For a copy of this annual report and accounts and any previous years, please contact Philip Gowland, Director of Corporate Assurance at p.gowland@nhs.net.
Presented to parliament pursuant to schedule 7, paragraph 25(4)(a) of the National Health Service Act (2006).
Performance report
This section provides an introduction to the annual report from the chief executive and chair. It describes the trust and highlights some of the major achievements in the year, the risks we have faced and provides some facts and figures about the Rotherham Doncaster and South Humber NHS Foundation Trust (RDaSH).
Chair introduction
It gives me great pleasure to welcome you to this year’s annual report and accounts.
I should start this introduction with the great news that we’ve balanced our books in what has been and still is an increasingly difficult financial period for the NHS. It has been incredibly hard to do this with a lot of dedication from the leadership team across the trust, and with strong leadership from board colleagues. I want to thank everyone for their support. Despite the financial difficulty, we are well on target to poverty proof our services, helping our patients the best way we can, by delivering promise 6, for example by funding additional transport to support some patients to be able to attend appointments.
We have also been able to invest in patient care services, with new peer support roles, additional specialist psychology roles, and an expansion of our learning disabilities teams. We are clear that more of the monies that we do have need to be spent on direct patient care and that is a path we have been taking over the last eighteen months. We have also introduced from April 2025 the real living wage. I’m so proud of this. We were aware of the impact on our staff who were receiving less than the real living wage, not only on our colleagues but their families and the communities in which they live. It gives our staff a bit more money in their pocket and it also shows we are not prepared to pay our colleagues wages they can’t live on. It has been helpful to have strong support for these changes from trade union colleagues.
Staff wise we continue to attract and retain an excellent calibre of people. It will be a pleasure in May 2025 to reintroduce, post pandemic, face to face celebrations for long and distinguished service, to complement our ever-expanding awards and recognition system. Our recruitment is strong, and we are running at the least vacancies ever. Our trust people council has also been introduced and quickly became a success giving an extra voice to staff and groups, such as our range of networks. It’s great to see them making such a positive impact on the work we do.
That council includes our staff governors, who form part of the wider council of governors. That council, led with the support of our lead governor Joan Cox, now has unprecedented scale and reach: it should provide a challenging environment on behalf of local people to the pace of change and the depth of reform that we need.
Our apprenticeship programme is also having a real impact. Its growth is helping our people gain the skills and qualifications they need to move their careers forward or for our new recruits, to begin their career with vital education. This is one part of our commitment to learning and education. Last July I chaired an entire board meeting focused on this important space, and since September all our people have had access to monthly learning half day sessions. This is in addition to ringfenced training spend across all our disciplines with new ‘bottom up’ training plans in place.
We’ve also more volunteers in our organisation, supporting us with our work across most of our teams and departments. The different mix of volunteers we have is excellent and it’s great to see the work they do having such an impact on our patients. It’s also fabulous to see some of our volunteers gain the experience they need and to move into employment. We’ve also made big strides forward with our community partners and I want them to know how much they are valued, as they challenge us and support us in delivering all of our 28 promises. It’s also great to see our promises being delivered, they are clearly not just words on a page.
Finally, I want to thank colleagues in the integrated care boards and in the provider collaboratives for their dedication and support, at a time which is clearly tough for them with recent announcements of significant NHS changes in the months ahead. I want them to know how we really value their contributions.
So, a big thank you to everyone who works so hard to help Rotherham, Doncaster and South Humber NHS Foundation Trust deliver our promises and to deliver the best patient care possible. I hope you feel that this report is an honest reflection not only of what has worked well and improved, but also what still need to do better.
Kathryn Lavery, Chair 26 June 2025.
Chief executive introduction
Thank you for taking the time read through the annual report for the twelve months that end in March 2025. The report, alongside a suite of other published material, is intended to reflect openly on the quality of care we provide to patients, carers and communities locally. The law requires that this report contains certain information in a certain format, and my colleagues have worked hard nonetheless to seek to make that material accessible to those we work for and with.
Some very positive steps have been taken, as a trust, and in partnership at neighbourhood and place levels, in the past twelve months. The move to widespread use of patient feedback through tools including care opinion have the potential to transform relationships between those receiving or waiting for care, and colleagues who provide that care. We are excited that over 900 people have chosen to share their experiences with us, and with one another. We will want to build on that work in the year ahead, as it is integral to two promises that we made within our strategy in 2023 (promises 4 and 5).
Equally importantly, we have taken decisive steps to change our staffing as a trust. Most importantly the number of vacant posts we have has reduced dramatically, as we have succeeded in recruiting, and indeed begun to reduce turnover (or in plain English, people leaving for other jobs or well-earned retirement). We enter the year April 2025 to March 2026 almost below 100 vacancies. At the same time, we have grown our bank workforce in partnership with NHS professionals, who took on the employment of our flexible staff contracts in October 2024. Finally, we have almost ended the use of agency staffing across the trust, a huge improvement in quality and cost, and one made possible by flexibility among established staff. The board is crystal-clear that only by being fully staffed, and having stable teams, can we embed the learning, care standards, and support among our staff, that high quality healthcare requires.
Looking ahead, we have a dual focus on two major measures of change in 2025: promises 14 and 19. Having documented and prioritised those waiting for care in our services, we are now working hard to make changes in how we work to meet our commitment to a short wait service. For many of our pathways of care, a short wait with us means someone will not need to rely on other health and care services. In 2025 we are still using beds for care a long way away from our local communities. These out of area placements are ways of working we have committed to reducing and that will mean we need to work in different ways within our wards and community teams.
Some baseline measures of safety in our care provide a level of assurance about quality. These include our work on assertive outreach care planning, consideration of the lessons from nationally published enquiries including Greater Manchester, and our rapid response to issues raised by our local coroner in respect of all-age care. Clinical and managerial colleagues should be proud of new work this year to ensure that health based places of safety are open consistently, and that no patient remains within one for longer than twenty four hours.
However, our ambition to deploy a broader quality and safety improvement plan in 2024 has not happened; albeit groundwork to do so, including baseline adoption of national culture of care standards, is now in place. Likewise, the trust has led work to assess eating disorder services across South Yorkshire and consider how to meet national medical emergencies in eating disorders (MEED) guidance. The trust’s peer review process which we commenced in late 2023 is now enhanced through the role of patients as reviewers, and through an extensive programme of ‘out of hours’ visits. Put more simply, seeing how care is experienced at weekends and of an evening. The annual governance statement contained within this report continues to suggest, in my view, that the trust has work to do to use quantified information consistently to measure the care we provide, and, in particular, to test the personalisation of care plans and risk assessments.
Whether we apply improvement work to quality of care, staff experience, partnerships with others or finance, we can draw some lessons from where we have succeeded over the year under review. By year-end we are consistently able to offer access to child and adolescent mental health services (CAMHS) within a four-week window, and with immediate and urgent response much more quickly than that: in all three places in which we work. Determined work to build partnerships has led our virtual ward in Doncaster to be able to look after more citizens than ever before, and our community intravenous therapy (IV) service is actively growing to help avoid admissions to acute hospital care. Tackling historic long waits for memory services, including dementia diagnosis, has allowed many more people to receive support from both the trust, local GPs, and the voluntary sector, especially in North Lincolnshire and in Rotherham. These examples of sizeable, quantified changes are important markers of what the directorates and care group teams, supported by our backbone colleagues and the board’s leaders, can deliver.
The trust provides high quality education and research, as well as patient care. External accreditation, and scale of trial studies and of students (and their feedback), suggest these traditional trust strengths continue to be nurtured well. Both will be crucial as we look, in the years before 2028, to make our mission of nurturing the power in our communities something that we embed in how we work, not simply in what we do.
Toby Lewis, Chief Executive 26 June 2025.
Our services
The trust is registered with the Care Quality Commission (CQC) to provide safe care that is responsive and effective and as such provides a range of health and social care services across three localities through a care group (and directorate) model in Rotherham, Doncaster and North Lincolnshire.
We structure to management of our services into groups, with five of our six being clinical. Within those clinical care groups, we now manage services in aggregate through 13 directorates. The details of these arrangements are listed below:
Children’s care group
- Children’s mental health directorate, providing services across Doncaster, North Lincolnshire and Rotherham.
- Children’s physical health directorate, providing services across Doncaster, North Lincolnshire and Rotherham.
Physical health and neurodiversity care group
- Neurodiversity directorate, providing services across Doncaster, North Lincolnshire and Rotherham.
- Community and long-term conditions directorate, providing physical health services across Doncaster.
- Rehabilitation directorate, providing physical health services across Doncaster.
Doncaster adult mental health and learning disabilities care group
- Learning disabilities and forensic directorate, providing forensic services to the communities of Doncaster and learning disabilities services across Doncaster, North Lincolnshire and Rotherham.
- Community directorate, providing adult and older peoples mental health services within Doncaster.
- Acute directorate, providing adult and older peoples mental health inpatient and crisis services within Doncaster.
North Lincolnshire adult mental health and talking therapies care group
- Talking therapies directorate, providing services across Doncaster, North Lincolnshire and Rotherham.
- Community directorate, providing adult and older peoples mental health services within North Lincolnshire.
- Acute directorate, providing adult and older peoples mental health inpatient and crisis services within North Lincolnshire.
Rotherham adult mental health care group
- Community directorate, providing adult and older peoples mental health services within Rotherham.
- Acute directorate, providing adult and older peoples mental health inpatient and crisis services within Rotherham.
The history of Rotherham Doncaster and South Humber NHS Foundation Trust
The trust provides a range of health and social care services across three localities, Rotherham, Doncaster, North Lincolnshire serving a population of approximately 749,700.
The trust operates from over 60 community and inpatient sites, employs 3,606 (average whole time equivalent) staff and had an annual income of approximately £249,000,000. This will rise above £250,000,000 in the year April 2025 to March 2026. The trust was originally formed in October 1999 and in 2002, took on responsibility for the delivery of mental health services in Rotherham. On 1 August 2007, the trust was authorised to operate as an NHS Foundation Trust under the NHS Act 2006. On 1 October 2010, the transfer of tier 2 primary mental health child and adolescent mental health services (CAMHS) from Doncaster Council (DMBC) and tier 3 child and adolescent mental health services from Doncaster and Bassetlaw Hospitals NHS Foundation Trust (DBH) to the trust took place. Also in 2010, the trust integrated with Doncaster Community Healthcare and Rotherham Community Health Services under the Transforming Community Services programme. The trust was renamed Rotherham Doncaster and South Humber NHS Foundation Trust (formerly known as Rotherham Doncaster and South Humber Mental Health NHS Foundation Trust) to reflect the range of services provided.
In 2021 the trust was appointed lead provider for the Adult Eating Disorder Provider Collaborative within the South Yorkshire Integrated Care System (ICS) and as such has commissioning responsibilities in respect of the adult eating disorder service across the whole of South Yorkshire. We anticipate these services being managed through a new Joint Committee of the four local trusts and integrated care board (ICB) during the year April 2025 to March 2026.
The trust operates a wholly owned community interest company (CIC) called Flourish, which in addition to its community activities, provides social care services. A separate annual report for Flourish is issued, reflecting its distinct governance.
The trust’s board members are charitable trustees for the organisation’s charity, now named Your Hearts and Minds, previously called the trust charitable fund. This holds assets of £1,800,000 and, again reflecting separate governance arrangements, produces a distinct annual report and audited accounts.
Trust strategy
The trust’s strategy (2023 to 2028) was developed after eighteen months of staff and community engagement and co-production. It is very much at the heart of how the trust is managed and which priorities we set. It is a strategy to deliver five objectives, which are to:
- nurture partnerships with patients and citizens to support good health
- create equity of access, employment, and experience to address differences in outcome
- extend our community offer, in each of, and between, physical, mental health, learning disability, autism and addiction services
- deliver high quality and therapeutic bed-based care on our own sites and in other settings
- help to deliver social value with local communities through outstanding partnerships with neighbouring local organisations
The five objectives are underpinned by 28 promises (further detail is available within the Clinical and organisational strategy 2023 to 2028 on the trust’s website) made to our community, due to be achieved during the lifetime of the strategy. During the year an outline of the challenge and potential of achieving individual strategic objectives has been reported. For each promise, the trust board has received a rating to outline if there is a specific delivery plan been developed and the likelihood of delivery. The rating is dynamic and is considered every eight weeks. Over the course of the year, we have made progress with the majority of promises.
Stronger achievement is visible for objectives 1 and 5 than for the objectives we set on inequalities, community first, and our high-quality therapeutic care commitment. Our efforts in the year April 2025 to March 2026 will seek to redress that balance.
- Strategic objective 1: delivery is in two parts; because promises 3 (volunteers), 4 (patient feedback) and 5 (involving people in decision making) are seeing strong progress, measured in data we track, and in the feedback of others, notwithstanding the developments highlighted above. Both our carers network (promise 2) and peer support workers (promise 1) are much broader pieces of work that need more systematic planning in the year April 2025 to March 2026.
- Strategic objective 2: we have not fully delivered promise 9 (our workforce offer for excluded communities), but in the year April 2025 to March 2026 will be increasing evidence of this work as we aim to reshape our workforce offer. This includes work with veterans and homeless citizens, bringing people into employment as well as expanding our service offer. Baseline work in support of promise 6 (poverty proofing) and 12 (meeting the needs of rural communities) is taking place across the trust, and a huge mobilisation has taken place to support delivery of more annual health checks than ever before. The expectation of delivery of the promise 8 (RDaSH 5) is clear to those involved and will continue to be the focus of significant attention: each has been reviewed with the clinical leadership executive (CLE) subgroup and will now feature in the relevant delivery review of for that care group on a routine basis. Promise 7 (Core20PLUS5 and annual health checks for people with a severe mental illness or learning disability) is, in effect, stayed pending resolution of material data issues, albeit trust level data against all bar one measure is now reportable.
- Strategic objective 3: Work now starting for promise 17 on school readiness. Data flow for promise 16 regarding integrated neighbourhood working needs further development. Likewise, the urgent care work we need to do within promise 14 (wating times) has been conceptualised; and investments made to support the “elective care” and productivity changes designed to deliver promise 14 as a whole. All three care groups now have community clozapine delivery plans to support promise 13 (our home first ethos), and the expansion of the community intravenous services continues. The trust is deeply involved in work in both integrated care boards to consider how best to support integrated neighbourhood team working.
- Strategic objective 4: The new contract with South Yorkshire Housing, is likely to be the first of several to deepen the relationship between local providers and the trust as part of implementing promise 23 (investment in long-term care outside of wards). Virtual ward remains solely a physical health construct, albeit we want to expand it to support both adult and older adult mental health, and children’s services. In moving forward personalised care plans, shorter bed based length of stay, and admission and discharge across weekends, the trust will move closer to delivering these promises within this objective, in the year April 2024 to March 2025 we have socialised these ideas; deployment of patient driven outcomes will help us, if well used, to improve the calibre of our care planning, which will be critical to Care Quality Commission outcomes.
- Strategic objective 5: We have work to do moving into the coming year, to make both education (promise 24) and research (promise 28) a routine part of the local management language and obligation. Care groups put considerable time into being ready for promise 25 (real living wage) implementations, in particular by ensuring roles that should properly be band 3 posts were adjusted and back-pay met in the year 2024 to March 2025. Adaptation planning associated with promise 27 (green initiatives), and the trust has identified the scale of investment that would be required to significantly move towards net zero for carbon emissions. Work to tackle perceived and actual discrimination among line managers (promise 26) has started to be planned bottom up, but we know there is far more to do to become truly inclusive as a trust.
In the year April 2024 to March 2025, the trust’s investment fund supported peer support worker growth (promise 1) as well as commitments to tackle issues of safety and risk. In the coming year, the primary focus of investment is in the same domains, but with further investment to ensure that we address our short wait commitments (promise 14) which we know matter very much to our patients and their loved ones.
Health inequalities
The trust is committed to reducing the health inequalities in our communities. Our work to address health inequalities is ingrained in a range of promises made in our clinical and organisational strategy 2023 to 2028. Our commitment to reducing health inequalities is not exclusively confined to strategic objective 2, presented below is the progress made with a range of promises that contribute to addressing the needs of underserved communities.
Promise 6, poverty proof our services and tackle discrimination including through digital exclusion.
Working with a national expert organisation, we have begun the process to poverty proof all of our services. This focuses upon the financial barriers people face in receiving health services. Following an initial pilot in three services in the year April 2024 to March 2025 (children and young people’s mental health service (CAMHS) in North Lincolnshire, podiatry in Doncaster, early intervention in psychosis in Rotherham), a number of services across the trust have been poverty proofed with a view for all patient facing services being so over the next 18 months. A baseline to demonstrate the impact of the review has been set, which is to reduce “did not attend” and or “was not brought”, by 7% in our most deprived areas.
We have also worked with the three Citizens Advice organisations that cover Rotherham, Doncaster, and North Lincolnshire respectively to provide dedicated money and debt advice to patients and to our staff.
Promise 7, deliver all ten health improvements made in the Core20PLUS5 programme to address healthcare inequalities among children and adults: achieving 95% coverage of health checks for citizens with serious mental illness and those with learning disabilities from 2024
A focus of our work in the year April 2024 to March 2025 for promise 7 has been to significantly increase the number of people with a severe mental illness or learning disability receiving their annual health checks. By the end of December, 95% of such people we support had a health check in place, which exceeded any national targets and expectations. We identified that different parts of the health system held different information about who was entitled to health checks, meaning there was a risk of people missing out. We have invested and are working with colleagues in primary care in particular to address this gap.
During the year April 2024 to March 2025, we also identified the tangible contribution we would make to the 5 elements of that national “Core20PLUS5” initiative relevant to our patients over the lifetime of our Strategy. This will be:
- children and adolescent mental health: increasing access to mental health service for children with a black ethnic background by 10%. Reduce was not brought (WNB) appointments from most deprived postcodes of our trust footprint to 7% (aligned with promise 6)
- children’s epilepsy: work to a locally agreed metric of all children and young people with an intellectual disability and or autism diagnosis being seen by a specialist epilepsy nurse within 4 weeks
- adult chronic respiratory disease: targeted work in Doncaster and vaccination promotion for all, with a focus upon people on the community nursing caseload and the specialist respiratory nursing caseload
- adult early cancer diagnosis: number of ‘cancer awareness’ events completed by the cancer information team
- adult hypertension case finding and optimal management and lipid optimal management: targeted work in Doncaster, increase in the number of referrals to primary care following blood pressure check by 100%, work is underway to establish our baseline for this measure, which should be completed by September 2025
Promise 8, research, create and deliver five impactful changes to inequalities faced by our population in accessing and benefitting from our autism, learning disability and mental health services as part of our wider drive to tackle inequality (the RDaSH 5).
In the year April 2024 to March 2025, we defined four areas under this promise which are:
- learning disability life expectancy: focus on ensuring physical health checks for people with a learning disability, especially from minority communities
- dementia: increase in diagnostic rates for people with dementia and better community support for people and those who support them, this includes people from minority and rural communities
- talking therapies: pro-actively focus on access for under-served parts of the community and their recovery rates for depression, anxiety and trauma for older adults
- autism: to improve on our journey to becoming autism friendly services, from a patient, environment and workforce perspective (focus upon inpatient settings)
Baselines have or are being established, and plans are being developed that will help drive the improvements we want to achieve. The fifth commitment within the “RDaSH 5” relates to inequalities of access to perinatal mental health care, where locally, as nationally, there is apparently low take up and referral of families from black and minority ethnic residents.
Promise 10, be recognised by 2027 as an outstanding provider of inclusion health care, implementing National Institute for Health and Care Excellence (NICE) and NHS England (NHSE) guidance in full, in support of local Gypsy, Roma and travellers (GRT), sex workers, prisoners, people experiencing homelessness and misusing substances, and forced migrants.
We have been working with the gypsy, Roma, and traveller community in Doncaster to support access to health care. This includes the use of the health bus at various sites, where people can get general and specific advice about primary and secondary care services.
The trust has commissioned the pathway organisation, a national charity with acknowledged international expertise, to host our review of inclusion health work in RDaSH. We expect that work to lead to the development of a specialist homeless health team working alongside the local authority’s complex lives service.
Specialist services are only part of the right response to the National Institute for Health and Care Excellence guidance, we also need to take action to ensure “mainstream” services are available to all.
Promise 11, deliver in full the NHS commitment to veterans and those within our service communities, recognising the specific needs many have, especially for access to suitable mental health and trauma response services.
We have established arrangements to engage with veterans in our community. There has also been work in our services to increase awareness of veterans’ needs and to begin to ensure we meet the NHS commitment to give priority access to veterans (where their condition relates to time served). In the year April 2024 to March 2025, we were also reaccredited with “Veteran Aware” status showing our contribution to the NHS’s commitment to the Armed Forces Covenant. This re-accreditation will assist further development of best practice, driving improvements across the NHS and standard of care for the armed forces community.
Promise 17, embed our child and psychological health teams alongside schools, early years and nursery providers to help tackle poor educational and school readiness and structural inequalities.
As part of our commitment to work with communities and other organisations to make sure more children achieve “school readiness”, we have undertaken detailed research to understand the position and challenges in our three places. This also includes looking at the needs of specific communities (for example, the gypsy, Roma, and traveller (GRT) community). We have outlined the universal offer from antenatal through to school that are available for children and their families, as well as targeted support and the community offer that is available. This is being used to develop further community engagement, change the frequency of how we track if a child is school ready, look to integrate the offer to families, and work with gypsy, Roma, and traveller community.
We recognise that there is more to do to make sure we underpin the work we are doing on health inequalities. Two of the five strategic delivery risks (SDR) aligned to our objectives are:
- the trust’s inability to work effectively with a diverse population using diverse methods and create alignment between the trust’s agenda and that of the patients and communities (links to strategic objective 1)
- challenges generating data and or evidence to support interventions to address health inequalities (links to strategic objective 2)
Aligned to the above risk, during the year April 2025 to March 2026 we will ensure that our reported data is presented to show age, sex, ethnicity and deprivation.
Working with our integrated care boards
The trust is engaged with its “place” partners and at an integrated care board level. Partnerships are developed through commissioning and service developments. The director of strategic development leads on the evaluation of the benefits of working with partner organisations, by undertaking a review of financial and quality benefits. Governance is managed via partnership boards and agreements in place. The trust undertakes regular planning days to assess potential partners and undertakes a strengths, weaknesses, opportunities and threats (SWOT) analysis to determine the best approach.
It is important to appreciate that many of the most important partnerships we have sit outside the NHS itself. Care groups hold responsibility now for developed meaningful partnerships with local voluntary and community sector enterprises (VCSE) groups and with primary care. Executive relationship managers are in place for our integrated care board and local authority collaborations.
Our arrangements are necessarily complex. The trust works in two integrated care boards, albeit we are hosted by South Yorkshire Integrated Care Board, and we work across three places (in each case a local authority area). Neighbourhood working arrangements vary in their scale and depth and remain to be refined further with the publication of the NHS Ten Year Plan.
The board has established (in March 2024) a public health patient involvement and partnerships committee (PHPIP), that has a remit to oversee key partnerships the trust is involved with, with other key board committees also playing a role in ensuring effective partnering is in place. This role is embedded in terms of reference and ways of working and formed part of our audit programme over the last twelve months: a rating of significant assurance was offered by our internal auditors.
The trust has a wholly owned subsidiary (community interest company) Flourish Enterprises Ltd (Flourish). Flourish has its own directors, and the trust has designated Philip Gowland, RDaSH Director of Corporate Assurance as its shareholder representative, who provides regular reports to the Public Health, Patient Involvement and Partnerships (PHPIP) Committee throughout the year.
The trust is the lead provider for the South Yorkshire Adult Eating Disorder Provider Collaborative. This includes commissioning beds from independent sector providers that is supported by financial and quality oversight: this is delivered through a joint agreement with other providers in South Yorkshire, with the public health patient involvement and partnerships committee overseeing progress on behalf of the board.
Summary of principal risks
The trust faces a broad spectrum of risks but risks around waiting times and patient flow continue to emerge as persistent and significant challenges across the trust. Although these risks are often the most prominent, they exist within a wider landscape that includes workforce availability, regulatory changes, and resource constraints. Each of these factors influences our ability to deliver timely, high-quality care and maintain patient safety and well-being.
Over the past year, our approach to risk management has hinged on thorough oversight and proactive planning. We have improved our workforce initiatives, prioritising both recruitment and retention so that services remain adequately staffed. At the same time, we have introduced streamlined patient pathways and digital solutions to reduce waiting lists where possible, maintain timely access to care, and improve overall flow. These actions reflect our commitment to continuous improvement and adaptability. Over the past year, we monitored emerging threats and adjusted our response when necessary.
Looking ahead, our focus remains on strengthening resilience across the trust through proactive planning, targeted investment, and a sustained focus on patient safety and service quality. Maintaining forward-thinking outlook helps ensure that all services, particularly those influenced by changes in demand and capacity, continue to deliver compassionate, timely care to our communities.
The trust’s strategic delivery risks are structured for the effective and focused management of the principal risks in meeting the trust’s key objectives. All strategic delivery risks have an executive director lead who has reviewed these risks and the associated actions in place on a regular basis to progress mitigation. The strategic risks in place during April 2024 to March 2025 were:
- if our “changed ways of working” with the diverse population (including excluded communities) are not delivered by 2027 because of the leadership’s ability to identify, communicate and engage then it will lead to a loss of confidence locally and likely non-delivery of strategic objective 1 (nurture partnership with patients and citizens to support good health)
- if we do not execute plans to consistently create, use and respond to data inside our services and with others because our leaders lack the time, skills or diligence to see through specific changes or are distracted by wider system priorities then this will lead to a lack of precision in how the trust reshapes services
- if we cannot agree with local GPs and the wider primary care leadership how to coordinate care at health care transition (HCT), primary care network, neighbourhood level because there is not the skill to change, or confidence to experiment in both parties; or funding models are restrictive then we cannot deliver our new community offer with the effectiveness that our strategy requires and shared care will not be achieved and patients will suffer harm
- if seven day working and other bed-based service alterations are not implemented fully because of resistance, inflexibility or affordability, with colleagues able to move elsewhere (where such difficulties are not occurring) then we will continue to place patients out of area and see severe stress and burnout; and increased turnover, among our own employees
- if we do not achieve the step-up in institutional and system capability to deliver multiple time-bound simultaneous changes with impact by 2027 because we do not develop and practice the skillsets required to make change occur then the trust’s strategy will not achieve what it has promised and we will face reorganisation, frustration and turnover among employees
| Category | Indicator | Performance April 2024 to March 2025 | Performance April 2023 to March 2024 |
|---|---|---|---|
| NHS England | NHS Oversight Framework segmentation (1 to 4 with 1 equalling maximum autonomy) | 3 | 2 |
| Care Quality Commission (CQC) | Overall rating (either inadequate, requires improvement, good or outstanding) | Requires improvement. Note, no inspection since 2020 hence rating remains as per that given in 2020. | Requires improvement. Note, no inspection since 2020 hence rating remains as per that given in 2020. |
| Finance | The group accounting deficit was £1,000,000 for the financial year April 2024 to March 2025. The position against which operational performance is measured by NHS England (NHSE) was a surplus of £500,000 compared to a planned deficit of £300,000. A reconciliation between the group deficit and the surplus for operational NHSE performance purposes is included on cost allocation and charging to the accountability report | ||
| National targets | National target relevant to mental health and community services, see operational performance and quality improvement priorities for the year April 2024 and March 2025 | Partially compliant (5 out of 7) | Partially compliant (5 out of 7) |
Reduction in segmentation was linked to our planned deficit and the planned deficit of the South Yorkshire Integrated Care Board and was consistent with segmentation that all South Yorkshire providers were placed in.
Going concern
These accounts have been prepared on a going concern basis. The financial reporting framework applicable to NHS bodies, derived from the HM Treasury Financial Reporting Manual, defines that the anticipated continued provision of the entity’s services in the public sector is normally sufficient evidence of going concern. The directors have a reasonable expectation that this will continue to be the case.
Significant events since year end and overseas operations
There have been no important events since the end of the financial year affecting the trust nor is there any overseas operations to report against.
Performance analysis
How the trust measures performance
The board of directors of the trust is primarily accountable for setting the strategic direction of the organisation and ensuring that the trust effectively communicates its objectives. The quality committee monitor national, local and access performance standards. However, the responsibility for quality and performance remains a shared commitment across all staff, with ultimate accountability resting with the chief executive and the executive team. This accountability is executed through the monthly clinical leadership executive and through a series of delivery reviews which ensure that all aspects of care delivery are considered in one conversation to allow the real balance of safety, workforce development and finance to be considered.
The core principle guiding the trust’s approach is that quality and performance are the shared responsibility of every staff member. This is reinforced through staff appraisals, which empower individuals to perform at their best and foster a clear understanding of quality and performance expectations within their respective roles. Objective setting serves as the framework for performance measurement, whether through nationally mandated targets, locally defined metrics, or individual contributions to team or ward goals. Throughout the year the trust has continued to deliver its 5-year strategy and the associated 28 promises, which remain the focus until March 2028.
Performance is measured through ongoing monitoring of key frameworks, including the “top ten” metrics, which are aligned with the April 2024 to March 2025 Long-Term Plan targets, the NHS Oversight Framework, the trust Promises and other essential metrics. The top ten represent a purposeful sub section of performance metrices which the trust would like all staff to focus on, in a digestible way but represent a focus on improving quality and patient care. For example, we want to increase access to people in a timely way for talking therapies or we want to make sure patients are accessing their annual serious mental illnesses health check.
These are captured in a series of reports channelled into the integrated quality performance report (IQPR), which integrates quality, workforce, and financial data. The clinical leadership executive (CLE), along with its subgroups, and several board committees review and discuss the integrated quality performance report and understand trends, risks and success of what the performance is telling us. This is triangulated in relation to the trust delivery reviews before escalation to the board. The integrated quality performance report provides a consistent, comprehensive “golden thread” across the organisation.
The trust continues to monitor progress through monthly delivery reviews, chaired by the chief executive, to provide focused oversight of critical areas including performance, quality and safety, workforce, and financial management. They are framed on data and key lines of enquiry, relevant to the directorates. These reviews bring together senior leaders to assess progress on the trust’s performance and take corrective action as needed. They are aligned to a similar process within care groups with each of their respective directorates (13 in total).
Additionally, the trust maintains a comprehensive set of service-specific key performance indicators (KPIs), which are monitored at the care group, directorate or service-specific level in accordance with a range of service contracts.
Operational performance
In the year April 2024 to March 2025, the trust rolled over a number of existing metrics, to maintain continuity and then added additional measures which aligned to the promises to drive improvement into “the top ten” metrics. Outlined below, several of the metrics are also broken down into sub-sections in order to monitor our performance more widely than is required nationally.
| Top ten references | Integrated quality performance report reference | Metric description | Trust metric April 2024 to March 2025 | National metric April 2024 to March 2025 | Trust metric April 2025 to March 2026 | National metric April 2025 to March 2026 |
|---|---|---|---|---|---|---|
| 01 | LTP01a (sub metric) | The number of adults and older adults with severe mental illness (SMI) who accessed NHS or NHS commissioned community mental health services, defined as 2 or more care contacts. | Yes | |||
| 01 | LTP01b (top ten metric) | The number of adults and older adults with severe mental illness (SMI) who accessed NHS or NHS commissioned transformed community mental health services, defined as 2 or more care contacts. | Yes | Yes | ||
| 02 | LTP02a (sub metric) | The number of people with common mental health problems accessing talking therapies treatment: trust wide. | Yes | Yes | ||
| 02 | LTP02b (top ten metric) | The percentage number of patients that achieve reliable recovery when compared with the number of people who are discharged having received at least 2 treatment appointments, which meet caseness at the start of treatment in the reporting period: trust wide. | Yes | Yes | Yes | |
| 02 | LTP02c (top ten metric) | The percentage of patients that achieve reliable improvement when compared with the number of people who are discharged having received a least 2 treatment appointments in the reporting period: trust wide. | Yes | Yes | Yes | |
| 03 | LTP03b (top ten metric) | The number of women in the perinatal period who receive support: perinatal only, includes maternal mental health service Sheffield Health and Social Care (255 estimated) | Yes | Yes | Yes | |
| 04 | LTP04a (top ten metric) | Children and young people accessing services 1 contact | Yes | Yes | Yes | |
| 05 | LTP05a (top ten metric) | The number of active inappropriate adult acute out of area placements on the last day of the reporting period | Yes | Yes | Yes | |
| 06 | LTP06a (sub metric) | Virtual ward occupancy day 1 | Yes | Yes | ||
| 06 | LTP06b (sub metric) | Virtual ward occupancy day 15 | Yes | Yes | ||
| 06 | LTP06c (top ten metric) | Virtual ward occupancy day 30 | Yes | Yes | Yes | |
| 07 | LTP07 (top ten metric) | The diagnosis rate for people aged 65 and over with a diagnosis of dementia recorded in primary care, expressed as a percentage of the estimated prevalence based on GP registered populations: place target | Yes | Yes | ||
| 08 | LTP08a (top ten metric) | Annual health checks for people with serious mental illness: place target. (OP61a) | Yes | Yes | ||
| 08 | LTP08b (sub metric) | Annual health checks for people with serious mental illness: promise includes declines (OP61b) | Yes | |||
| 08 | LTP08c (sub metric) | Annual health checks for people with serious mental illness: promise Quality and Outcomes Framework (OP61C) | Yes | Yes | ||
| 09 | LTP09a (top ten metric) | Adult attention deficit hyperactivity disorder | Yes | Yes | ||
| 09 | LTP09b (top ten metric) | Children’s neurodiversity | Yes | Yes | ||
| 10 | LTP10 (top ten metric) | Section 136 breaches over 24 hours: occupancy hours lost to breaches. New from 1 August 2024. | Yes | Yes |
The monthly performance clinics provide enhanced oversight and a targeted approach to performance management. Tailored improvement plans, along with weekly performance monitoring and forecasting enabled the trust to successfully achieve key targets, including those for children and young people’s access (LTP04), community mental health transformation 2 or more Contacts (LTP01), perinatal access (LTP03), virtual ward occupancy (LTP06), talking therapies reliable improvement (LTP02c) and dementia diagnosis (LTP07).
We also achieved the internal metrices set for annual serious mental illness health checks (LTP08b) and seen real progress on the 24-hour metrices for section 136 suites (LTP10), which for example in March 2025 we only lost 11 hours to breaches (for example, patients staying longer than was needed).
During the year April 2024 to March 2025, we have redefined our referral to treatment (RTT) pathways shadow reporting prior to submission from 1 April 2025 onwards. Performance against the new referral to treatment pathways within mental health have surpassed the 92% target achieving 96.10%. Significant work has been ongoing in all care groups but in particular, in our North Lincolnshire’s memory service all of which will have a positive impact on service performance, delivery and patient outcomes. This progress is crucial given the increasing demand for dementia and related care as the population ages. Continued focus on these services across all 3 localities will be key to maintaining and further enhancing these improvements as we move into 2025 and beyond. However, in our physical health service the 18-week referral to treatment has seen a deterioration in performance reporting 84.62%. As we move into April 2025, proactive monitoring of assessment and treatment waits will be provided by the deputy care group director supported by the performance team. Across both physical and mental health, we are reporting zero 52 week waits.
Quality improvement priorities for the year April 2024 to March 2025
The safety and quality priorities for the year April 2024 to March 2025 are outlined below.
What is our priority?
Deliver on our promises under strategic objective 1, with a focus on promise 4 to put patient feedback at the heart of how care is delivered in the trust, encouraging all staff to shape services around individuals’ diverse needs.
What did we expect to achieve?
- Maximise the impact of use of text messaging (SMS) and digital to gather feedback, building on our work in talking therapies during the year April 2023 to March 2024.
- Introduce, develop and evaluate care opinion as our main mechanism for gathering feedback from people in our communities’ using services: this will ensure much faster and wider visibility for our employees of feedback from their patients.
- Each quarter, the clinical leadership executive will discuss and act on a summary of feedback gathered through these methods.
- In quarter 4 of the year April 2024 to March 2025, patient feedback will become a key measure within organisational management of its directorates within the delivery review process.
What have we achieved?
- The use of text messages (SMS) has been rolled out across all talking therapies services.
- Care Opinion has been rolled out across all of our services, including estates and facilities, with managers at team and service level responding directly to this feedback to provide a more personalised and timely response. Care opinion posters are available and it is referred to in patient leaflets. iPads are being used in some areas to support gathering feedback.
- We have seen over 600 stories told in the first 9 months of care opinion. Although this is fewer than the number of your opinion counts forms received in the year 2023 to 2024, we expect care opinion stories to increase as there has been an upward trend since it’s first implementation.
- The roll out of care opinion has been undertaken with a high level of success and accuracy for stories being coded against correct services in order to enable timely feedback.
What have we learned?
- Executive support at the outset enabled care opinion to be well received across the trust and to achieve roll out at this pace.
- Monitoring licences are available on request by Healthwatch, integrated care boards and Care Quality Commission to support ongoing assessment of the trust.
- Further work is being undertaken with uptake in older people mental health, forensic and learning disabilities services in order to be inclusive of these patient groups. The trust is liaising with similar trusts to learn from their experience and this will be ongoing in 2025 to 2026.
- Further work is needed on how to roll out text messaging (SMS) to obtain patient feedback across other services.
The trust has transformed our approach to feedback from patients over the recent past. Feedback is going directly to local leaders and clinicians to inform and shape their thinking. The potential of these approaches is significant for the year ahead and beyond, we need both to act on the learning from this feedback to change, and celebrate and retain the actions and care that provides for such positive feedback from patients.
What was our priority?
We publish our quality and safety plan which will set out a series of safety measures, as always events, designed to improve the consistency of our care
What did we expect to achieve?
- The safety plan’s successful implementation will demonstrate improvements in key measures of psychiatric and physical care, including timely rights compliance, consenting, malnutrition universal screening tool (MUST) assessments and venous thromboembolism (VTE) screening.
- The safety plan work will also see us improve the pace of assessment in community pathways, especially where urgent referrals have been made.
- Our quality plan implementation will see improvements initially in three areas: at risk mental state (ARMS) services as part of early intervention in psychosis (EIP), work to improve toilet training among children and young people (CYP) teams’ client groups, and improved speed of wound healing in district nursing services.
What have we achieved?
- We have drafted a quality and safety plan that will demonstrate how the organisation will maintain quality and safety, and the key measures we will use to measure this.
- Whilst this has taken longer than initially planned, we will approve this at the board of directors in May 2025, and embed the quality and safety plan in the year April 2025 to March 2026
What have we learned?
- We need to be disciplined in choosing what to prioritise as terms such as safety and quality can mean very different things to different people inside and outside the trust.
- Making sure that data is available and used at all levels of the organisation will be central to achieving delivery of the plan.
- It has taken time to support some leaders previously under-involved in quality improvement to recognise that quality and safety is everyone’s responsibility. We are confident this is now understood.
What was our priority?
We will implement improvements to deliver a good rating under the Care Quality Commission framework, including our work on culture of care within mental health inpatient settings.
What did we expect to achieve?
- To deploy our inpatient improvement plan in year, using external expertise to assess our progress, whilst working with the collaborative to ensure that we have learnt from local partners.
- To implement our safe staffing reporting improvement measures, reducing use of temporary staffing, staff sickness, and filling vacancies in the organisation. to ensure all inpatients have a personalised care plan.
What have we achieved?
- We are developing processes in which we demonstrate self-assessment against the Care Quality Commission key lines of enquiry, both to provide board oversight of whether the services we deliver are safe, caring, responsive and effective, but also prepare for any future Care Quality Commission inspections.
- We asses collaboratively lessons learnt from other organisations following recent Care Quality Commission inspections
- We have created clear internal processes around Safer Staffing including monthly review processes to provide oversight, challenge, and review of rostering periods.
- From October 2024, we transitioned to NHS Professionals (NHSP) for the provision of our bank workforce. By transitioning to this and with tight controls in relation to agency spends, we have not required agency nurses for 6 months. Clear processes are in place to approve agency use, with a fundamental principle of ensuring patient safety if future agency workers were required.
- We are part of the culture of care national programme, however we are taking a personalised approach linked with our strategy as agreed with the national culture of care director.
- We have worked with the national patient experience lead in terms of exploring a patient led version of the tool, and local patient experience partners to create a patient version.
- We have completed a baseline assessment for culture of care, with feedback from patients and staff in all areas including adult, older peoples and forensic services and are using the results as part of our high-quality therapeutic care taskforce work.
What have we learned?
- Patients and staff identified some areas of good practice within the initial culture of care assessment. However, it was also clear that access to peer support, and work on equity including for those with neurodiversity, needs to be continued to have real impact.
- We learnt that the previous launch of the mental health optimal staffing tool (MHOST) within the trust did not have the desired effect, and that plans to re-launch this were paused due to a national update of the MHOST, which will be rolled out into quarter 2 of April 2025 to March 2026. We will use the relaunch of this tool to re-evaluate our ward establishments and provide key information into our annual investment cycle where staffing levels need to change into April 2026 to March 2027.
What was our priority?
We will make progress to deliver promises 14 and 19 within our strategy.
What did we expect to achieve?
- Identify the route to meet our March 2026 four week wait guarantee, making initial progress in the child and adolescent mental health service (CAMHS), community nursing services, and memory clinics.
- Waiting times for children and adult neurodiversity services will reduce significantly.
- Work to deliver our aim of no inappropriate out of area placements: with an initial intent to hold consistently, below 15, the number of patients away from their local area for care.
What have we achieved?
Promise 14
- Progress has been made in all care groups regarding waiting times for routine referrals. Significant work has been undertaken to increase visibility of waiting lists, with full scoping from health informatics, performance and care groups to ensure all waits are now visible with live data refresh daily. This has supported a large piece of validation work to ensure that all relevant data is accurate, complete and timely and represent true waits. All waiting lists are scrutinised weekly at care group level, with a weekly subgroup of the operational management group (OMG) providing oversight of this process and presenting an update monthly to OMG to ensure that progress is maintained.
- Child and adolescent mental health service (CAMHS) services have been the forerunner for this work and have achieved a maximum 4 week wait in North Lincolnshire and Doncaster, except in cases of patient choice. Neurodevelopment services within children’s and attention deficit hyperactivity disorder services in adults have received additional investment and are working towards trajectories to allow achievement of a 4 week wait. Progress within our other mental and physical health services is summarised below when compared to 1st April 2024 baseline.
- Thorough demand and supply modelling has occurred for 80% of services throughout this financial year and those services with true gaps in supply have placed investment bids that will make achievement of the 4 week target achievable across all services by April 2026. In addition, scoping has been conducted of current booking processes to implement new ways of booking in patients to allow sufficient notice of appointment to be given within the 4-week timescale.
Promise 19
- We have focused on improving a number of areas. This has included establishing a complex clinically ready for discharge forum with all 3 local authorities in October 2024 and there has been a marked improvement in all 3 Places. We have prioritised work on the Section 136 suites, with the successful introduction of a 24- hour metric which means suites remain open and patients are seen in a timely way. There was also a sixth suite opened in January 2025, following system wide demand and capacity work which means more patients have access to suites in their own Place.
- We have relaunched the 3 monthly ‘Multiagency Admissions and Discharges Events (MADE) in each care group facilitated by patient flow and attended by ward staff, local authority and integrated care board colleagues. This is an opportunity to discuss the trusts acute, older adult and psychiatric intensive care unit pathways from a system level to improve flow through the pathway and the experience of those who access our services.
- The 24-hour flow team have reviewed a number of processes to ensure patients are discussed in a timelier way, ensuring there is better opportunity to consider community alternatives working with system partners and the community teams.
- In February 2025 we established the high quality therapeutic care task force, chaired by the chief executive and with a majority of clinicians as participants, as well as patients and social care partners. This think tank will support the elimination of out of area placements (OAP) in the year April 2025 to March 2026 and executive time is being spent with clinical colleagues in reviewing the approach.
What have we learned?
Assess people referred urgently inside 48 hours from 2025 (or under four where required)
This element of the promise is behind plan for achievement from 2025. Initial scoping has been conducted which has highlighted inconsistencies with referral categorisation across services, with 34 different definitions of urgent referrals being used across services. In addition, services are not currently operating in a way that allows for triage and assessment across all services that receive urgent referrals. Standardised urgent referral pathways trust-wide will be implemented, inclusive of all teams and service areas; the extension of operational hours to allow for 7 day per week triage and assessment and a full informatic system redesign to streamline processes and allow close monitoring of the metric.
Deliver a four-week maximum wait for all referrals from April 2026
Trajectories are being developed for all services not currently achieving the 4-week maximum wait time so that forecasts can be developed for the proportion of lists achieving throughout the year.
Pathway work has been identified as required in a number of services to improve efficiency so this will inform the trajectories. This is being undertaken at a service level and will continue throughout the year April 2025 to March 2026.
New booking processes are being rolled out to support patient choice and ability to attend appointments within the 4-week timeframe. This work is being supported by the roll out of the patient portal (an approved investment bid), which will allow 2-way communication with patients, the ability to triage online, and the ability for appointments to be cancelled and adjusted by patients. This will be rolled out using a risk-based approach with clinical oversight.
Promise 19
We believe substantial improvement is possible, and a revised timetable for elimination will be assessed in quarter 1 of 2025. Our general plans for the year April 2025 to March 2026 assume sizeable change from July 2025.
This will require a focus on what happens while in an inpatient setting and especially addressing length of stay, achieving the national benchmark of an average of 32 days across all the adult mental health wards. We will continue to focus on safe discharges and reducing extended stays when patients are ready to return to their communities. We will also focus on admissions, to be able to consider where safe and therapeutically appropriate community alternatives can be considered. This will require close work with systems partners; better use of our “crisis houses” and investment in rehabilitation services across all Places
Patient feedback
Patient feedback is received in a variety of ways, primarily care opinion, patient advice and liaison service (PALS) contacts, compliments and complaints.
The ‘your opinion counts’ was the primary form of feedback available to patients, carers in families in previous years. It was recognised that this method was outdated and required review. As a result, the trust transferred to using care opinion from 1 June 2024 and this was rolled out across all services.
The majority of your opinion counts comments and care opinion stories are positive about our services which is always reassuring to hear, but we welcome those who are critical. 10% of care opinion stories have been mildly or moderately critical. These stories give us the building blocks to improve our services and look at them with a fresh eye (a number of stories are presented below).
The reduction in the number of PALS contacts is likely due to the introduction of care opinion as patients and carers have been directed to using that as a means of contact directly with the service concerned. The PALS service does remain in place should anyone remain dissatisfied with the response from the service.
The table below shows the feedback received from 1 April 2024 to 31 March 2025, along with the figures for the previous year.
| Feedback | April 2024 to March 2025 | April 2023 to March 2024 |
|---|---|---|
| Patient Advice and Liaison (number of contacts) | 417 | 695 |
| Your Opinion Counts (number of returned forms, 1 April 2024 to 31 May 2024) | 667 | 1189 |
| Care Opinion stories (1 June 2024 to 31 March 2025) | 666 |
Care Opinion
We have reviewed care opinion to look at what our patients are telling us and shared customer feedback (outlined in the speech bubbles). When combined with the delivery of the key metrics this provides a comprehensive picture of performance within RDaSH and whilst response times, access rates and service usage are a good indicator for the numerical side of performance the positive customer feedback adds that additional qualitative layer. This provides insight into how those metrics are experienced by service users, their families and carers.
Within physical health services the virtual ward (LTP06) is a community-based initiative providing patients with care at home rather than requiring hospitalisation. Occupancy rates have remained consistently above the 80% target on the 1st and 30th day of the calendar month and in March 2025 remained above on all 3 points of the calendar month thus demonstrating strong and sustained performance.
Care Opinion quote: “My son is coming to child and adolescent mental health service (CAMHS) almost weekly. She is the nicest, most devoted, professional, kind, caring woman I’ve met in a long time. Secondly, she’s gone above and beyond her duties to my son and is helping the whole family. The service had been wonderful to us.”
In children’s services, the trust successfully met the target for the second consecutive year with regards the number of children and young people (CYP) receiving one clinical contact within a 12-month rolling period (LTP04), with 9,791 children and young people accessing services, surpassing the target of 9,783. The children’s eating disorder service performed well, with 100% of the most urgent cases seen within one week across the full year and 93.18% of referrals seen within four weeks, just short of the 95% target.
Care Opinion quote: “It’s been an absolute pleasure. The staff are so kind, helpful and caring. Nothing is too much trouble. They support you and are always there for you. I cannot praise and thank them enough.” For community mental health services for adults and older people (LTP01), the trust continued to exceed the target, with 10,005 individuals receiving two clinical contacts within a 12-month period, exceeding the target of 8,533. This reflects effective engagement and care provision, crucial to alleviating pressures on inpatient services and promoting recovery in the community. Care Opinion quote: “I felt alone, worthless, worried, anxious, not good enough and guilty after I had my baby. I have had a wonderful perinatal health visitor named Nicola by my side and she has been a breath of fresh air. I’d have been lost without her and wish I could have kept her attendance much longer as her knowledge and expertise was far more than the role she was doing, she made me see my worth again and see things from a different and more healthy perspective. I can’t thank Nicola enough for her time, patience and guidance and I will be forever thankful for her.”
The joint perinatal and maternal mental health service (LTP03), in collaboration with Sheffield Health and Social Care, exceeded expectations, with 830 women receiving support during the year April 2024 to March 2025, surpassing the target of 617. This service remains a key focus for the year ahead, with a task and finish group dedicated to maintaining high performance levels.
Care Opinion quote: “Thanks for being so empathetic and caring.”
While the trust made strides in improving access to talking therapies (LTP02a), demand still fell short of the year-to-date expectations despite ongoing efforts to engage diverse communities and strengthen referral pathways. We are particularly trying to focus on communities who really need our support in accessing talking therapies such as older people, people from world heritage communities and people with a level of learning disability. That said, the performance in quarter 4 of the year April 2024 to March 2025 outperformed the access rates for the same period in the year April 2023 to March 2024 demonstrating that the service is starting to see a gradual and sustained increase in the number of patients entering treatment. There remains a significant number of further actions to embed and sustain this change whilst also further building capacity and demand to deliver the target as we move into the year April 2025 to March 2026. For reliable recovery (LTP02b), year to date performance was 47%, just short of the 48% target, but still reflecting sustained improvement from the November 2024 position. Reliable Improvement for our talking therapies services (LTP03c) performed well achieving above the 67% target.
Care Opinion quote: “Came for a health check, did feel well during. Everyone I saw were fantastic. Felt really supported and looked after. Everyone’s so friendly. Couldn’t ask for more help. Even a cuppa tea. Thank you”
The metric measuring the number of SMI patients having a full annual health check (LTP08) is a Place target and, as such, data is released nationally a quarter in arrears therefore data to demonstrate achievement of this metric is not available. Internally, performance is measured against a cohort of patients with forming a register that we have internal oversight of based on Quality and Outcomes Framework (QOF) code. Performance against this measure, excluding declines, is reporting 79.36% against a 95% target. Continued focus is being placed for the year April 2024 to March 2025 on reducing the number of patients who decline elements of their health check such as BMI and blood tests. A key piece of work has commenced and is ongoing through the early part of the year April 2025 to March 2026 with GP surgeries in the three localities to cleanse and cross-reference these internal registers with those held by GPs with the goal of having 1 register per place which can be kept accurate and up to date.
A notable challenge throughout the year April 2024 to March 2025 was the high number of inappropriate out-of-area placements (LTP05). By the end of March, 19 patients remained placed outside the RDaSH footprint, and we have ranged between 7 to 37 over the year. A range of improvements were introduced but there is a recognition of significant work to do. The trust is fully committed to addressing this issue and will be a key focus as we go into the year April 2025 to March 2026. A High-Quality Therapeutic Care task force was launched in February 2025, acting as a think tank for Q1 in the year April 2025 to March 2026 to start significantly reducing out of area placements placement from Q2.
Care Opinion quote: “On going issue with the current waiting list for attention deficit hyperactivity disorder assessment. I have been on the list now for almost 2 years. When I have phoned to question the length of time I will be waiting for, I have been told sorry, but you are on a waiting list, and you will be seen at some point.”
Neurodevelopment services (LTP09) continue to remain challenging due to the high number of referrals into these services and lengthy waiting lists in both our adult attention deficit hyperactivity disorder and children and young people neurodevelopmental services remain high. While a national issue, RDaSH are prioritising this work on this due to the impact on patients and their families of lengthy waiting for assessments. The care groups have redeveloped the trajectories to build in nuances that were not already accounted for regarding capacity within the service to support with the delivery of the four-week wait by April 2026 however 4,518 (3,668 waiting as at March 2024) Adult’s remain on the attention deficit hyperactivity disorder waiting list and 2,872 (2,823 waiting as at March 2024) children and young people remain on the neurodevelopment (attention deficit hyperactivity disorder and autism) waiting list as at the end of March 2025.
Mental health community survey
The mental health community survey is an independently administered national survey of patients receiving mental health care in community settings. The survey is comprehensive and provides valuable quantitative data to facilitate comparison with other trusts and benchmark our services numerically against a range of indicators. The survey for RDaSH in 2024 contacted 1232 service users, of which 245 completed the survey.
The trust rated as ‘much better than expected’ in overall experience by the Care Quality Commission.
The results for specific questions are categorised depending on whether they are ‘better’, ‘worse’ or ‘about the same’ compared with other trusts. For RDaSH the breakdown was as follows:
- In 22 questions, RDaSH was ‘About the Same’
- In 2 questions, RDaSH was ‘Somewhat Better.
- In 8 questions, RDaSH was ‘Better’
- In 3 questions, RDaSH was ‘Much Better’
Complaint handling
We acknowledge that in the year April 2024 to March 2025 we did not meet the standards that we expected in responding to complaints. We failed our complainants and their families in providing an answer to their concerns and we failed our services in providing the opportunity to listen and learn from the voices of our patients. We have taken significant steps to address this and as a result, believe that we are now in a stronger position moving into the year April 2025 to March 2026.
Complaints are a valuable source of learning and insight. Our ambition is to increase the availability of the complaints option, expecting to see complaints rise, but to reduce the number of reopened complaints.
| Indicator | April 2024 to March 2025 | April 2023 to March 2024 |
|---|---|---|
| Number of complaints received | 80 | 70 |
| Number acknowledged within 3 working days | 70 | 64 |
| Number ongoing (still open) | 37 | 40 |
| Number upheld | 7 | 2 |
| Number partially upheld | 11 | 12 |
| Number not upheld | 7 | 13 |
| Number withdrawn | 14 | 3 |
| Number investigated to the Ombudsman | 0 | 1 |
| Number of clinical negligence claims raised which had previously been a complaint | 2 | 3 |
The 2 new clinical negligence claims made by complainants in the period 1 April 2024 to 31 March 2025 both remain ongoing as at 31 March 2025.
The main three categories for complaints in were:
| Category | Number |
|---|---|
| Patient care | 25 |
| Communication | 11 |
| Values and behaviour of staff | 12 |
| Category | Number |
|---|---|
| Patient care | 26 |
| Communication | 10 |
| Values and behaviour of staff | 10 |
Financial performance
Revenue
Total operating revenue in year April 2024 to March 2025 amounted to £249,000,000 (£226,000,000 in the year April 2023 to March 2024), an increase, on the prior year total, of £23,000,000.
Around £211,000,000 (85%) of our income is received from NHS bodies for the purchase of healthcare activity. A further £22,000,000 (9%) is received from local authorities for public health activity. Overall revenue also included £11,600,000 (4.7%) of notional income recorded in the accounts for additional pension contributions which have been paid directly to NHS pensions in year (compared to £7,100,000 in the year April 2023 to March 2024).
Expenditure
Our operating expenditure excluding financing costs was £248,000,000 and the largest element of this was the pay bill for our staff costs of £199,000,000 (80%). Other significant components of the trust’s expenditure baseline are the purchase of healthcare services from other providers of £10,000,000 (4%), establishment and premise costs of £11,000,000 (4%) and supplies, service, and drugs costs of £12,000,000 (5%).
Capital and cash
The group had a cash balance of £32,200,000 (£34,400,000 in April 2023 to March 2024) at the close of the financial year. Capital expenditure excluding lease additions in April 2024 to March 2025 totalled £8,000,000 (£7,000,000 in the year April 2023 to March 2024), of which £2,800,000 (35%) was spent on clinical refurbishment and reconfiguration, £2,900,000 (36%) on IT, £2,000,000 (25%) on estate maintenance and £300,000 (4%) on equipment and vehicles.
Group position and underlying position for NHS England monitoring purposes
The accounts included in the annual report reflect a group position which consolidates the Foundation Trust, Charitable Funds accounts and Flourish CIC. The Charitable Funds accounts had a net adverse movement in funds of £500,000 in the year April 2024 to March 2025, with Flourish CIC finishing the year with a £2,000 surplus.
A reconciliation from the overall group position as reported in the statement of comprehensive income to the underlying deficit for NHSE operational performance purposes is shown below:
| Underlying surplus for NHSE operational performance | Surplus (deficit) (£000) |
|---|---|
| Rotherham, Doncaster and South Humber NHS Foundation Trust | (527) |
| Flourish CIC | 2 |
| Charitable fund | (484) |
| Group position | (1,009) |
| Remove impairment reversal credited to operating expense | (41) |
| Remove capital donation and peppercorn lease impact | 3 |
| Remove Private Finance Initiative revenue costs on an IFRS 16 basis | 2,730 |
| Add back Private Finance Initiative revenue costs on a UK GAAP basis | (1,835) |
| Remove non-cash pension movement | (19) |
| Remove net impact of Department of Health and Social Care centrally procured inventories | 198 |
| Remove Charitable Fund Deficit | 484 |
| Underlying deficit for NHS England operational performance | 512 |
Cost allocation and charging
The trust has complied with the cost allocation and charging guidance issued by HM Treasury.
Political donations
No political donations were made in the year April 2024 to March 2025 (none in the year April 2023 to March 2024).
Better payment practice code
The trust adopts the better payment practice code in respect of invoices received from suppliers. The code requires the trust to aim to pay all undisputed invoices within 30 calendar days of receipt of goods or a valid invoice (whichever is later) unless other payment terms have been agreed. The table below shows the performance against this metric by NHS and Non-NHS supplier and shows the volume and value of invoices paid. The target of paying 95% of valid invoices within 30 days has not been achieved, although there has been significant improvement since the year April 2023 to March 2024 when 83.3% of invoices by number and 85.9% by value were paid within 30 days.
Process enhancements have been implemented in year which vastly improved payments against the target in the last quarter of the year. These enhancements, including the introduction of an extra payment run every week, are expected to ensure the target is achieved in the year April 2025 to March 2026.
| Enhancements | NHS | Non NHS | Total |
|---|---|---|---|
| Total | 1,524 | 18,473 | 19,997 |
| Paid in 30 days | 1,424 | 16,879 | 18,303 |
| Not paid in 30 days | 100 | 1,594 | 1,694 |
| Percentage (%) paid in 30 days | 93.3% | 91.4% | 91.5% |
| Enhancements | NHS | Non NHS | Total |
|---|---|---|---|
| Total | 16,163 | 43,969 | 60,132 |
| Paid in 30 days | 15,002 | 40,196 | 55,198 |
| Not paid in 30 days | 1,161 | 3,773 | 4,934 |
| Percentage (%) paid in 30 days | 92.8% | 91.4% | 91.8% |
Interest liability
No interest was accrued and paid by the trust for failing to pay invoices within the 30-day period where obligated to do so and this is the same as for the year April 2023 to March 2024.
Income generation
The trust has not levied any fees and charges where the full cost exceeds £1 million or the service is otherwise material to the accounts. In accordance with Section 43(2A) of the NHS Act 2006, the trust can confirm that income from the provision of goods and services for the purposes of the health service in England is greater than our income from the provision of goods and services for any other purposes. The trust has, therefore, met this requirement. Also, in accordance with section 43(3A) of the NHS Act 2006, the trust can confirm that the other income received has had no impact on the provision of goods and services for the purposes of the health service in England.
Forward look to the year April 2025 to
arch 2026
The financial outlook going into the year April 2025 to March 2026 continues to be a challenging one. The trust has submitted a breakeven plan for April 2025 to March 2026 (£300,000 planned deficit in the year April 2024 to March 2025), which includes £2,400,000 of nonrecurrent deficit support funding and £13,300,000 of planned efficiency savings (£6,600,000 in the year April 2024 to March 2025) comprising of £8,500,000 cash savings and £4,800,000 from productivity improvements. The financial outlook is consistent with local, regional and national NHS systems and will require collaborative working with a wide range of partners to identify new ways of working and recurrent savings, whilst continuing to improve health outcomes for the population we serve.
Performance report signed on behalf of the board of directors.
Toby Lewis, Chief Executive, 26 June 2025.
Accountability report
Staff report
The trust values its employees and has 3,606 staff working across our geographical footprint.
| Staff costs | Permanent (£000) | Other (£000) | Total (£000) April 2024 to March 2025 | Total (£000) April 2023 to March 2024 |
|---|---|---|---|---|
| Staff executive directors (RDaSH operated an internal staff bank up to 20 October 2024; these costs are included within “other”) | 145,542 | 3,938 | 149,480 | 135,331 |
| Social security costs | 14,238 | 0 | 14,238 | 13,782 |
| Apprenticeship levy | 697 | 0 | 697 | 668 |
| Employer’s contributions to NHS pensions | 17,814 | 0 | 17,814 | 16,152 |
| Pension cost: employer contributions paid by NHSE on provider’s behalf | 11,569 | 0 | 11,569 | 7,063 |
| Pension cost: other | 90 | 0 | 90 | 97 |
| Other post-employment benefits | 0 | 0 | 0 | 0 |
| Agency | 0 | 2,956 | 2,956 | 7,555 |
| External bank (internal bank staff transferred to NHS Professionals from 21 October 2024) | 0 | 2,719 | 2,719 | 0 |
| Total staff costs | 189,950 | 9,613 | 199,563 | 180,647 |
| Of which costs capitalised as part of assets | 181 | 18 | 199 | 75 |
| Of which total staff costs excluding capitalised costs | 189,769 | 9,594 | 199,364 | 180,572 |
| Of which termination benefits | 206 | 0 | 206 | 74 |
| Average number of employees (working time equivalent basis) | Permanent working time equivalent | Other working time equivalent | Total working time equivalent April 2024 to March 2025 | Total working time equivalent April 2023 to March 2024 |
|---|---|---|---|---|
| Medical and dental | 65 | 44 | 109 | 79 |
| Administration and estates | 1,061 | 21 | 1,082 | 929 |
| Healthcare assistants and support staff | 596 | 96 | 692 | 751 |
| Nursing | 1,157 | 23 | 1,180 | 1,138 |
| Scientific and technical staff | 539 | 4 | 543 | 509 |
| Total Average numbers | 3,418 | 188 | 3,606 | 3,450 |
| Of which Average engaged on capital projects | 4 | 0 | 4 | 2 |
The above data is subject to audit.
Year-end analysis
The profile of staff in post (by headcount) was:
| Workforce | Male April 2024 to March 2025 | Female April 2024 to March 2025 | Male April 2023 to March 2024 | Female April 2023 to March 2024 |
|---|---|---|---|---|
| Directors | 10 | 8 | 9 | 9 |
| Senior managers (band 8a and above) | 38 | 130 | 33 | 100 |
| Others | 624 | 3,294 | 688 | 3,667 |
| Total | 672 | 3,432 | 730 | 3,776 |
| Workforce | White | Black and minority ethnic | Not stated |
|---|---|---|---|
| Directors | 15 | 3 | 0 |
| Senior managers (band 8a and above) | 159 | 8 | 1 |
| Others | 3,510 | 378 | 30 |
| Total | 3,684 | 389 | 31 |
| Data | April 2024 to March 2025 | April 2023 to March 2024 |
|---|---|---|
| Sickness figure | 6.4% | 5.9% |
| Working time equivalent days lost | 58,489 | 52,558 |
| Average working time equivalent | 3,489 | 3,382 |
| Days per employee (working time equivalent) | 16.71 | 15.54 |
Staff turnover
Turnover data is published by NHS Digital.
We were a people promise exemplar site and our turnover has gradually reduced during the financial year to 9.74% which is pleasing given our drive to fill our vacancies but to also retain the talent we already have within the trust.
Staff policies and actions applied during April 2024 to March 2025
We have a full suite of people policies which are developed and reviewed in partnership with staff side representatives. These include recruitment and selection (including how applications for employment by those with disabilities will be given full and fair consideration), learning and development, attendance management, flexible working, conduct and standards and performance management. These policies are underpinned by processes that provide opportunity for employees with a disability and their managers to agree and put in place reasonable adjustments to support them within the workplace throughout their career, which are captured within their personal Health Passport. We are committed to employ, retain and develop our disabled staff. We undertake an equality impact assessment on all of our people policies to ensure that our employment practices do not discriminate against colleagues.
Our people policies are also used in the event that a member of staff develops a disability or long-term condition during their employment with us.
During the recruitment process, we are committed to putting in place adjustments where necessary to ensure a fair and inclusive process. Candidates who have declared a disability need only to meet the essential criteria to be guaranteed an interview. Managers are responsible for ensuring that all adverts, job descriptions and person specifications provided to the recruitment team exclude any statements which could be deemed discriminatory.
The Recruitment team ensure that any direct or indirect reference to discrimination is removed from all application forms and that the equality and inclusion information is removed from the shortlisting process.
The supporting health wellbeing and attendance management policy allows for increased levels of absence where it is recognised that a declared disability may impact upon levels of absence. Time off for treatment or rehabilitation, which may be categorised as disability leave may be given as a reasonable adjustment. In addition, where an employee’s disability will increase the levels of disability related sickness the trust may, as a reasonable adjustment, allow a greater level of absence before progressing through the stages of the policy.
Access to education, training and development is as open and inclusive as possible, with no discrimination in terms of the protected characteristics and is readily available to parttime and full-time staff irrespective of working pattern and geographical location. Courses are advertised via the staff portal and electronic staff record (ESR) for self-booking and are available to all.
An analysis on protected characteristics is undertaken in relation to how our training budgets are spent, this report is presented to our educational and learning group meeting. This helps us to monitor and ensure that their underrepresented groups are not disadvantaged.
The trust acknowledges that “no one size fits all” with regards to training and supports access to a range of learning and development opportunities that meet individuals’ learning styles and circumstances.
We endeavour to ensure that all our training is accessible for every colleague, our main training facility at Tickhill Road has disabled access. We ensure that all learning styles are accommodated throughout the training delivery. Colleagues can and do actively request reasonable adjustments prior to training commencing such as handouts in advance, larger font, hearing loop. We have accommodated training for a colleague who required an assistant dog, and we adapt lessons according to need. Where training requires an assessment, colleagues are supported throughout the process, given continual feedback and additional time and support is offered. We work with colleagues across the wider organisation to ensure that the training is trauma informed.
The trust is committed to supporting staff to remain in and thrive at work and have developed a supporting health and wellbeing and attendance management policy which is used for all employees with a disability who make their needs known, either at the recruitment stage and for those staff who are currently employed by the trust who become disabled during their employment.
Staff engagement
There continues to be a multitude of ways that the trust continues to engage with the workforce, below are just some of the ways the trust gather views and feedback from colleagues:
- the quarterly people pulse survey is an email survey about individual experiences of working within the organisation
- the annual staff survey goes to all colleagues and gathers their views and experiences (see staff survey to expenditure on consultancy for the results of the last survey)
- the introduction of the trust staff council
- the launch of the new leadership development offer for the top 150 leaders within the organisation
- board meetings are advertised regularly and are open for all colleagues to attend in person if they wish or to dial in remotely. Alongside this all meetings are recorded and available to watch at a later time
- the chief executive offers a regular series of drop-in meetings across the geographical footprint to gather first hand feedback and views from the workforce
- we actively seek engagement and involvement in the trusts performance, an example this year being the drive to achieve 4 week waits across a number of our services.
- Chair’s video post board meeting – staff are always welcome to feedback comments to the chair or chief executive directly
- the chief executive weekly vlog updates colleagues on current issues whilst also welcoming direct feedback
- there is a monthly email with news and updates to all backbone staff
- we have a monthly meeting with our staff side colleagues, joint consultative committee (JCC) and a bimonthly meeting with our medical staff side colleagues to facilitate engagement and wider collaboration. This is supported by additional meetings to discuss matters as and when they arise.
Freedom to Speak Up
The trust’s freedom to speak up (FTSU) guardian provides bi-annual reports to the trust’s people and organisational development committee. The reports provide an overview of the key areas of work the trust is focusing on and information is also provided on the trust’s legal and contractual obligations, NHS standards, charters, and areas of good practice. In addition to the guardian, we have 76 FTSU champions and a further 14 colleagues have expressed an interest in becoming a FTSU champion.
Freedom to speak up (FTSU) concepts continue to highlight opportunities for improvement and are taken on board at RDaSH. This biannual report is provided to the board of directors meeting, to provide assurance that FTSU processes are in place in RDaSH and are being utilised. The trust people council is a new board sub committee which focuses on the culture of the trust, and the guardian is a key member of this non-executive led body.
To ensure best practice and the guidance is adhered to, the structured reports include issues; potential patient safety or worker safety and experience issues; action taken to improve FTSU culture; learning and improvement; and recommendations.
The guardian continues to deliver training around civility in respect in conjunction with colleagues from the organisational development department in order to promote principles of speaking up as well as increasing visibility. We continue to promote the FTSU pathway and the learning from concerns raised is shared with individuals, at care group level and in the quality and safety group.
During the year April 2024 to March 2025 there were 88 concerns raised (98 raised in the year April 2023 to March 2024) within the trust. Each of the concerns raised has been discussed and progressed at a team level, with learning then explored at an organisational level, triangulating learning and data through care group, directorate and people and organisational development and quality and safety meetings, identifying opportunities to learn and improve.
We remain dedicated to exploring innovative ways to encourage open dialogue, ensuring every team member feels safe and supported when raising concerns. The work on increasing the number of champions, monthly drop-in sessions for care groups and backbone staff, quarterly supervision sessions for all champions and the guardian being present at all peer review’s help to develop this ethos within the trust. Our commitment is to build a culture grounded in trust, respect, civility, and include civility within our teams and across the entire organisation. The guardian has worked alongside peers in the North East and Yorkshire FTSU guardians’ network and is in the process of rolling out a standard operating procedure for staff suffering from adverse effects due to speaking up (detriment). As well as this there has been a new implementation of improvement of feedback mechanism within FTSU around detriment. All concerns raised to FTSU, now have followup anonymous emails sent to them 3, 6 and 12 months after closure. These anonymous emails give staff members the opportunity to make the guardian aware that they have suffered detriment after raising and FTSU concern in order for the guardian to take appropriate steps and escalate on their behalf.
All our people can access the new FTSU e-learning on the electronic staff record (ESR). The first module, Speak Up, is for all workers, second module, Listen Up, is for managers and anyone that supervises people this module focuses on listening and understanding the barriers to speaking up. The final module, Follow Up is now available, it is for senior leaders to support the of Freedom to Speak Up as part of the strategic vision for organisations and system.
The FTSU Guardian is actively engaging with the organisation and is arranging visits to all our champions in their workplace environments to build connectivity and engagement. There has been a change to the format of how the guardian interacts with the champions due to the growing number. Implementation of a monthly freedom to speak up face-to-face drop-in session for corporate staff alongside the drop-in sessions that were already in place for each care groups have the aim of increasing awareness of FTSU corporate staff as well as explaining the service and process. There has also been a new implementation of quarterly supervision sessions the freedom to speak up champions delivered by the guardian. This is a forum for champions to discuss any concerns there have for the guardian to either support them raising this concern or sign post them. The guardian also discusses recent updates from the national guardians office as well as best practice for freedom to speak up.
Work has continued to take place regarding increasing FTSU communication and enhanced induction for new starters including the international nurses. Information on speaking up is shared in trust publications. The guardian continues to deliver induction engagement sessions to the IEW’s speaking about the importance of the FTSU agenda.
Speaking up and staff diversity networks
The RDaSH FTSU guardian continues to attend virtual meetings for all the staff networks, being visible and creating safe psychological spaces for colleagues to discuss their concerns. The role of FTSU guardian is seen as a vital mechanism to ensure that people can continue to care for patients safely and to support staff wellbeing.
Half day learning event Freedom to Speak Up
The guardian facilitates half day learning events initially focusing on how managers react when a FTSU concern or any concern in general is raised regarding the specific area. It contains practical steps that leaders can take in order to support anyone raising the concern and they are wider team members. There will be a further half day learning event for FTSU which all staff will be able to attend and will contain information around the general principles of FTSU and how to access it.
Widening cultures via communities of Freedom to Speak Up practice
Our RDaSH FTSU approach is to be fully embedded in a range of networks, enabling us to benefit from our collective, supportive framework speaking up. Our freedom speak up guardian actively participates in regional meetings and regularly accesses peer support, ensuring ongoing resilience in their role. Meanwhile, the national guardians office offers psychological sessions and webinar based support to guardians. This continuous support not only helps our guardian remain fully effective within their role within the organisation but also reinforces a culture of respect, civility and mutual support across all levels. In addition to individual support, these communities provide structured opportunities for sharing best practice, learning from challenges, and collectively developing into innovative solutions that normally enhance our speaking up framework but also contribute to broader organisational developments in culture and patient’s safety.
Visibility of the guardian
The guardian has focused on increasing visibility through the organisation and visits each care group once every 4 to 6 weeks to help develop trust within the staff group and to help ‘spread the word’ of what FTSU does. Some other action the guardian has taken are below:
- present at each staff diversity network
- present in all peer reviews
- expanded champion’s network
- shadowing opportunities with the guardian
- substantive FTSU Guardian now in place from February 2024
- confidentiality is maintained throughout the process with oversight from the guardian
- confidentiality is discussed with champion in the FTSU champions network.
- peer network with other guardians in the region
Freedom to Speak Up month October 2024 (listen up)
The theme for the month was listening up, emphasising the transformative power of active listening. During the face-toface sessions the guardian spent time explaining that it is important not to just encourage everyone to speak up but also ensuring that every concern, idea, and peace of feedback is heard with genuine care and prompt action. Listening up serves as a call to all leaders and colleagues alike to create safe, open spaces where voices can be shared freely, where stories of both challenges and successes are acknowledged, and where our collective commitment to improving patient care and staff will wellbeing is reinforced. The guardian based themselves in a different locality each week. Trust communications were sent every week for the month of October with senior leaders throughout the organisation promoting the importance and value of listening up within the context of FTSU.
Learning and improvement
There are 19 concerns open at present (this includes 1 case where staff spoke up on the same issue). All other concerns have been closed.
Below is a list of learning points (high level only) related to the concerns raised within the year April 2024 to March 2025.
- civility and respect issues, civility framework and behavioural charter to tackle some of these issues is being explored
- recruitment of more FTSU champions, this has been addressed, and training has been delivered to the new volunteers
- concerns around lack of visibility of senior leadership
- guardian attending all peer reviews in inpatient setting
- patient safety experiences
- lack of support and understanding of the role of medical personal assistant’s
- staff fatigue and staff shortage, worker experience
- team dynamics, potential disruption of teams working together post pandemic, remote working, pressure, and fatigue
- concerns around staff conduct outside of work
- issues around communication and feedback
- implementation of supervision sessions for FTSU champions
- concerns around increasing pay for band 2 and subsequent effect on band 3
- development of standard operating procedure for staff suffering from adverse effects of speaking up (detriment)
- improvement of feedback mechanism for detriment for FTSU concerns (3, 6 and 12 months post closure)
Staff support
The trust is committed to supporting the health and wellbeing of our colleagues and recognises that maintaining both the physical, mental, emotional and spiritual needs of its workforce impacts upon the quality of patient care we provide and also impacts positively upon employee experience.
The trust has a commitment to work in a trauma informed way. The trust’s healthy workplaces staff support and stress at work policy outlines a wide range of interventions that can be accessed by colleagues.
The support offered for staff continues to be well accessed and includes staff support services, face to face counselling, financial advice, access to online training and development sessions, coaching, distance supervision, personal resilience, team effectiveness and team reflective practice.
The quarterly people pulse survey and annual NHS staff survey is used to measure the impact of the above interventions and the well-being of the workforce.
Health and wellbeing
The trust health and wellbeing offer is a broad offer which covers all the primary elements of wellbeing including physical, emotional, mental, financial and spiritual wellbeing. The health and wellbeing interventions on offer include citizen’s advice for financial advice and support, weight management classes, fitness classes, wellbeing campaigns throughout the year, menopause advice and support.
During the year April 2024 to March 2025, 1,800 employees attended appointments with the occupational health service with a total of 6,647 referrals broken down as follows:
- wellbeing 2,235
- case management 1,947
- vaccinations and bloods 1,039
- musculo-skeletal issues (MSK) 859
- health surveillance 511
- neurodiversity 56
The highest reason for case management referral was mental health at 41% with the main reason being stress, followed by anxiety with 68% of staff were in work at the time of referral. There were 8 employees who were referred for needlestick injuries.
Policies in relation to countering fraud and corruption
The trust has a fraud, corruption and bribery policy in place (policy reference 197) and has an identified executive director who is the trust’s fraud champion. The role of a fraud champion is to support and challenge the organisation in relation to its commitment to fraud work. The champion will help promote a zero-tolerance approach to fraud within our organisation. The role and duties of the fraud champion includes:
- promoting awareness of fraud, bribery and corruption within your organisation
- understanding the threat posed by fraud, bribery and corruption
- understanding best practice on counter fraud
The trust also has an accredited person, nominated to the NHS Counter Fraud Authority, to undertake the full range of counter fraud, bribery and corruption work, including proactive work to prevent and deter fraud, bribery and corruption, and reactive work to hold those who commit fraud, bribery or corruption to account.
Our policies, procedures and staff training reflect our commitment to acting ethically in all our business relationships, and to implementing effective systems and controls to protect public funds and mitigate the risk of fraud.
Equality, diversity and inclusion
Promise 26, sets out our ambition in part to become an anti-racist organisation by 2025. This promise not only relates to racism but cover all forms of discrimination, and the trust’s commitment to address and actively fight discrimination of any kind.
Our staff survey results, showed more responses were submitted by RDaSH colleagues, and whilst our results remained comparatively good, both within our ‘sector’ and locally they have deteriorated from the previous year. Our workforce race equality standard (WRES) data contained an increase in the proportion of colleagues reporting positive improvements. With both the number of global majority colleagues experiencing discrimination from their manager and colleagues in the previous 12 months our results improved along with the number of global majority colleagues reporting the trust provides equal opportunities for career progression. Whilst the results are showing positive signs of improvement, we recognise further work is required.
During August 2024, employees, patients and communities faced the riots and violence associated with protests about immigration. The trust’s response to those events whilst being positively received, did give rise to more insights about what matters to our colleagues and the depth of the entrenched behaviours.
The trust messaging throughout this period was clear that we will not accept nor tolerate racist behaviour, but this does not remove the distress our colleagues had experienced, in August and the months and years prior. We are determined that this must act as a platform to further amplify our work on promise 26 to make a positive difference in this area.
The trust people council is where the feedback and voices from our 5 staff networks come together to shape how we work together to address cultural challenges. Each of the networks provides a platform for colleagues to voice their opinions, share their experiences, support and advise on improving working practices, services and information on diversity and inclusion policies, initiatives and longer-term ambitions.
From our workforce disability standard (WDES) data we saw a slight increase in disabled colleagues experiencing harassment, bullying or abuse from patients and service users or members of the public but a reduction in those experiencing the same behaviour from managers and colleagues, with a significant reduction in the colleague harassment, bullying or abuse from colleagues, but overall, a lower number of colleagues who experienced the harassment or abuse reporting it. Colleagues reported significantly lower levels of pressure to attend work from their manager when they were not well enough to do so, which is a positive but we have work to do on colleagues feeling they have access to career progression and the extent we value colleagues’ work.
The following networks are currently in place within the trust:
- ReaCH, Racial Equality and Cultural Heritage Network
- DAWN, Disability and Wellbeing Network
- Rainbow Network
- Women’s Network
- Carer’s Network, this is our newest network, launched in February 2025
Alongside this we have had 8 established leaders and 5 aspiring leaders actively participate in a reciprocal mentoring programme which ran from September 2024 to June 2025. The focus of the programme is understanding lived experiences, inclusion, cultural diversity and career progression and development. Feedback from the programme is positive.
Staff survey
The trust has a variety of ways of getting feedback from people who work in the organisation. The national staff survey is one such approach and over 2200 colleagues completed this for 2024, which is an improvement of 4% on last year’s survey.
The NHS staff survey is conducted annually, and we use a mixed model approach (paper and digital surveys) to ensure that we are not digitally excluding colleagues from completing the survey due to a lack of access to IT or IT skills.
From the year April 2021 to March 2022 the survey questions align to the seven elements of the NHS ‘People Promise’, retaining two previous themes of engagement and morale. All indicators are based on a score out of 10 for specific questions with the indicator score being the average of those.
The response rate to the survey in the year April 2024 to March 2025 among trust staff was 57% (in the year April 2023 to March 2024: 53%).
Scores for each indicator together with that of the survey benchmarking group (50 organisations across mental health and learning disability and community trusts) are presented overleaf.
| People promise elements and themes | Trust score April 2024 to March 2025 | Benchmarking group score April 2024 to March 2025 | Trust score April 2023 to March 2024 | Benchmarking group score April 2023 to March 2024 | Trust score April 2022 to March 2023 | Benchmarking group score April 2022 to March 2023 |
|---|---|---|---|---|---|---|
| We are compassionate and inclusive | 7.58 | 7.55 | 7.63 | 7.58 | 7.7 | 7.5 |
| We are recognised and rewarded | 6.34 | 6.35 | 6.41 | 6.41 | 6.5 | 6.3 |
| We each have a voice that counts | 6.93 | 6.94 | 7.06 | 7.01 | 7.2 | 7 |
| We are safe and healthy | 6.5 | 6.4 | 6.57 | 6.38 | 6.6 | 6.2 |
| We are always learning | 5.83 | 5.93 | 5.95 | 5.93 | 5.9 | 6.1 |
| We work flexibly | 7.05 | 6.83 | 7.09 | 6.84 | 7.1 | 6.7 |
| We are a team | 7.11 | 7.15 | 7.17 | 7.18 | 7.2 | 7.1 |
| Staff engagement | 7.02 | 7.07 | 7.19 | 7.11 | 7.3 | 7 |
| Morale | 6.27 | 6.2 | 6.38 | 6.17 | 6.40 | 6 |
A breakdown of the trusts performance against the benchmarking group for the 9 key themes and areas in the year April 2024 to March 2025 is detailed below:
| People promise elements and themes | Best | Trust | Average | Worst |
|---|---|---|---|---|
| We are compassionate and inclusive | 7.9 | 7.58 | 7.55 | 7.03 |
| We are recognised and rewarded | 6.83 | 6.34 | 6.35 | 5.98 |
| We each have a voice that counts | 7.31 | 6.93 | 6.94 | 6.18 |
| We are safe and healthy | 6.72 | 6.5 | 6.4 | 5.86 |
| We are always learning | 6.37 | 5.83 | 5.93 | 5.11 |
| We work flexibly | 7.34 | 7.05 | 6.83 | 6.27 |
| We are a team | 7.48 | 7.11 | 7.15 | 6.78 |
| Staff engagement | 7.49 | 7.02 | 7.07 | 6.32 |
| Morale | 6.66 | 6.27 | 6.2 | 5.46 |
Areas of focus for the year April 2025 to March 2026
The focus of work over the next 6 months will be working with colleagues across the trust to think through what good practice we need to make trust wide. Our new trust people council, which includes our staff governors, will play a key role in that work.
We have valuable anonymised comments from around 15% of those who responded. We will look to use regular pulse surveys in the year ahead to build on that work.
The initial review of our data shows that:
- we scored higher than our peer group average in the following categories:
- staff morale
- we are compassionate and inclusive
- we are safe and healthy
- we work flexibly
- but at or slightly lower than our peer group average in others:
- staff engagement
- recognised and rewarded
- always learning
- voice that counts
- we are a team
The trust has 1 vision “nurturing the power in our communities” which is underpinned by 5 strategic objectives, with 28 clearly defined ‘promises’ which we will deliver. In the context of our workforce, the trust has a people and teams plan (workforce strategy) which outlines our ambitions to attract, create and enhance a sense of belonging for our colleagues and to cultivate their talent.
We have agreed for year that started in April 2025 to have three trust wide priority areas (appraisal, learning and discrimination) which will be supported by local areas of focus (two or three) from each of our directorates.
Modern slavery
Although the trust is not classed as a “commercial organisation” for the purpose of the Modern Slavery Act 2015, a number of steps have been taken to ensure that slavery and human trafficking is not taking place in any of our supply chains or in any part of our business to the best of our knowledge, through recruitment and payroll processes. The inclusion of statements in contracts that the trust enters into with providers that states that the supplier agrees that it is responsible for controlling its own supply chain and that it shall encourage compliance with ethical standards, human rights, health and safety and environmental standards by any subsequent supplier of goods and services that are used by the supplier when performing its obligations under this agreement.
Trade Union facility time
Total number of trust employees who were relevant union officials during the relevant period (1 April 2024 to 31 March 2025):
| Number of employees who were relevant union officials during the relevant period | Full time equivalent employee number |
|---|---|
| 9 | 4,122 |
Number of trust employees who were relevant union officials employed during the relevant period spending 0%, 1% to 50%, 51% to 99%, 100% of their working hours on facility time:
| Percentage of time | Number of employees |
|---|---|
| 0% | 2 |
| 1% to 50% | 5 |
| 50% to 99% | 1 |
| 100% | 1 |
The information in the table below determines the percentage of the trust total pay bill spent on paying employees who were relevant union officials for facility time during the relevant period (April 2024 to March 2025):
| Costs | Figures |
|---|---|
| Total cost of facility time (includes gross salary, employer pension contribution and national insurance contributions) | 57,733 |
| Total trust pay bill | 199,364,000 |
| Percentage of the total pay bill spent on facility time is calculated as: (total cost of facility time divided total pay bill) times 100 | 0.46% |
Total pay bill, this figure differs from the ‘total staff costs’ presented on year-end analysis; total pay bill represents the expenditure of directly employed individuals and excludes costs such as those associated with agency staff, journaled expenditure and secondment arrangements.
This means the calculation more closely aligns to the staff that the paid union staff represent.
| Costs | Figure |
|---|---|
| Time spent on paid trade union activities as a percentage of total paid facility time hours is calculated as: (total hours spent on paid trade union activities by relevant union officials during the relevant period divided by total paid facility time hours) times 100 | 0.24% |
Details of the trade union facility time disclosures are published on the governments website at sector trade union facility time.
Expenditure on consultancy
As per note 6 to the accounts, the trust spent a total of £0 on consultancy in the financial year (During April 2023 to March 2024 – £250,000). It was part of the financial plan in the year April 2024 to 2025 to eliminate consultancy spend.
Off-payroll arrangements
The trust adheres to the HM Treasury recommendations that for central government departments and their arm’s length bodies, all new engagements and contract renewals for board members and senior officials with significant financial responsibility should be on the organisation’s payroll, unless there are exceptional circumstances, in which case the Accounting Officer should approve the arrangements, and such exceptions should exist for no longer than six months.
The trust is required to disclose certain information in connection with such arrangements as set out in the three tables below.
| Engagement length | Number of existing engagement as of 31 March 2025 |
|---|---|
| Number that have existed for less than one year at time of reporting. 0 | 0 |
| Number that have existed for between one and two years at time of reporting | 2 |
| Number that have existed for between two and three years at time of reporting | 0 |
| Number that have existed for between three and four years at time of reporting | 0 |
| Number that have existed for four or more years at time of reporting | 0 |
| Group | Number of off-payroll workers engaged during the year ended 31 March 2025 |
|---|---|
| Not subject to off-payroll legislation (a worker that provides their services through their own limited company or another type of intermediary to the client will be subject to off-payroll legislation and the trust must undertake an assessment to determine whether that worker is in scope of Intermediaries legislation (IR35) or out of scope for tax purposes) | 0 |
| Subject to off-payroll legislation and determined as in scope of IR35 (a worker that provides their services through their own limited company or another type of intermediary to the client will be subject to off-payroll legislation and the trust must undertake an assessment to determine whether that worker is in scope of Intermediaries legislation (IR35) or out of scope for tax purposes) | 40 |
| Subject to off-payroll legislation and determined as out of scope of IR35 (a worker that provides their services through their own limited company or another type of intermediary to the client will be subject to off-payroll legislation and the trust must undertake an assessment to determine whether that worker is in scope of Intermediaries legislation (IR35) or out of scope for tax purposes) | 0 |
| Number of engagements reassessed for compliance or assurance purposes during the year | 0 |
| Of which: number of engagements that saw a change to IR35 status following review | 0 |
| Off-payroll engagement | Number |
|---|---|
| Number of off-payroll engagements of board members, and or senior officials with significant financial responsibility, during the financial year | 0 |
| Number of individuals that have been deemed ‘board members and or senior officials with significant financial responsibility’ during the financial year. This figure must include both off-payroll and on-payroll engagements | 22 |
Staff exit packages (subject to audit)
For the year April 2024 to March 2025:
| Exit package cost band | Number of compulsory redundancies | Number of other departures agreed | Total number of exit packages by cost band |
|---|---|---|---|
| Less than £10,000 | 2 | 0 | 2 |
| £10,000 to £25,000 | 0 | 0 | 0 |
| £25,001 to £50,000 | 1 | 0 | 1 |
| £50,001 to £100,000 | 0 | 0 | 0 |
| £100,000 to £150,000 | 0 | 0 | 0 |
| £150,001 to £200,000 | 1 | 0 | 1 |
| Greater than £200,000 | 0 | 0 | 0 |
| Total number of exit packages by type | 4 | 0 | 4 |
| Total cost (£000) | 206 | 0 | 206 |
For the year April 2023 to March 2024:
| Exit package cost band | Number of compulsory redundancies | Number of other departures agreed | Total number of exit packages by cost band |
|---|---|---|---|
| Less than £10,000 | 0 | 0 | 0 |
| £10,000 to £25,000 | 0 | 0 | 0 |
| £25,001 to £50,000 | 0 | 0 | 0 |
| £50,001 to £100,000 | 0 | 0 | 0 |
| £100,000 to £150,000 | 0 | 0 | 0 |
| £150,001 to £200,000 | 0 | 0 | 0 |
| Greater than £200,000 | 0 | 0 | 0 |
| Total number of exit packages by type | 0 | 0 | 0 |
| Total cost (£000) | 0 | 0 | 0 |
Exit packages: non-compulsory departure payments
In the year April 2024 to March 2025, there were no non-compulsory departure payments. This is the same as for the year April 2023 to March 2024.
Gender pay gap
In accordance with the Equality Act 2010 (gender pay gap information) Regulations 2017, employers with 250 or more employees are required to publish information on the pay gap between male and female employees as of 31 March each year. This information must be published on the employer’s website. The gender pay gap report is based on a snapshot date of pay of 31 March 2024.
RDaSH data can be compared to other organisations by using the government gender pay gap reporting portal.
Whilst the 2025 data has not yet been published, our work on reducing the gender pay gap is having a positive impact, whilst recognising we still have further work to do. The March 2024 gender pay gap (based on Median Hourly Rate of Pay) was 7.27 and in March 2025 it was 5.09 and a further improvement in April 2025 when we paid the real living wage and it became 3.53.
| Gender | March 2022 | March 2023 | March 2024 | March 2025 |
|---|---|---|---|---|
| Male | 16.13 | 16.84 | 17.82 | 18.87 |
| Female | 14.26 | 15.21 | 16.52 | 17.91 |
| Difference | 1.85 | 1.62 | 1.29 | 0.96 |
| Pay gap percentage | 11.52 | 9.64 | 7.27 | 5.09 |
Environmental matters
On 12 February 2025, RDaSH held a climate adaptation day at a community venue in Rotherham. The key aim was to; hear about what climate adaptation is, understand what others are doing about it, consider how we will care for our patients in 2035 and to start to plan to adapt our services. This was done by creating simulations of what the environment and weather is expected to look like in 2035, based upon real data.
This exercise was in line with promise 27 from our 2023 to 2028 Organisational and Clinical Strategy which is to “deliver the NHS Green Plan and match commitments made by our local authorities to achieve net zero, whilst adapting our service models to climate change”. We focused on the second part of the promise which is around adaptation.
As well as looking at the suggestions made, we will be using the climate adaptation framework for NHS organisations to both guide and inform our work. The Framework is a benchmarking exercise which will help us to understand the challenge so we can make informed decisions based on actual or expected change. By developing this capability, we will gather evidence on climate risks and vulnerabilities, then integrate these into internal systems and procedures.
In the year April 2024 to March 2025, we have developed an RDaSH heat decarbonisation plan (HDP). The HDP outlines how we aim to reduce its reliance on fossil fuels used for heating; the main premise is to phase in electrically powered heating systems and understand the architectural and infrastructural constraints that need to be overcome to make the transition. Our analysis shows that gas is the biggest emitter and has therefore been an area of focus for the year April 2024 to March 2025. We have broken down emissions, building by building, and what solutions exist to move away from the use of gas. The ongoing decarbonisation of the UK’s electricity grid means that electricity consumption has less emissions associated with it than gas and oil. However, due to the limited capacity of the electricity grid, amplified by the increasing use of electric vehicles, our HDP acknowledges that all energy efficiencies, especially thermal efficiencies, must be made to reduce the energy load of the building and or estate. As we have been reviewing the use of our estate, which will culminate in a new estates plan, we have identified a number of sites that we will be seeking to invest in alternative sources of energy. The investment needed will be significant, if we are to achieve our net zero ambition.
Waste management
A proactive approach is taken to waste management, last year we reported that approximately 54% of waste, including food waste, produced by the trust is reused or recycled: this year this has increased to 59.8% Waste overall increase from 530 to 533 tonnes. Food waste decreased in the year April 2024 to March 2025 from 101 in the year April 2023 to March 2024 to 99 tonnes.
We reported last year that during the year April 2023 to March 2024 the trust achieved its zero to land fill promise, and in the year April 2024 to March 2025 we continued to do so.
The NHS clinical waste strategy requires trusts to meet or better a 60:20:20 target. That is 60% offensive waste (OW), 20% alternative treatment (AT) and 20% high temperature incineration (HTI). The trust percentage is 87 OW:11 AT: 2 HTI which is significantly better than the target.
Task force on climate-related financial disclosures (TFCD)
Introduction
Task force on climate-related financial disclosures.
NHS England’s NHS foundation trust annual reporting manual has adopted a phased approach to incorporating the TCFD recommended disclosures as part of sustainability annual reporting requirements for NHS bodies, stemming from HM Treasury’s TCFD aligned disclosure guidance for public sector annual reports. TCFD recommended disclosures as interpreted and adapted for the public sector by the HM Treasury TCFD aligned disclosure application guidance, will be implemented in sustainability reporting requirements on a phased basis up to April 2025 to March 2026 financial year. Local NHS bodies are not required to disclose scope 1, 2 and 3 greenhouse gas emissions under TCFD requirements as these are computed nationally by NHS England.
The phased approach incorporates the disclosure requirements of the governance, risk management and metrics and targets pillars for April 2024 to March 2025. These disclosures are provided below.
Governance
Climate related issues form part of the trust’s Clinical and Operational Strategy. The equity and inclusion plan include promise 27 ‘’Deliver the NHS Green Plan and match commitments made by our local authorities to achieve net zero, whilst adapting our service modes to climate change’’. Progress on overall equity and inclusion plan is formally reported into the public health, patient involvement and partnerships committee (PHPIP), which then reports progress into the board. Out-briefs are presented to the board by the committee chair.
The board have received reports on progress against this promise. In May 2024, the board considered the ‘finish lines’ (outcomes) for all the promises and the overall focus of how they will be delivered (in this case, corporately). In September 2024, an outline in the promises ‘scorecard’ report which was an assessment of the delivery plan and the likelihood of delivery which was carried out for all 28 promises. This also took place at the board in November 2024, January 2025 and March 2025.
The delivery of promise 27 is undertaken by the sustainability group and progress is overseen by the estates and sustainability group which reports to clinical leadership executive (CLE). Progress and escalation is taken to CLE on matters in relation to promise 27. The director of strategic development is overall responsible for the management of the trust’s work on promise 27, bringing options and proposals through the respective governance structure.
Identifying and assessing climate-related risks
We identify climate-related risks as part of our overall risk management framework, considering both the immediate and longer-term implications of climate change. Our assessment process is embedded in existing risk reviews at service and corporate levels. Climate-related risks are identified through a mix of strategic planning and input from operational teams. They are then assessed using our standard scoring model based on likelihood and impact. The framework allows us to judge how material a risk is and how it compares to other threats we face across the organisation.
At this stage, climate-related risks are not among our highest rated or principal risks, but we recognise their increasing relevance. Given their potential to grow in significance over time, especially in relation to estate management, service continuity and community wellbeing, they are being monitored more closely.
Managing climate-related risks
Once we’ve identified climate-related risks, we decide how best to respond. We use the same core principles we apply to all risk types, deciding whether to mitigate the risk, transfer it, accept it, or put controls in place. These decisions are made in the context of how the risk aligns with our objectives and what options are realistically available to us.
In assessing and prioritising these risks, we make assumptions about the likely direction of climate policy, expected changes to the environment, and developments in national or local regulations. We use materiality as a guide, looking at how climate-related impacts could affect our services, reputation, and the people we support. We also refer to external frameworks and government guidance to help shape our approach and keep our understanding current.
Integration into overall risk management
Climate risks are not managed in isolation. They are considered as part of our overall risk management process, sitting alongside operational, clinical, financial, and strategic risks. These risks are reviewed through existing governance channels and included in directorate-level risk registers and corporate oversight discussions.
Although climate-related risks are not currently identified as one of our principal risks, we are continuing to strengthen how they are considered and integrated.
Metrics and targets
RDaSH has already made some progress towards reducing its carbon emissions from Scope 1 and 2 since 2010 (see Figure 3). In 2010, RDaSH produced 7,111 tonnes of carbon emissions and this has been successfully reduced by approximately 50% over the last 14 years. The carbon emissions now stand at 3,562 tonnes. In order to achieve NHS targets, we must cut our emissions further to reach an 80% reduction target by 2032. This means our emissions need to reach 1,422 carbon emissions by 2032, prior to reaching Net Zero in 2040.
Internally at RDaSH, it is felt that many of the “easy wins” have already been utilised in order to reach our current success with halving emissions. This implies that the journey to Net Zero will be much trickier, and potentially more costly, from now on.

With regards to the quantitative progress data of the carbon footprint, as an NHS foundation trust we are not required to disclose or develop processes to disclose scope 1, scope 2 and scope 3 emissions under the ‘metrics and targets pillar’ in the HM Treasury guidance as emissions estimates for the NHS in England are derived centrally by NHS England.
Our CO2 emission for business travel went up in the year April 2024 to March 2025 from 702 to 893 tonnes, an increase of 21.4%. In the year April 2025 to March 2026, we will be looking at business miles as part of the review of our remote working arrangements. The carbon intensity of our fleet decreased from 96 tonnes in the year April 2023 to March 2024 to 87 tonnes in the year April 2024 to March 2025, through the use of more efficient vehicles.
Our use of gas increased, and mean our emissions went from 1900 tonnes in the year April 2023 to March 2024 to 1915 tonnes in the year April 2024 to March 2025.
Directors report
The board of directors has a wide range of skills and experience and considers it is balanced and complete in its composition, and appropriate to the requirements of the trust, and is in line with the NHS England’s Code of Governance for NHS FTs and with our standing orders.
All directors are required to comply with the fit and proper persons test requirements (FFPR) to meet the requirements of the general conditions of the provider licence and are required to make an annual declaration of compliance in this regard. All Directors were considered to meet the requirements in year.
Board of directors profiles
There were a number of changes to board membership through the year, the details of which can be found in the remuneration report. The descriptions below of each director’s expertise and experience demonstrates the relevance of the skills, knowledge and expertise that each director brings to the trust. Where terms of office expire in the coming year necessary processes of extension or succession are in hand.
Kathryn Lavery, Non-Executive Chair
Term of office expires 30 November 2025.
Kath joined the trust as chair in December 2022. She was first appointed to an NHS board in 1998 and since then served as the chair of West Hull Primary Care Trust and NHS Hull, as a nonexecutive director of NAViGO (a community interest company which runs NHS mental health services in Northeast Lincolnshire) and as a Hull City Councillor.
Kath is currently also chair ACCIA Yorkshire and Humber Panel, chair of the Advisory Board Space2BHeard CIC HULL and non-executive director at Locala Community Interest Company.

Dave Vallance, Non-Executive Director, Vice Chair and Senior Independent Director
Term of office expires 13 December 2025.
Dave joined the trust as non-executive director in December 2019 and was re-appointed in December 2022.
Dave built up a vast range of HR experience through working for over 20 years with Walgreen Boots Alliance, and was latterly HR director, Global Brands.
He previously worked in the NHS for The Audit Commission for 5 years, evaluating the value for money of a range of health and local government organisations.
He has been a trustee of one of the largest UK Pension schemes, a school governor and holds a Master of Business Administration (MBA) and a BA in Organisation Studies.

Pauline Vickers, Non-Executive Director
Term of office expires 31 March 2026.
Pauline joined the board of directors in April 2021 and was reappointed by the council of governors in April 2023.
Prior to joining the trust, she was a non-executive director and senior independent director with Bradford Teaching Hospitals NHS Foundation Trust. She worked for Royal Mail since graduating in 1985 across a range of leadership and commercial executive roles, most recently as export director for Royal Mail’s International business. Pauline now enjoys a portfolio career as an accredited executive coach and is an end point assessor for the business sales degree apprenticeship courses at Leeds Trinity and Middlesex Universities.
She holds a degree in management science from the University of Manchester Institute of Science and Technology, a post graduate diploma in personnel training and development from Leeds Metropolitan University and is a Chartered Member of the Institute of Personnel and Development.

Sarah Fulton Tindall, Non-Executive Director
Term of office expires 31 December 2027.
Sarah joined the trust as a non-executive director in January 2022. She was reappointed this year.
She has a strong executive level professional services delivery background in the Higher Education sector. Sarah spent over 20 years in a wide range of leadership roles at the University of Sheffield, and more latterly advising universities both in the UK and overseas.
Sarah has extensive experience in leading successful organisation-wide strategy, business transformation and people talent growth.
In addition to her current role, Sarah is also a member of the patient participation group at a local GP practice and an Age UK Readers’ Panel member.
Sarah holds a BA (Hons) in politics and social policy from the University of Sheffield.

Janusz Jankowski, Non-Executive Director
Left the trust on 31 March 2025.
Janusz joined the trust as a non-executive director in December 2022.
Janusz has holistic leadership experience having served in health roles including mental wellbeing in the UK, European Union, North America, the Middle East and the Pacific Region as Deputy Vice Chancellor, National Clinical Advisor, and Academic Consultant Physician.
He is a strong and effective advocate of mental health and disability services having supported appropriate guidelines from the National Institute for Health and Care Excellence (NICE). He is also a successful, experienced, executive coach and mentor who, has helped improve institutional culture and the subsequent Care Quality Commission inspection outcomes.

Kathryn Gillatt, Non-Executive Director
Term of office expires 31 March 2026.
Kathryn joined the trust in April 2023 and became chair of audit committee 1 January 2024.
Kathryn is a graduate of Nottingham University and is a Chartered Accountant by profession. Her career to date includes roles as a finance and corporate services director in a number of sectors including frontline NHS and children’s services, the department for transport, community pharmacy services, the leisure industry, chemical manufacturing, audit and tax services. She is also a non-executive director at NHS Business Services Authority and chairs their audit and risk committee.

Rachael Blake, Non-Executive Director
Term expires 30 April 2027.
Rachael lives in Doncaster and joined the trust in May 2024.
She started her career by qualifying as a Registered General Nurse and has now amassed 40 years’ experience in the NHS, Local Government, voluntary and community sector and in the private sector in a range of roles from front line delivery to chief officer and board level positions.
She currently works in the rail industry as a people and transformation lead and is a local councillor with City of Doncaster Council. She was previously a non-executive director at North Lincolnshire and Goole NHS Foundation Trust.

Dr Richard Falk, Non-Executive Director
Term expires 30 November 2027.
Richard joined the board of directors in May 2024 as an associate non-executive director and was appointed by the council of governors in November 2024 as a full non-executive director.
He is a retired local GP and clinical leader with extensive experience working at PCT and CCG board level within the NHS and therefore has skills as both a commissioner and provider. After retirement from his NHS role Richard worked for nearly 3 years in Western Australia as a Medicare GP before returning to the UK in 2019.
Prior to joining RDASH he worked in an advisory capacity with Weldricks Pharmacy a local pharmaceutical services provider.

Toby Lewis, Chief Executive Toby
joined the trust in March 2023 from The King’s Fund where he was a senior visiting fellow in health inequalities, with a focus on poverty and inclusion health. He joined the NHS in 1994 and began his career in Worksop. He has worked in primary care, mental and community health, and hospitals in London, West Yorkshire and the West Midlands.
After working in Downing Street, he joined his first NHS board in 2005 and has served in executive roles since that time, including eight years as chief executive of an integrated care organisation in the Black Country. He helped establish a new medical school at Aston University and led work to use the apprenticeship levy to the benefit for often excluded populations, such as care leavers and those at risk of experiencing homelessness, creating jobs as a route to better health. He holds a Masters degree in Public Health from Edinburgh University and degrees in occupational psychology and history from Oxford and London.

Dr Diarmid Sinclair, Chief Medical Officer
Diarmid was formerly the deputy medical director (since March 2023) prior to becoming the chief medical officer in September 2024.
Diarmid joined the trust in 2015 as a Consultant Psychiatrist, although he spent time in the trust as a resident doctor before this. Prior to joining RDaSH he worked over South Yorkshire and the East Midlands as a psychiatrist having first completed his medical degree in London. He has led on the recruitment of international educated medical staff. Diarmid continues to work clinically part time as a Consultant Psychiatrist in the Crisis Resolution and Home Treatment Team.

Steve Forsyth, Chief Nursing Officer
Steve joined the trust in April 2024 from Birmingham and Solihull Mental Health NHS Foundation Trust where he was the chief nurse since October 2022. Prior to this Steve was the director of nursing at Betsi Cadwaladr University Health Board in North Wales.
Over the last two decades, Steve has worked in criminal justice, physical health, commissioning, and mental health services. He is a registered nurse in both adult nursing and mental health.
Steve is a member of the national global majority chief nurse officer group, an active and proud member of the Jabali network, the Nola Ishmael executive nurses’ group, Asian professionals National Alliance (APNA) and British Indian Nurses Association (BINA), the Gambian Police Force and a director, trustee for the African Caribbean Community Initiative.

Izaaz Mohammed, Executive Director of Finance and Estates
Izaaz joined RDaSH in August 2022 as deputy director of finance, becoming the executive director of finance and estates in July 2024 following a period on being the interim director. He has previously worked in senior finance roles across acute, community, and mental health providers in West Yorkshire.
Izaaz is a chartered accountant and a fellow of the Association of Chartered Certified Accountants (ACCA). Outside of work Izaaz is the chair of a school governing body, and trustee of a learning disability charity.

Carlene Holden, Executive Director of People and Organisational Development
Carlene was formally the deputy director of HR and learning at our trust and prior to up the role of director of people and organisational development in May 2024. Carlene held several senior roles in human resources and organisational development in local commissioner and provider trusts. Prior to joining the NHS in 2003 Carlene worked in a range of HR roles in the private sector.
Carlene is an experienced HR practitioner who has undertaken further academic studies in both employment law and management and leadership. Carlene is also a qualified coach and mediator.

Richard Chillery, Executive Chief Operating Officer
Richard took up the post of Chief Operating Officer in October 2023, from his previous role where he was Deputy Chief Operating Officer for Lancashire and South Cumbria NHS Foundation Trust. For part of his time with Lancashire he was a Poverty Truth Civic Commissioner with the Morecombe Bay Poverty Truth Commission. He was also a non-executive director with Sheffield Childrens NHS Foundation Trust, so part of their Unitary Board from June 2019 to December 2023.
Prior to these roles Richard has had a range of senior NHS management roles within acute, community and mental health services and has been a Technical Advisor with Public Health England. He has worked in Public Services both in the UK and New Zealand, since 1989.
Richard remains a registered social worker and has a range of different psychosocial training for working with children, young people and their families and spent much of his clinical career working in Child and Adolescent Mental Health Services.

Richard Banks, Director of Health Informatics
Richard was appointed to his current role in 2016. Before this he was the director of business assurance from 2009. He has had a number of senior roles since joining the trust in 2000, including as the director of performance, planning and service improvement, at the time the trust achieved Foundation status in 2007.
Prior to joining RDaSH he worked in local government, the Sheffield FHSA, Health Authority and Community Health Sheffield, before joining RDaSH in 2000 as Head of Planning.
Richard has a degree in economic and social history, a post graduate certificate in managing health and social care and has completed the Kings Fund top manager programme. In 2016 he gained an MSc in Health and Social Care leadership.

Philip Gowland, Director of Corporate Assurance and Board Secretary
Philip was appointed as director of corporate assurance in February 2016 having joined the trust as Head of Corporate Affairs in 2007. He has been the board secretary since 2009.
Prior to joining the trust Philip was internal audit manager for a number of NHS organisations having worked for Internal Audit Consortia across both South and West Yorkshire.
Philip is a member of the Institute of Chartered Secretaries and Administrators (ICSA); a qualified accountant (Chartered Institute of Public Finance and Accountancy CIPFA) and holds a degree in Accounting and Management Control from Sheffield Hallam University.

Joanne McDonough, Director of Strategic Development
Joanne joined the trust in April 2011 when the Community Services transferred into the trust from the Primary Care Trust in Doncaster.
Prior to that she worked with a range of public sector organisations on service improvement with the Audit Commission for 11 years including working with NHS Providers on improving mental health and physical health services.
Since joining the trust, Joanne has held a number of roles including deputy director for business assurance, head of business services unit and care group director for Doncaster. She moved into the director of strategic development role in 2020 which includes responsibility for communications. Joanne holds a Master of Business Administration (MBA).

Dr Judith Graham BEM QN, Director of Psychological Professionals and Therapies
After working as a clinical Consultant in the trust for a number of years Judith joined the board of directors in 2016. Judith was appointed as interim director of people and organisational development in 2019 and progressed to the substantive director for psychological professionals later that year. Since 2022 Judith has had expanded portfolio with inclusion of wider therapeutic professionals including allied health professionals and social work.
As well as her trust role, Judith has also held a number of national positions related to the work of health and social care. These have included board member on the NHS Confederations Mental Health Network Board, Clinical Fellow at NICE, Member of the FTSU National Advisory Panel and currently a trustee at the Queens Nursing Institute.
Judith is a registered mental health nurse, holds a Post Graduate Bachelor’s Degree in Forensic and Intensive Mental Health Care, a Post Graduate Master’s Degree in Cognitive Behavioural Psychotherapy, a second Master’s Degree in Advanced Clinical Practice, and a Professional Doctorate in Psychotherapy. Judith has chartered MCIPD status with the Chartered Institute of Personnel and Development, she has Accreditation as Master Practitioner and Executive Coach via the European Mentoring Coaching Council and has also completed the Kings Fund Top Managers programme.
During the year there were a number of changes to the board of directors as follows:
- Nicola McIntosh left the trust on 28 April 2024 after which Carlene Holden became the executive director of people and organisational development on the 1 May 2024.
- Ian Currell left the trust on 14 July 2024 after which Izaaz Mohammed became the executive director of finance and estates following a recruitment process on 1 July 2024 following a period on being the interim director.
- Dr Graeme Tosh, medical director left the trust on 31 August 2024, after which Dr Diarmid Sinclair became the chief medical officer.
- Dawn Leese, non-executive director stepped down from her role on 30 November 2024 when her final third term was completed.
In the year April 2023 to March 2024 the NExT director scheme was introduced into the trust and 2 successful candidates each commenced a 24-month placement. This scheme is a development programme created and designed to help find and support the next generation of talented people who are currently under-represented on our NHS boards into the non-executive roles.
Lea Fountain, NExT Director
Lea joined the trust as a NExT director in October 2023. She brings 25 years’ experience in engaging communities, influencing change and building reputation, through roles in the media, the NHS and local government.
She is currently associate director of communications at Cambridgeshire Community Services NHS Trust. Her previous communication and engagement leadership roles include Sheffield Children’s NHS Foundation Trust, Milton Keynes University Hospital FT and the Gibraltar Health Authority. She is a Chartered Institute of Public Relations (CIPR) chartered practitioner, committed to ethical working to bring meaningful changes to improve the experiences of service users and NHS staff.

Jyoti Mehan, NExT Director
Jyoti joined the trust as a NExT director in April 2023. She has broad background in public and private sector healthcare provision, specifically in operational and performance improvement. Jyoti is the CEO of an at scale multi-site General Practice provider.
Jyoti holds a BA in Business Economics and is currently undertaking an MBA.
Jyoti stepped down from her role in February 2025 to take up the position of a nonexecutive director at another NHS trust, the precise purpose of the entry programme.

Director independence and register of interests
The trust is committed to ensuring that the board of directors is comprised of a majority of independent non-executive directors who objectively challenge management. Our nonexecutive directors provide a wide range of skills and experience. They bring strong, independent oversight and judgement on issues of strategy, performance and risk through their contribution at board and committee meetings. The board of directors considers that throughout the year each non-executive director was independent in character and judgement.
The council of governors is responsible for all decisions to reappoint non-executive directors and is supported in its consideration by the recommendations it receives from the chair and the nominations committee. Non-executive directors declare their interests and in the unlikely event that such interests conflict with those of the trust, then the individual would be excluded from any discussion and decision relating to that specific matter.
All board directors are required to disclose their relevant interests as defined in our constitution. These are recorded in a publicly available register that is formally reported to the board of directors at the beginning of each meeting. A copy of the full register of declarations is available on the website or on request from the director of corporate assurance, board secretary at Woodfield House, Tickhill Road Hospital Site, Balby, Doncaster DN4 8QN or email rdash.doi@nhs.net.
Furthermore, all members of the Board of Directors are subject to the requirements of the fit and proper persons test which is considered on appointment and on an annual basis. All Directors were deemed to meet these requirements.
Role of the board of directors
The board of directors acts as a unitary board and has corporate responsibility for the decisions it makes. It is the legally responsible body for the delivery of high quality, effective services, and for making decisions relating to the strategic direction, financial control and performance of the trust. It comprises both executive directors and nonexecutive directors:
- Eight non-executive directors (including the chair), bring independent judgement and scrutiny to the board of directors to make sure that sound and well informed decisions are made.
- Six executive directors (including the chief executive), responsible for implementing trust policy and for the effective day-to-day running of the organisation.
In addition, the director of health informatics, director of psychological professions and therapies, director of strategic development and director of corporate assurance attend each board of directors meeting.
The composition of the board of directors is in accordance with our constitution and it is appropriately composed to fulfil its statutory and constitutional function and to meet the terms of the licence issued by NHS England.
There is a clear division of responsibilities between the chair and chief executive. The chair has throughout the year been responsible for the effective working of the board of directors, and for ensuring the board of directors has a strategy that delivers a service that meets the expectations and requirements of the communities we serve, ensuring all directors are able to play their full part in the strategic direction of the trust and its performance. The chair also facilitates the contribution of non-executive directors and their constructive relationships with the Executives. The chair also chairs the council of governors meetings and ensures that there is effective communication between the board of directors and the council of governors and that, where necessary, the views of the governors are obtained and considered by the board of directors. Non-executive directors attend the council of governors meetings along with the chief executive and director of corporate assurance. The chair supported by the senior independent director, also seeks to foster a strong, engaging relationship between the board of directors and the council of governors. There is frequent attendance at the board of directors by governors and during 2024 governors were identified as members of the Board’s committees in line with promise 5 to involve our communities at every level of decision making in our trust. Further details of governors’ involvement at the trust are provided.
This engagement helps ensure that all parties maintain an understanding of the views and aspirations of the trust and our members and contribute to the future development of the organisation. Furthermore, the Board of Directors meetings always include a patient or staff member story – allowing the Board members the opportunity to hear first-hand, the experiences of others. During the year the stories have focused on experiences of accessing child and adolescent mental health services (CAMHS) in Rotherham, the apprenticeship route to career development, the use of Restrictive Interventions and the work across the trust to reduce their use; and accessing learning disabilities services in North Lincolnshire.
The chief executive is responsible for all aspects of the management of the trust. This includes the leadership of the executive team and for implementing our clinical and organisational strategy and delivering our overall objectives, and for ensuring that we have an appropriate risk management system in place. While the executive directors are responsible for the day-to-day operational management of the trust, the non-executive directors share the corporate responsibility for ensuring that the organisation is run efficiently, economically and effectively. Non-executive directors use their expertise, interest and experience, and attend the meetings of the board and its committees to achieve this. Regular involvement in the peer review process and service and site visits are undertaken by all directors in order to gain a more rounded understanding of the services being delivered and the issues faced by our colleagues in those services.
The chair and chief executive continue to review the board of directors balance, completeness and appropriateness, and ensure that this is maintained when new appointments are made. During the year, our performance, clinically and financially was closely monitored by the board of directors through the presentation and discussion of key performance information at every one of its meetings, in the integrated quality and performance report (IQPR).
The board of directors acknowledges its responsibility for preparing the annual report and accounts and considers that, taken as a whole, they are fair, balanced and understandable and provide the information necessary for patients, regulators and other stakeholders to assess the trust’s performance, business model and strategy. As far as the board of directors are aware, there is no relevant audit information of which the External Auditors are unaware. Each of the directors has taken all the steps they ought to have taken as directors, in order to make themselves aware of any relevant audit information and to establish that the trust’s auditor is aware of that information. Attendance by directors at the board’s meetings in the year is presented in the board of directors’ attendance table at the end of this section.
The terms of reference of the board and its committees are focused in line with Clinical and Organisational Strategy and the forward trajectory of the trust. This included the introduction of new committee, public health, patient involvement and partnerships in January 2024 and dissolvement of the commissioning committee in April 2024. Each committee provides a report to the board of directors after every meeting outlining key areas of discussion.
Audit Committee
The Audit Committee provides the board of directors with a means of independent and objective review of financial, clinical, corporate, education and research governance and risk management across the whole of the trust’s activities.
The committee has delegated responsibility from the board of directors for specific areas of concern and to work alongside other committees to assess control strengths, weaknesses and themes. The committee is a non-executive body of three members, one with recent and relevant financial experience. Also in regular attendance at meetings are the director of finance and estates, chief nursing officer, director of corporate assurance and board secretary, representatives from internal and external audit and the trust’s anti-crime specialist.
Internal audit and anti-crime services are provided by 360 Assurance who predominantly focus on delivery of services to the NHS and associated partners, 360 Assurance has a strong reputation of providing quality services.
External audit is provided by Deloitte and the year of April 2024 to March 2025 was their eighth year since their appointment. A protocol is in place following agreement with the Council of Governors for the engagement of the external auditors to undertake work outside of the Audit Code. The agreement includes provisions to ensure continued external auditor independence.
The significant risks identified by Deloitte for their audit are validity of accruals, management override of controls and property valuation.
In addition to the board and its committee, as part of the operating model, there is a clinical leadership executive with a range of supporting groups in place. The meeting structure is depicted in the diagram overleaf.
Governance structure
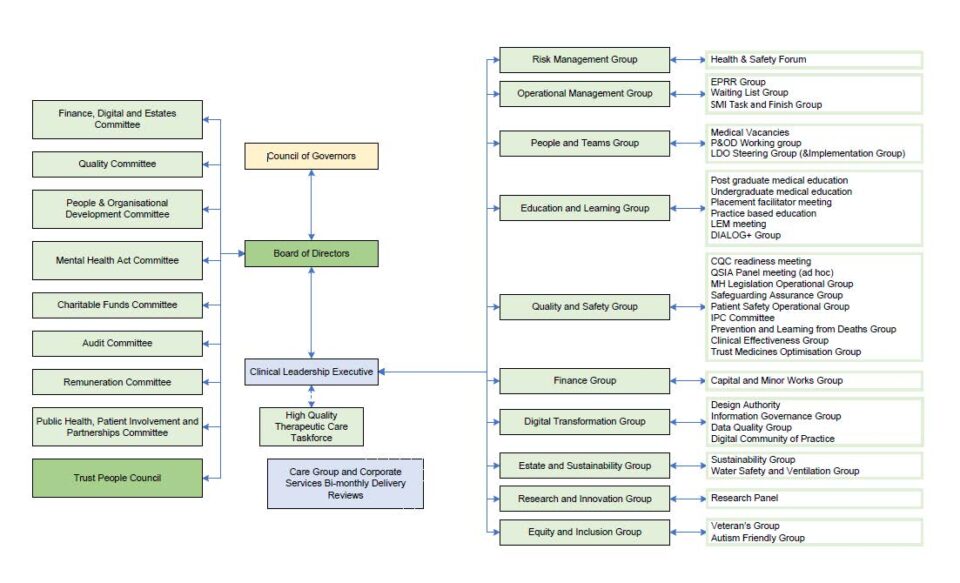
Structure overview
The following committee’s report to the board of directors.
Committee's reporting to the board of directors
- Finance, Digital and estates Committee.
- Quality Committee.
- People and Organisational development Committee.
- Mental Health Act Committee.
- Charitable Funds Committee.
- Audit Committee.
- Remuneration Committee.
- Public Health, Patient Involvement and Partnerships Committee.
- Trust People Council.
The board of directors reports and is reported to be the council of governors and clinical leadership executive. The high quality therapeutic care taskforce report also report to the clinical leadership executive. Care group and corporate services have bi-monthly delivery reviews.
The following reporting to the clinical leadership executive:
Risk Management Group
Health and safety forum.
Operational management group
- Emergency preparedness, resilience and response (EPRR) group.
- Waiting list group.
- Serious mental ilnness task and finish group.
People and teams group
- medical vacancies.
- People and organisational development working group.
- Leadership development offer (LDO) steering group and implementation group.
Education and learning group
- Post graduate medical education.
- Undergraduate medical education
- Placement facilitator group.
- Practice based education.
- Local engagement meeting.
- DIALOG+ group.
Quality and safety group
- Care Quality Commission readiness meeting.
- Quality and safety impact assessment (QSIA) panel meeting (ad hoc).
- Mental health legislation operational group.
- Safeguarding assurance group.
- Patient safety operational group.
- Infection, Prevention and Control Committee.
- Prevention and learning from deaths group.
- Clinical effectiveness group.
- Trust medicines optimisation group.
Finance group
Capital and minor works group.
Digital transformation group
- Design authority.
- Information governance group.
- Data quality group.
- Digital community of practice.
Estate and sustainability group
- Sustainability group.
- Water safety and ventilation group.
Research and innovation group
Research panel.
Equity and inclusion group
- Veteran’s group.
- Autism friendly group.
The table overleaf shows the attendance of the board of directors at the board, its committees during the financial year 1 April 2024 to 31 March 2025. Details on the council of governors is available at the council of governors.
| Director | Title | Board of directors | Audit | Renumeration | Mental Health Act | Charitable funds | Public health, patient involvement and partnerships | Quality | People and organisational development | Finance, digital and estates |
|---|---|---|---|---|---|---|---|---|---|---|
| Kathryn Lavery | Chair | 5 out of 6 | 3 out of 3 | 4 out of 4 | ||||||
| Dave Vallance | Non-executive director and vice chair | 4 out of 6 | 3 out of 3 | 5 out of 6 | 5 out of 6 | 5 out of 6 | ||||
| Dawn Leese | Non-executive director | 4 out of 4 | 3 out of 4 | 1 out of 2 | 4 out of 4 | 4 out of 4 | ||||
| Pauline Vickers | Non-executive director | 5 out of 6 | 6 out of 6 | 2 out of 3 | 4 out of 4 | 4 out of 6 | 6 out of 6 | |||
| Sarah Fulton Tindall | Non-executive director | 6 out of 6 | 2 out of 3 | 6 out of 6 | 3 out of 4 | 2 out of 2 | 6 out of 6 | |||
| Dr Janusz Jankowski | Non-executive director | 0 out of 6 | 2 out of 3 | 5 out of 6 | 6 out of 6 | 5 out of 6 | ||||
| Kathy Gillatt | Non-executive director | 6 out of 6 | 6 out of 6 | 2 out of 3 | 4 out of 4 | |||||
| Rachael Blake | Non-executive director | 3 out of 6 | 2 out of 3 | 2 out of 2 | 4 out of 5 | 4 out of 5 | ||||
| Dr Richard Falk | Non-executive director | 4 out of 6 | 2 out of 2 | 2 out of 3 | 1 out of 2 | 2 out of 2 | ||||
| Toby Lewis | Chief executive | 6 out of 6 | 6 out of 6 | 4 out of 4 | 5 out of 6 | |||||
| Steve Forsyth | Chief nursing officer | 6 out of 6 | 4 out of 5 | 4 out of 4 | 6 out of 6 | 4 out of 6 | ||||
| Dr Graeme Tosh | Medical director | 2 out of 2 | 1 out of 3 | 2 out of 2 | 2 out of 2 | |||||
| Dr Diarmid Sinclair | Chief medical officer | 4 out of 4 | 3 out of 3 | 2 out of 4 | 4 out of 4 | |||||
| Ian Currell | Director of finance and estates | 1 out of 1 | 1 out of 1 | 1 out of 1 | ||||||
| Izaaz Mohammed | Director of finance and estates | 5 out of 5 | 4 out of 5 | 4 out of 4 | 5 out of 5 | |||||
| Nicola McIntosh | Director of people and organisational development | 1 out of 1 | 1 out of 1 | |||||||
| Carlene Holden | Director of people and organisational development | 5 out of 5 | 6 out of 6 | 5 out of 5 | 5 out of 5 | |||||
| Richard Chillery | Chief operating officer | 6 out of 6 | 6 out of 6 | 5 out of 6 | ||||||
| Richard Banks | Director of health informatics | 5 out of 6 | 5 out of 6 | 5 out of 6 | ||||||
| Philip Gowland | Director of corporate assurance and board secretary | 6 out of 6 | 5 out of 6 | |||||||
| Joanne McDonough | Director of strategic development | 6 out of 6 | 4 out of 4 | 6 out of 6 | ||||||
| Dr Judith Graham | Director of psychological professionals and therapies | 5 out of 6 | 5 out of 6 | 3 out of 6 | 5 out of 6 |
With the permission of the chair, and to allow for personal and work commitments during the year, Dr Jankowski did not attend the board of directors meetings in person, but joined those meetings via digital link in order to observe them.
Remuneration report
In accordance with the requirements of the HM Treasury Financial Reporting Manual and reporting requirements issued by NHS England, this report is in three parts:
- Annual statement on remuneration describes the major decisions on senior managers’ remuneration as well as any substantial changes to senior managers’ remuneration which were made during the year and the context in which those changes occurred and decisions taken.
- Senior managers’ remuneration policy sets out information about the trusts policy.
- Annual report on remuneration includes details about senior managers’ service contracts and sets out other matters such as committee membership, attendance and the business transacted.
A senior manager is defined as “Those persons in senior positions having authority or responsibility for directing or controlling the major activities of the foundation trust.” For the trust, the report covers eight non-executive directors (including the chair), six executive directors (including the chief executive), the director of health informatics, director of corporate assurance, director of psychological professions and therapies and the director of strategic development, these are the senior managers.
Whilst the annual report is prepared on a group basis, Flourish CIC and the Charity are not considered to be material and as such none of the senior managers of Flourish CIC meet the definition of senior manager above and are not therefore included in this Remuneration Report. Similarly, given their informal role with the trust, the two named NExT directors are also not considered to be within the definition of ‘senior manager’ for the purposes of this Remuneration Report.
Details of the directors including their start date in their role and their relative experience and expertise are on board of directors profiles. For detail on the number of meetings attended please refer to the remuneration report.
Annual statement on remuneration
The trust has two committees responsible for reviewing the remuneration of the senior managers:
- Nominations committee of the council of governors – chair and non-executive directors (as detailed in the directors report on board of directors profiles)
- Remuneration committee – executive directors and other directors (as detailed in the directors report on board of directors profiles)
The two committees aim to ensure that senior managers’ remuneration is set appropriately taking into account relevant market conditions and to ensure that the senior managers are fairly rewarded for their individual contribution to the trust, having proper regard for affordability based on the corporate performance of the trust.
In setting the remuneration, the committees take due account of any guidance issued for NHS staff regarding the level of pay inflation which may be awarded, for example the annual agenda for change and very senior manager (VSM) guidance but does not consult with those employees. The committee also takes due account of national benchmarking data collated particularly that distributed annually by NHS Providers. This allows for sector and geographical comparisons to be made.
During the year April 2024 to March 2025 the nominations committee were involved in three new appointments to the role of non-executive director and one re-appointment:
- appointment of non-executive director, Rachael Blake
- appointment of non-executive director, Dr Richard Falk
- appointment of non-executive director, Maria Clark (from 1 May 2025)
- re-appointment of non-executive director, Sarah Fulton Tindall
The remuneration committee met on 3 occasions during the year April 2024 to March 2025. The key matters discussed at the meetings included:
- Changes to the executive group, progress with PDRs and objectives and performance specific to the Chief Executive only
- Annual review of remuneration
In the year April 2024 to March 2025, 16 board members received expenses and the total amount reimbursed was approximately £13,025 (£10,845 in the year Aril 2023 to March 2024). Senior managers’ remuneration policy In any recruitment process undertaken, the trust utilises open, widely advertised recruitment processes, with on occasion external professional support, to ensure the best candidates are identified and appointed.
For information on the policy for equality, diversity and inclusion please refer to staff policies and actions applied during April 2024 to March 2025 and equality, diversity and inclusion within the staff report.
Non-executive directors
The remuneration of the chair and non-executive directors has, since 2019, been in line with the guidance document entitled “Structure to align remuneration for chairs and nonexecutive directors of NHS trusts and NHS foundation trusts Implementation document: November 2019”. No review of the chair and non-executive director remuneration has since taken place. The trust, and specifically the nominations committee of the council of governors, awaits a further update to that guidance, although at the present time no agreed date for such has been published.
The component of the remuneration packages for the non–executive directors is shown overleaf:
| Element | Policy |
|---|---|
| Fee payable | A “spot fee” which is in line with the guidance document referred to above |
| Additional fee | The senior independent director receives an additional £1,000; the vice chair receives an additional £1,000; and the chair of the audit committee an additional £2,000 |
| Percentage uplifts (cost of living increase) | The current remuneration is line with the guidance document entitled Structure to align remuneration for chairs and non-executive directors of NHS trusts and NHS foundation trusts November 2019, no uplift has been considered or actioned since 2020 |
| Travel | Travel and subsistence expenses are reimbursed and paid with remuneration via payroll |
| Pension contributions | Non-executive directors do not have access to the NHS pension scheme |
| Other remuneration | None |
The chair and non-executive directors do not have a notice period.
The letters of appointment include no provisions or obligations which could give rise to, or impact on, remuneration payments or payments for loss of office.
Executive directors
The component of the remuneration packages for these senior managers is shown below:
| Element | Policy |
|---|---|
| Salary | A “spot” salary which is reviewed annually; the setting of that salary and the subsequent review are undertaken with reference to relevant guidance and other related information as described above, this is the maximum amount that will be paid; there are no provisions for the recovery of sums paid or for the withholding of the payments |
| Salary (medical director) | The initial post holder’s (Dr Graeme Tosh) total remuneration comprises of a ‘spot’ salary, for the role of medical director, together with a Level 3 clinical excellence award and separate contract for clinical duties performed for the Rotherham Adult Mental Health Care Group (including a 3% on-call allowance) |
| Percentage uplifts (cost of living increase) | Reviewed annually by the remuneration committee taking into consideration national pay awards, benchmarking data and the related financial implications |
| Travel benefits | Travel and subsistence expenses are reimbursed and paid with salary via payroll |
| Annual performance related bonuses | The chief executive’s contract includes 10% of earn back pay (a requirement to meet agreed performance objectives to earn back an element of base pay placed at risk; subject to an annual review and agreement between the chair and the chief executive with the outcome reported to the remuneration committee) |
| Long-term performance related bonuses | No long-term performance related bonuses are paid |
| Pension related benefits | Executive directors and directors can access the NHS pension scheme |
The current senior managers are on substantive contracts that incorporate a six month notice period, except for the director of health informatics, director of strategic development, director of psychological professions and therapies and the director of corporate assurance and board secretary who have a three month notice period.
The contracts include no provisions or obligations which could give rise to, or impact on, remuneration payments or payments for loss of office.
Annual report on remuneration
The council of governors has responsibility for the appointment, re-appointment, remuneration and appraisal of the chair and non-executive directors. The work to discharge that responsibility is undertaken by the nominations committee which comprises seven governors (four service user and or carer or public governors and three appointed or staff governors).
The nominations committee is chaired by the lead governor, Joan Cox, community services, carer and is supported administratively by the director of corporate assurance and board secretary. Non-executive directors are appointed for a fixed term of office, following an open, advertised recruitment campaign in which representatives of the nominations committee join the chair and an external assessor to form an interview panel that recommends an appointment to the full council of governors.
The remuneration committee is chaired by Kath Lavery, chair. The remaining members of the committee are the other non- executive directors. By invitation from the chair of the committee, the chief executive attends meetings as does the director of corporate assurance and board secretary and the executive director for people and organisational development.
The remuneration committee has delegated responsibility for all aspects of remuneration and terms of service for the executive directors and directors. Its responsibility includes all aspects of salary, provision for other benefits including pensions, arrangements for termination of employment, and other contractual terms.
The chief executive is remunerated at a level greater than £150,000 (this equates to the Prime Minister’s ministerial and parliamentary salary). The remuneration paid to this director is considered to be reasonable for the post given the relative position in terms of benchmarking with similar foundation trusts.
During the year, neither the remuneration committee nor the nominations committee sought nor received advice or services from any person that materially assisted their consideration of these matters.
| Director | Salary (bands of £5,000) | Taxable benefits total to nearest £100 | Performance pay and bonuses (bands of £5000) | Long term performance pay and bonuses (bands of £5000) | All pension related benefits (bands of £2,500) | Total (bands of £5,000) |
|---|---|---|---|---|---|---|
| Kathryn Lavery, Chair | 40 to 45 | 0 | 0 | 0 | 0 | 40 to 45 |
| Toby Lewis, Chief executive | 175 to 180 | 0 | 15 to 20 | 0 | 25 to 27.5 | 220 to 225 |
| Graeme Tosh, Medical director: 1 April to 31 August 2024 | 70 to 75 | 0 | 0 | 0 | 0 | 70 to 75 |
| Diarmid Sinclair, Chief medical officer: from 1 September 2024 | 115 to 120 | 0 | 0 | 0 | 120 to 122.5 | 235 to 240 |
| Steve Forsyth, Chief nursing officer: from 1 April 2024 | 125 to 130 | 9,000 | 0 | 0 | 122.5 to 125 | 255 to 260 |
| Ian Currell, Director of finance and estates: 1 April to 14 July 2024 | 45 to 50 | 0 | 0 | 0 | 0 | 45 to 50 |
| Izaaz Mohammed, Director of finance and estates: from 5 June 2024 | 100 to 105 | 13,500 | 0 | 0 | 22.5 to 25 | 135 to 140 |
| Richard Chillery, Chief operating officer | 140 to 145 | 0 | 0 | 0 | 132.5 to 135 | 275 to 280 |
| Judith Graham, Director of psychological professionals and therapies | 100 to 105 | 9,400 | 0 | 0 | 55 to 57.5 | 165 to 170 |
| Nicola McIntosh, Director of people and organisational development: 1 to 28 April 2024 | 10 to 15 | 0 | 0 | 0 | 7.5 to 10 | 15 to 20 |
| Carlene Holden, Director of people and organisational development: from 1 May 2024 | 95 to 100 | 0 | 0 | 0 | 167.5 to 170 | 265 to 270 |
| Joanne McDonough, Director of strategic development | 110 to 115 | 0 | 0 | 0 | 20 to 22.5 | 130 to 135 |
| Richard Banks, Director of health informatics | 105 to 110 | 0 | 0 | 0 | 10 to 12.5 | 120 to 125 |
| Philip Gowland, Director of corporate assurance and board secretary | 105 to 110 | 0 | 0 | 0 | 12.5 to 15 | 120 to 125 |
| Dave Vallance, Non-executive director | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
| Dawn Leese, Non-executive senior independent director: 1 April to 30 November 2024 | 5 to 10 | 0 | 0 | 0 | 0 | 5 to 10 |
| Pauline Vickers, Non-executive director | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
| Sarah Fulton Tindall, Non-executive director | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
| Janusz Jankowski, Non-executive director | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
| Kathryn Gillatt, Non-executive director | 15 to 20 | 0 | 0 | 0 | 0 | 15 to 20 |
| Rachael Blake, Non-executive director | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
| Richard Falk, Non-executive director | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
The above data is subject to audit.
Three executive directors leased a vehicle through the trust’s salary sacrifice lease car scheme in in April 2024 to March 2025. These salary sacrifice arrangements are disclosed as taxable benefits in the remuneration table.
Executive directors are members of the NHS defined benefit pension scheme managed by NHS Pension Authority. All pension related benefits’ disclosed above show the increase in ‘lifetime’ pension which has arisen in the year April 2024 to March 2025; it is not the amount paid into the pension during the year. The sum reported reflects the amount by which the annual pension received on retirement age has increased in April 2024 to March 2025, multiplied by 20 (the average number of years a pension is paid to members of the NHS scheme following retirement). ‘All pension related benefits’ exclude employee contributions as directed in the Finance Act 2004. The figures tend to be highest when an individual is promoted to an executive director role within the current or previous financial year.
Where a salary amount sits exactly on a pay boundary then the salary is reported at the lower band. For example, if an employee had a salary of £50,000, they would be shown in the salary band (£’000) 45 to 50.
Where an employee has been in post for part of the year, their pay and pension amount are time apportioned to reflect time in post. Any start and end dates are shown in the table April 2024 to March 2025.
Dr Tosh spent circa 16% of his time on clinical work and Dr Sinclair undertakes, on average, two clinical sessions a week. The remainder of their respective time was as the Medical Director.
A proportion (10%) of the chief executive’s salary is performance related, the table below set out the objectives for April 2024 and March 2025:
| Objective | Narrative description | Weighting | Agreed outcome and actual performance | Achievement in April 2024 and March 2025 |
|---|---|---|---|---|
| 1 | Personal development or wellbeing | 5% | Public health masters’ degree achieved | Yes |
| 2 | Delivery of MHLDA Collab goals | 5% | Success with 2 of 4 ambitions set by collaborative board | Yes |
| 3 | Embed safety plan into trust | 25% | Drive towards good rating in Care Quality Commission assessment | No |
| 4 | Introduce LHDs (part of L and E plan) | 10% | Successful launch after evaluated pilot | Yes |
| 5 | Develop executive team and wider TLC | 20% | Launch of Leadership development offer, and improved EG performance via PDR scores | Yes |
| 6 | Safely achieve agency reduction plan | 10% | Meet agency budget at heart of trust CIP plan | Yes |
| 7 | Deliver stipulated subset of promises | 25% | Progress with promise 3, 4, 5, 9, 14, 19, 25 and 26 | Yes |
New national very senior managers (VSM) guidance removes as outdated the national requirement for “clawback” clauses: and from 2025 and 2026 no performance related pay will apply to any trust directors
| Names and titles | Salary and fees paid by the trust (bands of £5,000) £000 | Salary and fees associated to director role at the trust (bands of £5,000) £000 | Taxable benefits (rounded to the nearest £100) £s | Annual Performance related bonuses (bands of £5,000) £000 | Long-term Performance related bonuses (bands of £5,000) £000 | Pension related benefit (bands of £2,500) £000 | Total (bands of £5,000) £000 |
|---|---|---|---|---|---|---|---|
| Kathryn Lavery, Chair | 40 to 45 | 40 to 45 | 0 | 0 | 0 | 0 | 40 to 45 |
| Toby Lewis, Chief Executive | 185 to 190 | 185 to 190 | 0 | 0 | 0 | 0 | 185 to 190 |
| Sheila Lloyd, Director of Nursing and Deputy Chief Executive | 145 to 150 | 145 to 150 | 0 | 0 | 0 | 77.5 to 80 | 225 to 230 |
| Graeme Tosh, Medical Director | 175 to 180 | 175 to 180 | 0 | 0 | 0 | 0 | 175 to 180 |
| Ian Currell, Director of Finance and Estates | 140 to 145 | 140 to 145 | 0 | 0 | 0 | 0 | 140 to 145 |
| Richard Chillery, Chief Operating Officer (from 9 October 2023) | 65 to 70 | 65 to 70 | 0 | 0 | 0 | 15 to 17.5 | 80 to 85 |
| Marie Watkins, Interim Chief Operating Officer (1 April 2023 to 8 October 2023) | 70 to 75 | 55 to 60 | 0 | 0 | 0 | 37.5 to 40 | 95 to 100 |
| Judith Graham, Director of Psychological Professionals and Therapies | 90 to 95 | 90 to 95 | 0 | 0 | 0 | 0 | 90 to 95 |
| Nicola McIntosh, Director of People and Organisational Development | 110 to 115 | 110 to 115 | 0 | 0 | 0 | 30 to 32.5 | 140 to 145 |
| Joanne McDonough, Director of Strategic Development | 105 to 110 | 105 to 110 | 0 | 0 | 0 | 0 | 105 to 110 |
| Richard Banks, Director of Health Informatics | 100 to 105 | 100 to 105 | 0 | 0 | 0 | 0 | 100 to 105 |
| Philip Gowland, Director of Corporate Assurance and Board Secretary | 100 to 105 | 100 to 105 | 0 | 0 | 0 | 0 | 100 to 105 |
| Dave Vallance, Non-Executive Director | 10 to 15 | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
| Dawn Leese, Non-Executive Senior Independent Director | 10 to 15 | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
| Justin Shannahan, Non-Executive Director | 10 to 15 | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
| Pauline Vickers, Non-Executive Director | 10 to 15 | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
| Sarah Fulton Tindall, Non-Executive Director | 10 to 15 | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
| Janusz Jankowski, Non-Executive Director | 10 to 15 | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
| Kathryn Gillatt, Non-Executive Director | 10 to 15 | 10 to 15 | 0 | 0 | 0 | 0 | 10 to 15 |
Pension entitlement (subject to audit)
The pension benefit table provides further information on the pension benefits accruing to the individual.
As non-executive directors do not receive pensionable remuneration, there are no entries in respect of pensions for non-executive directors.
| Name and title | Real increase in pension at pension age (bands of £2,500) real increase in pension (£000) | Lump sum at pension age (bands of £2,500) (£000) | Total accrued pension at pension age at 31 March 2025 (bands of £5,000) (£000) | Lump sum at pension age related to accrued pension at 31 March 2025 (bands of £5,000) (£000) | Cash equivalent transfer value at 1 April 2024 (£000) | Real increase in cash equivalent transfer value (£000) | Cash equivalent transfer value at 31 March 2025 (£000) | Employers contribution to stakeholder pension (£000) |
|---|---|---|---|---|---|---|---|---|
| Toby Lewis, Chief Executive | 2.5 to 5 | 0 | 75 to 80 | 200 to 205 | 1576 | 31 | 1737 | 0 |
| Graeme Tosh, Medical director: 1 April to 31 August 2024 0 | 0 | 0 | 40 to 45 | 100 to 105 | 809 | 0 | 839 | 0 |
| Diarmid Sinclair, Chief medical officer: from 1 September 2024 | 5 to 7.5 | 12.5 to 15 | 35 to 40 | 95 to 100 | 507 | 101 | 737 | 0 |
| Ian Currell, Director of finance and estates: 1 April to 14 July 2024 | 0 | 0 | 60 to 65 | 165 to 170 | 1440 | 0 | 1520 | 0 |
| Izaaz Mohammed, Director of finance and estates: from 5 June 2024 | 0 to 2.5 | 0 | 5 to 10 | 0 | 59 | 8 | 89 | 0 |
| Richard Chillery, Chief Operating Officer | 5 to 7.5 | 12.5 to 15 | 55 to 60 | 155 to 160 | 1219 | 156 | 1474 | 0 |
| Steve Forsyth, Chief nursing officer: from 1 April 2024 | 5 to 7.5 | 10 to 12.5 | 45 to 50 | 110 to 115 | 719 | 108 | 891 | 0 |
| Judith Graham, Director of Psychological Professionals and Therapies | 2.5 to 5 | 2.5 to 5 | 25 to 30 | 65 to 70 | 447 | 45 | 534 | 0 |
| Nicola McIntosh, Director of people and organisational development: 1 to 28 April 2024 | 0 to 2.5 | 0 | 0 | 15 to 20 | 250 | 10 | 278 | 0 |
| Carlene Holden, Director of people and organisational development: from 1 May 2024 | 7.5 to 10 | 17.5 to 20 | 25 to 30 | 70 to 75 | 373 | 155 | 580 | 0 |
| Joanne McDonough, Director of Strategic Development | 0 to 2.5 | 0 | 25 to 30 | 0 | 431 | 19 | 493 | 0 |
| Richard Banks, Director of Health Informatics | 0 to 2.5 | 0 | 50 to 55 | 130 to 135 | 1100 | 19 | 1207 | 0 |
| Philip Gowland, Director of Corporate Assurance and Board Secretary | 0 to 2.5 | 0 | 40 to 45 | 105 to 110 | 847 | 17 | 934 | 0 |
Pensions figures included in the above table are for senior managers that have pensions paid directly by RDaSH and include all of their NHS Service not just pension payments that relate to April 2024 to March 2025.
Where an employee has been in post for part of the year, their pension amount is time apportioned to reflect time in post. Graeme Tosh, Diarmid Sinclair, Ian Currell, Izaaz Mohammed, Nicola McIntosh and Carlene Holden were in post for part of the year.
The cash equivalent transfer value (CETV) is the estimated amount that would transfer if the pension benefits were moved from one scheme to another.
The pension calculation uses an inflation value of 6.7% on previous year values which can make previous pension, lump sum and CETV values appear to have decreased in the year April 2024 to March 2025. Where these values are negative they are shown as zero.
This information has been audited.
Payments for loss of office
In the year to 31 March 2025, no payments were made by the trust to senior managers for loss of office. This is the same as for the year April 2023 to March 2024.
Payments to past senior managers
In the year to 31 March 2025, no payments were made by the trust to past senior managers. This is the same as for the year April 2023 to March 2024.
Fair pay disclosures (subject to audit)
NHS foundation trusts are required to disclose the relationship between the remuneration of the highest-paid director in their organisation and the lower quartile, median and upper quartile remuneration of the organisation’s workforce.
The banded remuneration for the highest-paid director in the organisation in the financial year April 2024 to March 2025 was £195,000 to £200,000 (for April 2023 to March 2024 it was £185,000 to £190,000). This is a change between years of 5%. Another director appointed part way through the year, had annualised remuneration as a director within the £200,000 to £205,000 banding, which is a change between years of 8%.
For employees of the trust as a whole, the range of remuneration in 2024 and2025 was from £22,817 to £258,500 (2023 and 2024 £15,350 to £311,695). The percentage change in average employee remuneration (based on total for all employees on an annualised basis divided by full time equivalent number of employees) between years is 3.4%. 4 employees received remuneration in excess of the highest-paid director by annualised remuneration in 2024 and 2025 (11 in 2023 and 2024).
The remuneration of the employee at the 25th percentile, median and 75th percentile is set out below. The pay ratio shows the relationship between the total pay and benefits of the highest paid director (excluding pension benefits) and each point in the remuneration range for the organisation’s workforce.
| Highest paid director by actual remuneration | 25th percentile | Median | 75th percentile |
|---|---|---|---|
| Salary component of pay | 25,674 | 36,483 | 44,962 |
| Total pay and benefits excluding pension benefits | 26,877 | 36,351 | 45,304 |
| Pay and benefits excluding pension: pay ratio for highest paid director | 7.35:1 | 5.43:1 | 4.36:1 |
| Highest paid director by annualised remuneration | 25th percentile | Median | 75th percentile |
|---|---|---|---|
| Salary component of pay | 25,674 | 36,483 | 44,962 |
| Total pay and benefits excluding pension benefits | 26,877 | 36,351 | 45,304 |
| Pay and benefits excluding pension: pay ratio for highest paid director | 7.53:1 | 5.56:1 | 4.46:1 |
| Highest paid director by annualised remuneration | 25th percentile | Median | 75th percentile |
|---|---|---|---|
| Salary component of pay | 24,336 | 34,581 | 42,618 |
| Total pay and benefits excluding pension benefits | 25,147 | 34,581 | 42,912 |
| Pay and benefits excluding pension: pay ratio for highest paid director | 7.46:1 | 5.42:1 | 4.37:1 |
Remuneration report signed on behalf of the board of directors.
Toby Lewis, Chief Executive, 26 June 2025.
The council of governors
The council of governors comprises 36 seats for members of the public, service users and patients, carers, colleagues and representatives from partner organisations. This composition was subject to a review and change during the year.
Governors have responsibility for:
- advising the trust on its strategic direction
- representing the interests of members and partner organisations and regularly feeding back to their constituency
- appointing (and removing) of the chair and non-executive directors
- approving the appointment of the chief executive
- appointing the trust’s auditor and receiving the annual accounts, auditor’s report and annual report
- informing NHS England of any unresolved issues
The council of governors provides an important link between the trust, the local community and key organisations, sharing information and views that can be used to develop and improve services. The council of governors is chaired by Kathryn Lavery, who ensures that there are strong links between the council of governors and the board of directors. The lead governor Joan Cox, community services, carer, took up the lead governor position in June 2021 having been in the governor role since August 2017.
The board of directors is responsible for the operational management of the trust, the delivery of high quality, effective services, and for making decisions relating to the strategic direction, financial control and performance of the trust. The board of directors takes account of the views of the governors, and members of the board of directors have attended council of governors meetings in the last year. Below sets out the composition of the council of governors:
Public 11
- 4 in Doncaster.
- 4 in Rotherham.
- 2 in North Lincolnshire.
- 1 in rest of England.
Patient and carer 9
9 governors.
Staff 6
- Rotherham adult mental health care group.
- Doncaster mental health and learning disabilities care group.
- Physical health and neurodiversity care group.
- North Lincolnshire adult mental health and talking therapies care group.
- Children’s care group.
- Corporate backbone.
Partner 10
- 1 city of Doncaster Council
- 1 Rotherham Metropolitan Borough Council.
- 1 North Lincolnshire Council.
- 1 university.
- 1 general practitioner.
- 1 integrated care board.
- 2 youth forum.
- 1 Healthwatch.
- 1 community voluntary sector.
At the start of the year, 21 governors were in post. Over the year there have been a number of changes to those holding positions on the council of governors, through resignations and elections (see below), resulting in 30 seats being filled at the year end. Preparation to fill the remaining seats started in quarter four with elections scheduled to begin in April 2025.
Four meetings were chaired by the chair of the trust. Meetings were attended by members of the board of directors. The governors and their attendance at the meetings are shown in the table below:
| Council of governors | June 2024 | September 2024 | December 2024 | March 2024 | Total number of meetings | Percentage attendance | Term expiry | Appoint or elected |
|---|---|---|---|---|---|---|---|---|
| Alex Haig | Attended | Attended | Did not attend | 3 | 67% | Left February 2025 | Elected | |
| Ann Llewellyn | Attended | Attended | Attended | Attended | 4 | 100% | November 2026 | Elected |
| Arun Chaudhary | Attended | Did not attend | 2 | 50% | November 2027 | Elected | ||
| Champion Solesi | Attended | Did not attend | 2 | 50% | November 2027 | Appointed | ||
| Chris Pope | Attended virtually | Attended virtually | Attended | Attended | 2 | 100% | November 2027 | Elected |
| David Vickers | Did not attend | Attended | Attended | Did not attend | 4 | 50% | November 2025 | Elected |
| Dean Eggitt | Did not attend | Did not attend | Did not attend | Did not attend | 4 | 0% | February 2026 | Appointed |
| Emma Price | Attended | Attended | 2 | 100% | November 2027 | Appointed | ||
| Emma Wilsher | Attended | Did not attend | 2 | 50% | November 2027 | Elected | ||
| Hannah Hall | Attended | Attended | 2 | 100% | November 2027 | Elected | ||
| Ian Spowart | Attended | Did not attend | Attended | Attended | 4 | 75% | November 2026 | Elected |
| Jennie Gauld | Attended | Attended | 2 | 100% | November 2027 | Elected | ||
| Jessica Williams | Attended | Did not attend | 2 | 50% | November 2027 | Elected | ||
| Joan Cox | Attended | Attended | Attended | Attended | 4 | 100% | November 2026 | Elected |
| Joy Bullivant | Did not attend | Did not attend | Attended | Attended | 4 | 50% | November 2026 | Elected |
| Kamlesh Vatish | Attended | Attended | Attended | Attended | 4 | 100% | November 2027 | Elected |
| Kevin Hodgkiss | Attended | Did not attend | 2 | 50% | November 2027 | Elected | ||
| Lee Golze | Attended | Attended | Attended | Attended | 4 | 100% | November 2026 | Appointed |
| Linda Beresford | Attended | Did not attend | 2 | 50% | November 2027 | Appointed | ||
| Mark Johnson | Did not attend | Attended | Did not attend | Did not attend | 4 | 25% | November 2025 | Elected |
| Maureen Young | Attended | Attended | Attended | Attended | 4 | 100% | November 2027 | Elected |
| Mike Seneviratne | Did not attend | Attended | Attended | Did not attend | 4 | 50% | November 2025 | Elected |
| Mohamed Suleman | Attended | Did not attend | Did not attend | Did not attend | 4 | 25% | November 2025 | Elected |
| Prachi Goulding | Attended | Attended | 2 | 100% | November 2027 | Elected | ||
| Richard Rimmington | Did not attend | Attended | Attended | Attended | 4 | 75% | November 2026 | Elected |
| Roxanne Kirby | Did not attend | Did not attend | Did not attend | Did not attend | 4 | 0% | September 2026 | Appointed |
| Ruth O’Shea | Attended | Did not attend | Did not attend | Did not attend | 4 | 25% | November 2025 | Elected |
| Ruth Sanderson | Did not attend | Attended | Did not attend | Did not attend | 4 | 25% | November 2025 | Elected |
| Victoria Stocks | Did not attend | Did not attend | 2 | 0% | November 2027 | Elected | ||
| Sally French | Attended | Did not attend | Did not attend | 3 | 33% | Left November 2024 | Elected | |
| Mohammed Ramzan | Attended | Did not attend | Attended | 3 | 67% | Left November 2024 | Elected | |
| Kym Gleeson | Attended | 1 | 100% | March 2028 | Appointed | |||
| Debra Taylor | Attended | 1 | 100% | March 2028 | Appointed |
Register of interests
The interests for the council of governors are presented to the council of governors at each meeting and are part of the register of interests. The register of interests is a public document and is available via the trust’s website.
Expenses
Governors receive no remuneration for their role. However, the trust provides appropriate reimbursement, for example to cover travel expenses for governors who participate in events or activities arranged by the trust. In the year April 2024 to March 2025, one governor received expenses and the total amount paid and or reimbursed to support their attendance was approximately £49. In the year April 2023 to March 2024 the total amount paid and or reimbursed to support their attendance was approximately £125.
How to contact your governor
Governors represent the members of their respective constituencies. If you have any comments, concerns or questions, or if you have any other need to speak to the governor who represents you, contact can be through the Corporate Assurance team:
Foundation trust membership
Becoming a member of the trust offers local people a unique opportunity to have their say and to be involved in how the trust and its services are developed. The trust wants to build a meaningful and representative membership.
New employees automatically become members of the trust. As with all members, they can influence plans for the trust and its services for the benefit of service users and carers. They can elect to the council of governors and stand for election themselves. All our colleagues are encouraged to be actively involved as members and to spread the word, highlighting the benefits of membership.
The trust continued its engagement with members in the wider community (patients, service users, carers and public) through attendance at a range of community events such as The Rotherham Show and PRIDE events in both Doncaster and North Lincolnshire. Members are also invited to the Annual Members Meeting held by the trust. These are great opportunities to speak to the members and hear from them about their experiences with the trust and its services. They also allow for suggestions and information sharing. The trust has also engaged members during the governor election process and on a more regular basis through its website, social media such as X, Facebook and Instagram and via the new trust app.
Membership constituencies
Anyone aged 16 or over is eligible to become a member. The trust has three membership constituencies:
Public
To be eligible for membership to one of our public constituencies, people should live in the four electoral areas of either:
- Rotherham Metropolitan Borough Council
- City of Doncaster Council
- North Lincolnshire Council
- Rest of England (rather than defining a further boundary for those living in close proximity to our localities, the trust chooses to add a ‘Rest of England’ to include those people in neighbouring boroughs who may be interested).
Service users and carers
To be eligible for membership of the service user and carers constituency, a person should have accessed within the last five years any of our services as a service user or as the carer of a service user in any of our services.
Staff
A member of the staff constituency is a person who is employed by the trust under a contract of employment which has no fixed term, or a fixed term of at least 12 months, or who has been continuously employed by the trust for at least 12 months. New members of staff automatically become members of the foundation trust, although they are given the opportunity to opt out if they wish. Members of the staff constituency are allocated to the following areas:
- Doncaster adult mental health and learning disabilities care group Rotherham adult mental health care group
- North Lincolnshire adult mental health and Talking Therapies care group
- Physical health and neurodiversity care group
- Children’s care group
- Corporate and other services
As at 31 March 2025, the trust had a total membership of 461 (for April 2023 to March 2024 this was 9,297).
Membership size and movement
During the year the trust undertook a purposeful and significant review of its membership with the primary aim of ensuring that only those that recently expressed or reconfirmed their interest in continuing as a member remained as members. In addition, ensuring that there were up to date contact details on record too.
Whilst the resultant movement was a sizeable reduction, the trust has now a smaller, but more engaged membership. As well as being determined to increase that membership further, the trust will expect greater involvement and engagement with its members, supporting the delivery of promises linked to strategic objective one in the main, but to other promises too.
| Consistency | 1 April 2024 | New members | Leavers | 31 March 2025 |
|---|---|---|---|---|
| Public constituency | 6,221 | 173 | 5,984 | 410 |
| Service User and Carer constituency | 1,448 | 7 | 1,404 | 51 |
| Staff constituency | 3,932 | 621 | 449 | 4,104 |
During the period from April 2025 there will be focused work undertaken to grow the membership numbers, ensuring that it is representative of the communities served. We will ensure membership is purposeful and rewarding for those that engage with us on an increasing scale, with more benefits and opportunities provided to those that engage and are involvement the most. This work forms part of Promise 5 of the trust’s strategy.
The home of membership
Our membership home is structured into gold, silver and bronze rooms:
Bronze room
If you attend and participate in the public annual member meeting, and participate in online surveys which are shared with you from trust, we will:
- share Trust Matters
- share a quarterly newsletter
- share the annual report
- invite you to take part in a membership appreciation project locally.
All in easy read format and sent to you.
If you do this, we will offer you the chance to step up to the silver room, keeping all the bronze room perks.
Silver room
If you participate in a minimum of 3 involvement activities during a 12-month period, we will:
- reimburse you for your expenses and pay sessional fees for certain activities as per the reimbursement policy
- offer the opportunity to shadow trust colleagues for learning, insight, and experience for 2 days per annum
- invite you to a bi-annual networking and social event within your locality of Doncaster, Rotherham or North Lincolnshire
- invite you to the annual involvement and volunteering celebration and thank you event.
- offer access to sessional curriculum vitae (CV) writing support
- offer a rucksack project for people who are homeless or rough sleeping
- offer sessional access to NHS computers, technology and digital cafe
Gold room
If you regularly volunteer with us or are a governor, we will:
- provide you with an NHS email so that you can access a Blue Light discount card
- provide a points scheme card where you can gain and accumulate points to exchange for vouchers, cinema tickets, value of a gym membership etc online with volunteered hours
- offer a full electric car charge when on trust premises (1 per month) or an annual cycle maintenance session at Cycle Shack
- fund local providers who teach English as a second language and support you to access this where required
- offer access to one internal or external training course (commitment to be matched with role)
- offer a free laundry every 6 months
- offer you access to chaplaincy and spiritual care and occupational health support
- support you to access internal apprenticeships and access to maths and English where required, or support towards trust employment
- support you with free room hire on trust premises for appropriate usage
- enter you in to a prize draw for an annual winter warmer hamper
| Age | Number of members | Eligible membership |
|---|---|---|
| 0 to 16 | 7 | 176,724 |
| 17 to 21 | 11 | 47,912 |
| 22 and over | 400 | 696,740 |
| Not stated | 43 | 0 |
| Ethnicity | Number of members | Eligible membership |
|---|---|---|
| White | 183 | 839,964 |
| Mixed | 1 | 11,887 |
| Asian or Asian British | 11 | 31,325 |
| Black or Black British | 9 | 8,437 |
| Other | 0 | 8,929 |
| Not stated | 257 | 0 |
| Social grade | Number of members | Eligible membership |
|---|---|---|
| AB | 91 | 51,265 |
| C1 | 117 | 100,711 |
| C2 | 95 | 100,101 |
| DE | 107 | 139,112 |
| Gender | Number of members | Eligible membership |
|---|---|---|
| Male | 245 | 454,688 |
| Female | 95 | 466,687 |
| Transgender | 121 | 0 |
| Unspecified | 0 | 0 |
For the purpose of the tables, the eligible membership is taken as those members of the public that live in the trust’s principle geographical locations, Doncaster, Rotherham and North Lincolnshire. There is, however, Rest of England membership constituency which effectively means that any member of the public in England can be a member.
NHS Foundation Trust code of governance disclosures
The purpose of the code of governance is to assist NHS foundation trust boards in improving their governance practices by bringing together the best practice of public and private sector corporate governance. The code is issued as best practice advice but imposes a number of disclosure requirements.
Rotherham Doncaster and South Humber NHS Foundation Trust has applied the principles of the code on a comply or explain basis. The board of directors and council of governors are committed to continuing to operate according to the highest standards of corporate governance, and support and agree with the principles set out in the Code.
Provision A 2.1
Requirement: the board of directors should assess the basis on which the trust ensures its effectiveness, efficiency and economy, as well as the quality of its healthcare delivery over the long term, and contribution to the objectives of the ICP and integrated care board, and place based partnerships. The board of directors should ensure the trust actively addresses opportunities to work with other providers to tackle shared challenges through entering into partnership arrangements such as provider collaboratives. The trust should describe in its annual report how opportunities and risks to future sustainability have been considered and addressed, and how its governance is contributing to the delivery of its strategy.
Compliance
We are involved in several provider collaboratives. As well as being the lead provider for South Yorkshire Adult Eating Disorder Provider Collaborative. We actively seek opportunities to collaborate with other providers, and we do this through the MHLDA Alliance, networking, and fostering relationships with other mental health and community providers. The strategic development team reviews opportunities that align with our objectives as outlined in the trust’s 2023 to 2028 Clinical and Organisational Strategy. See also role of the board.
Provision A 2.3
Requirement: the board of directors should assess and monitor culture. Where it is not satisfied that policy, practices or behaviour throughout the business are aligned with the trust’s vision, values and strategy, it should seek assurance that management has taken corrective action. The annual report should explain the board’s activities and any action taken, and the trust’s approach to investing in, rewarding and promoting the wellbeing of its workforce.
Compliance
Provision A 2.8
Requirement: the board of directors should describe in the annual report how the interests of stakeholders, including system and place based partners, have been considered in their discussions and decision-making, and set out the key partnerships for collaboration with other providers into which the trust has entered. The board of directors should keep engagement mechanisms under review so that they remain effective. The board should set out how the organisation’s governance processes oversee its collaboration with other organisations and any associated risk management arrangements.
Compliance
Provision B 2.6
Requirement: the board of directors should identify in the annual report each non-executive director it considers to be independent. Circumstances which are likely to impair, or could appear to impair, a non-executive director’s independence include, but are not limited to, whether a director:
- has been an employee of the trust within the last two years
- has, or has had within the last two years, a material business relationship with the trust either directly or as a partner, shareholder, director or senior employee of a body that has such a relationship with the trust
- has received or receives remuneration from the trust apart from a director’s fee, participates in the trust’s performance-related pay scheme or is a member of the trust’s pension scheme
- has close family ties with any of the trust’s advisers, directors or senior employees
- holds cross directorships or has significant links with other directors through involvement with other companies or bodies
- has served on the trust board for more than six years from the date of their first appointment
- is an appointed representative of the trust’s university medical or dental school.
Where any of these or other relevant circumstances apply, and the board of directors nonetheless considers that the non-executive director is independent, it needs to be clearly explained why.
Compliance
Board of directors profiles, director independence, register of interests, and remuneration report.
Provision B 2.13
Requirement: the annual report should give the number of times the board and its committees met, and individual director attendance.
Compliance
Provision C 2.17
Requirement: for foundation trusts, this schedule should include a clear statement detailing the roles and responsibilities of the council of governors. This statement should also describe how any disagreements between the council of governors and the board of directors will be resolved. The annual report should include this schedule of matters or a summary statement of how the board of directors and the council of governors operate, including a summary of the types of decisions to be taken by the board, the council of governors, board committees and the types of decisions which are delegated to the executive management of the board of directors.
Compliance
Provision C 2.5
Requirement: if an external consultancy is engaged, it should be identified in the annual report alongside a statement about any other connection it has with the trust or individual directors.
Compliance
Provision C 2.8
Requirement: the annual report should describe the process followed by the council of governors to appoint the chair and non-executive directors. The main role and responsibilities of the nominations committee should be set out in publicly available written terms of reference.
Compliance
Provision C 4.2
Requirement: the board of directors should include in the annual report a description of each director’s skills, expertise and experience.
Compliance
Provision C 4.7
Requirement: all trusts are strongly encouraged to carry out externally facilitated developmental reviews of their leadership and governance using the Well-led framework every three to five years, according to their circumstances. The external reviewer should be identified in the annual report and a statement made about any connection it has with the trust or individual directors.
Compliance
The Office of Modern Governance undertook a well-led review in 2022 and the trust will be commissioning a review in the year April 2025 to March 2026.
Provision C 4.13
Requirement: the annual report should describe the work of the nominations committees, including:
- the process used in relation to appointments, its approach to succession planning and how both support the development of a diverse pipeline
- how the board has been evaluated, the nature and extent of an external evaluator’s contact with the board of directors and individual directors, the outcomes and actions taken, and how these have or will influence board composition
- the policy on diversity and inclusion including in relation to disability, its objectives and linkage to trust vision, how it has been implemented and progress on achieving the objectives
- the ethnic diversity of the board and senior managers, with reference to indicator nine of the NHS Workforce Race Equality Standard and how far the board reflects the ethnic diversity of the trust’s workforce and communities served
- the gender balance of senior management and their direct reports.
Compliance
Provision C 5.15
Requirement: foundation trust governors should canvass the opinion of the trust’s members and the public, and for appointed governors the body they represent, on the NHS foundation trust’s forward plan, including its objectives, priorities and strategy, and their views should be communicated to the board of directors. The annual report should contain a statement as to how this requirement has been undertaken and satisfied.
Compliance
Provision D 2.4
Requirement: the annual report should include:
- the significant issues relating to the financial statements that the audit committee considered, and how these issues were addressed
- an explanation of how the audit committee (and or auditor panel for an NHS trust) has assessed the independence and effectiveness of the external audit process and its approach to the appointment or reappointment of the external auditor; length of tenure of the current audit firm, when a tender was last conducted and advance notice of any retendering plans
- where there is no internal audit function, an explanation for the absence, how internal assurance is achieved and how this affects the external audit
- an explanation of how auditor independence and objectivity are safeguarded if the external auditor provides non audit services
Compliance
Provision D 2.6
Requirement: the directors should explain in the annual report their responsibility for preparing the annual report and accounts, and state that they consider the annual report and accounts, taken as a whole, is fair, balanced and understandable, and provides the information necessary for stakeholders to assess the trust’s performance, business model and strategy.
Compliance
Provision D 2.7
Requirement: the board of directors should carry out a robust assessment of the trust’s emerging and principal risks. The relevant reporting manuals will prescribe associated disclosure requirements for the annual report.
Compliance
Annual governance statement and summary of principal risks confirm the use of the Risk Management Framework to establish and manage the principal risks to the organisation.
Provision D 2.8
Requirement: the board of directors should monitor the trust’s risk management and internal control systems and, at least annually, review their effectiveness and report on that review in the annual report. The monitoring and review should cover all material controls, including financial, operational and compliance controls. The board should report on internal control through the annual governance statement in the annual report.
Compliance
Provision D 2.9
Requirement: in the annual accounts, the board of directors should state whether it considered it appropriate to adopt the going concern basis of accounting when preparing them and identify any material uncertainties regarding going concern. Trusts should refer to the Department of Health and Social Care group accounting manual and NHS foundation trust annual reporting manual which explain that this assessment should be based on whether a trust anticipates it will continue to provide its services in the public sector. As a result, material uncertainties over going concern are expected to be rare.
Compliance
Provision E 2.3
Requirement: where a trust releases an executive director, for example, to serve as a non-executive director elsewhere, the remuneration disclosures in the annual report should include a statement as to whether or not the director will retain such earnings.
Compliance
Not applicable.
Appendix B, paragraph 2.3
Requirement: the annual report should identify the members of the council of governors, including a description of the constituency or organisation that they represent, whether they were elected or appointed, and the duration of their appointments. The annual report should also identify the nominated lead governor.
Compliance
Appendix B, paragraph 2.14
Requirement: the board of directors should ensure that the NHS foundation trust provides effective mechanisms for communication between governors and members from its constituencies. Contact procedures for members who wish to communicate with governors and or directors should be clear and made available to members on the NHS foundation trust’s website and in the annual report.
Compliance
Appendix B, paragraph 2.15
Requirement: the board of directors should state in the annual report the steps it has taken to ensure that the members of the board, and in particular the non-executive directors, develop an understanding of the views of governors and members about the NHS foundation trust, for example, through attendance at meetings of the council of governors, direct face-to-face contact, surveys of members’ opinions and consultations.
Compliance
Additional requirement of foundation trust annual reporting manual resulting from legislation
Requirement: if, during the financial year, the Governors have exercised their power (Power to require one or more of the directors to attend a governors’ meeting for the purpose of obtaining information about the foundation trust’s performance of its functions or the directors’ performance of their duties (and deciding whether to propose a vote on the foundation trust’s or directors’ performance) under paragraph 10C (As inserted by section 151 (6) of the Health and Social Care Act 2012)) of schedule 7 of the NHS Act 2006, then information on this must be included in the annual report.
This is required by paragraph 26(2)(aa) of schedule 7 to the NHS Act 2006, as amended by section 151 (8) of the Health and Social Care Act 2012.
Compliance
Not applicable.
There are no provisions within the NHS Code of Governance that we did not comply with for the period 1 April 2024 to 31 March 2025.
NHS England well-led framework
NHS England’s well-led framework identifies the characteristics required of good provider organisations that ensure quality services are provided:
- leadership capacity and capability
- clear vision and credible strategy
- culture of high-quality care
- clear responsibilities, roles and systems of accountability
- clear and effective processes for managing risks
- robust and appropriate information effectively processed and challenged people using services, the public, staff and partners engaged and involved
- robust systems and processes for learning, continuous improvement and innovation.
The trust has robust quality and corporate governance arrangements in place to ensure the quality of services it provides, and reviews these on an annual basis to consider further improvements. Quality governance and quality performance are covered in detail in the Annual Governance Statement as well as in the performance section of the annual report.
The board undertakes regular reviews of its performance and effectiveness as this provides a useful opportunity to step back and reflect. This includes:
- the chair conducts individual performance evaluations of the non-executive directors and the chief executive, as well as executive directors in relation to their duties as board members.
- the senior independent director conducts a performance evaluation of the chair having collectively met with all other non-executive directors and received feedback from governors and executive directors
- the chief executive conducts performance evaluations of the executive directors
Care Quality Commission (CQC)
The trust is required to register with the Care Quality Commission (CQC) and its current registration status is ‘Registered with no conditions applied’. The CQC has not taken enforcement action against the trust during the year April 2024 to March 2025.
The latest inspection by the Care Quality Commission was a “Well-led” inspection of the trust that took place in November 2019 and the inspection report was published in February 2020. The trust received an overall rating of ‘Requires Improvement’, with ratings of ‘Good’ in the domains of Caring and Responsive and a rating of ‘Requires Improvement’ in the domain of Safe, Effective and Well Led. Action was taken by the trust in response all recommendations made.
The trust has not participated in any reviews during the year April 2024 to March 2025.
NHS system oversight framework
NHS England’s NHS Oversight Framework provides the framework for overseeing systems including providers and identifying potential support needs. NHS organisations are allocated to one of four ‘segments’.
A segmentation decision indicates the scale and general nature of support needs, from no specific support needs (segment 1) to a requirement for mandated intensive support (segment 4). A segment does not determine specific support requirements. By default, all NHS organisations are allocated to segment 2 unless the criteria for moving into another segment are met. These criteria have two components:
- objective and measurable eligibility criteria based on performance against the six oversight themes using the relevant oversight metrics (the themes are: quality of care, access and outcomes; people; preventing ill-health and reducing inequalities; leadership and capability; finance and use of resources; local strategic priorities)
- additional considerations focused on the assessment of system leadership and behaviours, and improvement capability and capacity
An NHS foundation trust will be in segment 3 or 4 only where it has been found to be in breach or suspected breach of its licence conditions.
Segmentation
Rotherham Doncaster and South Humber NHS Foundation Trust received the segmentation rating of 3 as at 5 March 2025 (most recently published rating). This decision related to the trust’s financial plan for April 2024 to March 2025 being a deficit plan. This plan has been exceeded in year as reported within this document. Segmentation also relates to the host Integrated Care Board’s financial position, which shows a deficit plan and delivery.
Current segmentation information for NHS trusts and foundation trusts is published on the NHS England website.
A new performance management framework, including revised segmentation parameters, will be implemented during the period April 2025 to March 2026.
Counter fraud, bribery and corruption
The NHS counter fraud authority provide the framework through which trust’s sought to minimise losses through fraud. The chief executive and director of finance and estates are jointly responsible for ensuring the trust meets its obligation and are supported by the local counter fraud specialist (LCFS). A work plan has been completed in the year by the LCFS. The work plan addresses the requirements of the trust’s counter fraud, bribery and corruption policy. The key aims are to seek to proactively create an anti-fraud culture, implement appropriate deterrents and preventative controls and to ensure that allegations of fraud are appropriately investigated.
Regular reports are received throughout the year by the audit committee as well as an annual report. Reported concerns have been investigated by our LCFS specialists in liaison with the NHS counter fraud authority (CFA) and the police as necessary. The audit committee reviewed the levels of fraud reported and detected, and the arrangements in place to prevent, minimise and detect fraud and bribery.
Further information on policy is provided with the staff report, see equality, diversity and inclusion.
Statement of the chief executive’s responsibilities as the accounting officer of Rotherham Doncaster and South Humber NHS Foundation Trust
The NHS Act 2006 states that the chief executive is the accounting officer of the NHS foundation trust. The relevant responsibilities of the accounting officer, including their responsibility for the propriety and regularity of public finances for which they are answerable, and for the keeping of proper accounts, are set out in the NHS Foundation Trust Accounting Officer Memorandum issued by NHS England.
NHS England has given Accounts Directions which require Rotherham Doncaster and South Humber NHS foundation trust to prepare for each financial year a statement of accounts in the form and on the basis required by those Directions. The accounts are prepared on an accruals basis and must give a true and fair view of the state of affairs of Rotherham Doncaster and South Humber NHS foundation trust and of its income and expenditure, other items of comprehensive income and cash flows for the financial year.
In preparing the accounts and overseeing the use of public funds, the Accounting Officer is required to comply with the requirements of the Department of Health and Social Care Group Accounting Manual and in particular to:
- observe the Accounts Direction issued by NHS England, including the relevant accounting and disclosure requirements, and apply suitable accounting policies on a consistent basis
- make judgements and estimates on a reasonable basis
- state whether applicable accounting standards as set out in the NHS Foundation Trust Annual Reporting Manual (and the Department of Health and Social Care Group Accounting Manual) have been followed, and disclose and explain any material departures in the financial statements
- ensure that the use of public funds complies with the relevant legislation, delegated authorities and guidance
- confirm that the annual report and accounts, taken as a whole, is fair, balanced and understandable and provides the information necessary for patients, regulators and stakeholders to assess the NHS foundation trust’s performance, business model and strategy and
- prepare the financial statements on a going concern basis and disclose any material uncertainties over going concern. The accounting officer is responsible for keeping proper accounting records which disclose with reasonable accuracy at any time the financial position of the NHS foundation trust and to enable them to ensure that the accounts comply with requirements outlined in the above mentioned Act.
The Accounting Officer is also responsible for safeguarding the assets of the NHS foundation trust and hence for taking reasonable steps for the prevention and detection of fraud and other irregularities.
As far as I am aware, there is no relevant audit information of which the foundation trust’s auditors are unaware, and I have taken all the steps that I ought to have taken to make myself aware of any relevant audit information and to establish that the entity’s auditors are aware of that information.
To the best of my knowledge and belief, I have properly discharged the responsibilities set out in the NHS Foundation Trust Accounting Officer Memorandum.
Toby Lewis, Chief Executive. 26 June 2025.
Annual governance statement
Scope of responsibility
As accounting officer, I have responsibility for maintaining a sound system of internal control that supports the achievement of the NHS foundation trust’s policies, aims and objectives, whilst safeguarding the public funds and departmental assets for which I am personally responsible, in accordance with the responsibilities assigned to me. I am also responsible for ensuring that the NHS foundation trust is administered prudently and economically and that resources are applied efficiently and effectively. I also acknowledge my responsibilities as set out in the NHS Foundation Trust Accounting Officer Memorandum.
The purpose of the system of internal control
The system of internal control is designed to manage risk to a reasonable level rather than to eliminate all risk of failure to achieve policies, aims and objectives; it can therefore only provide reasonable and not absolute assurance of effectiveness. The system of internal control is based on an ongoing process designed to identify and prioritise the risks to the achievement of the policies, aims and objectives of Doncaster Rotherham and South Humber NHS Foundation Trust, to evaluate the likelihood of those risks being realised and the impact should they be realised, and to manage them efficiently, effectively and economically. The system of internal control has been in place in Doncaster Rotherham and South Humber NHS Foundation Trust for the year ended 31 March 2025 and up to the date of approval of the annual report and accounts.
Capacity to handle risk
The trust’s capacity to manage risk effectively is supported through clear governance, visible leadership, and the provision of appropriate training and guidance to staff. A structured approach ensures risk management is not viewed as a standalone activity but as a fundamental part of delivering safe, high-quality care.
Leadership for risk management is driven through a combination of executive commitment, operational accountability, and well-defined governance routes. The risk management group (RMG) plays a central role in embedding risk management practice across the organisation. Chaired by the chief nursing officer, the RMG brings together senior clinical and corporate leaders to oversee how risks are identified, assessed, and managed within care groups and corporate functions. Positioned within the governance structure, the RMG provides a formal route through which both operational and higher-level risks are reviewed, challenged, and either addressed or escalated, depending on their likelihood and impact. The group reports into the clinical leadership executive (CLE), ensuring that risk related issues inform clinical decision-making and organisational priorities.
Broader leadership support is evident through executive leads who take ownership of key risk domains and model good practice by actively engaging in risk discussions and reviews. Updates on the implementation of the risk management framework, including progress, challenges, and improvements in consistency of practice, are provided to the audit committee. This reinforces the trust’s commitment to strengthening risk maturity and transparency at the most senior level.
In the year under review and responding the auditor’s comments on the year ending March 2024, the trust’s board has wholly altered its approach to strategic risk management, including the board assurance framework. The Internal audit review conducted of those changes offers confidence that the full board is actively engaged with the longer-term risks to delivery of the trust’s strategy, with a focus on data relating to inequalities, the capability to engage with our communities and primary care, a shift to a more seven day model of service delivery, and the relationships we have with general practice.
Staff across the organisation are supported to manage risk in a way that aligns with their role and level of responsibility. This begins with access to tailored training, and targeted workshops for senior managers and risk owners, which focus on the core principles of risk assessment, escalation, and register management. These are complemented by direct support from risk and governance leads embedded in directorates, who provide one-to-one guidance and help teams apply the framework consistently.
In addition to formal training, staff are supported through accessible, practical resources such as the trust’s risk management framework, guidance on writing risk descriptions, scoring tools, and templates that help standardise the approach. These materials are regularly updated to reflect learning and best practice. The trust is committed to continuous improvement and learning. Good practice is identified through thematic analysis of risk registers, incident reviews, and inter-team collaboration. The RMG serves as a key forum for sharing learning across directorates, helping to spread effective risk mitigation strategies.
The risk and control framework
The trust’s risk management framework provides a structured and consistent approach to identifying, evaluating, and managing risk across all levels of the organisation and also includes the trust’s risk appetite statement. Risks are identified through a range of sources including incident reporting, audits, clinical reviews, regulatory feedback, data monitoring, and local intelligence. Once identified, risks are described using a standardised format that captures the cause, risk event, and potential impact, supporting shared understanding and appropriate escalation.
The trust’s appetite for risk is defined by the board and outlines the amount and type of risk the trust is prepared to accept, tolerate or be exposed to at any point in time.
Risks are assessed using a consistent scoring methodology that considers both the likelihood and consequence of the risk materialising. This scoring determines the level of oversight required. Control measures are documented along with assigned owners responsible for implementing and reviewing mitigation plans.
A key tool in the management of risk is the trust’s risk register, which serves as a live, structured record of current risks across clinical and backbone areas. The register enables monitoring, trend analysis, and assurance at every level of the organisation. To improve ownership and visibility, the trust has adopted a directorate first approach to risk registration. This ensures that risks are captured and reviewed as close to the point of origin as possible, encouraging early intervention and shared responsibility across operational teams.
All risks are subject to ongoing review through the appropriate governance route, with mitigating actions tracked and regularly tested for effectiveness. Risk owners are expected to review and update risk entries regularly, ensuring that the register reflects the current position and that learning from incidents, audits, and reviews is used to inform risk control.
Risk management is embedded into the organisation’s day-to-day operations through active use of the risk register, structured governance oversight, and ongoing engagement with clinical and corporate teams. The risk management group, chaired by the chief nursing officer and reporting into the clinical leadership executive, plays a key role in promoting consistency, supporting the use of the framework, and sharing good practice.
The trust is registered with the Care Quality Commission with no conditions applied and the statement of purpose is regularly updated and changes reported to the Care Quality Commission.
The trust is committed to supporting patient safety by ensuring information is accessible, its integrity is protected against loss or damage, and confidentiality is maintained. The trust recognises that information handling represents a corporate risk in that failures to protect information properly, or to use it appropriately, can have a damaging impact on the safety of our patients and the reputation of the organisational.
Information risk management is monitored via our information risk management framework. As part of this, information risks are clearly recognised, and the appropriate controls implemented through the risk management framework. The senior information risk owner (SIRO) is responsible for overseeing the development and implementation of the information risk management framework. The SIRO is supported in this by the information governance (IG) team and by the information asset owners (IAO) within each business area. IAO’s are responsible for managing information risks to the assets within their control.
Quality of data is overseen by the Information quality work programme, which audits and kitemarks key performance metrics set by the trust as part of its floor to board assurance and reported to the finance digital and estates committee. More broadly the performance team who are embedded in operational services undertake regular data quality samples of the performance data reported both internally and externally.
NHS Foundation Trust License Condition Compliance
As an NHS Foundation Trust, the trust is required by its license to apply relevant principles, systems and standards of good corporate governance (FT4). To discharge this requirement the trust has a board of directors and committee structure with responsibilities set out in formal terms of reference. The board and its committees have associated reporting lines, performance and risk management systems. Each committee is chaired by a non-executive director and has an associated executive team member as its executive lead. The work plans of the committees are reviewed regularly, and the board considers any proposed amendments to their terms of reference.
A self-assessment of compliance against the trust’s licence is undertaken by the director of corporate assurance and reviewed by the board of directors. The board of directors has not identified any principal risks to compliance with provider licence condition FT4 and is satisfied with the timeliness and accuracy of information to assess risks to compliance with the provider licence and degree of rigour of oversight it has over performance.
The trust also has a comprehensive programme of internal audit in place aligned to key areas of potential financial and operational risk. This will increasingly be examined, set, and managed alongside our clinical audit programme, as we look to work on an integrated basis.
Stakeholder relations
The trust recognises the importance of working in partnership with others including statutory organisations, voluntary sector and communities. During the year April 2024 to March 2025, we have continued to review our key partnerships with stakeholders in Rotherham, Doncaster and North Lincolnshire and across the two integrated care systems that we work in. A new approach to managing stakeholder relations and partnerships is being rolled out which will involve executive directors taking a relationship manager role with each key partner. The public health, patient involvement and partnerships committee (PHPIP) has a remit to focus on our partnership working.
The trust has a social enterprise called “Flourish”. Flourish was formed in 2014 and is a wholly owned subsidiary of the trust. It is incorporated as a community interest company and is registered with Companies House. It was established with the following objectives that improve people’s health and wellbeing:
- to provide work, vocational training and therapeutic opportunities to the people who need our support
- to work with partners and stakeholders to provide a valuable contribution to the local economy
- to provide opportunities for community involvement
The trust is also the lead provider for the South Yorkshire Adult Eating Disorder Provider Collaborative. This includes commissioning beds from independent sector providers that is supported by financial and quality oversight: this is delivered through a joint agreement with other providers in South Yorkshire. Funding is provided via NHS England’s specialist commissioning team. The purpose is to provide the highest quality eating disorder care that is person centred, supports recovery, is responsive and is delivered as close to home as possible. By doing this we are reducing the need of people to need care in hospital and support people to lead successful lives supported in their local community.
The trust has a range of patient and public involvement activities and consultation with its communities and empowering them. There are many examples of this. We work with our voluntary and charity sectors to deliver our Aspire drug and alcohol services. This includes a strong peer support model. In Rotherham we have invested fully in community resources to support individuals beyond traditional service boundaries. Local community groups were micro-commissioned and funded according to the needs of our service users and were provided in communities across Rotherham. This included peer support, befriending, activity and exercise. We have also supported community groups through our charitable funds, where organisations are working in partnership with services in the trust.
The People Focused Group (PFG) working in the voluntary sector are our patient participation partner and together we engage with many parts of our communities to work with them on designing and delivering services. PFG deliver part of our services for people experiencing a mental health crisis by providing the safe space service in Doncaster. The service is delivered by a large network of peer support workers and provides much needed care to our communities. We also commission PFG to provide a range of other community based services in Doncaster.
As part of our strategic plan promise 5, we have actively sought to make our work on involvement go further. We have systematically started to involve our communities at every level of decision making in our trust throughout the year, extending our membership offer and delivering the annual priorities set by our staff and public governors. This includes:
- changed the constitution of our council of governors to expand access to governor positions to a wider range of local people, and organisations, whilst including for the first time specific places for children and young people within our leadership
- changed all of the board’s committees and included within them both a specific obligation of partnership working, elected governors now represent views from patients, carers and communities within these committees
- established our long-term executive operating model and restructured the management of our five care groups, again, creating places for representatives drawn from our local communities, as well as reserving roles for seldom heard voices among our employees
- began the work of changing our membership arrangements to better support meaningful participation in issues that matter to our members
Safe staffing and workforce development
The trust continues to have regard for the national quality board (NQB) requirements, endorsed by the Care Quality Commission. The guidance articulates for all NHS providers the accountabilities in respect of safe sustainable and productive staffing and recommends that the board of directors should have processes in place to provide assurance that the right staff with the right skills are in the right place at the right time.
We contribute to the national reporting system by submitting our data and providing insights into our staffing levels and practices. This shared information contributes to a broader understanding of healthcare staffing across the country.
Internally, we maintain our own safe staffing data. This data helps us to ensure safe and effective management on our wards. By closely monitoring our staffing levels, we ensure a secure and supporting environment for both our staff and the individuals under our care.
The trust’s safe staffing policy describes the process that should be followed to anticipate, plan and manage optimal staffing requirements. The policy provides guidance to ensure that rosters are safe, balanced and efficient. It also outlines the required actions and governance arrangements required to support the management of rosters and escalation mechanisms where there are shortfalls in staffing number.
The trust presents a safe staffing report to the quality and safety group on a bi-monthly basis and an annual declaration is submitted to board of directors. The annual safe staffing declaration was last presented to board of directors in March 2025. The trust publishes safer staffing data on the public website.
All service changes have a quality and safety impact assessment (QSIA) and are reviewed by the QSIA panel. This provides scrutiny and advice on monitoring arrangements.
In line with national guidance the trust also reports via UNIFY (a reporting system to NHS England) each month the care hours per patient day (CHPPD) data.
Compliance statements
The foundation trust is fully compliant with the registration requirements of the Care Quality Commission.
The foundation trust has published on its website an up-to-date register of interests, including gifts and hospitality, for decision-making staff (as defined by the trust with reference to the guidance) within the past twelve months as required by the managing conflicts of interest in the NHS guidance.
As an employer with staff entitled to membership of the NHS pension scheme, control measures are in place to ensure all employer obligations contained within the Scheme regulations are complied with. This includes ensuring that deductions from salary, employer’s contributions and payments into the scheme are in accordance with the scheme rules.
Control measures are in place to ensure that all the organisation’s obligations under equality, diversity and human rights legislation are complied with.
The foundation trust has undertaken risk assessments on the effects of climate change and severe weather and has developed a green plan following the guidance of the Greener NHS programme. The trust ensures that its obligations under the Climate Change Act and the adaptation reporting requirements are complied with.
Review of economy, efficiency and effectiveness of the use of resources
The finance, digital and estates committee (FDEC) and ultimately the board of directors ensure through a series of robust review mechanisms, that the use of resources is planned in an efficient and effective manner, and that our financial position is monitored and scrutinised. They oversee the monthly position against the approved financial plan for the year though their primary focus is underlying financial viability on a multi-year basis.
I have responsibility for ensuring that the resources used in the day-to-day operational activities of the trust are done so in an economic, efficient and effective manner. This is discharged through two formal systems. A sub-group of the clinical leadership executive oversees financial performance. Every month by rotation our care groups and each corporate directorate undertake a delivery review, where alongside safety, workforce and wider delivery matters, financial control is discussed, and relevant actions taken. In the year April 2024 to March 2025 every single care group and corporate directorate met its budgetary obligations, despite a 4% cost improvement programme. This is testimony to local control and has benefitted too from central and corporate teams’ support.
In addition to the monthly budgetary control system, the trust ensures economy, efficiency and effectiveness as well as value for money through the implementation of a suite of effective and consistently applied financial controls, effective tendering procedures and procurement practices, robust establishment controls and continuous service improvement and modernisation programmes. Our standing financial instructions have been reviewed and revisited in-year through the board.
We have a bi-monthly audit committee that includes reports from internal and external audit. The auditors provide their respective views to the committee on our overall governance and control processes. FDEC and the audit committee are two of the eight committees put in place by the board of directors as part of its governance structure. For further details on the structure and the attendance of directors at meetings of the board. The annual assessment of compliance statement with the corporate governance code is provided in the annual report.
Information governance
The trust has a nominated senior information risk officer (SIRO) at executive level who has been nominated responsibility for information risk. The data protection officer (DPO), overseas data protection compliance throughout the trust and provides independent advice to the trust.
Information governance incidents are monitored through the information governance group (chaired by the SIRO) on a monthly basis. During the year April 2024 to March 2025 there have been 572 incidents reported (543 incidents were reported in the year April 2023 to March 2024) none of which required notifications to the Information Commissioner via Data Security and Protection toolkit (during the year April 2023 to March 2024 there were four incidents).
Data quality and governance
Quality of data is overseen by the information quality work programme, which audits and kitemarks key performance metrics set by the trust as part of its floor to board assurance and reported via the integrated quality and performance report (IQPR). Metrics assessed and kitemarked are reported to finance digital and estates committee. More broadly the performance team and the data support officers who are embedded in operational services undertake regular data quality samples of the performance data reported both internally and externally.
The trust has published a data quality policy, management information guide and quality assurance and performance framework flow chart, these three documents support the coproduction of reports through development to sign off, which includes data quality testing. The management information guide also set out ongoing responsibilities for the oversight and escalation of data quality. In addition, the data quality group (monthly meeting) is a forum for data quality issues to be escalated, explored and corrected. The data quality group reports into the digital transformation group which subsequently reports to the clinical leadership executive (CLE).
In terms of elective waits, the trusts access and waiting times policy outlines the services for which it applies the principles of referral to treatment (RTT). The trust performance team monitors waits on a monthly basis and escalates concerns to the responsible care groups. Data quality issues are investigated as part of this process. Additionally, the information quality team audit and kitemark the waits in scope of national RTTs which are also monitored internally through the IQPR. Whilst this work provides a measure of confidence on the data quality, latest audit reviews suggest we have some further documentation of local processes to complete in the first half of the coming year.
Review of effectiveness
Based on the work undertaken during the year April 2024 to March 2025 the Head of Internal Audit has stated that their Head of Internal Audit Opinion as significant assurance as detailed below.
I am providing an opinion of significant assurance that there is a generally sound framework of governance, risk management and control designed to meet the organisation’s objectives, and controls are generally being applied consistently.
Throughout our programme of work we have evidenced improvements across all key areas considered in our overall opinion. The outturn of individual audit assignments is largely positive although we have provided some areas of moderate and limited assurance. Organisational change is occurring at pace in line with the trust’s strategy and promises, however a theme arising from our work this year is that this isn’t always supported by clear planning, and some systems of governance and control continue to embed. The trust’s audit plan this year was proactively pointed toward some continually developing areas, and agreed recommendations to strengthen those areas have been progressed.
I have also reflected on the improvement in action implementation versus previous years, as well as strengthened and embedded strategic risk management arrangements.
As Accounting Officer, I have responsibility for reviewing the effectiveness of the system of internal control. My review of the effectiveness of the system of internal control is informed by the work of the internal auditors, clinical audit and the executive managers and clinical leads within the NHS foundation trust who have responsibility for the development and maintenance of the internal control framework. I have drawn on performance information available to me. My review is also informed by comments made by the external auditors in their management letter and other reports. I have been advised on the implications of the result of my review of the effectiveness of the system of internal control by the board, the audit committee, the quality committee, the people and organisational development committee, the finance, digital and estate committee, public health, patient involvement and partnerships committee and the mental health act committee and a plan to address weaknesses and ensure continuous improvement of the system is in place.
During the period from April 2024 to March 2025, we have made continued progress in implementing an operating model that we adopted through our board of directors in late 2023. Two reviews of that model in practice, commissioned through Good Governance Institute (GGI), suggest good adherence to the intent of those changes, and particularly positive changes in the involvement of patients’ voices within our processes.
In considering these controls in practice, I do not have material concerns to highlight. At the same time, we have not yet established the full range of management systems that we will need to achieve our aims. We recognise that the trust is transitioning its management arrangements to rely more carefully and precisely on the use of data, both qualitative and quantitative. This transition is not yet completed and the year ahead needs to see a further step-change.
That step-change relates particularly to the use of near-live data in managing quality and safety governance. The adoption of the RADAR system from May 1, 2025, will contribute greatly to this work, as will rollout of our safety plan during the coming year. Some services offered by the trust have established datasets and points of comparison, while others do not. Our increasing movement to directorate led management processes across thirteen clinical directorates will help us to ensure that we are considering the full range of care services, in proportion of risk when we synthesis our views of safety.
Over the year that ended in March 2025, we have aligned our finance and personnel datasets with much greater discipline. This has enabled us to look across data sources and consider staffing safety, the commitment of resources, and issues of retention and recruitment. Increasingly this data forms part of the mainstream conversation of the trust at a local level, as well as corporately. This intention must be maintained in the year ahead, as our fully staffed position is one that we intend to maintain, with less reliance of bank employees, and no upswing in agency use.
The substantial reduction in waiting times that we intend to achieve in the year ahead will rely on data quality, governance of that data quality, and feedback from staff and patients. It will be important that all stakeholders have confidence that significant improvements in delivery are grounded in real world change. For our core wait time promise (promise 14 – 4-week wait) this dataset is largely within our control. For the commitment to address out of area placements (promise 19) it is a shared obligations alongside our integrated care board partners.
The annual report outlines the scale and potential of patient voice, in particular, through the care opinion system we have used. The use of voice, including staff voice, alongside more formal data, is an important part of the organisation’s practice. We continue to seek to embed those voices not only at the most senior corporate level but into the practice of our management systems at local level, for example directorates and care groups. Our success in doing that will be material in the likelihood of the year ahead seeing the changes we seek in pursuit of the strategy.
The significant improvement in risk management grip, and in board oversight of strategic risks, as well as partnership working, over this last year are to be noted. They serve as an important foundation for the improvements in management control that we need to demonstrate. Our investment in improved business intelligence for the year ahead points clearly to where we need to see further change if we are to maximise that potential.
Conclusion
The board of directors considered our self-assessment of how well-led the trust is in November 2024. A further submission was considered in May 2025. The trust has developed a range of management and leadership development programmes in place to support its work, for first time managers, clinicians in management, and those working corporately including among the executive group. These interventions attest to a determination to ensure that good quality leadership practice is distributed across the trust as a whole. The results of audit review and other advice in this annual governance statement reinforce the view that this spread is needed to achieve even better control as a trust.
Our board’s work on risk appetite from March 2023, renewed in April 2025, suggests that we need to match controls in line with our scheme of delegation, with a commitment to pace and innovation. Directorate led working will allow frontline managers to make decisions and manage risk, whilst more senior leaders focus on the challenges presented by the future landscape of population need, workforce supply, and financial constraint.
With the addition of the better data needed to manage quality and safety, the controls we have position the trust well to meet the future challenges of the NHS reset and of the long term plan. Consistent application of our best practice needs to be the focus of our drive to further improve the effectiveness of our approach, which we had committed will be community powered, clinically led, and system enabled. That ‘internal’ system is now fit for purpose and no significant internal control issues have been identified, but it can be improved in the specific respects outlined by my review and that of our auditors and advisors. This view has been discussed with our audit committee, board of directors and council of governors.
Accountability report signed on behalf of the board of directors.
Toby Lewis, Chief Executive 26 June 2025
Auditors report
Independent auditor’s report to the Council of Governors and Board of Directors of Rotherham Doncaster and South Humber NHS Foundation Trust.
Report on the audit of the financial statements
Opinion
In our opinion the financial statements of Rotherham Doncaster and South Humber NHS Foundation Trust (the “foundation trust” or the “trust”) and its subsidiaries (the “group”):
- give a true and fair view of the state of the group’s and the foundation trust’s affairs as at 31 March 2025 and of the group’s and foundation trust’s income and expenditure for the year then ended;
- have been properly prepared in accordance with the accounting requirements of the Department of Health and Social Care Group Accounting Manual, as directed by NHS England; and
- have been prepared in accordance with the requirements of the National Health Service Act 2006.
We have audited the financial statements which comprise:
- the Consolidated Statement of Comprehensive Income;
- the Consolidated and trust Statement of Financial Position;
- the group and trust Statements of Changes in Equity;
- the group and trust Statements of Cash Flows; and
- the related notes 1 to 38.
The financial reporting framework that has been applied in their preparation is applicable law and the accounting requirements of the Department of Health and Social Care Group Accounting Manual, as directed by NHS England.
Basis for opinion
We conducted our audit in accordance with International Standards on Auditing (UK) (ISAs (UK)), the Code of Audit Practice issued by the Comptroller and Auditor General and applicable law. Our responsibilities under those standards are further described in the auditor’s responsibilities for the audit of the financial statements section of our report.
We are independent of the group and the foundation trust in accordance with the ethical requirements that are relevant to our audit of the financial statements in the UK, including the Financial Reporting Council’s (the ‘FRC’s’) Ethical Standard, and we have fulfilled our other ethical responsibilities in accordance with these requirements. We believe that the audit evidence we have obtained is sufficient and appropriate to provide a basis for our opinion.
Conclusions relating to going concern
In auditing the financial statements, we have concluded that the accounting officer’s use of the going concern basis of accounting in the preparation of the financial statements is appropriate.
Based on the work we have performed, we have not identified any material uncertainties relating to events or conditions that, individually or collectively, may cast significant doubt on the Group’s and the foundation trust’s ability to continue as a going concern for a period of at least twelve months from when the financial statements are authorised for issue.
Our responsibilities and the responsibilities of the directors with respect to going concern are described in the relevant sections of this report.
The going concern basis of accounting for the Group and the foundation trust is adopted in consideration of the requirements set out in the Department of Health and Social Care Group Accounting Manual which require entities to adopt the going concern basis of accounting in the preparation of the financial statements where it is anticipated that the services which they provide will continue into the future.
Other information
The other information comprises the information included in the annual report, other than the financial statements and our auditor’s report thereon. The accounting officer is responsible for the other information contained within the annual report. Our opinion on the financial statements does not cover the other information and, except to the extent otherwise explicitly stated in our report, we do not express any form of assurance conclusion thereon.
Our responsibility is to read the other information and, in doing so, consider whether the other information is materially inconsistent with the financial statements or our knowledge obtained in the course of the audit, or otherwise appears to be materially misstated. If we identify such material inconsistencies or apparent material misstatements, we are required to determine whether this gives rise to a material misstatement in the financial statements themselves. If, based on the work we have performed, we conclude that there is a material misstatement of this other information, we are required to report that fact.
We have nothing to report in this regard.
Responsibilities of accounting officer
As explained more fully in the Statement of the chief executive’s responsibilities as the accounting officer of Rotherham Doncaster and South Humber NHS Foundation Trust, the accounting officer is responsible for the preparation of the financial statements and for being satisfied that they give a true and fair view, and for such internal control as the accounting officer determines is necessary to enable the preparation of financial statements that are free from material misstatement, whether due to fraud or error.
In preparing the financial statements, the accounting officer is responsible for assessing the group’s and the foundation trust’s ability to continue as a going concern, disclosing, as applicable, matters related to going concern and using the going concern basis of accounting unless they have been informed by the relevant national body of the intention to dissolve the foundation trust without the transfer of the foundation trust’s services to another public sector entity.
Auditor’s responsibilities for the audit of the financial statements
Our objectives are to obtain reasonable assurance about whether the financial statements as a whole are free from material misstatement, whether due to fraud or error, and to issue an auditor’s report that includes our opinion. Reasonable assurance is a high level of assurance, but is not a guarantee that an audit conducted in accordance with ISAs (UK) will always detect a material misstatement when it exists. Misstatements can arise from fraud or error and are considered material if, individually or in the aggregate, they could reasonably be expected to influence the economic decisions of users taken on the basis of these financial statements.
A further description of our responsibilities for the audit of the financial statements is located on the FRC’s website. This description forms part of our auditor’s report.
Extent to which the audit was considered capable of detecting non-compliance with laws and regulations, including fraud
Irregularities, including fraud, are instances of non-compliance with laws and regulations. We design procedures in line with our responsibilities, outlined above, to detect material misstatements in respect of irregularities, including fraud. The extent to which our procedures are capable of detecting irregularities, including fraud is detailed below.
We considered the nature of the Group and its control environment, and reviewed the Group’s documentation of their policies and procedures relating to fraud and compliance with laws and regulations. We also enquired of management, internal audit and local counter fraud about their own identification and assessment of the risks of irregularities, including those that are specific to the National Health Service and public sector.
We obtained an understanding of the legal and regulatory framework that the Group operates in, and identified the key laws and regulations that:
- had a direct effect on the determination of material amounts and disclosures in the financial statements. This included the National Health Service Act 2006
- do not have a direct effect on the financial statements but compliance with which may be fundamental to the Group’s ability to operate or to avoid a material penalty. These included the Data Protection Act 2018 and relevant employment legislation
We discussed among the audit engagement team including relevant internal specialists such as valuations, pensions and IT regarding the opportunities and incentives that may exist within the organisation for fraud and how and where fraud might occur in the financial statements.
As a result of performing the above, we identified the greatest potential for fraud in the following area, and our specific procedures performed to address it are described below: the validity of accruals recorded at 31 March 2025 and the timing of their recognition are subject to potential management bias: we tested a sample of accruals to supporting documentation to assess whether the liability had been incurred as at 31 March 2025.
In common with all audits under ISAs (UK), we are also required to perform specific procedures to respond to the risk of management override. In addressing the risk of fraud through management override of controls, we tested the appropriateness of journal entries and other adjustments; assessed whether the judgements made in making accounting estimates are indicative of a potential bias; and evaluated the business rationale of any significant transactions that are unusual or outside the normal course of business.
In addition to the above, our procedures to respond to the risks identified included the following:
- reviewing financial statement disclosures by testing to supporting documentation to assess compliance with provisions of relevant laws and regulations described as having a direct effect on the financial statements
- performing analytical procedures to identify any unusual or unexpected relationships that may indicate risks of material misstatement due to fraud
- enquiring of management and internal audit concerning actual and potential litigation and claims, and instances of non-compliance with laws and regulations; and
- reading minutes of meetings of those charged with governance and reviewing internal audit reports.
Report on other legal and regulatory requirements
Opinions on other matters prescribed by the National Health Service Act 2006
In our opinion:
- the parts of the Remuneration Report and Staff Report subject to audit have been prepared properly in accordance with the National Health Service Act 2006 in all material respects; and
- the information given in the Performance Report and the Accountability Report for the financial year for which the financial statements are prepared is consistent with the financial statements.
Matters on which we are required to report by exception
Use of resources
Under the Code of Audit Practice and Schedule 10(1(d)) of the National Health Service Act 2006, we are required to report to you if we have not been able to satisfy ourselves that the foundation trust has made proper arrangements for securing economy, efficiency and effectiveness in its use of resources.
We have nothing to report in respect of this matter.
Respective responsibilities of the accounting officer and auditor relating to the Foundation Trust’s arrangements for securing economy, efficiency and effectiveness in the use of resources
The accounting officer is responsible for putting in place proper arrangements to secure economy, efficiency and effectiveness in the use of the foundation trust’s resources.
We are required under the Code of Audit Practice and Schedule 10(1(d)) of the National Health Service Act 2006 to satisfy ourselves that the foundation trust has made proper arrangements for securing economy, efficiency and effectiveness in its use of resources.
We are not required to consider, nor have we considered, whether all aspects of the foundation trust’s arrangements for securing economy, efficiency and effectiveness in its use of resources are operating effectively.
We undertake our work in accordance with the Code of Audit Practice, having regard to the Auditor Guidance Notes issued by the Comptroller and Auditor General, as to whether the foundation trust has proper arrangements for securing economy, efficiency and effectiveness in the use of resources against the specified criteria of financial sustainability, governance, and improving economy, efficiency and effectiveness.
The Comptroller and Auditor General has determined that under the Code of Audit Practice, we discharge this responsibility by reporting by exception if we have reported to the foundation trust a significant weakness in arrangements to secure economy, efficiency and effectiveness in its use of resources for the year ended 31 March 2025. Other findings from our work, including our commentary on the foundation trust’s arrangements, will be reported in our separate Auditor’s Annual Report.
Annual governance statement and compilation of financial statements
Under the Code of Audit Practice, we are required to report to you if, in our opinion:
- the Annual Governance Statement does not meet the disclosure requirements set out in the NHS Foundation Trust Annual Reporting Manual, is misleading, or is inconsistent with information of which we are aware from our audit; or
- proper practices have not been observed in the compilation of the financial statements
We are not required to consider, nor have we considered, whether the Annual Governance Statement addresses all risks and controls or that risks are satisfactorily addressed by internal controls.
We have nothing to report in respect of these matters.
Reports in the public interest or to the regulator
Under the Code of Audit Practice, we are also required to report to you if:
- any matters have been reported in the public interest under Schedule 10(3) of the National Health Service Act 2006 in the course of, or at the end of the audit; or
- any reports to the regulator have been made under Schedule 10(6) of the National Health Service Act 2006 because we have reason to believe that the foundation trust, or a director or officer of the foundation trust, is about to make, or has made, a decision involving unlawful expenditure, or is about to take, or has taken, unlawful action likely to cause a loss or deficiency.
We have nothing to report in respect of these matters.
Certificate of completion of the audit
As at the date of this audit report, we have not yet completed our work in respect of the trust’s consolidation returns for the year ended 31 March 2025 and have not received confirmation from the National Audit Office that the audit of the NHS group consolidation is complete.
In accordance with Auditor Guidance Note 07, we are therefore unable to certify that we have completed our audit of Rotherham Doncaster and South Humber NHS Foundation Trust for the year ended 31 March 2025 in accordance with the requirements of the National Health Service Act 2006 and the National Audit Office Code of Audit Practice. We are satisfied that our remaining work in this area is unlikely to have a material impact on the financial statements.
Use of our report
This report is made solely to the Council of Governors and Board of Directors (the boards) of Rotherham Doncaster and South Humber NHS Foundation Trust, as a body, in accordance with paragraph 4 of Schedule 10 of the National Health Service Act 2006. Our audit work has been undertaken so that we might state to the Boards those matters we are required to state to them in an auditor’s report and for no other purpose. To the fullest extent permitted by law, we do not accept or assume responsibility to anyone other than the Boards as a body, for our audit work, for this report, or for the opinions we have formed.
Kenny (Key Audit Partner), for and on behalf of Deloitte LLP, Appointed Auditor, Newcastle upon Tyne, United Kingdom, 30 June 2025.
Accounts
Foreword to the accounts
These accounts, for the year ended 31 March 2025, have been prepared by Rotherham Doncaster and South Humber NHS Foundation Trust in accordance with paragraphs 24 and 25 of Schedule 7 within the National Health Service Act 2006.
Toby Lewis Job, Chief Executive, 26 June 2025.
| Category | Note | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|---|
| Operating income from patient care activities | 3 | 235,706 | 212,521 |
| Other operating income | 4 | 13,372 | 12,738 |
| Operating expenses | 6 | (247,878) | (226,162) |
| Operating surplus or (deficit) | 1,200 | (903) | |
| Finance income | 11 | 1,873 | 2,157 |
| Finance expenses | 12 | (1,898) | (1,602) |
| PDC dividends payable | (2,257) | (1,992) | |
| Net finance costs | (2,282) | (1,437) | |
| Other gains | 13 | 54 | 17 |
| (Deficit) for the year | (1,028) | (2,323) |
| Category | Note | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|---|
| Will not be reclassified to income and expenditure: Impairments 7 | 7 | (1,640) | (4,959) |
| Will not be reclassified to income and expenditure: revaluations | 16 and 17 | 1,334 | 6,847 |
| Will not be reclassified to income and expenditure: remeasurements of the net defined benefit pension scheme liability or asset | 33 | (162) | (244) |
| May be reclassified to income and expenditure when certain conditions are met: fair value gains on financial assets mandated at fair value through OCI | 20 | 28 | 84 |
| May be reclassified to income and expenditure when certain conditions are met: other comprehensive (expense) or income for the year, net of tax | (440) | 1,728 | |
| Total comprehensive (expense) for the period | (1,468) | (595) |
| Non-current assets | Note | Group 31 March 2025 (£000) | Group 31 March 2024 (£000) | Trust 31 March 2025 (£000) | Trust 31 March 2024 (£000) |
|---|---|---|---|---|---|
| Intangible assets | 15 | 2,372 | 2,058 | 2,372 | 2,058 |
| Property, plant and equipment | 16 | 94,045 | 91,910 | 94,045 | 93,130 |
| Right of use assets | 19 | 12,492 | 11,580 | 12,492 | 11,580 |
| Investment property | 18 | 3,670 | 3,579 | 3,670 | 3,129 |
| Other investments or financial assets | 20 | 1,447 | 2,082 | 22 | 22 |
| Receivables | 24 | 145 | 98 | 145 | 98 |
| Pension asset | 33 | 143 | 143 | ||
| Total non-current assets | 114,171 | 111,450 | 112,746 | 110,160 |
| Current assets | Note | Group 31 March 2025 (£000) | Group 31 March 2024 (£000) | Trust 31 March 2025 (£000) | Trust 31 March 2024 (£000) |
|---|---|---|---|---|---|
| Inventories | 23 | 315 | 620 | 299 | 602 |
| Receivables | 24 | 7,297 | 6,339 | 7,340 | 6,667 |
| Non-current assets held for sale | 25 | 86 | 86 | ||
| Cash and cash equivalents | 26 | 32,208 | 34,411 | 31,421 | 33,447 |
| Total current assets | 39,906 | 41,370 | 39,146 | 40,716 |
| Current liabilities | Note | Group 31 March 2025 (£000) | Group 31 March 2024 (£000) | Trust 31 March 2025 (£000) | Trust 31 March 2024 (£000) |
|---|---|---|---|---|---|
| Trade and other payables | 27 | (16,395) | (16,010) | (16,200) | (15,744) |
| Borrowings | 29 | (3,181) | (2,768) | (3,181) | (2,768) |
| Provisions | 30 | (653) | (87) | (653) | (87) |
| Other liabilities | 28 | (294) | (403) | (167) | (291) |
| Total current liabilities | (20,523) | (19,268) | (20,201) | (18,890) | |
| Total assets less current liabilities | 133,554 | 133,552 | 131,691 | 131,986 |
| Non-current liabilities | Note | Group 31 March 2025 (£000) | Group 31 March 2024 (£000) | Trust 31 March 2025 (£000) | Trust 31 March 2024 (£000) |
|---|---|---|---|---|---|
| Borrowings | 29 | (28,841) | (29,588) | (28,841) | (29,588) |
| Provisions | 30 | (734) | (857) | (734) | (857) |
| Total non-current liabilities | (29,575) | (30,445) | (29,575) | (30,445) | |
| Total assets employed | 103,979 | 103,107 | 102,116 | 101,541 |
| Financer | Note | Group 31 March 2025 (£000) | Group 31 March 2024 (£000) | Trust 31 March 2025 (£000) | Trust 31 March 2024 (£000) |
|---|---|---|---|---|---|
| Public dividend capital | 44,870 | 42,530 | 44,870 | 42,530 | |
| Revaluation reserve | 37,307 | 37,613 | 37,307 | 38,383 | |
| Income and expenditure reserve | 19,985 | 20,672 | 19,939 | 20,628 | |
| Charitable fund reserves | 22 | 1,817 | 2,292 | ||
| Total taxpayers’ equity | 103,979 | 103,107 | 102,116 | 101,541 |
The notes to accounts to related parties form part of these accounts.
Toby Lewis, Chief Executive, 26 June 2025.
| Group | Note | Public dividend capital (£000) | Revaluation reserve (£000) | Income and expenditure reserve (£000) | Charitable fund reserves (£000) | Total (£000) |
|---|---|---|---|---|---|---|
| Taxpayers’ and others’ equity at 1 April 2024 – brought forward | 42,530 | 37,613 | 20,672 | 2,292 | 103,107 | |
| (Deficit) for the year | (525) | (503) | (1,028) | |||
| Net Impairments | 7 and 16 | (1,640) | (1,640) | |||
| Revaluations | 16 and 17 | 1,334 | 1,334 | |||
| Fair value gains on financial assets mandated at fair value through OCI | 28 | 28 | ||||
| Remeasurements of the defined net benefit pension scheme liability or asset | 33 | (162) | (162) | |||
| Total comprehensive (expense) for the period | (306) | (687) | (475) | (1,468) | ||
| Public dividend capital received | 2,340 | 2,340 | ||||
| Taxpayers’ and others’ equity at 31 March 2025 | 44,870 | 37,307 | 19,985 | 1,817 | 103,979 |
| Group | Note | Public dividend capital (£000) | Revaluation reserve (£000) | Income and expenditure reserve (£000) | Charitable fund reserves (£000) | Total (£000) |
|---|---|---|---|---|---|---|
| Taxpayers’ and others’ equity at 1 April 2023 – brought forward | 40,855 | 35,725 | 29,180 | 2,867 | 108,627 | |
| Application of IFRS 16 measurement principles to Private Finance Initiative liability on 1 April 2023 | (6,600) | (6,600) | ||||
| (Deficit) for the year | (1,664) | (659) | (2,323) | |||
| Net Impairments | 7 and 16 | (4,959) | (4,959) | |||
| Revaluations | 16 and 17 | 6,847 | 6,847 | |||
| Fair value gains on financial assets mandated at fair value through OCI | 84 | 84 | ||||
| Remeasurements of the defined net benefit pension scheme liability or asset | 33 | (244) | (244) | |||
| Public dividend capital received | 1,675 | 1,675 | ||||
| Taxpayers’ and others’ equity at 31 March 2024 | 42,530 | 37,613 | 20,672 | 2,292 | 103,107 |
| Trust | Note | Public dividend capital (£000) | Revaluation reserve (£000) | Income and expenditure reserve (£000) | Total (£000) |
|---|---|---|---|---|---|
| Taxpayers’ and others’ equity at 1 April 2024 – brought forward | 42,530 | 38,383 | 20,628 | 101,541 | |
| (Deficit) for the year | (527) | (527) | |||
| Impairments | 7 and 16 | (1,640) | (1,640) | ||
| Revaluations | 16 and 17 | 1,334 | 1,334 | ||
| Other: trust only Investment Property classification | (770) | (770) | |||
| Remeasurements of the defined net benefit pension scheme liability or asset | 33 | (162) | (162) | ||
| Total comprehensive (expense) for the period | (1,076) | (689) | (1,765) | ||
| Public dividend capital received | 2,340 | 2,340 | |||
| Taxpayers’ and others’ equity at 31 March 2025 | 44,870 | 37,307 | 19,939 | 102,116 |
| Trust | Note | Public dividend capital (£000) | Revaluation reserve (£000) | Income and expenditure reserve (£000) | Total (£000) |
|---|---|---|---|---|---|
| Taxpayers’ and others’ equity at 1 April 2023 – brought forward | 40,855 | 36,446 | 29,138 | 106,439 | |
| (Deficit) for the year | (1,666) | (1,666) | |||
| (Deficit) for the year | 7 and 16 | (4,959) | (4,959) | ||
| Revaluations | 16 and 17 | 6,847 | 6,847 | ||
| Remeasurements of the defined net benefit pension scheme liability or asset | 33 | (244) | (244) | ||
| Public dividend capital received | 1,675 | 1,675 | |||
| Other: trust only Investment Property classification | 49 | 49 | |||
| Taxpayers’ and others’ equity at 31 March 2024 | 42,530 | 38,383 | 20,628 | 101,541 |
Information on reserves
Public dividend capital
Public dividend capital (PDC) is a type of public sector equity finance based on the excess of assets over liabilities at the time of establishment of the predecessor NHS organisation. Additional PDC may also be issued to trusts by the Department of Health and Social Care. A charge, reflecting the cost of capital utilised by the trust, is payable to the Department of Health and Social Care as the public dividend capital dividend.
Revaluation reserve
Increases in asset values arising from revaluations are recognised in the revaluation reserve, except where, and to the extent that, they reverse impairments previously recognised in operating expenses, in which case they are recognised in operating income. Subsequent downward movements in asset valuations are charged to the revaluation reserve to the extent that a previous gain was recognised unless the downward movement represents a clear consumption of economic benefit or a reduction in service potential.
Income and expenditure reserve
The balance of this reserve is the accumulated surpluses and deficits.
Charitable funds reserve
This reserve comprises the ring-fenced funds held by the NHS charitable funds consolidated within these financial statements. These reserves are classified as restricted or unrestricted; a breakdown is provided in note 22.
Statements of cash flows
| Cash flow | Note | Group 2024 and 2025 (£000) | Group 2023 and 2024 (£000) | Trust 2024 and 2025 (£000) | Trust 2023 and 2024 (£000) |
|---|---|---|---|---|---|
| Operating surplus or (deficit) | 1,200 | (903) | 1,774 | (160) |
| Cash flow | Note | Group 2024 and 2025 (£000) | Group 2023 and 2024 (£000) | Trust 2024 and 2025 (£000) | Trust 2023 and 2024 (£000) |
|---|---|---|---|---|---|
| Depreciation and amortisation | 6 | 6,553 | 6,122 | 6,553 | 6,122 |
| Net impairments | 7 | (41) | (1,451) | (41) | (1,451) |
| Income recognised in respect of capital donations | (44) | (217) | (44) | (217) | |
| Non-cash movements in on-SoFP pension liability | (19) | 83 | (19) | 83 | |
| (Increase) or decrease in receivables and other assets | (981) | 7,161 | (695) | 6,811 | |
| Decrease or (increase) in inventories | 305 | (115) | 305 | (115) | |
| (Decrease) in payables | (235) | (6,533) | (164) | (6,503) | |
| (Decrease) in other liabilities | (109) | (982) | (124) | (1,094) | |
| Increase or (decrease) in provisions | 430 | (287) | 430 | (287) | |
| Movements in charitable fund working capital | 2 | (46) | |||
| Other movements in operating cash flows | (42) | 2 | (40) | 1 | |
| Net cash flows from operating activities | 7,019 | 2,834 | 7,933 | 3,190 |
| Cash flow | Group 2024 and 2025 (£000) | Group 2023 and 2024 (£000) | Trust 2024 and 2025 (£000) | Trust 2023 and 2024 (£000) |
|---|---|---|---|---|
| Cash flows from investing activities interest received | 1,805 | 1,989 | 1,800 | 1,988 |
| Purchase of intangible assets | (833) | (271) | (833) | (271) |
| Purchase of PPE and investment property | (6,274) | (6,425) | (6,274) | (6,425) |
| Sales of PPE and investment property | 9 | 9 | ||
| Receipt of cash donations to purchase assets | 25 | 25 | ||
| Cash flows from charitable fund investing activities | 87 | 169 | ||
| Net cash flows (used in) investing activities | (5,206) | (4,513) | (5,298) | (4,683) |
| Cash flow | Group 2024 and 2025 (£000) | Group 2023 and 2024 (£000) | Trust 2024 and 2025 (£000) | Trust 2023 and 2024 (£000) |
|---|---|---|---|---|
| Public dividend capital received | 2,340 | 1,675 | 2,340 | 1,675 |
| Movement on loans from Department of Health and Social Care | (363) | (363) | (363) | (363) |
| Capital element of lease liability repayments | (1,337) | (1,311) | (1,337) | (1,311) |
| Capital element of private finance initiative, local improvement finance trusts and other service concession payments | (1,224) | (1,647) | (1,224) | (1,647) |
| Interest on loans | (144) | (158) | (144) | (158) |
| Interest element of lease liability repayments | (147) | (144) | (147) | (144) |
| Interest paid on Private Finance Initiative, Local Improvement Finance trusts and other service concession obligations | (1,157) | (661) | (1,157) | (661) |
| Net cash flows from charitable fund financing activities | 645 | 445 | ||
| PDC dividend (paid) or refunded | (2,629) | (2,041) | (2,629) | (2,041) |
| Net cash flows (used in) financing activities | (4,016) | (4,205) | (4,661) | (4,650) |
| (decrease) in cash and cash equivalents | (2,203) | (5,884) | (2,026) | (6,143) |
| Cash flow | Note | Group 2024 and 2025 (£000) | Group 2023 and 2024 (£000) | Trust 2024 and 2025 (£000) | Trust 2023 and 2024 (£000) |
|---|---|---|---|---|---|
| Cash and cash equivalents at 1 April – brought forward | 34,411 | 40,295 | 33,447 | 39,590 | |
| Cash and cash equivalents at 31 March | 26 | 32,208 | 34,411 | 31,421 | 33,447 |
Notes to the accounts
Note 1 accounting policies and other information
Note 1.1 basis of preparation
NHS England has directed that the financial statements of the trust shall meet the accounting requirements of the Department of Health and Social Care Group Accounting Manual (GAM), which shall be agreed with HM Treasury. Consequently, the following financial statements have been prepared in accordance with the GAM 2024 and 2025 issued by the Department of Health and Social Care. The accounting policies contained in the GAM follow International Financial Reporting Standards to the extent that they are meaningful and appropriate to the NHS, as determined by HM Treasury, which is advised by the Financial Reporting Advisory Board. Where the GAM permits a choice of accounting policy, the accounting policy that is judged to be most appropriate to the particular circumstances of the trust for the purpose of giving a true and fair view has been selected. The particular policies adopted are described below. These have been applied consistently in dealing with items considered material in relation to the accounts.
Accounting convention
These accounts have been prepared under the historical cost convention modified to account for the revaluation of property, plant and equipment, investment properties and certain financial assets and financial liabilities.
Note 1.2 going concern
These accounts have been prepared on a going concern basis. The financial reporting framework applicable to NHS bodies, derived from the HM Treasury Financial Reporting Manual, defines that the anticipated continued provision of the entity’s services in the public sector is normally sufficient evidence of going concern. The directors have a reasonable expectation that this will continue to be the case.
Note 1.3 consolidation
NHS charitable fund
The trust is the corporate trustee to the Rotherham Doncaster and South Humber NHS charitable fund. The trust has assessed its relationship to the charitable fund and determined it to be a subsidiary because the trust is exposed to, or has rights to, variable returns and other benefits for itself, patients, and staff from its involvement with the charitable fund and could affect those returns and other benefits through its power over the fund.
The charitable fund’s statutory accounts are prepared to 31 March each year in accordance with the UK Charities Statement of Recommended Practice (SORP) which is based on UK Financial Reporting Standard (FRS) 102. On consolidation, necessary adjustments are made to the charity’s assets, liabilities, and transactions to:
- recognise and measure them in accordance with the trust’s accounting policies and
- eliminate intra-group transactions, balances, gains and losses
Other subsidiaries
Flourish Enterprises Community Interest Company (Flourish) is a wholly owned subsidiary of the trust.
Subsidiary entities are those over which a trust is exposed to, or has rights to, variable returns from its involvement with the entity and can affect those returns through its power over the entity. The income, expenses, assets, liabilities, equity and reserves of subsidiaries are consolidated in full into the appropriate financial statement lines.
The amounts consolidated are drawn from the financial statements of the subsidiary for the year ended 31 March 2025.
Flourish prepares its financial statements in accordance with Financial Reporting Standard 102.
Where subsidiaries’ accounting policies are not aligned with those of the trust (including where they report under UK FRS 102), then amounts are adjusted during consolidation where the differences are material. Inter-entity balances, transactions and gains or losses are eliminated in full on consolidation.
Note 1.4 revenue from contracts with customers
Where income is derived from contracts with customers, it is accounted for under IFRS 15. The GAM expands the definition of a contract to include legislation and regulations which enables an entity to receive cash or another financial asset that is not classified as a tax by the Office of National Statistics (ONS).
Revenue in respect of goods or services provided is recognised when (or as) performance obligations are satisfied by transferring promised goods or services to the customer and is measured at the amount of the transaction price allocated to those performance obligations. At the year end, the trust accrues income relating to performance obligations satisfied in that year. Where the trust’s entitlement to consideration for those goods or services is unconditional a contract receivable will be recognised. Where entitlement to consideration is conditional on a further factor other than the passage of time, a contract asset will be recognised. Where consideration received or receivable relates to a performance obligation that is to be satisfied in a future period, the income is deferred and recognised as a contract liability.
Payment is typically received within thirty days of the satisfaction of the performance obligations and as such has no impact on contract balances.
Revenue from NHS contracts
The main source of income for the trust is contracts with commissioners for health care services. Funding envelopes are set at an Integrated Care System (ICS) level. The majority of the trust’s NHS income is earned from NHS commissioners under the NHS Payment Scheme (NHSPS). The NHSPS sets out rules to establish the amount payable to trusts for NHS-funded secondary healthcare.
The trust also receives income from commissioners under the Commissioning for Quality Innovation (CQUIN) scheme. Delivery under this scheme is part of how care is provided to patients. As such CQUIN payments are not considered distinct performance obligations in their own right; instead they form part of the transaction price for performance obligations under the overall contract with the commissioner and are accounted for as variable consideration under IFRS 15. Payment for CQUIN is included in the fixed element of API contracts with adjustments for actual achievement being made at the end of the year.
Where the relationship with a particular integrated care board is expected to be a low volume of activity (annual value below £500,000), an annual fixed payment is received by the provider as determined in the NHSPS documentation. Such income is classified as ‘other clinical income’ in these accounts.
Elective recovery funding provides additional funding to integrated care boards to fund the commissioning of elective services within their systems. Trusts do not directly earn elective recovery funding, instead earning income for actual activity performed under API contract arrangements. The level of activity delivered by the trust contributes to system performance and therefore the availability of funding to the trust’s commissioners.
Mental health provider collaboratives
NHS led provider collaboratives for specialised mental health, learning disability and autism services involve an NHS lead provider taking responsibility for managing services, care pathways and specialised commissioning budgets for a population. As lead provider for the South Yorkshire Adult Eating Disorder Provider Collaborative, the trust is accountable to NHS England and as such recognises the income and expenditure associated with the commissioning of services from other providers in these financial statements. Where the trust is the provider of commissioned services, this element of income is recognised in the provision of services, after eliminating internal transactions.
Revenue from research contracts
Where research contracts fall under IFRS 15, revenue is recognised as and when performance obligations are satisfied. For some contracts, it is assessed that the revenue project constitutes one performance obligation over the course of the multi-year contract. In these cases, it is assessed that the trust’s interim performance does not create an asset with alternative use for the trust, and the trust has an enforceable right to payment for the performance completed to date. It is therefore considered that the performance obligation is satisfied over time, and the trust recognises revenue each year over the course of the contract. Some research income alternatively falls within the provisions of IAS 20 for government grants.
Note 1.5 other forms of income
Grants and donations
Government grants are grants from government bodies other than income from commissioners or trusts for the provision of services. Where a grant is used to fund revenue expenditure it is taken to the Statement of Comprehensive Income (SOCI) to match that expenditure. Where the grants are used to fund capital expenditure, they are credited to the consolidated statement of comprehensive income once conditions attached to the grant have been met. Donations are treated in the same way as government grants.
Apprenticeship service income
The value of the benefit received when accessing funds from the Government’s apprenticeship service is recognised as income at the point of receipt of the training service. Where these funds are paid directly to an accredited training provider from the trust’s apprenticeship service account held by the Department for Education, the corresponding notional expense is also recognised at the point of recognition for the benefit.
Note 1.6 expenditure on employee benefits
Short-term employee benefits
Salaries, wages and employment-related payments such as social security costs and the apprenticeship levy are recognised in the period in which the service is received from employees. The cost of annual leave entitlement earned but not taken by employees at the end of the period is recognised in the financial statements to the extent that employees are permitted to carry-forward leave into the following period.
Pension costs: NHS Pension Scheme
Past and present employees are covered by the provisions of the two NHS Pension Schemes. Both schemes are unfunded, defined benefit schemes that cover NHS employers, general practices and other bodies, allowed under the direction of Secretary of State for Health and Social Care in England and Wales. The scheme is not designed in a way that would enable employers to identify their share of the underlying scheme assets and liabilities. Therefore, the scheme is accounted for as though it is a defined contribution scheme: the cost to the trust is taken as equal to the employer’s pension contributions payable to the scheme for the accounting period. The contributions are charged to operating expenses as and when they become due.
Additional pension liabilities arising from early retirements are not funded by the scheme except where the retirement is due to ill-health. The full amount of the liability for the additional costs is charged to the operating expenses at the time the trust commits itself to the retirement, regardless of the method of payment.
Pension costs: Local Government Pension Scheme
There are trust employees that are members of the Local Government Pension Scheme which is a defined benefit pension scheme. The scheme assets and liabilities attributable to these employees can be identified and are recognised in the trust’s accounts. The assets are measured at fair value, and the liabilities at the present value of future obligations.
The increase in the liability arising from pensionable service earned during the year is recognised within operating expenses. The net interest cost during the year arising from the unwinding of the discount on the net scheme liabilities is recognised within finance costs. Remeasurements of the defined benefit plan are recognised in the income and expenditure reserve and reported in the Statement of Comprehensive Income as an item of ‘other comprehensive income’.
The trust’s involvement with the Local Government Pension Scheme is subject to an asset ceiling or cap which limits the asset value recorded within these accounts.
Note 1.7 expenditure on other goods and services
Expenditure on goods and services is recognised when, and to the extent that they have been received, and is measured at the fair value of those goods and services. Expenditure is recognised in operating expenses except where it results in the creation of a non-current asset such as property, plant and equipment.
Note 1.8 property, plant and equipment
Recognition
Property, plant and equipment is capitalised where:
- it is held for use in delivering services or for administrative purposes
- it is probable that future economic benefits will flow to, or service potential be provided to, the trust
- it is expected to be used for more than one financial year
- the cost of the item can be measured reliably
- the item has cost of at least £5,000, or
- collectively, a number of items have a cost of at least £5,000 and individually have cost of more than £250, where the assets are functionally interdependent, had broadly simultaneous purchase dates, are anticipated to have similar disposal dates and are under single managerial control.
Where a large asset, for example a building, includes a number of components with significantly different asset lives, for example, plant and equipment, then these components are treated as separate assets and depreciated over their own useful lives.
Subsequent expenditure
Subsequent expenditure relating to an item of property, plant and equipment is recognised as an increase in the carrying amount of the asset when it is probable that additional future economic benefits or service potential deriving from the cost incurred to replace a component of such item will flow to the enterprise and the cost of the item can be determined reliably. Where a component of an asset is replaced, the cost of the replacement is capitalised if it meets the criteria for recognition above. The carrying amount of the part replaced is de-recognised. Other expenditure that does not generate additional future economic benefits or service potential, such as repairs and maintenance, is charged to the Statement of Comprehensive Income in the period in which it is incurred.
Impairments
In accordance with the GAM, impairments that arise from a clear consumption of economic benefits or of service potential in the asset are charged to operating expenses. A compensating transfer is made from the revaluation reserve to the income and expenditure reserve of an amount equal to the lower of (i) the impairment charged to operating expenses; and (ii) the balance in the revaluation reserve attributable to that asset before the impairment.
An impairment that arises from a clear consumption of economic benefit or of service potential is reversed when, and to the extent that, the circumstances that gave rise to the loss is reversed. Reversals are recognised in operating expenditure to the extent that the asset is restored to the carrying amount it would have had if the impairment had never been recognised. Any remaining reversal is recognised in the revaluation reserve. Where, at the time of the original impairment, a transfer was made from the revaluation reserve to the income and expenditure reserve, an amount is transferred back to the revaluation reserve when the impairment reversal is recognised.Other impairments are treated as revaluation losses. Reversals of ‘other impairments’ are treated as revaluation gains.
Measurement: valuation
All property, plant and equipment assets are measured initially at cost, representing the costs directly attributable to acquiring or constructing the asset and bringing it to the location and condition necessary for it to be capable of operating in the manner intended by management. Assets are measured subsequently at valuation.
Assets which are held for their service potential and are in use (that is, operational assets used to deliver either front line services or back office functions) are measured at their current value in existing use. Assets that were most recently held for their service potential but are surplus with no plan to bring them back into use are measured at fair value where there are no restrictions on sale at the reporting date and where they do not meet the definitions of investment properties or assets held for sale.
Revaluations of property, plant and equipment are performed with sufficient regularity to ensure that carrying values are not materially different from those that would be determined at the end of the reporting period. Current values in existing use are determined as follows:
- Land and non-specialised buildings – market value for existing use
- Specialised buildings – depreciated replacement cost on a modern equivalent asset basis.
For specialised assets, current value in existing use is interpreted as the present value of the asset’s remaining service potential, which is assumed to be at least equal to the cost of replacing that service potential. Specialised assets are therefore valued at their depreciated replacement cost (DRC) on a modern equivalent asset (MEA) basis. An MEA basis assumes that the asset will be replaced with a modern asset of equivalent capacity and meeting the location requirements of the services being provided. Assets held at depreciated replacement cost are valued on an alternative site basis.
Valuation guidance issued by the Royal Institute of Chartered Surveyors states that valuations are performed net of VAT where the VAT is recoverable by the entity. This basis has been applied to the trust’s Private Finance Initiative (PFI) scheme where the construction is completed by a special purpose vehicle and the costs have recoverable VAT for the trust.
Properties in the course of construction for service or administration purposes are carried at cost, less any impairment loss (if any). Cost includes professional fees. Assets are revalued and depreciation commences when the assets are brought into use.
IT equipment, transport equipment, furniture and fittings, and plant and machinery that are held for operational use are valued at depreciated historic cost where these assets have short useful lives or low values or both, as this is not considered to be materially different from current value in existing use. Assets which are not sufficiently low value and, or do not have sufficiently short lives are valued at depreciated historic cost as a proxy for current value in existing use.
Measurement: depreciation
Items of property, plant and equipment are depreciated, on a straight line basis, over their remaining useful lives in a manner consistent with the consumption of economic or service delivery benefits. Freehold land is considered to have an infinite life and is not depreciated. Property, plant and equipment which has been reclassified as ‘held for sale’ cease to be depreciated upon the reclassification. Assets in the course of construction are not depreciated until the asset is brought into use.
Measurement: revaluation gains and losses
Revaluation gains are recognised in the revaluation reserve, except where, and to the extent that, they reverse a revaluation decrease that has previously been recognised in operating expenses, in which case they are recognised in operating expenditure.
Revaluation losses (impairments) are charged to the revaluation reserve to the extent that there is an available balance for the asset concerned, and thereafter are charged to operating expenses.
Gains and losses recognised in the revaluation reserve are reported in the Statement of Comprehensive Income as an item of ‘other comprehensive income’.
De-recognition
Assets intended for disposal are reclassified as ‘held for sale’ once the criteria in IFRS 5 are met. The sale must be highly probable and the asset available for immediate sale in its present condition.
Following reclassification, the assets are measured at the lower of their existing carrying amount and their ‘fair value less costs to sell’. Depreciation ceases to be charged. Assets are de-recognised when all material sale contract conditions have been met.
Property, plant and equipment which is to be scrapped or demolished does not qualify for recognition as ‘held for sale’ and instead is retained as an operational asset and the asset’s useful life is adjusted. The asset is de-recognised when scrapping or demolition occurs.
Donated and grant funded assets
Donated and grant funded property, plant and equipment assets are capitalised at their fair value on receipt. The donation or grant is credited to income at the same time, unless the donor has imposed a condition that the future economic benefits embodied in the grant are to be consumed in a manner specified by the donor, in which case, the donation or grant is deferred within liabilities and is carried forward to future financial years to the extent that the condition has not yet been met.
The donated and grant funded assets are subsequently accounted for in the same manner as other items of property, plant and equipment.
Private finance initiative
Private Finance Initiative (PFI) and Local Improvement Finance trusts (LIFT) transactions which meet the IFRIC 12 definition of a service concession, as interpreted in HM Treasury’s FReM, are accounted for as ‘on-Statement of Financial Position’ by the trust. Annual contract payments to the operator (the unitary charge) are apportioned between the repayment of the liability including the finance cost, the charges for services and lifecycle replacement of components of the asset.
Initial recognition
In accordance with HM Treasury’s FReM, the underlying assets are recognised as property, plant and equipment, together with an equivalent liability. Initial measurement of the asset and liability are in accordance with the initial measurement principles of IFRS 16 (see leases accounting policy 1.14).
Subsequent measurement
Assets are subsequently accounted for as property, plant and equipment and, or intangible assets as appropriate.
The liability is subsequently reduced by the portion of the unitary charge allocated as payment for the asset and increased by the annual finance cost. The finance cost is calculated by applying the implicit interest rate to the opening liability and is charged to finance costs in the Statement of Comprehensive Income. The element of the unitary charge allocated as payment for the asset is split between payment of the finance cost and repayment of the net liability.
Where there are changes in future payments for the asset resulting from indexation of the unitary charge, the trust remeasures the Private Finance Initiative liability by determining the revised payments for the remainder of the contract once the change in cash flows takes effect. The remeasurement adjustment is charged to finance costs in the Statement of Comprehensive Income.
The service charge is recognised in operating expenses in the Statement of Comprehensive Income.
Initial application of International Financial Reporting Standards 16 liability measurement principles to private finance initiative and Local Improvement Finance trust liabilities in 2023 and 2024
International Financial Reporting Standards 16 liability measurement principles were applied to private finance initiative (PFI), Local Improvement Finance trusts and other service concession arrangement liabilities in these financial statements from 1 April 2023. The change in measurement basis was applied using a modified retrospective approach with the cumulative impact of remeasuring the liability on 1 April 2023 recognised in the income and expenditure reserve.
Useful lives of property, plant and equipment
Useful economic lives reflect the total life of an asset and not the remaining life of an asset. The range of useful economic lives is set out in note 16.3 of the accounts.
Note 1.9 intangible assets
Recognition
Intangible assets are non-monetary assets without physical substance controlled by the trust. They are capable of being sold separately from the rest of the trust’s business or arise from contractual or other legal rights. Intangible assets are recognised only where it is probable that future economic benefits will flow to, or service potential be provided to, the trust and where the cost of the asset can be measured reliably.
Software
Software which is integral to the operation of hardware, for example, an operating system, is capitalised as part of the relevant item of property, plant and equipment. Software which is not integral to the operation of hardware, for example, application software, is capitalised as an intangible asset where it meets recognition criteria.
Management
Intangible assets are recognised initially at cost, comprising all directly attributable costs needed to create, produce and prepare the asset to the point that it can operate in the manner intended by management.
Subsequently intangible assets are measured at current value in existing use. Where no active market exists, intangible assets are valued at the lower of depreciated replacement cost and the value in use where the asset is income generating. Revaluations gains and losses and impairments are treated in the same manner as for property, plant and equipment. An intangible asset which is surplus with no plan to bring it back into use is valued at fair value where there are no restrictions on sale at the reporting date and where they do not meet the definitions of investment properties or assets held for sale.
Intangible assets held for sale are measured at the lower of their carrying amount or fair value less costs to sell.
Amortisation
Intangible assets are amortised over their expected useful lives, on a straight line basis, in a manner consistent with the consumption of economic or service delivery benefits.
Useful economic lives of intangible assets
Useful economic lives reflect the total life of an asset and not the remaining life of an asset. The range of useful economic lives is set out in note 15.1 of the accounts.
Note 1.10 inventories
All of the trust’s inventories are in respect of consumables. Inventories are valued at the lower of cost and net realisable value. The cost of inventories is measured using the first in, first out (FIFO) method.
Between 2020 and 2021 and 2023 and 2024 the trust received inventories including personal protective equipment from the Department of Health and Social Care at nil cost. In line with the GAM and applying the principles of the IFRS Conceptual Framework, the trust has accounted for the receipt of these inventories at a deemed cost, reflecting the best available approximation of an imputed market value for the transaction based on the cost of acquisition by the Department. Distribution of inventories by the Department ceased in March 2024.
Note 1.11 investment properties
Investment properties are measured at fair value. Changes in fair value are recognised as gains or losses in income or expenditure.
Only those assets which are held solely to generate a commercial return are considered to be investment properties. Where an asset is held, in part, for support service delivery objectives, then it is considered to be an item of property, plant and equipment. Properties occupied by employees, whether they pay rent at market rates, are not classified as investment properties.
Note 1.12 cash and cash equivalents
Cash is cash in hand and deposits held with established financial institutions claimable without penalty on notice of not more than 24 hours. Cash equivalents are investments that mature in 3 months or less from the date of establishment and that are readily convertible to cash with insignificant risk of change in face value.
Note 1.13 financial assets and financial liabilities
Recognition
Financial assets and financial liabilities arise where the trust is party to the contractual provisions of a financial instrument, and as a result has a legal right to receive or a legal obligation to pay cash or present other financial instruments in settlement. The GAM expands the definition of a contract to include legislation and regulations which give rise to arrangements that, in all other respects, would be a financial instrument and do not give rise to transactions classified as a tax by the Office of National Statistics (ONS).
This includes the purchase or sale of non-financial items (such as goods or services), which are entered into in accordance with the trust’s normal purchase, sale or usage requirements and are recognised when, and to the extent which, performance occurs, for example, when receipt or delivery of the goods or services is made.
Classification and measurement
Financial assets and financial liabilities are initially measured at fair value plus or minus directly attributable transaction costs except where the asset or liability is not measured at fair value through income and expenditure. Fair value is taken as the transaction price, or otherwise determined by reference to quoted market prices or valuation techniques.
Financial assets are classified as subsequently measured at amortised cost or fair value through other comprehensive income.
Financial liabilities are classified as subsequently measured at amortised cost.
Financial assets and financial liabilities at amortised cost
Financial assets and financial liabilities at amortised cost are those held with the objective of collecting contractual cash flows and where cash flows are solely payments of principal and interest. This includes cash equivalents, contract and other receivables, trade and other payables, rights and obligations under lease arrangements and loans receivable and payable.
After initial recognition, these financial assets and financial liabilities are measured at amortised cost using the effective interest method less any impairment (for financial assets). The effective interest rate is the rate that exactly discounts estimated future cash payments or receipts through the expected life of the financial asset or financial liability to the gross carrying amount of a financial asset or to the amortised cost of a financial liability.
Interest revenue or expense is calculated by applying the effective interest rate to the gross carrying amount of a financial asset or amortised cost of a financial liability and recognised in the Statement of Comprehensive Income and a financing income or expense. In the case of loans held from the Department of Health and Social Care, the effective interest rate is the nominal rate of interest charged on the loan.
Financial assets measured at fair value through other comprehensive income
A financial asset is measured at fair value through other comprehensive income where business model objectives are met by both collecting contractual cash flows and selling financial assets and where the cash flows are solely payments of principal and interest. Movements in the fair value of financial assets in this category are recognised as gains or losses in other comprehensive income except for impairment losses. On derecognition, cumulative gains and losses previously recognised in other comprehensive income are reclassified from equity to income and expenditure, except where the trust elected to measure an equity instrument in this category on initial recognition.
Impairment of financial assets
The trust’s financial assets which are measured at amortised cost, are in respect of contract and other receivables. At the Statement of Financial Position date, the trust assesses whether any receivables are impaired. Financial receivables are impaired and credit losses recognised if, and only if, there is objective evidence of impairment because of one or more events which occurred after the initial recognition of the asset and which has an impact on future cash flows of the asset.
For financial assets measured at amortised cost, the amount of the impairment loss is measured as the difference between the asset’s carrying value and the expected future cash flow from the asset.
The trust assess potential credit loss on an ongoing basis and makes provision based on actual credit loss. A review of historic credit loss provides evidence that such losses are not material and therefore the trust does not make provision for expected general credit loss.
Expected losses are charged to operating expenditure within the Statement of Comprehensive Income and reduce the net carrying value of the financial asset in the Statement of Financial Position.
Derecognition
Financial assets are de-recognised when the contractual rights to receive cash flows from the assets have expired or the trust has transferred substantially all the risks and rewards of ownership.
Financial liabilities are de-recognised when the obligation is discharged, cancelled or expires.
Note 1.14 leases
A lease is a contract or part of a contract that conveys the right to use an asset for a period of time in exchange for consideration. An adaptation of the relevant accounting standard by HM Treasury for the public sector means that for NHS bodies, this includes lease-like arrangements with other public sector entities that do not take the legal form of a contract. It also includes peppercorn leases where consideration paid is nil or nominal (significantly below market value) but in all other respects meet the definition of a lease.
The trust does not apply lease accounting to new contracts for the use of intangible assets. The trust determines the term of the lease term with reference to the non-cancellable period and any options to extend or terminate the lease which the trust is reasonably certain to exercise.
The trust as a lessee: initial recognition and measurement
At the commencement date of the lease, being when the asset is made available for use, the trust recognises a right of use asset and a lease liability.
The right of use asset is recognised at cost comprising the lease liability, any lease payments made before or at commencement, any direct costs incurred by the lessee, less any cash lease incentives received. It also includes any estimate of costs to be incurred restoring the site or underlying asset on completion of the lease term.
The lease liability is initially measured at the present value of future lease payments discounted at the interest rate implicit in the lease. Lease payments includes fixed lease payments, variable lease payments dependent on an index or rate and amounts payable under residual value guarantees. It also includes amounts payable for purchase options and termination penalties where these options are reasonably certain to be exercised.
Where an implicit rate cannot be readily determined, the trust’s incremental borrowing rate is applied. This rate is determined by HM Treasury annually for each calendar year. A nominal rate of 4.72% applied to new leases commencing in 2024 and 4.81% to new leases commencing in 2025.
The trust does not apply the above recognition requirements to leases with a term of 12 months or less or to leases where the value of the underlying asset is below £5,000, excluding any irrecoverable VAT. Lease payments associated with these leases are expensed on a straight line basis over the lease term or other systematic basis. Irrecoverable VAT on lease payments is expensed as it falls due.
The trust as a lessee: subsequent measurement
As required by a HM Treasury interpretation of the accounting standard for the public sector, the trust employs a revaluation model for subsequent measurement of right of use assets, unless the cost model is considered to be an appropriate proxy for current value in existing use or fair value, in line with the accounting policy for owned assets. Where consideration exchanged is identified as significantly below market value, the cost model is not considered to be an appropriate proxy for the value of the right of use asset.
The trust subsequently measures the lease liability by increasing the carrying amount for interest arising which is also charged to expenditure as a finance cost and reducing the carrying amount for lease payments made. The liability is also remeasured for changes in assessments impacting the lease term, lease modifications or to reflect actual changes in lease payments. Such remeasurements are also reflected in the cost of the right of use asset. Where there is a change in the lease term or option to purchase the underlying asset, an updated discount rate is applied to the remaining lease payments.
The trust as lessor
The trust assesses each of its leases and classifies them as either a finance lease or an operating lease. Leases are classified as finance leases when substantially all the risks and rewards of ownership are transferred to the lessee. All other leases are classified as operating leases. Where the trust is an intermediate lessor, classification of the sublease is determined with reference to the right of use asset arising from the headlease.
The trust as lessor: finance leases
Amounts due from lessees under finance leases are recorded as receivables at the amount of the trust’s net investment in the leases. Finance lease income is allocated to accounting periods to reflect a constant periodic rate of return on the trust’s net investment outstanding in respect of the leases.
The trust as lessor: operating leases
Income from operating leases is recognised on a straight-line basis or another systematic basis over the term of the lease. Initial direct costs incurred in negotiating and arranging an operating lease are added to the carrying amount of the leased asset and recognised as an expense on a straight-line basis over the lease term.
Note 1.18 provisions
The trust recognises a provision where it has a present legal or constructive obligation of uncertain timing or amount; for which it is probable that there will be a future outflow of cash or other resources; and a reliable estimate can be made of the amount. The amount recognised in the Statement of Financial Position is the best estimate of the resources required to settle the obligation.
Where the effect of the time value of money is significant, the estimated risk-adjusted cash flows are discounted using HM Treasury’s discount rates effective from 31 March 2025:
| Provision | Length | Nominal rate | Prior year rate |
|---|---|---|---|
| Short-term | Up to 5 years | 4.03% | 4.26% |
| Medium-term | After 5 years up to 10 years | 4.07% | 4.03% |
| Long-term | Exceeding 10 years | 4.81% | 4.72% |
| Very long-term | Exceeding 40 Years | 4.55% | 4.40% |
HM Treasury provides discount rates for general provisions on a nominal rate basis. Expected future cash flows are adjusted for the impact of inflation before discounting using nominal rates. The following inflation rates are set by HM Treasury, effective from 31 March 2025:
| Year | Inflation rate | Prior year rate |
|---|---|---|
| Year 1 | 2.6% | 3.6% |
| Year 2 | 2.3% | 1.80% |
| Into perpetuity | 2% | 2% |
Clinical negligence costs
NHS Resolution operates a risk pooling scheme for which the trust pays an annual contribution. NHS Resolution in turn settles all clinical negligence claims. Although NHS Resolution is administratively responsible for all clinical negligence cases, the legal liability remains with the trust. The total value of clinical negligence provisions carried by NHS Resolution on behalf of the trust is disclosed on note 29.1 but is not recognised in the trust’s accounts.
Non-clinical risk pooling
The trust participates in the Property Expenses Scheme and the Liabilities to Third Parties Scheme. Both are risk pooling schemes under which the trust pays an annual contribution to NHS Resolution and in return receives assistance with the costs of claims arising. The annual membership contributions, and any excesses payable in respect of these claims, are charged to operating expenditure when liability arises.
Note 1.17 contingencies
Contingent assets (that is, assets arising from past events whose existence will only be confirmed by one or more future events not wholly within the trust’s control) are not recognised as assets, but are disclosed on note 30 where an inflow of economic benefits is probable. Contingent liabilities are not recognised, but are disclosed in note 30, unless the probability of a transfer of economic benefits is remote.
Contingent liabilities are defined as:
- possible obligations arising from past events whose existence will be confirmed only by the occurrence of one or more uncertain future events not wholly within the entity’s control; or
- present obligations arising from past events but for which it is not probable that a transfer of economic benefits will arise or for which the amount of the obligation cannot be measured with sufficient reliability
Note 1.18 public dividend capital
Public dividend capital (PDC) is public sector equity finance based on the excess of assets over liabilities at the time of establishment of the predecessor NHS organisation. HM Treasury has determined that PDC is not a financial instrument within the meaning of IAS 32.
The Secretary of State can issue new PDC to, and require repayments of PDC from, the trust. PDC is recorded at the value received.
A charge, reflecting the cost of capital utilised by the trust, is payable as public dividend capital dividend. The charge is calculated at the rate set by HM Treasury (currently 3.5%) on the average relevant net assets of the trust during the financial year. Relevant net assets are calculated as the value of all assets less the value of all liabilities, with certain additions and deductions as defined by the Department of Health and Social Care.
This policy is available at guidance on financing available to NHS trusts and foundation trusts.
In accordance with the requirements laid down by the Department of Health and Social Care (as the issuer of PDC), the dividend for the year is calculated on the actual average relevant net assets as set out in the pre-audit version of the annual accounts. The dividend calculated is not revised should any adjustment to net assets occur as a result the audit of the annual accounts.
Note 1.19 value added tax
Most of the activities of the trust are outside the scope of VAT. In general, output tax does not apply and input tax on purchases is not recoverable. Irrecoverable VAT is charged to the relevant expenditure category or included in the capitalised purchase cost of fixed assets. Where output tax is charged or input VAT is recoverable, the amounts are stated net of VAT.
Note 1.20 corporation tax
All activities of the trust are exempt from corporation tax. Flourish, the subsidiary of the trust, is subject to corporation tax at the rate of 19% (2034 and 2024:19%). The Corporate tax rates changes with government budgets.
Note 1.21 foreign exchange
The functional and presentational currency of the trust is sterling. A transaction which is denominated in a foreign currency is translated into the functional currency at the spot exchange rate on the date of the transaction. The trust has very few foreign currency transactions.
Note 1.22 third party assets
Assets belonging to third parties in which the trust has no beneficial interest (such as money held on behalf of patients) are not recognised in the accounts. However, they are disclosed on a separate note to the accounts in accordance with the requirements of HM Treasury’s FReM.
Note 1.23 losses and special payments
Losses and special payments are items that Parliament would not have contemplated when it agreed funds for the health service or passed legislation. By their nature they are items that arise outside the expected norms of operating services. They are therefore subject to special control procedures compared with the generality of payments. They are divided into different categories, which govern the way that individual cases are handled.
Losses and special payments are charged to the relevant functional headings in expenditure on an accrual basis. Losses and special payments note is compiled directly from the losses and compensations register which reports on an accrual basis except where they are provisions for future known losses.
Note 1.24 gifts
Gifts are items that are voluntarily donated without preconditions and expectations of any returns. Gifts include all transactions economically equivalent to free and unremunerated transfers, such as the loan of an asset for its expected useful life, and the sale or lease of assets at below market value.
The trust received no gifts in this or the previous reporting period.
Note 1.25 early adoption of standards, amendments, and interpretations
No new accounting standards or revisions to existing standards have been early adopted in 2024 and 2025.
Note 1.26 standards, amendments and interpretations in issue but not yet effective or adopted
The Department of Health and Social Care GAM does not require the following IFRS Standards to be applied in 2024 and 2025:
- IFRS 17 Insurance Contracts: the standard is effective for accounting periods beginning on or after 1 January 2023. IFRS 17 has been adopted by the FReM from 1 April 2025. Adoption of the Standard for NHS bodies will therefore be in 2025 and 2026. The Standard revises the accounting for insurance contracts for the issuers of insurance. Application of this standard from 2025 and 2026 is not expected to have a material impact on the financial statements.
- IFRS 18 Presentation and Disclosure in Financial Statements: the Standard is effective for accounting periods beginning on or after 1 January 2027. The Standard is not yet UK endorsed and not yet adopted by the FReM. Early adoption is not permitted. The expected impact of applying the standard in future periods has not yet been assessed.
- IFRS 19 Subsidiaries without Public Accountability: disclosures, the Standard is effective for accounting periods beginning on or after 1 January 2027. The Standard is not yet UK endorsed and not yet adopted by the FReM. Early adoption is not permitted. The expected impact of applying the standard in future periods has not yet been assessed.
- Changes to non-investment asset valuation – Following a thematic review of non-current asset valuations for financial reporting in the public sector, HM Treasury has made a number of changes to valuation frequency, valuation methodology and classification which are effective in the public sector from 1 April 2025 with a 5 year transition period. NHS bodies are adopting these changes to an alternative timeline.
- Changes to subsequent measurement of intangible assets and PPE classification or terminology to be implemented for NHS bodies from 1 April 2025:
- withdrawal of the revaluation model for intangible assets. Carrying values of existing intangible assets measured under a previous revaluation will be taken forward as deemed historic cost
- removal of the distinction between specialised and non-specialised assets held for their service potential. Assets will be classified according to whether they are held for their operational capacity
- Changes to valuation cycles and methodology to be implemented for NHS bodies in later periods:
- a mandated quinquennial revaluation frequency (or rolling programme) supplemented by annual indexation in the intervening years
- removal of the alternative site assumption for buildings valued at depreciated replacement cost on a modern equivalent asset basis. The approach for land has not yet been finalised by HM Treasury
The impact of applying these changes in future periods has not yet been assessed.
Note 1.27 critical judgements in applying accounting policies
The following are the judgements, apart from those involving estimations (see below) that management has made in the process of applying the trust accounting policies and that have the most significant impact on the amounts recognised in the financial statements:
Valuation of buildings
The Department of Health and Social Care (DHSC) guidance specifies that the trust’s land and buildings should be valued on the basis of depreciated replacement cost, applying the Modern Equivalent Asset (MEA) concept. The MEA is defined as ‘the cost of a modern replacement asset that has the same productive capacity as the property being valued’. Therefore the MEA is not a valuation of the existing land and buildings that the trust holds but a theoretical calculation for accounting purposes of what the trust could need to spend in order to replace the current assets. The trust does this on an alternative site basis.
In determining the MEA the trust developed Modern Equivalent Asset Value (MEAV) designs of an alternative site, and these have been reviewed and approved by its appointed Valuer (the Valuation Office Agency). The trust is satisfied that the assumptions underpinning the MEA valuation are practically achievable, and would meet the service levels currently offered with no impact on service delivery or the level and volume of service provided. The trust has no plans to implement any of the theoretical assumptions that underpin the MEA valuation.
The valuation of the trust’s land and buildings is done on a quinquennial (5-year) cycle, as per the Government Financial Reporting Manual (the FReM) adaptation of IAS 16 Property Plant and Equipment. This is supplemented by indexation and, or desktop revaluations in intervening years.
The last full revaluation of the trust’s land and buildings was done in 2023 and 2024, with a desktop valuation having been carried out in 2024 and 2025. The next full revaluation is due to be completed in 2028 and 2029, per the FReM requirements.
In applying critical judgements, the trust has satisfied itself that there is no material difference caused by performing a desktop revaluation in 2024 and 2025 as compared with a full revaluation by confirming that there are no material changes to service delivery so the alternative site is still fit for purpose; and by disclosure of all capital expenditure on trust buildings to the trust’s valuer for including in the desktop calculation and by disclosure of any significant dilapidations of buildings to the trust’s valuer for including in the desktop calculation. There were no significant dilapidations of buildings during 2024 and 2025.
Note 1.28 sources of estimation uncertainty
The following are assumptions about the future and other major sources of estimation uncertainty that have a significant risk of resulting in a material adjustment to the carrying amounts of assets and liabilities within the next financial year:
- Property valuation and asset lives: Property valuations are undertaken by an independent external valuer. These values are subject to market conditions and market values. Asset lives are also estimated by the external valuer and are subject to their professional judgement.
- Accruals: Estimates of accruals are based on the best available information. This is applied in conjunction with historic experience and individual circumstance.
- Provisions: Provisions have been calculated after recognising obligating events during the year and include estimates and assumptions relating to the carrying amounts and timing of anticipated payments. Litigation provisions are based on estimates provided through NHS Resolution and injury benefit provisions calculated on figures from NHS Business Services Authority. Refer to Paragraph 1.15 for further details.
- Local government pension scheme: Estimation of the net liability of the local government pension fund depends on several complex judgements relating to the discount rate used, the rate at which salaries are projected to increase, changes in retirement ages, mortality rates and the expected return on pension fund assets. Hymans Robertson LLP is engaged through South Yorkshire Pension Fund to provide the trust with expert advice on the assumptions used.
Note 2 operating segments
Most of the activity of the Rotherham Doncaster and South Humber NHS Foundation Trust is healthcare. The Board of Directors is considered to be the chief operating decision maker (CODM); management information provided to the CODM reports activities as a whole and not segmentally.
Note 3 operating income from patient care activities (Group)
All income from patient care activities relates to contract income recognised in line with accounting policy 1.4.
Note 3.1 income from patient care activities (by nature)
| Service | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Mental health services: income from commissioners under API contracts | 143,359 | 128,960 |
| Mental health services: income for commissioning services in a mental health collaborative | 4,168 | 4,370 |
| Mental health services: services delivered under a mental health collaborative | 2,416 | |
| Mental health services: other clinical income from mandatory services | 1,806 | 4,627 |
| Community services: income from commissioners under API contracts | 50,531 | 47,524 |
| Community services: income from other sources (for example, local authorities) | 21,837 | 19,939 |
| All services: national pay award central funding | 20 | 38 |
| All services: additional pension contribution central funding | 11,569 | 7,063 |
| Total income from activities | 235,706 | 212,521 |
Aligned payment and incentive contracts are the main form of contracting between NHS providers and their commissioners. More information can be found in the 2023 and 2025 NHS Payment Scheme documentation.
Comparative income was included within “other clinical income from mandatory services” in 2023 and 2024.
Additional funding was made available directly to providers by NHS England in 2024 and 2025 and 2023 and 2024 for implementing the backdated element of pay awards where government offers were finalised after the end of the financial year. NHS Payment Scheme prices and API contracts are updated for the weighted uplift in in-year pay costs when awards are finalised.
Increases to the employer contribution rate for NHS pensions since 1 April 2019 have been funded by NHS England. NHS providers continue to pay at the former rate of 14.3% with the additional amount being paid over by NHS England on providers’ behalf. The full cost of employer contributions (23.7%, 2023 and 2024: 20.6%) and related NHS England funding (9.4%, 2023 and 2024: 6.3%) have been recognised in these accounts.
Note 3.2 income from patient care activities (by source)
| Income from patient care activities received from | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| NHS England | 18,128 | 12,050 |
| Department of Health and Social Care | 257 | |
| Integrated care boards | 191,116 | 175,546 |
| Other NHS providers | 4,222 | 4,627 |
| Local authorities | 21,837 | 19,939 |
| Non NHS: other | 146 | 359 |
| Total income from activities | 235,706 | 212,521 |
Note 4 other operating income (group)
| Operating income group | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Research and development | 1,413 | 757 |
| Education and training (excluding notional apprenticeship levy income) | 6,674 | 6,493 |
| Non-patient care services to other bodies | 1,709 | 1,483 |
| Income in respect of employee benefits accounted on a gross basis | 1,220 | 1,529 |
| Education and training – notional income from the apprenticeship fund | 550 | 577 |
| Peppercorn leased assets recognised | 44 | 192 |
| Cash donations for the purchase of capital assets received from NHS charities | 25 | |
| Contributions to expenditure – consumables (inventory)donated from The Department of Health and Social Care group bodies for COVID response | 19 | |
| Rental revenue from operating leases | 593 | 587 |
| Charitable fund incoming resources | 317 | 218 |
| Other contract income | 852 | 858 |
| Total other operating income | 13,372 | 12,738 |
Note 5
Note 5.1 transaction price allocated to remaining performance obligations
| Revenue | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Revenue recognised in the reporting period that was included in contract liabilities at the previous period end | 187 |
This disclosure was not made in 2023 and 2024 accounts.
Note 5.2 income from activities arising from commissioner requested services
Under the terms of its provider licence, the trust is required to analyse the level of income from activities that has arisen from commissioner requested and non-commissioner requested services. Commissioner requested services are defined in the provider licence and are services that commissioners believe would need to be protected in the event of provider failure. This information is provided in the table below:
| Income source | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Income from services designated as commissioner requested services | 214,809 | 192,582 |
| Income from services not designated as commissioner requested services | 34,269 | 32,677 |
| Total | 249,078 | 225,259 |
The income from activities arising from commissioner requested services is in respect of the consolidated income of the trust and Flourish and excludes charitable fund income of £385,000 (2023 and 2024: £237,000).
Note 5.3 profits and losses on disposal of property, plant and equipment
There was one sale of property, plant or equipment in 2024 and 2025 (2023 and 2024. Nil). This asset was not used in the provision of commissioner requested services.
The sale was for a tractor for £9,000 which had an accumulated cost and accumulated depreciation of £28,000, accordingly the profit on sale was £9,000 as further disclosed in note 13.
Note 6 operating expenses (group)
| Expense | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Purchase of healthcare from NHS and the Department of Health and Social Care group bodies | 20 | 13 |
| Purchase of healthcare from non-NHS and non-Department of Health and Social Care bodies | 5,136 | 5,789 |
| Mental health collaboratives (lead provider) purchase of healthcare – from NHS bodies | 64 | 61 |
| Mental health collaboratives (lead provider) purchase of healthcare – from non-NHS bodies | 4,330 | 4,276 |
| Staff and executive directors costs | 195,906 | 180,498 |
| Remuneration of non-executive directors | 173 | 154 |
| Supplies and services – clinical (excluding drugs costs) | 6,378 | 6,363 |
| Supplies and services – general | 2,349 | 2,319 |
| Drug costs (drugs inventory consumed and purchase of non-inventory drugs) | 3,610 | 3,170 |
| Consultancy costs | 250 | |
| Establishment | 2,390 | 2,299 |
| Premises – business rates paid to local authorities | 820 | 665 |
| Premises – other | 7,696 | 7,017 |
| Transport (including patient travel) | 2,920 | 2,896 |
| Depreciation on property, plant and equipment and right of use assets | 6,024 | 5,548 |
| Amortisation on intangible assets | 529 | 574 |
| Net impairments | (41) | (1,451) |
| Movement in credit loss allowance: contract receivables or contract assets | 33 | 7 |
| Change in provisions discount rates | 1 | (60) |
| Audit fees payable to the external auditor | 277 | 338 |
| Internal audit costs | 125 | 116 |
| Clinical negligence | 754 | 765 |
| Legal fees | 627 | 279 |
| Insurance | 215 | 210 |
| Research and development staff costs (comparative figures for 2023 and 2024 were disclosed in “staff and executive directors costs”. A reallocation for 2023 and 2024 and 2024 and 2025 has been performed for these cost categories as per the classification requirements) | 1,466 | |
| Research and development non staff 14 26 Education and training staff costs (comparative figures for 2023 and 2024 were disclosed in “staff and executive directors costs”. A reallocation for 2023 and 2024 and 2024 and 2025 has been performed for these cost categories as per the classification requirements) | 1,786 | |
| Education and training non staff | 1,525 | 1,044 |
| Expenditure on short term leases | 493 | 91 |
| Education and training – notional expenditure funded from the apprenticeship fund | 550 | 577 |
| Redundancy | 206 | 74 |
| Car parking and security | 128 | 251 |
| Losses, ex gratia and special payments | 6 | 64 |
| Other NHS charitable fund resources expended | 888 | 962 |
| Other | 480 | 977 |
| Total | 247,878 | 226,162 |
| Expense | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Contracted fee | 221 | 210 |
| Additional fees in relation to 2022 and 2023 paid in 2023 and 2024 | 0 | 119 |
| Additional fees in relation to 2023 and 2024 paid in 2024 and 2025 | 47 | 0 |
| Flourish statutory audit undertaken by GBAC | 9 | |
| Total | 277 | 329 |
Note 6.1 limitation on auditor’s liability (group)
The limitation on the auditor’s liability for external audit work is £1,000,000 (2023 and 2024: £1,000,000).
Note 7 impairment of assets (group)
| Net impairments charged to operating surplus or deficit resulting from | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Changes in market price | (41) | (1,451) |
| Total net impairments charged to operating surplus or deficit | (41) | (1,451) |
| Impairments charged to the revaluation reserve | 1,640 | 4,959 |
| Total net impairments | 1,599 | 3,508 |
As at 31 March 2025 land and buildings were valued using an alternative site methodology. This resulted in a net reversal of impairment to operating expenses of £41,000 (2023 and 2024: £1,451,000) and a net impairment to the revaluation reserve of £1,640,000 (2023 and 2024 £4,959,000).
Note 8 employee benefits (group)
| Costs | Total 2024 and 2025 (£000) | Total 2023 and 2024 (£000) |
|---|---|---|
| Staff and executive directors costs | 149,480 | 135,331 |
| Non – executive directors | 173 | 154 |
| Social security costs | 14,238 | 13,782 |
| Apprenticeship levy | 697 | 668 |
| Employer’s contributions to NHS pensions | 17,814 | 16,152 |
| Pension cost – employer contributions paid by NHSE on provider’s behalf | 11,569 | 7,063 |
| Pension cost – other | 90 | 97 |
| Temporary staff – external bank | 2,719 | |
| Temporary staff (agency) | 2,956 | 7,555 |
| Total gross staff costs | 199,736 | 180,802 |
| Included within costs capitalised as part of assets | 199 | 75 |
| Total employee benefits excluding capitalised costs | 199,537 | 180,727 |
| Operating expenditure analysed as: employee expenses, staff and executive directors | 196,079 | 180,652 |
| Research and development | 1,466 | |
| Education and training | 1,786 | |
| Termination benefits – redundancy | 206 | 74 |
| Total | 199,537 | 180,727 |
Trust operated an internal bank until 20 October 2024 for which these costs were disclosed in ‘staff and executive directors costs’. From 21 October 2024 the trust moved to an external bank, hence no comparative information for 2023 and 2024.
Comparative figures for 2023 and 2024 were disclosed in ‘Staff and executive directors costs’. A reallocation for 2023 and 2024 and 2024 and 2025 has been performed for these cost categories as per the classification requirements.
Note 8.1 retirements due to ill-health (group)
During 2024 and 2025 there were 2 early retirements from the trust agreed on the grounds of ill-health (8 in the year ended 31 March 2024). The estimated additional pension liabilities of these ill-health retirements is £427,000 (£255,000 in 2023 and 2024).
Note 9 pension costs
Past and present employees are covered by the provisions of the NHS Pension Schemes. Details of the benefits payable and rules of the schemes can be found on the NHS Pensions website. Both the 1995 and 2008 and 2015 schemes are accounted for, and the scheme liability valued, as a single combined scheme. Both are unfunded defined benefit schemes that cover NHS employers, GP practices and other bodies, allowed under the direction of the Secretary of State for Health and Social Care in England and Wales. They are not designed to be run in a way that would enable NHS bodies to identify their share of the underlying scheme assets and liabilities. Therefore, each scheme is accounted for as if it were a defined contribution scheme: the cost to the NHS body of participating in each scheme is taken as equal to the contributions payable to that scheme for the accounting period.
In order that the defined benefit obligations recognised in the financial statements do not differ materially from those that would be determined at the reporting date by a formal actuarial valuation, the FReM requires that “the period between formal valuations shall be four years, with approximate assessments in intervening years”. An outline of these follows:
Accounting valuation
A valuation of scheme liability is carried out annually by the scheme actuary (currently the Government Actuary’s Department) as at the end of the reporting period. This utilises an actuarial assessment for the previous accounting period in conjunction with updated membership and financial data for the current reporting period, and is accepted as providing suitably robust figures for financial reporting purposes. The valuation of the scheme liability as at 31 March 2025, is based on valuation data as 31 March 2023, updated to 31 March 2025 with summary global member and accounting data. In undertaking this actuarial assessment, the methodology prescribed in IAS 19, relevant FReM interpretations, and the discount rate prescribed by HM Treasury have also been used.
The latest assessment of the liabilities of the scheme is contained in the Statement by the Actuary, which forms part of the annual NHS Pension Scheme Annual Report and Accounts. These accounts can be viewed on the NHS Pensions website and are published annually. Copies can also be obtained from The Stationery Office.
Full actuarial (funding) valuation
The purpose of this valuation is to assess the level of liability in respect of the benefits due under the schemes (considering recent demographic experience), and to recommend the contribution rate payable by employers.
The latest actuarial valuation undertaken for the NHS Pension Scheme was completed as at 31 March 2020. The results of this valuation set the employer contribution rate payable from 1 April 2024 to 23.7% of pensionable pay. The core cost cap cost of the scheme was calculated to be outside of the 3% cost cap corridor as at 31 March 2020. However, when the wider economic situation was taken into account through the economic cost cap cost of the scheme, the cost cap corridor was not similarly breached. As a result, there was no impact on the member benefit structure or contribution rates.
The 2024 actuarial valuation is currently being prepared and will be published before new contribution rates are implemented from April 2027.
Local government pension scheme
Some employees are members of the Local Government scheme, which is a defined benefit scheme. The scheme assets and liabilities attributable to these employees can be identified and are recognised in the trust’s financial statements. The assets are measured at fair value and the liabilities at the present value of future obligations.
The increase in the liability arising from pensionable service earned during the year is recognised within operating expenses. The net interest cost during the year arising from the unwinding of the discount on the net scheme liabilities is recognised within finance costs. Remeasurements of the defined benefit plan is recognised in the income and expenditure reserve and reported in the Statement of Comprehensive Income as an item of ‘other comprehensive income’.
National Employment Savings Trust (NEST) pension scheme
Some employees are members of the NEST pension scheme, a scheme set up by Government to enable employers to meet their pension duties and is free for employers to use. Employee and employer contribution rates were a combined minimum of 5% (with a minimum of 2.1% contributed by the trust) up to October 2018; from 2018 the combined contribution is 8% (with a minimum of 3% contributed by the trust). Employer contributions in 2024 and 2025 were £90,000 (2023 and 2024: £97,000).
Note 10 operating leases (group)
This note discloses income generated in operating lease agreements where Rotherham Doncaster and South Humber NHS Foundation Trust is the lessor.
Note 10.1 operating leases income (group) 2024
| Operating leases income | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Minimum lease receipts | 593 | 587 |
| Total | 593 | 587 |
Note 10.2 future lease receipts (group)
| Future lease receipts | 31 March 2025 (£000) | 31 March 2024 (£000) |
|---|---|---|
| Future minimum lease receipts due in: – not later than one year | 615 | 899 |
| Total | 615 | 899 |
Note 11 finance income (group)
Finance income represents interest received on assets and investments in the period.
| Income | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Interest on bank accounts | 1,786 | 2,072 |
| NHS charitable fund investment income | 68 | 85 |
| Other finance income | 19 | |
| Total finance income | 1,873 | 2,157 |
Note 12 finance expenditure (group)
Finance expenditure represents interest and other charges involved in the borrowing of money.
| Expenditure | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Interest expense: Loans from the Department of Health and Social Care | 143 | 155 |
| Interest on lease obligations | 148 | 144 |
| Main finance costs on Private Finance Initiatives and Local Improvement Finance Trust schemes obligations | 1,157 | 661 |
| Remeasurement of the liability resulting from change in index or rate | 437 | 559 |
| Total interest expense | 1,885 | 1,519 |
| Unwinding of discount on provisions | 13 | |
| Other finance costs | 83 | |
| Total finance costs | 1,898 | 1,602 |
Note 12.1 The late payment of commercial debts (interest) Act 1998
No payments were made in 2024 and 2025 under the late payment of commercial debts (interest) Act 1998. (2023 and 2024: nil).
Note 13 other gains and losses (group)
| Gains or losses | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Gains on disposal of assets | 9 | |
| Total gains or (losses) on disposal of assets | 9 | |
| Fair value gains on investment properties | 45 | 17 |
| Total other gains or (losses) | 54 | 17 |
Note 14 trust income statement and statement of comprehensive income In accordance with Section 408 of the Companies Act 2006, the trust is exempt from the requirement to present its own income statement and statement of comprehensive income. The trust’s deficit for the period was £527,000 (2023 and 2024: £1,666,000 deficit). The trust’s total comprehensive expense for the period was £1,765,000 deficit (2023 and 2024: £22,000 deficit).
Note 15 intangible assets 2024 and 2025
| Cost | Software licences (£000) | Intangible assets under construction (£000) | Total (£000) |
|---|---|---|---|
| Valuation or gross cost at 1 April 2024 | 5,887 | 5,887 | |
| Additions | 833 | 833 | |
| Reclassifications | 10 | 10 | |
| Disposals or derecognition | (1,806) | (1,806) | |
| Valuation or gross cost at 31 March 2025 | 4,924 | 4,924 | |
| Amortisation at 1 April 2024 | 3,829 | 3,829 | |
| Provided during the year | 529 | 529 | |
| Disposals or derecognition | (1,806) | (1,806) | |
| Amortisation at 31 March 2025 | 2,552 | 2,552 | |
| Net book value at 31 March | 2,372 | 2,372 | |
| Net book value at 1 April 2024 | 2,058 | 2,058 |
Note 15.1 intangible assets 2023 and 2024
| Cost | Software licences (£000) | Intangible assets under construction (£000) | Total (£000) |
|---|---|---|---|
| Valuation or gross cost at 1 April 2023 | 5,616 | 5,616 | |
| Additions | 271 | 271 | |
| Valuation or gross cost at 31 March 2024 | 5,887 | 5,887 | |
| Amortisation at 1 April 2023 | 3,255 | 3,255 | |
| Provided during the year | 574 | 574 | |
| Amortisation at 31 March 2024 | 3,829 | 3,829 | |
| Net book value at 31 March 2024 | 2,058 | 2,058 | |
| Net book value at 1 April 2023 | 2,361 | 2,361 |
Note 15.1 useful economic life of intangible assets
| Intangible asset | Minimum life (years) | Maximum life (years) |
|---|---|---|
| Software licenses | 2 | 10 |
Note 16 property, plant and equipment 2024 and 2025
| Category | Land (£000) | Buildings excluding dwellings (£000) | Dwellings (£000) | Assets under construction (£000) | Plant and machinery (£000) | Transport equipment (£000) | Information technology (£000) | Furniture and fittings (£000) | Total (£000) |
|---|---|---|---|---|---|---|---|---|---|
| Valuation or gross cost at 1 April 2024 | 5,107 | 81,209 | 160 | 10 | 2,344 | 103 | 11,909 | 702 | 101,544 |
| Additions | 4,124 | 555 | 327 | 83 | 2,106 | 7,195 | |||
| Impairments | (364) | (364) | |||||||
| Impairments charged to the revaluation reserve | (1,640) | (1,640) | |||||||
| Reversals of impairments | 405 | 405 | |||||||
| Revaluations | 150 | (2,081) | 30 | (1,901) | |||||
| Reclassifications | (10) | 31 | (31) | (10) | |||||
| Transfers to or from assets held for sale and assets in disposal groups | (35) | (55) | (90) | ||||||
| Disposals or derecognition | (28) | (5,674) | (5,702) | ||||||
| Valuation or gross cost at 31 March 2025 | 5,222 | 81,598 | 190 | 555 | 2,674 | 186 | 8,341 | 671 | 99,437 |
| Accumulated depreciation at 1 April 2024 | 1,217 | 103 | 7,873 | 441 | 9,634 | ||||
| Provided during the year | 3,230 | 9 | 157 | (0) | 1,264 | 39 | 4,699 | ||
| Revaluations | (3,226) | (9) | (3,235) | ||||||
| Transfers to or from assets held for sale and assets in disposal groups | (4) | (4) | |||||||
| Disposals or derecognition | (28) | (5,674) | (5,702) | ||||||
| Accumulated depreciation at 31 March 2025 | 1,346 | 103 | 3,463 | 480 | 5,392 | ||||
| Net book value at 31 March 2025 | 5,222 | 81,598 | 190 | 555 | 1,328 | 83 | 4,878 | 191 | 94,045 |
| Net book value at 1 April 2024 | 5,107 | 81,209 | 160 | 10 | 1,127 | 4,036 | 261 | 91,910 |
Note 16 (continued) property, plant and equipment 2024 and 2025
| Category | Land (£000) | Buildings excluding dwellings (£000) | Dwellings (£000) | Assets under construction (£000) | Plant and machinery (£000) | Transport equipment (£000) | Information technology (£000) | Furniture and fittings (£000) | Total (£000) |
|---|---|---|---|---|---|---|---|---|---|
| Valuation or gross cost at 1 April 2024 | 5,107 | 82,429 | 160 | 10 | 2,344 | 103 | 11,909 | 702 | 102,764 |
| Additions | 4,124 | 555 | 327 | 83 | 2,106 | 7,195 | |||
| Impairments | (364) | (364) | |||||||
| Impairments charged to the revaluation reserve | (1,640) | (1,640) | |||||||
| Reversals of impairments | 405 | 405 | |||||||
| Revaluations | 150 | (2,081) | 30 | (1,901) | |||||
| Reclassifications | (1,220) | (10) | 31 | (31) | (1,230) | ||||
| Transfers to or from assets held for sale and assets in disposal groups | (35) | (55) | (90) | ||||||
| Disposals or derecognition | (28) | (5,674) | (5,702) | ||||||
| Valuation or gross cost at 31 March 2025 | 5,222 | 81,598 | 190 | 555 | 2,674 | 186 | 8,341 | 671 | 99,437 |
| Accumulated depreciation at 1 April 2024 | 1,217 | 103 | 7,873 | 441 | 9,634 | ||||
| Provided during the year | 3,230 | 9 | 157 | (0) | 1,264 | 39 | 4,699 | ||
| Revaluations | (3,226) | (9) | (3,235) | ||||||
| Transfers to or from assets held for sale and assets in disposal groups | (4) | (4) | |||||||
| Disposals or derecognition | (28) | (5,674) | (5,702) | ||||||
| Accumulated depreciation at 31 March 2025 | (0) | 1,346 | 103 | 3,463 | 480 | 5,392 | |||
| Net book value at 31 March 2025 | 5,222 | 81,598 | 190 | 555 | 1,328 | 83 | 4,878 | 191 | 94,045 |
| Net book value at 1 April 2024 | 5,107 | 82,429 | 160 | 10 | 1,127 | 4,036 | 261 | 93,130 |
Note 16.1 property, plant and equipment 2023 and 2024
| Category | Land (£000) | Buildings excluding dwellings (£000) | Dwellings (£000) | Assets under construction (£000) | Plant and machinery (£000) | Transport equipment (£000) | Information technology (£000) | Furniture and fittings (£000) | Total (£000) |
|---|---|---|---|---|---|---|---|---|---|
| Valuation or gross cost at 1 April 2023 | 4,857 | 74,948 | 170 | 3,760 | 2,161 | 103 | 10,775 | 536 | 97,310 |
| Additions | 5,228 | 151 | 1,134 | 166 | 6,679 | ||||
| Additions: assets purchased from cash donations or grants | 25 | 25 | |||||||
| Impairments | (1,293) | (1,293) | |||||||
| Impairments charged to the revaluation reserve | (4,959) | (4,959) | |||||||
| Reversal of impairments | 218 | 2,526 | 2,744 | ||||||
| Revaluations | 32 | 1,029 | (10) | 1,051 | |||||
| Reclassifications | 3,730 | (3,750) | 7 | (13) | |||||
| Valuation or gross cost at 31 March 2024 | 5,10781,209 | 160 | 10 | 2,344 | 103 | 11,909 | 702 | 101,544 | |
| Accumulated depreciation at 1 April 2023 | 3,050 | 10 | 1,074 | 103 | 6,527 | 412 | 11,176 | ||
| Provided during the year | 2,727 | 9 | 143 | 1,346 | 29 | 4,254 | |||
| Revaluations | (5,777) | (19) | (5,796) | ||||||
| Accumulated depreciation at 31 March 2024 | 1,217 | 103 | 7,873 | 441 | 9,634 | ||||
| Net book value at 31 March 2024 | 5,107 | 81,209 | 160 | 10 | 1,127 | 4,036 | 261 | 91,910 | |
| Net book value at 1 April 2023 | 4,857 | 71,898 | 160 | 3,760 | 1,087 | 4,248 | 124 | 86,134 |
| Category | Land (£000) | Buildings excluding dwellings (£000) | Dwellings (£000) | Assets under construction (£000) | Plant and machinery (£000) | Transport equipment (£000) | Information technology (£000) | Furniture and fittings (£000) | Total (£000) |
|---|---|---|---|---|---|---|---|---|---|
| Valuation or gross cost at 1 April 2023 | 4,857 | 76,119 | 170 | 3,760 | 2,161 | 103 | 10,775 | 536 | 98,481 |
| Additions | 5,228 | 151 | 1,134 | 166 | 6,679 | ||||
| Additions: assets purchased from cash donations or grants | 25 | 25 | |||||||
| Impairments | (1,293) | (1,293) | |||||||
| Impairments charged to the revaluation reserve | (4,959) | (4,959) | |||||||
| Reversals of impairments | 218 | 2,526 | 2,744 | ||||||
| Revaluations | 32 | 1,029 | (10) | 1,051 | |||||
| Reclassifications | 3,779 | (3,750) | 7 | 36 | |||||
| Valuation or gross cost at 31 March 2024 | 5,107 | 82,429 | 160 | 10 | 2,344 | 103 | 11,909 | 702 | 102,764 |
| Accumulated depreciation at 1 April 2023 | 3,050 | 10 | 1,074 | 103 | 6,527 | 412 | 11,176 | ||
| Provided during the year | 2,727 | 9 | 143 | 1,346 | 29 | 4,254 | |||
| Revaluations | (5,777) | (19) | (5,796) | ||||||
| Accumulated depreciation at 31 March 2024 | 1,217 | 103 | 7,873 | 441 | 9,634 | ||||
| Net book value at 31 March 2024 | 5,107 | 82,429 | 160 | 10 | 1,127 | 4,036 | 261 | 93,130 | |
| Net book value at 1 April 2023 | 4,857 | 73,069 | 160 | 3,760 | 1,087 | 4,248 | 124 | 87,305 |
Note 16.2 property, plant and equipment financing 2024 and 2025
| Category | Land (£000) | Buildings excluding dwellings (£000 | Dwellings (£000) | Assets under construction (£000) | Plant and machinery (£000) | Transport equipment (£000) | Information technology (£000) | Furniture and fittings (£000) | Total (£000) |
|---|---|---|---|---|---|---|---|---|---|
| Net book value at 31 March 2025: owned – purchased | 5,222 | 55,992 | 190 | 555 | 1,307 | 83 | 4,878 | 191 | 68,418 |
| Net book value at 31 March 2025: on-SoFP Private Finance Initiative contracts and other service concession arrangements | 25,606 | 25,606 | |||||||
| Owned: donated or granted | 21 | 21 | |||||||
| NBV total at 31 March 2025 | 5,222 | 81,598 | 190 | 555 | 1,328 | 83 | 4,878 | 191 | 94,045 |
Note 16.3 property, plant and equipment financing 2023 and 2024
| Category | Land (£000) | Buildings excluding dwellings (£000) | Dwellings (£000) | Assets under construction (£000) | Plant and machinery (£000) | Transport equipment (£000) | Information technology (£000) | Furniture and fittings (£000) | Total (£000) |
|---|---|---|---|---|---|---|---|---|---|
| Net book value at 31 March 2024: owned – purchased | 5,107 | 55,678 | 160 | 10 | 1,127 | 4,036 | 261 | 66,379 | |
| Net book value at 31 March 2024: on-SoFP Private Finance Initiative contracts and other service concession arrangements | 25,531 | 25,531 | |||||||
| NBV total at 31 March 2024 | 5,107 | 81,209 | 160 | 10 | 1,127 | 4,036 | 261 | 91,910 |
| Category | Land (£000) | Buildings excluding dwellings (£000) | Dwellings (£000) | Assets under construction (£000) | Plant and machinery (£000) | Transport equipment (£000) | Information technology (£000) | Furniture and fittings (£000) | Total (£000) |
|---|---|---|---|---|---|---|---|---|---|
| Net book value at 31 March 2024: owned, purchased | 5,107 | 56,898 | 160 | 10 | 1,127 | /td> | 4,036 | 261 | 67,599 |
| Net book value at 31 March 2024: on-SoFP Private Finance Initiative contracts and other service concession arrangements | 25,531 | 25,531 | |||||||
| NBV total at 31 March 2024 | 5,107 | 82,429 | 160 | 10 | 1,127 | 4,036 | 261 | 93,130 |
Note 16.3 useful economic life of property, plant and equipment
| Group and trust | Minimum life (years) | Maximum life (years) |
|---|---|---|
| Land | Infinite | Infinite |
| Buildings, excluding dwellings | 5 | 46 |
| Dwellings | 21 | 21 |
| Plant and machinery | 3 | 30 |
| Transport equipment | 5 | 10 |
| Information technology | 4 | 10 |
| Furniture and fittings | 5 | 10 |
Note 17 revaluations of property, plant and equipment
The trust carried out a revaluation of land and buildings as at 31 March 2025. The valuation was performed by an independent RICS registered valuer from the District Valuer Service. The valuation was that of an alternative site basis
The revaluation is on hypothetical basis from an alternative site and assumes that clinical and support services will be delivered from three sites, Swallownest in Rotherham; Great Oaks in North Lincolnshire and Tickhill Road in Doncaster.
The Doncaster Private Finance Initiative is valued exclusive of VAT (as opposed to the trust owned land and buildings which are valued gross of VAT) and is therefore valued as a separate asset.
The valuation of the trust owned land and building resulted in an increase in value of £26,000 (2023 and 2024: increase £2,800,000). The valuation of the Private Finance Initiative resulted in a decrease in value of £291,000 (2023 and 2024: increase of £548,000).
Note 18 investment property
| Category | Group 2024 and 2025 (£000) | Group 2023 and 2024 (£000) | Trust 2024 and 2025 (£000) | Trust 2023 and 2024 (£000) |
|---|---|---|---|---|
| Carrying value at 1 April | 3,579 | 3,549 | 3,129 | 3,099 |
| Fair value gains taken to SoCI | 45 | 17 | 45 | 17 |
| Acquisitions in year | 46 | |||
| Reclassifications to or from PPE | 13 | 496 | 13 | |
| Carrying value at 31 March | 3,670 | 3,579 | 3,670 | 3,129 |
Note 18.1 investment property income and expenses (group)
| Category | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Direct operating expense arising from investment property which generated rental income in the period | ||
| Total investment property expenses | ||
| Investment property income | 90 | 386 |
IAS 40 defines investment property as property that is held by the owner to earn rentals or for capital appreciation or both. Investment properties are measured at fair value and are categorised at level 3 of the fair value hierarchy. The fair value is measured using the price per square metre for a building from observable market data (for example, prices derived from observed transactions involving comparable buildings in similar locations), adjusted to reflect differences in physical characteristics such as the quality of interior finishes, size and parking.
The trust carried out a revaluation of investment property as at 31 March 2025. The valuation was performed by an independent RICS registered valuer from District Valuer Service.
Note 19 leases Rotherham Doncaster and South Humber NHS Foundation Trust as a lessee
This note details information about leases for which the trust is a lessee.
The trust has a lease for land with The Rotherham NHS FT for the provision of an older people’s unit. It commenced in October 2009 and is for 99 years with a minimum lease term of 60 years.
All other leases are short term and are reviewed in accordance with service provision. These include buildings, lease cars, transport vehicles and other leases.
Note 19.1 right of use assets 2024 and 2025
| Category | Property (land and buildings) (£000) | Transport equipment (£000) | Total (£000) | Of which: leased from Department of Health and Social Care group bodies (£000) |
|---|---|---|---|---|
| Valuation or gross cost at 1 April 2024 – brought forward | 13,867 | 222 | 14,089 | 12,514 |
| Additions | 1,484 | 280 | 1,764 | |
| Remeasurements of the lease liability | 473 | 473 | 473 | |
| Reclassifications | (94) | |||
| Disposals or derecognition | (74) | (74) | ||
| Valuation or gross cost at 31 March 2025 | 15,824 | 428 | 16,252 | 12,893 |
| Accumulated depreciation at 1 April 2024: brought forward | 2,298 | 211 | 2,509 | 2,147 |
| Provided during the year | 1,257 | 68 | 1,325 | 1,091 |
| Disposals or derecognition | (74) | (74) | ||
| Accumulated depreciation at 31 March 2025 | 3,555 | 205 | 3,760 | 3,238 |
| Net book value at 31 March 2025 | 12,269 | 223 | 12,492 | 9,655 |
| Net book value at 31 March 2024 | 11,569 | 11 | 11,580 | 10,367 |
| Net book value of right of use assets leased from other NHS providers | 0 | |||
| Net book value of right of use assets leased from other Department of Health and Social Care group bodies | 9,655 |
Note 19.2 right of use assets 2023 and 2024
| Category | Property (land and buildings) (£000) | Transport equipment (£000) | Total (£000) | Of which: leased from Department of Health and Social Care group bodies (£000) |
|---|---|---|---|---|
| Valuation or gross cost at 1 April 2023 – brought forward | 12,651 | 222 | 12,873 | 11,309 |
| Additions | 348 | 348 | 9 | |
| Remeasurements of the lease liability | 1,205 | 1,205 | 1,205 | |
| Disposals or derecognition | (337) | (337) | ||
| Valuation or gross cost at 31 March 2024 | 13,867 | 222 | 14,089 | 12,514 |
| Accumulated depreciation at 1 April 2023 – brought forward | 1,148 | 136 | 1,284 | 1,037 |
| Provided during the year | 1,219 | 75 | 1,294 | 1,110 |
| Disposals or derecognition | (69) | (69) | ||
| Accumulated depreciation at 31 March 2024 | 2,298 | 211 | 2,509 | 2,147 |
| Net book value at 31 March 2024 | 11,569 | 11 | 11,580 | 10,367 |
| Net book value at 31 March 2023 | 11,503 | 86 | 11,589 | 10,272 |
| Net book value of right of use assets leased from other NHS providers | ||||
| Net book value of right of use assets leased from other Department of Health and Social Care group bodies | 10,367 |
Note 19.2 reconciliation of the carrying value of lease liabilities
Lease liabilities are included within borrowings in the statement of financial position. A breakdown of borrowings is disclosed in note 28.
| Category | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Carrying value at 1 April | 15,186 | 15,403 |
| Lease additions | 1,720 | 156 |
| Lease liability remeasurements | 473 | 1,205 |
| Interest charge arising in year | 148 | 144 |
| Early terminations | (39) | (268) |
| Lease payments (cash outflows) | (1,484) | (1,454) |
| Carrying value at 31 March | 16,004 | 15,186 |
Lease payments for short term leases, leases of low value underlying assets and variable lease payments not dependent on an index or rate are recognised in operating expenditure.
These payments are disclosed in Note 6. Cash outflows in respect of leases recognised on-SoFP are disclosed in the reconciliation above.
Note 19.3 maturity analysis of future lease payments at 31 March 2025
| Category | Total 31 March 2025 (£000) | Of which leased from Department of Health and Social Care group bodies 31 March 2025 (£000) |
|---|---|---|
| Undiscounted future lease payments payable in: not later than one year | 1,680 | 1,251 |
| Undiscounted future lease payments payable in: later than one year and not later than five years | 5,692 | 4,837 |
| Undiscounted future lease payments payable in: later than five years | 10,607 | 9,354 |
| Total gross future lease payments | 17,979 | 15,442 |
| Finance charges allocated to future periods | (1,975) | (1,417) |
| Net finance lease liabilities at 31 March 2025 | 16,004 | 14,025 |
| Of which: leased from other NHS providers | 4,172 | |
| Of which: leased from other Department of Health and Social Care group bodies | 9,853 |
Note 19.4 maturity analysis of future lease payments at 31 March 2024
| Category | Total 31 March 2024 (£000) | Of which leased from Department of Health and Social Care group bodies 31 March 2024 (£000) |
|---|---|---|
| Undiscounted future lease payments payable in: not later than one year | 1,353 | 1,221 |
| Undiscounted future lease payments payable in: later than one year and not later than five years | 5,002 | 4,706 |
| Undiscounted future lease payments payable in: later than five years | 10,378 | 10,333 |
| Total gross future lease payments | 16,733 | 16,260 |
| Finance charges allocated to future periods | (1,547) | (1,532) |
| Net finance lease liabilities at 31 March 2024 | 15,186 | 14,728 |
| Of which: leased from other NHS providers | 4,286 | |
| Of which: leased from other Department of Health and Social Care group bodies | 10,442 |
Note 20 other investments and financial assets (non-current)
| Category | Group 2025 and 2024 (£000) | Group 2023 and 2024 (£000) | Trust 2025 and 2024 (£000) | Trust 2023 and 2024 (£000) |
|---|---|---|---|---|
| Carrying value at 1 April | 2,082 | 2,527 | 22 | 22 |
| Acquisitions in year | 610 | 434 | ||
| Movement in fair value through OCI | 28 | 84 | ||
| Disposals | (1,273) | (963) | ||
| Carrying value at 31 March | 1,447 | 2,082 | 22 | 22 |
The balances for group is the consolidated Investment Portfolio of the subsidiary charity, for trust this is the investment share capital of the subsidiary Flourish Enterprises CIC.
Note 21 disclosure of interests in other entities
Flourish is a wholly owned subsidiary of the trust. The accounting date of Flourish is 31 March 2025. In 2024 and 2025 Flourish’s income was £2,592,000 (2023 and 2024: £2,538,000), the expenditure was £2,595,000 (2023 and 2024: £2,536,000), interest receivable was £5,000 (2023 and 2024: £Nil) At 31 March 2025 the net assets are £71,000 (At 31 March 24: £68,000). Flourish trading results are consolidated in the trust’s financial statements.
Note 22 analysis of charitable fund reserves
The Rotherham Doncaster and South Humber NHS Charitable Fund is a subsidiary of the trust and the Fund’s trading results are consolidated in the trust’s financial statements. The accounting date of the Fund is 31 March 2025.
| Fund | 31 March 2025 (£000) | 31 March 2024 (£000) |
|---|---|---|
| Unrestricted funds: unrestricted income funds | 607 | 1,120 |
| Restricted funds: other restricted income funds | 1,210 | 1,172 |
| Total funds | 1,817 | 2,292 |
Unrestricted income funds are accumulated income funds that are expendable at the discretion of the corporate trustee in furtherance of the charity’s objects. Unrestricted funds may be earmarked or designated for specific future purposes which reduces the amount that is readily available to the charity.
Restricted funds may be accumulated income funds which are expendable at the discretion of the corporate trustee only in furtherance of the specified conditions of the donor and the objects of the charity. They may also be capital funds (for example, endowments) where the assets are required to be invested, or retained for use rather than expended.
Note 23 inventories
| Consumables | Group 31 March 2025 (£000) | Group 31 March 2024 (£000) | Trust 31 March 2025 (£000) | Trust 31 March 2024 (£000) |
|---|---|---|---|---|
| Balance 1 April | 620 | 505 | 602 | 487 |
| Additions | 1,803 | 1,355 | 1,803 | 1,355 |
| Consumed and recognised in expenditure | (2,108) | (1,240) | (2,106) | (1,240) |
| Balance 31 March | 315 | 620 | 299 | 602 |
In response to the COVID 19 pandemic, the Department of Health and Social Care centrally procured personal protective equipment and passed these to NHS providers free of charge. During 2023 and 2024 the trust received £19,000 of items purchased by Department of Health and Social Care . Distribution of inventory by the Department ceased in March 2024. These inventories were recognised as additions to inventory at deemed cost with the corresponding benefit recognised in income. The utilisation of these items is included in the expenses disclosed above.
Note 24 receivables
| Receivables | Group 31 March 2025 (£000) | Group 31 March 2024 (£000) | Trust 31 March 2025 (£000) | Trust 31 March 2024 (£000) |
|---|---|---|---|---|
| Current: contract receivables | 2,041 | 1,963 | 2,027 | 1,947 |
| Current: contract receivables not yet invoiced | 3,668 | 2,996 | 3,739 | 3,350 |
| Current: allowance for impaired contract receivables | (153) | (120) | (153) | (114) |
| Current: prepayments (non-Private Finance Initiative) | 1,698 | 1,388 | 1,698 | 1,388 |
| Current: VAT receivable | 96 | 96 | ||
| Current: PDC dividend receivable | 25 | 25 | ||
| Current: clinician pension tax provision reimbursement funding from NHSE | 4 | 4 | ||
| Current: NHS charitable funds receivables | 14 | 16 | ||
| Total current receivables | 7,297 | 6,339 | 7,340 | 6,667 |
| Non-current: clinician pension tax provision reimbursement funding from NHSE | 145 | 98 | 145 | 98 |
| Total non-current receivables | 145 | 98 | 145 | 98 |
| Total receivables | 7,442 | 6,437 | 7,485 | 6,765 |
| Of which receivable from NHS and Department of Health and Social Care group bodies: current | 1,056 | 1,906 | 1,056 | 1,906 |
| Of which receivable from NHS and Department of Health and Social Care group bodies: non-current | 145 | 98 | 145 | 98 |
Note 25 non current assets held for sale
The trust has one asset held for sale (AHfS) as at 31 March 2025 (31 March 2024: none). The asset is a building asset. Prior to being held for sale, it had a carrying value of £86,000. AHfS should be measured at the lower of the carrying amount or fair value less costs to sell. The lower of these two values was the carrying amount, therefore the AHfS is held at the carrying amount of £86,000. As at 31 March 2025, the trust had put the property on the market, received offers, and accepted one of these offers. The sale is expected to complete by the second quarter of the financial year 2025 and 2026. There is no impairment to the asset since its last valuation on 31 March 2024. The buyer is not a related party.
Note 26 cash and cash equivalents movements
Cash and cash equivalents comprise cash at bank, in hand and cash equivalents. Cash equivalents are readily convertible investments of known value which are subject to an insignificant risk of change in value.
| Category | Group 2025 and 2024 (£000) | Group 2023 and 2024 (£000) | Trust 2025 and 2024 (£000) | Trust 2023 and 2024 (£000) |
|---|---|---|---|---|
| At 1 April | 34,411 | 40,295 | 33,447 | 39,590 |
| Net change in year | (2,203) | (5,884) | (2,026) | (6,143) |
| At 31 March | 32,208 | 34,411 | 31,421 | 33,447 |
| Broken down into: cash at commercial banks and in hand | 895 | 1,153 | 109 | 189 |
| Broken down into: cash with the Government Banking Service | 31,313 | 33,258 | 31,312 | 33,258 |
| Total cash and cash equivalents as in SoFP | 32,208 | 34,411 | 31,421 | 33,447 |
| Total cash and cash equivalents as in SoCF | 32,208 | 34,411 | 31,421 | 33,447 |
Note 26.1 third party assets held by the trust
Rotherham Doncaster and South Humber NHS Foundation Trust held cash and cash equivalents which relate to monies held by the trust on behalf of patients or other parties. This has been excluded from the cash and cash equivalents figure reported in the accounts.
| Category | Group and trust 31 March 2025 (£000) | Group and trust 31 March 2024 (£000) |
|---|---|---|
| Bank balances | 130 | 97 |
| Monies on deposit | 239 | 302 |
| Total third party assets | 369 | 399 |
Note 27 trade and other payables
| Category | Group 31 March 2025 (£000) | Group 31 March 2024 (£000) | Trust 31 March 2025 (£000) | Trust 31 March 2024 (£000) |
|---|---|---|---|---|
| Current: trade payables | 3,116 | 4,433 | 3,128 | 4,178 |
| Current: capital payables | 1,803 | 836 | 1,803 | 836 |
| Current: accruals | 5,046 | 4,877 | 4,851 | 4,877 |
| Current: social security costs | 1,806 | 1,658 | 1,806 | 1,658 |
| Current: VAT payable | 107 | 107 | ||
| Current: other taxes payable | 1,759 | 1,430 | 1,759 | 1,430 |
| Current: PDC dividend payable | 347 | 347 | ||
| Current: pension contributions payable | 2,545 | 2,193 | 2,545 | 2,193 |
| Current: other payables | 210 | 234 | 201 | 225 |
| Current: NHS charitable funds: trade and other payables | 3 | 2 | ||
| Total current trade and other payables | 16,395 | 16,010 | 16,200 | 15,744 |
| Non-current: other payables | ||||
| Total non-current trade and other payables | ||||
| Total trade and other payables | 16,395 | 16,010 | 16,200 | 15,744 |
| Of which payables from NHS and Department of Health and Social Care group bodies: current | 1,220 | 2,028 | 1,220 | 2,028 |
Note 28 other liabilities
| Category | Group 31 March 2025 (£000) | Group 31 March 2024 (£000) | Trust 31 March 2025 (£000) | Trust 31 March 2024 (£000) |
|---|---|---|---|---|
| Current Deferred income: contract liabilities | 294 | 403 | 167 | 291 |
| Total other current liabilities | 294 | 403 | 167 | 291 |
Note 29 Borrowings
| Category | 31 March 2025 (£000) | 31 March 2024 (£000) |
|---|---|---|
| Current: loans from Department of Health and Social Care | 369 | 370 |
| Current: lease liabilities | 1,476 | 1,213 |
| Current: obligations under Private Finance Initiative, Local Improvement Finance Trusts or other service concession contracts (excl. lifecycle) | 1,336 | 1,185 |
| Total current borrowings | 3,181 | 2,768 |
| Non-current: loans from Department of Health and Social Care | 3,115 | 3,478 |
| Non-current: lease liabilities | 14,528 | 13,973 |
| Non-current: obligations under Private Finance Initiative, Local Improvement Finance Trusts or other service concession contracts | 11,198 | 12,137 |
| Total non-current borrowings | 28,841 | 29,588 |
Note 29.1 reconciliation of liabilities arising from financing activities
| Category | Loans from Department of Health and Social Care (£000) | Lease liabilities (£000) | Private Finance Initiative and Local Improvement Finance Trust schemes (£000) | Total (£000) |
|---|---|---|---|---|
| Carrying value at 1 April 2024 | 3,848 | 15,186 | 13,322 | 32,356 |
| Cash movements: financing cash flows – payments and receipts of principal | (363) | (1,337) | (1,224) | (2,924) |
| Cash movements: financing cash flows – payments of interest | (144) | (147) | (1,157) | (1,448) |
| Non-cash movements: additions | 1,720 | 1,720 | ||
| Non-cash movements: lease liability remeasurements | 473 | 473 | ||
| Non-cash movements: application of effective interest rate | 143 | 148 | 1,157 | 1,448 |
| Non-cash movements: remeasurement of Private Finance Initiative or other service concession liability resulting from change in index or rate | 436 | 436 | ||
| Non-cash movements: early terminations | (39) | (39) | ||
| Carrying value at 31 March 2025 | 3,484 | 16,004 | 12,534 | 32,022 |
| Category | Loans from Department of Health and Social Care (£000) | Lease liabilities (£000) | Private Finance Initiative and Local Improvement Finance Trust schemes (£000) | Total (£000) |
|---|---|---|---|---|
| Carrying value at 1 April 2023 | 4,214 | 15,404 | 7,810 | 27,428 |
| Cash movements: financing cash flows, payments and receipts of principal | (363) | (1,311) | (1,647) | (3,321) |
| Cash movements: financing cash flows, payments of interest | (158) | (144) | (661) | (963) |
| Non-cash movements: application of IFRS 16 measurement principles to PFI liability on 1 April 2023 | 6,600 | 6,600 | ||
| Non-cash movements: additions | 156 | 156 | ||
| Non-cash movements: lease liability remeasurements | 1,205 | 1,205 | ||
| Non-cash movements: application of effective interest rate | 155 | 144 | 661 | 960 |
| Non-cash movements: remeasurement of PFI or other service concession liability resulting from change in index or rate | 559 | 559 | ||
| Non-cash movements: early terminations | (268) | (268) | ||
| Carrying value at 31 March 2024 | 3,848 | 15,186 | 13,322 | 32,356 |
Note 30 provisions for liabilities and charges analysis
| Category | Pensions: early departure costs (£000) | Pensions: injury benefits (£000) | Legal claims (£000) | Redundancy (£000) | Other (£000) | Clinicians’ pension reimbursement (£000) | Total (£000) |
|---|---|---|---|---|---|---|---|
| At 1 April 2024 | 132 | 128 | 47 | 74 | 465 | 98 | 944 |
| Change in the discount rate | 1 | (1) | |||||
| Arising during the year | 17 | 9 | 87 | 103 | 345 | 47 | 608 |
| Utilised during the year | (20) | (6) | (31) | (57) | (9) | (2) | (125) |
| Reversed unused | (9) | (17) | (34) | (60) | |||
| Unwinding of discount | 6 | 7 | 7 | 20 | |||
| At 31 March 2025 | 126 | 139 | 103 | 103 | 767 | 149 | 1,387 |
| Expected timing of cash flows: not later than one year | 19 | 6 | 93 | 103 | 428 | 4 | 653 |
| Expected timing of cash flows: later than one year and not later than five years | 70 | 24 | 10 | 193 | 16 | 313 | |
| Expected timing of cash flows: later than five years | 37 | 109 | 146 | 129 | 421 | ||
| Total | 126 | 139 | 103 | 103 | 767 | 149 | 1,387 |
Pension provisions are calculated using the criteria provided by the Government Actuary department. Payments are made over the lifetime of the member and on his or her death a reduced sum is paid to the survivor.
The personal injury allowance is in respect of one ex employee. The provision is calculated using information as to gender, life expectancy and amount of allowance payable.
The legal claim provision is in respect of personal injury claims and is calculated using information provided by NHS Resolution as to probability of outcome and cost.
The redundancy provision relates to the introduction of new models for the provision of services.
Other includes an agenda for change provision and a dilapidation provision relating to the ‘dilapidation’ costs for expired building leases.
The clinicians’ pension provision is in respect of liabilities arising from the 2019 and 2020 clinicians’ pension compensation scheme.
The exact timing of cash-flows is uncertain; the expected timing is shown above.
Note 30.1 clinical negligence liabilities
At 31 March 2025, £4,479,000 was included in provisions of NHS Resolution in respect of clinical negligence liabilities of the trust (31 March 2024: £2,609,000).
Note 31 contingent assets and liabilities
| Assets and liabilities | 31 March 2025 (£000) | 31 March 2024 (£000) |
|---|---|---|
| Value of contingent liabilities NHS Resolution legal claims | 12 | 20 |
| Gross value of contingent liabilities | 12 | 20 |
| Amounts recoverable against liabilities | ||
| Net value of contingent liabilities | 12 | 20 |
Contingent liabilities relate to employer and public personal injury claims.
Note 32 contractual capital commitments
| Contractual capital commitments | 31 March 2025 (£000) | 31 March 2024 (£000) |
|---|---|---|
| Property, plant and equipment | 4,164 | 217 |
| Total | 4,164 | 217 |
Capital commitments are £4,164,000 (2024: £217,000). The majority of this value (£3,994,000) is a refurbishment of the Scunthorpe Mental Health unit, Great Oaks. This refurbishment commenced in March 2025 and will be completed in the year 2025 and 2026. The remainder is items not completed from the 2024 and 2025 capital programme.
Note 33 defined benefit pension schemes
The following information relates to the South Yorkshire Local Government Pension Scheme:
Note 33.1 actuarial assumptions
The main actuarial assumptions used at the date of the Statement of Financial Position in measuring the present value of the defined benefit scheme liabilities are:
| Actuarial assumptions | 31 March 2025 | 31 March 2024 |
|---|---|---|
| Rate of increase in pensions (CPI) | 2.80% | 2.80% |
| Rate of increase in salaries | 3.40% | 3.40% |
| Discount rate | 5.80% | 4.80% |
Duration information at the end of the accounting year
As at the date of the most recent valuation, the duration of the Employer’s funded obligations is 15 years. The financial actuarial assumptions used for IAS19 calculations at the 31 March year ends depends on the market yields at that date. These yields vary from employer to employer depending on the duration of their pension liabilities. For accounting purposes, the duration is assessed as at the date of the latest formal actuarial valuation of the Fund (or the date of admission to the fund if later).
In June 2023, the UK High Court issued a ruling in the case of Virgin Media Limited v NTL Pension Trustees II Limited and other relating to the validity of certain historical pension changes. This judgement was appealed in 2024 and on 24 July 2024, it was confirmed that the earlier ruling by the Court was still applicable. On 5 June 2025, the UK Government announced it will introduce legislation relating to issues arising from this case and, as a result, no impact has been included in the liability of the Local Government Pension Scheme.
Note 33.2 sensitivity analysis
The sensitivities regarding the principal assumptions used to measure the scheme obligations are set out below: This methodology in regards to the sensitivity disclosures in respect of pensions, details the effect on the obligations of changes to the key assumptions in the sensitivity analysis below:
| Change in assumptions at 31 March 2025 | Approximate percentage increase in defined benefit obligation | Approximate monetary amount (£000) |
|---|---|---|
| 0.1% decrease in Real Discount Rate | 1% | 63 |
| 1 year increase in member life expectancy | 4% | 169 |
| 0.1% increase in Salary Increase Rate | 0% | 3 |
| 0.1% increase in the Pension Increase Rate (CPI) | 1% | 62 |
Note 33.3 detailed asset breakdown as at 31 March 2025
| Category | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Equities | 4,371 | 4,446 |
| Government bonds | 1,238 | 1,322 |
| Property | 504 | 519 |
| Cash or liquidity | 94 | 89 |
| Total | 6,207 | 6,376 |
The plan assets are invested in a wide range of categories of investments and therefore the trust is not exposed to any plan specific risks.
Note 33.4 changes in the defined benefit obligation and fair value of plan assets during the year
| Category | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Present value of the defined benefit obligation at 1 April | (4,892) | (4,862) |
| Current service cost | (28) | (34) |
| Interest cost | (231) | (228) |
| Contribution by plan participants | (7) | (8) |
| Remeasurement of the net defined benefit (liability) or asset: actuarial gains or (losses) | 724 | 79 |
| Remeasurement of the net defined benefit (liability) or asset: benefits paid | 203 | 230 |
| Remeasurement of the net defined benefit (liability) or asset: past service costs | (69) | |
| Present value of the defined benefit obligation at 31 March | (4,231) | (4,892) |
| Plan assets at fair value at 1 April | 5,035 | 5,332 |
| Interest income | 278 | 248 |
| Remeasurement of the net defined benefit (liability) or asset: return on plan assets | (306) | 180 |
| Remeasurement of the net defined benefit (liability) or asset: actuarial gain | ||
| Remeasurement of the net defined benefit (liability) or asset: changes in the effect of limiting a net defined benefit asset to the asset ceiling | (580) | (503) |
| Contributions by the plan participants | 7 | 8 |
| Benefits paid | (203) | (230) |
| Plan assets at fair value at 31 March | 4,231 | 5,035 |
| Plan surplus or (deficit) at 31 March | 143 |
Employer contributions in 2025 and 2026 are projected to be £27,000.
Note 33.5 reconciliation of the present value of the defined benefit obligation and the present value of the plan assets to the assets and liabilities recognised in the balance sheet
| Category | 31 March 2025 (£000) | 31 March 2024 (£000) |
|---|---|---|
| Present value of the defined benefit obligation | (4,231) | (4,892) |
| Plan assets at fair value | 4,231 | 5,035 |
| Net defined benefit (obligation) or asset recognised in the SoFP | 143 | |
| Fair value of any reimbursement right | ||
| Net asset or (liability) after the impact of reimbursement rights | 143 |
Note 33.6 Amounts recognised in the Statement of Comprehensive Income
| Category | 31 March 2025 (£000) | 31 March 2024 (£000) |
|---|---|---|
| Current service cost | (28) | (34) |
| Interest income or (expense) | 47 | 20 |
| Past service cost | (69) | |
| Total net gain or (charge) recognised in Statement of Comprehensive Income | 19 | (83) |
Note 34 on-statement of financial position (SoFP) private finance initiative
The Private Finance Initiative provides services accommodation for Mental Health services for Older People and for Mental Health Rehabilitation services. The Private Finance Initiative buildings are on the St Catherine’s site and Bentley in Doncaster.
The Private Finance Initiative agreement is with Albion Healthcare Ltd who have a contract with HBG (Facilities Management) Ltd to provide the hard facilities management services to the buildings. The Private Finance Initiative arrangement is for 27 years commencing in 2005 and ending in 2032. There are no renewal or termination options in the agreement.
The service element of the lease was bought out in 2017 and 2018 and payments now relate solely to the lease of the property. The annual payment in 2024 and 2025 was £2,382,000. The re-pricing of the annual charge is yearly on 1 April in line with the movement in the Retail Price Index.
The scheme has not resulted in any guarantees, commitments or other rights or obligations.
Note 34.1 on-statement of financial position (SoFP) private finance initiative obligations
The following obligations in respect of the private finance initiative are recognised in the statement of financial position:
| Category | 31 March 2025 (£000) | 31 March 2024 (£000) |
|---|---|---|
| Gross private finance initiative liabilities | 16,869 | 18,640 |
| Of which liabilities are due: not later than one year | 2,381 | 2,306 |
| Of which liabilities are due: later than one year and not later than five years | 9,526 | 9,224 |
| Of which liabilities are due: later than five years | 4,962 | 7,110 |
| Of which liabilities are due: finance charges allocated to future periods | (4,335) | (5,318) |
| Net private finance initiative obligation | 12,534 | 13,322 |
| Net private finance initiative obligation: not later than one year | 1,336 | 1,185 |
| Net private finance initiative obligation: later than one year and not later than five years | 6,678 | 5,926 |
| Net private finance initiative obligation: later than five years | 4,520 | 6,211 |
Note 34.2 total on-statement of financial position (SoFP) private finance initiative commitments
Total future commitments under these on-SoFP schemes are as follows:
| Category | 31 March 2025 (£000) | 31 March 2024 (£000) |
|---|---|---|
| Total future payments committed in respect of the PFI, LIFT or other service concession arrangements | 16,869 | 18,640 |
| Of which payments are due: not later than one year | 2,381 | 2,306 |
| Of which payments are due: later than one year and not later than five years | 9,526 | 9,224 |
| Of which payments are due: later than five years | 4,962 | 7,110 |
Note 34.3 analysis of amounts payable to service concession operator
This note provides an analysis of the unitary payments made to the service concession operator:
| Category | 2024 and 2025 (£000) | 2023 and 2024 (£000) |
|---|---|---|
| Unitary payment payable to service concession operator | 2,381 | 2,308 |
| Consisting of: interest charge | 1,157 | 661 |
| Consisting of: repayment of balance sheet obligation | 1,224 | 1,647 |
| Total amount paid to service concession operator | 2,381 | 2,308 |
Note 35 financial instruments
Note 35.1 financial risk management
Financial Reporting Standard IFRS 7 requires disclosure of the role that financial instruments have had during the year in creating or changing the risks a body faces in undertaking its activities. Because of the continuing service provider relationship that the trust has with the integrated care boards and local authorities and the way in which these bodies are financed, the trust is not exposed to the degree of financial risk faced by business entities. Also financial instruments play a much more limited role in creating or changing risk that would be typical of listed companies, to which the financial reporting standard mainly applies.
The trust has limited powers to borrow or invest surplus funds and financial assets and liabilities are generated by day-to-day operational activities rather than being held to change the risks facing the trust in undertaking its activities. The trust’s treasury management operations are carried out by the finance department, within parameters defined formally within the trust’s standing financial instructions and policies agreed by the board of directors. The trust’s treasury activity is subject to review by internal audit.
Currency risk
The trust is principally a domestic organisation with the great majority of transactions, assets and liabilities being in the UK and sterling based. The trust has no overseas operations; the trust therefore has low exposure to currency rate fluctuations.
Credit risk
Because the majority of the trust’s income comes from contracts with other public sector bodies, the trust has little exposure to credit risk. The maximum exposures at 31 March 2025 are in receivables from other customers, as disclosed in Trade and other receivables, note 24.
Liquidity risk
The trust’s operating costs are incurred under annual service agreements with integrated care boards and local authorities, which are financed from resources voted annually by Parliament. The trust is not, therefore exposed to significant liquidity risk.
Interest rate risk
The trust is not exposed to any interest rate risk. The only loan that the trust has is with the Department of Health and Social Care and this is at a fixed interest rate.
Note 35.2 carrying values of financial assets (group)
| Carrying values of financial assets as at 31 March 2025 | Held at amortised cost (£000) | Held at fair value through OCI (£000) | Total book value (£000) |
|---|---|---|---|
| Trade and other receivables excluding non financial assets | 5,484 | 5,484 | |
| Cash and cash equivalents | 31,777 | 31,777 | |
| Consolidated NHS Charitable fund financial assets | 445 | 1,447 | 1,892 |
| Total at 31 March 2025 | 37,706 | 1,447 | 39,153 |
| Carrying values of financial assets as at 31 March 2024 | Held at amortised cost (£000) | Held at fair value through OCI (£000) | Total book value (£000) |
|---|---|---|---|
| Trade and other receivables excluding non financial assets | 4,839 | 4,839 | |
| Cash and cash equivalents | 33,859 | 33,859 | |
| Consolidated NHS Charitable fund financial assets | 568 | 2,082 | 2,650 |
| Total at 31 March 2024 | 39,266 | 2,082 | 41,348 |
Note 35.2 carrying values of financial assets (trust)
| Carrying values of financial assets as at 31 March 2025 | Held at amortised cost (£000) | Held at fair value through OCI (£000) | Total book value (£000) |
|---|---|---|---|
| Trade and other receivables excluding non financial assets | 5,613 | 5,613 | |
| Other investments or financial assets | 22 | 22 | |
| Cash and cash equivalents | 31,421 | 31,421 | |
| Total at 31 March 2025 – | 37,056 | 37,056 |
| Carrying values of financial assets as at 31 March 2024 | Held at amortised cost (£000) | Held at fair value through OCI (£000) | Total book value (£000) |
|---|---|---|---|
| Trade and other receivables excluding non financial assets | 5,182 | 5,182 | |
| Cash and cash equivalents | 33,447 | 33,447 | |
| Total at 31 March 2024 | 38,629 | 38,629 |
Note 35.3 carrying values of financial liabilities (group)
| Carrying values of financial liabilities as at 31 March 2025 | Held at amortised cost (£000) | Total book value (£000) |
|---|---|---|
| Loans from the Department of Health and Social Care | 3,484 | 3,484 |
| Obligations under leases | 16,004 | 16,004 |
| Obligations under PFI, LIFT and other service concessions | 12,534 | 12,534 |
| Trade and other payables excluding non financial liabilities | 8,049 | 8,049 |
| Consolidated NHS charitable fund financial liabilities | 3 | 3 |
| Total at 31 March 2025 | 40,074 | 40,074 |
| Carrying values of financial liabilities as at 31 March 2024 | Held at amortised cost (£000) | Total book value (£000) |
|---|---|---|
| Loans from the Department of Health and Social Care | 3,848 | 3,848 |
| Obligations under leases | 15,186 | 15,186 |
| Obligations under PFI, LIFT and other service concessions | 13,322 | 13,322 |
| Trade and other payables excluding non financial liabilities | 11,945 | 11,945 |
| Consolidated NHS charitable fund financial liabilities | 2 | 2 |
| Total at 31 March 2024 | 44,303 | 44,303 |
Note 35.3 carrying values of financial liabilities (trust)
| Carrying values of financial liabilities as at 31 March 2025 | Held at amortised cost (£000) | Total book value (£000) |
|---|---|---|
| Loans from the Department of Health and Social Care | 3,484 | 3,484 |
| Obligations under leases | 16,004 | 16,004 |
| Obligations under PFI, LIFT and other service concessions | 12,534 | 12,534 |
| Trade and other payables excluding non financial liabilities | 7,857 | 7,857 |
| Total at 31 March 2025 | 39,879 | 39,879 |
| Carrying values of financial liabilities as at 31 March 2024 | Held at amortised cost (£000) | Total book value (£000) |
|---|---|---|
| Loans from the Department of Health and Social Care | 3,848 | 3,848 |
| Obligations under leases | 15,186 | 15,186 |
| Obligations under PFI, LIFT and other service concessions | 13,322 | 13,322 |
| Trade and other payables excluding non financial liabilities | 11,681 | 11,681 |
| Total at 31 March 2024 | 44,037 | 44,037 |
Note 35.4 fair values of financial assets and liabilities
The book value of the trust’s assets and liabilities at 31 March 2025 is a reasonable approximation of fair value.
Note 35.5 maturity of financial liabilities
The following maturity profile of financial liabilities is based on the contractual, undiscounted cash flows. This differs to the amounts recognised in the statement of financial position, which are discounted to present value.
| Category | Group 31 March 2025 (£000) | Group 31 March 2024 (£000) | Trust 31 March 2025 (£000) | Trust 31 March 2024 (£000) |
|---|---|---|---|---|
| In one year or less | 12,482 | 15,977 | 12,287 | 15,711 |
| In more than one year but not more than five years | 17,033 | 16,041 | 17,033 | 16,041 |
| In more than five years | 16,869 | 19,153 | 16,869 | 19,153 |
| Total | 46,384 | 51,171 | 46,189 | 50,905 |
Note 36 losses and special payments
| Category | Total number of cases | Total value of cases (£000) | Total number of cases | Total value of cases (£000) |
|---|---|---|---|---|
| Losses: cash losses (the cumulative costs are small and round down to £000 so displayed as a value of £Nil k) | 2 | 9 | 1 | |
| Losses: bad debts and claims abandoned | 1 | 12 | 1 | 1 |
| Losses: stores losses and damage to property (the cumulative costs are small and round down to £000 so displayed as a value of £Nil k) | 2 | 1 | 0 | |
| Total losses | 5 | 12 | 11 | 2 |
| Special payments: compensation under court order or legally binding arbitration award | 1 | 1 | 2 | 5 |
| Special payments: ex-gratia payments | 10 | 5 | 18 | 3 |
| Special payments: special severance payments | 1 | 14 | ||
| Total special payments | 11 | 6 | 21 | 22 |
| Total losses and special payments | 16 | 18 | 32 | 24 |
The cumulative costs are small and round down to £000 so displayed as a value of £Nil k.
Note 37 related parties
The trust is a body corporate established by order of the Secretary of State.
The Department of Health and Social Care is regarded as the ultimate controlling party. During the year the trust had a number of material transactions with the Department and with other entities for which the Department is regarded as the parent. The trust also had a number of material transactions with other Government departments and other central and local government bodies. These entities are listed below.
- The Department of Health and Social Care
- Other NHS providers
- integrated care boards and NHS England-Other health bodies
- Other Government departments
- Local authorities
The Board does not have any related party transactions to disclose.
Note 38 events after the reporting date
There are no events after the reporting date.
Page last reviewed: October 07, 2025
Next review due: October 07, 2026
Problem with this page?
Please tell us about any problems you have found with this web page.