emergency department or urology referral.
11.11.2 High risk patients
- These include patients with:
- urethral trauma
- renal failure
- post transurethral resection of the prostate (TURP)
- prostate cancer
- elderly or frail
- living alone
- heart valves
- Nurse to remain with patient for 1 hour.
- Follow up 1 hour following catheterisation take blood pressure.
- If any problems, urgent referral to emergency department (ED) or surgical assessment unit and on call surgical doctor.
- If no problems proceed to 11.11.3 step 2.
11.11.3 Catheterisation successful
- Successful, take blood pressure.
- Next working day unplanned nurse check blood pressure.
- Patient to be started on alpha blockers (see formulary) if no contraindication.
- Refer to specialist continence service for trial without catheter (acute retention) to be arranged for day 7.
- Trial without catheter performed by specialist continence service as per policy.
11.11.3.1 Trial without catheter unsuccessful
- Specialist continence service to re-catheterise or teach intermittent self-catheterisation.
- Referral to Doncaster Royal Infirmary urology.
11.11.3.2 Trial without catheter successful
- Successful, refer to the GP for a digital rectal examination (DRE) or prostate.
- Patient to be referred into lower urinary tract symptoms in men (LUTS) pathway review by specialist continence service in 2 weeks.
- Normal bloods or normal prostate: discharge.
- Abnormal bloods or symptoms, prostate-specific antigen (PSA) 2 times 4 weeks apart, abnormal digital rectal examination: referral to Doncaster Royal Infirmary urology.
11.12 Appendix L intermittent self catheterisation 3-day diary
Refer to appendix A: intermittent self catheterisation 3-day diary (staff access only)
11.13 Appendix M changing a leg bag procedure
Equipment:
- sterile dressing pack containing galipots or an indented plastic tray, low-linting swabs or medical foam, gloves (sterile and non-sterile), sterile field and disposable bag
- new leg bag
- receptacle for old leg bag
- appropriate fixing to support leg bag
| Action | Rationale |
|---|---|
| Explain and discuss the procedure with the patient Use suitable private area | To ensure the patient understands the procedure and gives informed consent. To ensure privacy |
| Decontaminate hands using alcohol hand gel or liquid soap and water or for community settings soapy hand wipes can be used followed by alcohol hand gel. Note, If in patients own home and hands are decontaminated with soap and water use only liquid soap and dry thoroughly with kitchen roll. Refer to hand hygiene procedure | Hand hygiene prior to contact with patient |
| Put on apron, open sterile dressing pack and apply sterile gloves | To prevent cross-infection |
| Place sterile towel under connection between catheter and bag | To prevent cross-infection |
| Separate leg bag from catheter using a gauze swab and insert the new leg bag immediately without touching the end of the new leg bag | To reduce risk of contamination and to minimise the length of time drainage system is broken |
| Secure new leg bag with chosen method of support | To prevent tension on the catheter by weight of urine |
| Risk assess the need to wear goggles. Empty urine in the night bag into sluice or toilet and discard night bag in appropriate waste stream | To prevent cross-infection, to prevent splash back |
| Dispose of equipment using appropriate waste stream | To prevent cross-infection |
| Remove and dispose of gloves and apron in the appropriate waste stream. Decontaminate hands with alcohol hand gel, soap and water or soapy hand wipes | To prevent cross-infection |
| Document the amount of urine drained and the date of the next change in the patients’ records. Document the date of change on the catheter bag | Comprehensive data for protection of nurse carrying out procedure and patient receiving the procedure |
11.14 Appendix N emptying a catheter bag procedure
Equipment:
- non-sterile gloves
- apron
- disposable pulp receptacle or jug (single use) Note, patients own home jug (kept for this purpose only)
- gauze or tissue
| Action | Rationale |
|---|---|
| Explain the procedure to the patient | To obtain consent and ensure the patient understands the procedure |
| Decontaminate hands using alcohol hand gel or liquid soap and water or for community settings soapy hand wipes can be used followed by alcohol hand gel. Note, if in patients own home and hands are decontaminated with soap and water use only liquid soap and dry thoroughly with kitchen roll. Refer to hand hygiene procedure | To prevent cross-infection |
| Put non-sterile gloves and apron on | To prevent cross-infection |
| Put pulp receptacle or jug under tap ensuring the tap does not come into contact with the jug. Open the tap and allow urine to drain until the bag is empty | To prevent cross-infection and ensure complete emptying of the bag |
| Close the tap and clean with gauze or tissue | To prevent leakage and prevent cross-infection |
| Risk assesses the need to wear goggles. Dispose of urine in the sluice or toilet | Assess risk of splash back. To prevent cross-infection |
| Dispose of pulp receptacle using appropriate waste stream. Note, in patients own home, clean the jug with appropriate cleansing solution | To prevent cross-infection |
| Remove and dispose of gloves and apron in the appropriate waste stream. Decontaminate hands with alcohol hand gel, soap and water or soapy hand wipes | To prevent cross-infection |
| Record urine measurement in notes if required | To maintain accurate fluid balance |
11.15 Appendix O single use night bag connecting procedure
Equipment:
- new single use night bag
- non-sterile gloves
- apron
- gauze
- catheter stand
| Action | Rationale |
|---|---|
| Explain procedure to patient | To ensure the patient understands the procedure and gives informed consent |
| Decontaminate hands using alcohol hand gel or liquid soap and water or for community settings soapy hand wipes can be used followed by alcohol hand gel. Note, If in patients own home and hands are decontaminated with soap and water use only liquid soap and dry thoroughly with kitchen roll. Refer to hand hygiene procedure | Hand hygiene prior to contact with patient |
| Put on apron and non-sterile gloves | To prevent cross-infection |
| Connect single use night bag to leg bag port, turn leg bag tap to open and ensure tubing is not kinked | To ensure free drainage from leg bag to night bag without breaking closed drainage system |
| Loosen leg bag supports and fix night bag to catheter stand on the floor or stand attached to the side of the bed. Decontaminate hands with alcohol hand gel, soap and water or soapy hand wipes | To facilitate drainage of urine and to aid patient comfort |
| Remove and dispose of gloves and apron in the appropriate waste stream | To prevent cross-infection |
| Document in the patients’ record that the night bag has been attached | Comprehensive data for protection of nurse carrying out procedure and patient receiving the procedure |
Note, for terminal patients who are nursed in bed or patients in the acute setting where the use of a leg bag is not required, a reusable night drainage bag may be attached directly to the catheter and changed every 7 days.
11.16 Appendix P my catheter passport
Refer to appendix P: my catheter passport (staff access only).
11.17 Appendix Q pad weighing instructions
Refer to appendix Q: pad weighing instructions (staff access only).
Document control
- Version: 4.
- Unique reference number: 485
- Approved by: clinical policies review and approval group.
- Date approved: 3 March 2026.
- Name of originator or author: clinical team lead, specialist continence service.
- Name of responsible individual: chief nurse.
- Date issued: 29 April 2026.
- Review date: 30 April 2029.
Page last reviewed: April 29, 2026
Next review due: April 29, 2027
Problem with this page?
Please tell us about any problems you have found with this web page.